Transfusion-associated graft-versus-host disease
| Transfusion-associated graft-versus-host-disease | |
|---|---|
| Other names: TA-GvHD | |
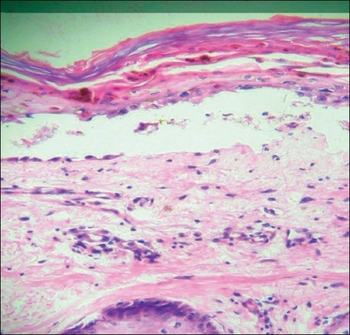 | |
| Transfusion associated graft versus host disease -Mononuclear cell infiltration and inflammation of affected epithelium, with focal vacuolation of basal epithelial cells | |
| Specialty | Hematology |
Transfusion-associated graft-versus-host disease (TA-GvHD) is a rare complication of blood transfusion, in which the immunologically competent donor T lymphocytes mount an immune response against the recipient's lymphoid tissue.[1] These donor lymphocytes engraft, recognize recipient cells as foreign and mount an immune response against recipient tissues.[2] Donor lymphocytes are usually identified as foreign and destroyed by the recipient's immune system. However, in situations where the recipient is severely immunocompromised, or when the donor and recipient HLA type is similar (as can occur in directed donations from first-degree relatives), the recipient's immune system is not able to destroy the donor lymphocytes. This can result in transfusion associated graft-versus-host disease.
Signs and symptoms
The clinical presentation is the same as GvHD occurring in other settings, such as bone marrow transplantation. TA-GvHD can develop two days to six weeks after the transfusion.[3] Typical symptoms include:[3]
- Fever
- Erythematous maculopapular rash, which can progress to generalised erythroderma
- Toxic epidermal necrolysis in extreme cases
- Hepatomegaly
- Diarrhea
Other symptoms can include cough, abdominal pain, vomiting, and profuse diarrhea (up to 8 liters/day).[citation needed]
Diagnosis
Laboratory findings include pancytopenia, marrow aplasia, abnormal liver enzymes, and electrolyte imbalance (when diarrhea is present).[citation needed]
TA-GvHD can be suspected from a biopsy of the affected skin or liver,[3] and established by HLA analysis of the circulating lymphocytes. This testing can identify circulating lymphocytes with a different HLA type than the tissue cells of the host.[citation needed]
Prevention
Prevention includes gamma irradiation of the lymphocyte-containing blood components such as red blood cells, platelets and granulocytes. Irradiated blood components should be issued in the following situations:[4]
- Intrauterine transfusions
- Prematurity, low birthweight, or erythroblastosis fetalis in newborns
- Congenital immunodeficiencies
- Certain hematologic malignancies (e.g. Hodgkin lymphoma)
- Patients undergoing hematopoietic stem cell transplantation
- Components that are HLA matched, or directed donations from a family member
- Patients receiving fludarabine therapy
- Patients receiving granulocyte transfusions
Treatment
Treatment is supportive. No available form of therapy has proven effective in treating TA-GvHD and it is fatal in more than 90% of cases.[2]
Epidemiology
The incidence of TA-GvHD in immunocompromised patients receiving blood transfusions is estimated to be 0.1–1.0%, and mortality around 80–90%. Mortality is higher in TA-GvHD than in GvHD associated with bone marrow transplantation, where the engrafted lymphoid cells in the bone marrow are of donor origin (in autotransplant) and therefore the immune reaction is not directed against them.[citation needed]
The most common causes of death in TA-GvHD are infections and hemorrhages secondary to pancytopenia and liver dysfunction.[citation needed]
References
- ↑ "Complications of Transfusion: Transfusion Medicine: Merck Manual Professional". Archived from the original on 2010-10-23. Retrieved 2009-02-09.
- ↑ 2.0 2.1 Savage, William J. (June 2016). "Transfusion Reactions". Hematology/Oncology Clinics of North America. 30 (3): 619–634. doi:10.1016/j.hoc.2016.01.012. ISSN 1558-1977. PMID 27113000.
- ↑ 3.0 3.1 3.2 "NHSN | CDC". www.cdc.gov. 2017-12-29. Archived from the original on 2018-09-21. Retrieved 2018-09-18.
- ↑ Technical manual. Fung, Mark K., Grossman, Brenda J., Hillyer, Christopher D., Westhoff, Connie M., American Association of Blood Banks. (18th ed.). Bethesda, Md.: American Association of Blood Banks. 2014. ISBN 978-1563958885. OCLC 881812415.
{{cite book}}: CS1 maint: others (link)
Further reading
- Anwar M, Bhatti F (2003). "Transfusion associated graft versus host disease". J Ayub Med Coll Abbottabad. 15 (3): 56–8. PMID 14727344. Archived from the original on 2021-06-18. Retrieved 2022-03-16.
- Gupta, A; Bansal, D; Dass, R; Das, A (2004). "Transfusion Associated Graft versus Host Disease" (PDF). Indian Pediatr. 41 (12): 1260–1264. PMID 15623910. Archived (PDF) from the original on 2017-08-11. Retrieved 2022-03-16.
- Darrell J. Triulzi: Transfusion associated graft vs. host disease and irradiated blood components
- Eric Kardon, eMedicine: Transfusion Reactions Archived 2021-04-22 at the Wayback Machine
| Classification |
|---|