Tonsil stones
| Tonsil stones | |
|---|---|
| Other names: Tonsillolith, tonsillolithiasis, tonsillar stones, chronic caseous tonsillitis | |
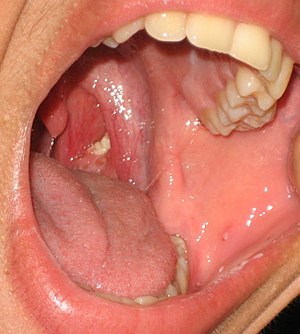 | |
| A tonsillolith lodged in the tonsillar crypt | |
| Specialty | Otorhinolaryngology |
| Symptoms | None, bad breath[1] |
| Risk factors | Recurrent throat infections[2] |
| Differential diagnosis | Calcified granulomatous disease, mycosis, syphilis[2] |
| Treatment | None, gargling with salt water, tonsillectomy[1] |
| Medication | Chlorhexidine[1] |
| Frequency | Up to 10%[1] |
Tonsil stones, also known as tonsilloliths, are mineralization of debris within the crevices of the tonsils.[1][3] When not mineralized, the presence of debris is known as chronic caseous tonsillitis (CCT).[1] Symptoms may include bad breath.[1] Generally there is no pain, though there may be the feeling of something present.[1]
Risk factors may include recurrent throat infections.[2] Tonsil stones contain a biofilm composed of a number of different bacteria.[1] While they most commonly occur in the palatine tonsils, they may also occur in the lingual tonsils.[3] Tonsil stones have been recorded weighing from 0.3 g to 42 g.[3] They may be found during medical imaging for other reasons.[4]
If tonsil stones do not bother a person, no treatment is needed.[1] Otherwise gargling salt water and manual removal may be tried.[1] Chlorhexidine may also be tried.[1] Surgical treatment may include partial or complete tonsil removal.[1][5] Up to 10% of people have tonsil stones.[1] Males and females are affected equally.[1] Older people are more commonly affected.[2]
Signs and symptoms
Tonsil stones may produce no symptoms or they may be associated with bad breath.[1] The smell may be that of rotting eggs.[6]
Occasionally there may be pain when swallowing.[7] Even when they are large, some tonsil stones are only discovered incidentally on X-rays or CAT scans. Other symptoms include a metallic taste, throat closing or tightening, coughing fits, and choking.
Larger tonsil stones may cause recurrent bad breath, which frequently accompanies a tonsil infection, sore throat, white debris, a bad taste in the back of the throat, difficulty swallowing, ear ache, and tonsil swelling.[8] A medical study conducted in 2007 found an association between tonsilloliths and bad breath in patients with a certain type of recurrent tonsillitis. Among those with bad breath, 75% of the subjects had tonsilloliths, while only 6% of subjects with normal halitometry values (normal breath) had tonsilloliths. A foreign body sensation may also exist in the back of the throat. The condition may also be an asymptomatic condition, with detection upon palpating a hard intratonsillar or submucosal mass.
-
A tonsillolith protrudes from the tonsil
-
Large tonsillolith half exposed on tonsil
-
Closeup of a tonsillolith
Pathophysiology

The mechanism by which these calculi form is subject to debate,[3] though they appear to result from the accumulation of material retained within the crypts, along with the growth of bacteria and fungi – sometimes in association with persistent chronic purulent tonsillitis.
In 2009, an association between biofilms and tonsilloliths was shown. Central to the biofilm concept is the assumption that bacteria form a three dimensional structure, dormant bacteria being in the center to serve as a constant nidus of infection. This impermeable structure renders the biofilm immune to antibiotic treatment. By use of confocal microscopy and microelectrodes, biofilms similar to dental biofilms were shown to be present in the tonsillolith, with oxygen respiration at the outer layer of tonsillolith, denitrification toward the middle, and acidification toward the bottom.[9]
Diagnosis

Diagnosis is usually made upon inspection. Tonsilloliths are difficult to diagnose in the absence of clear manifestations, and often constitute casual findings of routine radiological studies.
Classification
Tonsilloliths or tonsil stones are calcifications that form in the crypts of the palatal tonsils. They are also known to form in the throat and on the roof of the mouth. Tonsils are filled with crevices where bacteria and other materials, including dead cells and mucus, can become trapped. When this occurs, the debris can become concentrated in white formations that occur in the pockets.[8] Tonsilloliths are formed when this trapped debris accumulates and are expressed from the tonsil. They are generally soft, sometimes rubbery. This tends to occur most often in people who suffer from chronic inflammation in their tonsils or repeated bouts of tonsillitis.[8] They are often associated with post-nasal drip.
