Video:Visceral leishmaniasis
| Visceral leishmaniasis (Tutorial) | |
|---|---|
| Commons / NC | |
| Steps for video creation | |
| Step 1 | Preview my changes (10 sec) |
| Step 2 | Upload to Commons (10 min) |
Introduction
Visceral leishmaniasis also known as kala-azar, is the most severe form of leishmaniasis.Symptoms may include weakness, and an enlarged liver and spleen.[1]Treatment is often with liposomal amphotericin B; however, in Africa sodium stibogluconate and paromomycin work better, though there are greater side effects.[2]As of 2021, Leishmania-HIV coinfection has been identified in 45 countries.[1]
Presentation
When an individual develops visceral leishmaniasis, the most typical symptoms are fever, weight loss, anemia and the enlargement of the spleen, with enlargement of the liver sometimes being seen as well.[3]

Complications
Post-kala-azar dermal leishmaniasis is a recurrence of leishmaniasis that appears on the skin of affected individuals months and even up to 20 years after being partially treated, untreated or even in those considered adequately treated.[4][5]

Cause
Two species of Leishmania are known to give rise to the visceral form of the disease. The species commonly found in East Africa and the Indian subcontinent is L. donovani and the species found in Europe, North Africa, and Latin America is L. infantum, also known as L. chagasi.[6]

Diagnosis
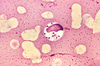
In terms of the diagnosis we find that tissue from bone marrow can be examined for the parasite under a microscope and via molecular tests. Detection of the antibody can also be done to establish the diagnosis via blood test.[7]

Prevention
As of 2018, there are no vaccines or preventive drugs for visceral leishmaniasis, but vaccines are in development.[8][9] The most effective method to prevent infection is to protect from sand fly bites via avoiding outdoor activities, especially from dusk to dawn, when sand flies are most active, applying insect repellent to exposed skin and finally wearing long-sleeved shirts, long pants, and socks when outdoors.[8][10]

Treatment
Liposomal amphotericin B is an antifungal medication that kills fungi and certain protozoa, it is administered via IV infusion and is approved for treating visceral leishmaniasis.[11]

Epidemiology
More than 90 percent of Visceral leishmaniasis cases occurred in seven countries in 2015, including Brazil, Ethiopia, India, Kenya, Somalia, South Sudan and Sudan.[12] Cases of Visceral leishmaniasis, however, are present in at least 60 countries worldwide.[12]

History
The Indian medical practitioner Upendra Nath Brahmachari was nominated for the Nobel Prize in Physiology or Medicine in 1929 for his discovery of ureastibamine, an antimonial compound for the treatment of kala-azar, and his work on a new disease, post kala-azar dermal leishmaniasis.[13]

References
- ↑ 1.0 1.1 "Leishmaniasis". www.who.int. Archived from the original on 26 July 2019. Retrieved 16 July 2023.
- ↑ van Griensven, J; Diro, E (March 2019). "Visceral Leishmaniasis: Recent Advances in Diagnostics and Treatment Regimens". Infectious disease clinics of North America. 33 (1): 79–99. doi:10.1016/j.idc.2018.10.005. PMID 30712769.
- ↑ Baker, John R.; Muller, Ralph; Rollinson, David (22 August 2002). Advances in Parasitology. Elsevier. p. 18. ISBN 978-0-08-049037-3. Archived from the original on 12 July 2023. Retrieved 11 July 2023.
- ↑ Banerjee N (December 1973). "Role of I.M.A. during natural calamities and national emergencies". Journal of the Indian Medical Association. 61 (11): 477–81. PMID 4600129.
- ↑ Rathi SK, Pandhi RK, Chopra P, Khanna N (2005). "Post-kala-azar dermal leishmaniasis: a histopathological study". Indian Journal of Dermatology, Venereology and Leprology. 71 (4): 250–3. doi:10.4103/0378-6323.16616. PMID 16394433.
- ↑ Chappuis F, et al. (2007). "Visceral leishmaniasis: what are the needs for diagnosis, treatment and control?" (PDF). Nature Reviews Microbiology. 5 (11): 873–82. doi:10.1038/nrmicro1748. PMID 17938629. S2CID 6963295. Archived (PDF) from the original on 2018-10-24. Retrieved 2022-03-21.
- ↑ Prevention, CDC-Centers for Disease Control and (5 October 2023). "CDC - Leishmaniasis - Diagnosis". www.cdc.gov. Retrieved 11 May 2024.
- ↑ 8.0 8.1 Prevention, CDC-Centers for Disease Control and (19 February 2020). "CDC - Leishmaniasis - Prevention & Control". www.cdc.gov. Retrieved 12 May 2024.
- ↑ Gillespie, Portia M.; Beaumier, Coreen M.; Strych, Ulrich; Hayward, Tara; Hotez, Peter J.; Bottazzi, Maria Elena (2016-06-03). "Status of vaccine research and development of vaccines for leishmaniasis". Vaccine. 34 (26): 2992–2995. doi:10.1016/j.vaccine.2015.12.071. ISSN 1873-2518. PMID 26973063.
- ↑ "Leishmaniasis, Visceral | CDC Yellow Book 2024". wwwnc.cdc.gov. Archived from the original on 22 June 2023. Retrieved 6 July 2023.
- ↑ Noor, Asif; Preuss, Charles V. (2024). "Amphotericin B". StatPearls. StatPearls Publishing.
- ↑ 12.0 12.1 Burza, Sakib; Croft, Simon L; Boelaert, Marleen (September 2018). "Leishmaniasis". The Lancet. 392 (10151): 951–970. doi:10.1016/S0140-6736(18)31204-2.
- ↑ Nobel Foundation (2008).The Nomination Database for the Nobel Prize in Physiology or Medicine, 1901-1951 Archived 2016-05-08 at the Wayback Machine