Video:Typhoid fever
| Typhoid fever (Tutorial) | |
|---|---|
| On Commons | |
| Steps for video creation | |
| Step 1 | Preview my changes (10 sec) |
| Step 2 | Upload to Commons (10 min) |
Definition
Typhoid fever, also known simply as typhoid, is a bacterial illness caused by Salmonella typhi.[1]
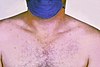
Onset of illness
Symptoms typically begin, six to thirty days after exposure to food or water, contaminated with the feces of an infected person.[2]

Symptoms
Early symptoms may vary from mild to severe.[3][4] Usually, there is a gradual onset of a high fever over several days;[3] weakness, abdominal pain, constipation, headaches, and mild vomiting.[4][5]

Other symptoms
Some people will develop a skin rash, with rose colored spots.[4]

Severe cases and carriers
In severe cases there may be confusion.[5] Without treatment, symptoms may last weeks or months.[4]

Carriers
Other people may carry the bacterium without being affected; however, they are still able to spread the disease to others.[2]

Causes
The cause is the bacterium Salmonella Typhi, that grows in the intestines and blood.[4][5]

Spread
Typhoid is spread by eating or drinking food or water contaminated with the feces of an infected person.

Risk factor
Risk factors include poor sanitation and poor hygiene.[1]

Risk factor 2
Those who travel in the developing world are also at risk.[5]
Diagnosis
Because symptoms are similar to those of many other infectious diseases,[5] diagnosis requires either culturing the bacteria, or detecting the bacterium's DNA in the blood, stool, or bone marrow.[4][1][6]

Bone marrow testing
Culturing the bacterium can be difficult, so [7] bone marrow testing is the most accurate.[6]

Prevention
The chlorination of public drinking water led to the sharp reduction of typhoid in developed nations.[8] In typhoid-endemic countries,

Typhoid vaccines have been shown to prevent 40 to 90% of cases during the first two years,[9] and may have some effect for up to seven years.[1]

Travel to endemic areas
Vaccination is recommended for those at high risk, or people traveling to areas where the disease is common.[2]

Other efforts
Other efforts to prevent the disease include providing clean drinking water, good sanitation, and handwashing.[4][2]
Infected persons quarantine
Until it has been confirmed that an individual's infection is cleared, the individual should not prepare food for others.[4]

Treatment
The disease is treated with antibiotics such as azithromycin, fluoroquinolones, or third generation cephalosporins.[1]

Resistance
Resistance to these antibiotics has been developing, which has made treatment more difficult.[1][10]

Epidemiology
In 2015, there were 12.5 million new cases worldwide.[11]
Epidemiology - geography
The disease is most common in India.[1]

Epidemiology - demographic
Children are most commonly affected.[1][2]

Prognosis
Rates of disease decreased in the developed world in the 1940s, as a result of improved sanitation, and use of antibiotics to treat the disease.[2]

Risk of death
The risk of death may be as high as 20% without treatment, and 1 to 4% with treatment.[2]

History
The most notorious carrier of typhoid fever, but by no means the most destructive, was Mary Mallon, also known as Typhoid Mary.

History 2
In 1907, she was the first typhoid carrier identified and traced, while working as a cook in New York. She was associated with 53 cases and three deaths.[12]

History 3
She died of pneumonia after 26 years in quarantine.

References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Wain, J; Hendriksen, RS; Mikoleit, ML; Keddy, KH; Ochiai, RL (21 March 2015). "Typhoid fever". Lancet. 385 (9973): 1136–45. doi:10.1016/s0140-6736(13)62708-7. PMID 25458731.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 "Typhoid vaccines: WHO position paper" (PDF). Wkly Epidemiol Rec. 83 (6): 49–59. February 8, 2008. PMID 18260212. Archived (PDF) from the original on April 2, 2015.
- ↑ 3.0 3.1 Anna E. Newton (2014). "3 Infectious Diseases Related To Travel". CDC health information for international travel 2014 : the yellow book. ISBN 9780199948499. Archived from the original on 2015-07-02.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 "Typhoid Fever". cdc.gov. May 14, 2013. Archived from the original on 6 June 2016. Retrieved 28 March 2015.
- ↑ 5.0 5.1 5.2 5.3 5.4 "Typhoid Fever". cdc.gov. May 14, 2013. Archived from the original on 2 April 2015. Retrieved 28 March 2015.
- ↑ 6.0 6.1 Crump, JA; Mintz, ED (15 January 2010). "Global trends in typhoid and paratyphoid Fever". Clin Infect Dis. 50 (2): 241–6. doi:10.1086/649541. PMC 2798017. PMID 20014951.
- ↑ Alan J. Magill (2013). Hunter's tropical medicine and emerging infectious diseases (9th ed.). London: Saunders/Elsevier. pp. 568–572. ISBN 9781455740437. Archived from the original on 2017-02-28.
- ↑ Leal, John L. (1909). "The Sterilization Plant of the Jersey City Water Supply Company at Boonton, N.J." Proceedings American Water Works Association. pp. 100–9.
- ↑ Milligan, R; Paul, M; Richardson, M; Neuberger, A (31 May 2018). "Vaccines for preventing typhoid fever". The Cochrane Database of Systematic Reviews. 5: CD001261. doi:10.1002/14651858.CD001261.pub4. PMID 29851031.
- ↑ Chatham-Stephens, K; Medalla, F; Hughes, M; Appiah, GD; Aubert, RD; Caidi, H; Angelo, KM; Walker, AT; Hatley, N; Masani, S; Nash, J; Belko, J; Ryan, ET; Mintz, E; Friedman, CR (11 January 2019). "Emergence of Extensively Drug-Resistant Salmonella Typhi Infections Among Travelers to or from Pakistan - United States, 2016-2018". MMWR. Morbidity and Mortality Weekly Report. 68 (1): 11–13. doi:10.15585/mmwr.mm6801a3. PMC 6342547. PMID 30629573.
- ↑ GBD 2015 Disease and Injury Incidence and Prevalence, Collaborators. (8 October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ↑ "Nova: The Most Dangerous Woman in America". Archived from the original on 2010-04-26.