Giant
Much rarer than the typical tonsil stones are giant tonsilloliths. Giant tonsilloliths may often be mistaken for other oral maladies, including peritonsillar abscess, and tumours of the tonsil.[10]
Differential diagnosis
Imaging diagnostic techniques can identify a radiopaque mass that may be mistaken for foreign bodies, displaced teeth or calcified blood vessels. CT scan may reveal nonspecific calcified images in the tonsillar zone. The differential diagnosis must be established with acute and chronic tonsillitis, tonsillar hypertrophy, peritonsillar abscesses, foreign bodies, phlebolites, ectopic bone or cartilage, lymph nodes, granulomatous lesions or calcification of the stylohyoid ligament in the context of Eagle syndrome (elongated styloid process).[11]
Differential diagnosis of tonsilloliths includes foreign body, calcified granuloma, malignancy, an enlarged temporal styloid process or rarely, isolated bone which is usually derived from embryonic rests originating from the branchial arches.[12]
Treatment
If tonsil stones do not bother a person, no treatment is needed.[1] Otherwise gargling saltwater and manual removal may be tried.[1] Chlorhexidine may also be tried.[1] Surgical treatment may include partial or complete tonsil removal.[1]
Some people are able to remove tonsil stones using a cotton swab or finger. Oral irrigators are also effective. Most electric oral irrigators are unsuitable for tonsil stone removal because they are too powerful and are likely to cause discomfort and rupture the tonsils, which could result in further complications such as infection. Irrigators that connect directly to the sink tap via a threaded attachment or otherwise are suitable for tonsil stone removal and everyday washing of the tonsils because they can jet water at low-pressure levels that the user can adjust by simply turning the sink tap, allowing for a continuous range of pressures to suit each user's requirements.[8]
Or, there is a tonsil stone remover in the manual pump system. manual pump-type tonsil stone remover can adjust the water pressure depending on the number of pumps, effectively removing tonsil stones.
More simply still, gargling with warm, salty water may help alleviate the discomfort of tonsillitis, which often accompanies tonsil stones. Vigorous gargling each morning can also keep the tonsil crypts clear of all but the most persistent tonsilloliths.[8]
Curettage
Larger tonsil stones may require removal by curettage (scooping) or otherwise, although thorough irrigation will still be required afterward to effectively wash out smaller pieces. Larger lesions may require local excision, although these treatments may not completely help the bad breath issues that are often associated with this condition.
Laser
Another option is to decrease the surface area (crypts, crevices, etc.) of the tonsils via laser resurfacing. The procedure is called a laser cryptolysis. It can be performed using a local anesthetic. A scanned carbon dioxide laser selectively vaporizes and smooths the surface of the tonsils. This technique flattens the edges of the crypts and crevices that collect the debris, preventing trapped material from forming stones.
Surgery
Tonsillectomy may be indicated if bad breath due to tonsillar stones persists despite other measures.[13]
Epidemiology
Tonsilloliths or tonsillar concretions occur in up to 10% of the population, frequently due to episodes of tonsillitis.[14] While small concretions in the tonsils are common, true stones are less so.[3] They commonly occur in young adults and are rare in children.[3]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 Ferguson, M; Aydin, M; Mickel, J (October 2014). "Halitosis and the tonsils: a review of management". Otolaryngology–Head and Neck Surgery. 151 (4): 567–74. doi:10.1177/0194599814544881. PMID 25096359.
- ↑ 2.0 2.1 2.2 2.3 White, Stuart C.; Pharoah, Michael J. (2014). Oral Radiology - E-Book: Principles and Interpretation. Elsevier Health Sciences. p. 527. ISBN 978-0-323-09634-8. Archived from the original on 29 August 2021. Retrieved 22 December 2019.
{{cite book}}: More than one of|accessdate=and|access-date=specified (help); More than one of|archivedate=and|archive-date=specified (help); More than one of|archiveurl=and|archive-url=specified (help) - ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Ram S, Siar CH, Ismail SM, Prepageran N (July 2004). "Pseudo bilateral tonsilloliths: a case report and review of the literature". Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 98 (1): 110–4. doi:10.1016/j.tripleo.2003.11.015. PMID 15243480.
- ↑ Textbook of Oral Radiology. Elsevier India. 2009. p. 607. ISBN 978-81-312-1148-9. Archived from the original on 29 August 2021. Retrieved 22 December 2019.
{{cite book}}: More than one of|accessdate=and|access-date=specified (help); More than one of|archivedate=and|archive-date=specified (help); More than one of|archiveurl=and|archive-url=specified (help) - ↑ Wong Chung, JERE; van Benthem, PPG; Blom, HM (May 2018). "Tonsillotomy versus tonsillectomy in adults suffering from tonsil-related afflictions: a systematic review". Acta Oto-Laryngologica. 138 (5): 492–501. doi:10.1080/00016489.2017.1412500. PMID 29241412.
- ↑ DeVault, Kenneth R.; Wallace, Michael B.; Aqel, Bashar A.; Lindor, Keith D. (2016). Practical Gastroenterology and Hepatology Board Review Toolkit. John Wiley & Sons. p. 59. ISBN 978-1-118-82907-3.
- ↑ Giudice M, Cristofaro MG, Fava MG, Giudice A (July 2005). "An unusual tonsillolithiasis in a patient with chronic obstructive sialoadenitis". Dentomaxillofac Radiol. 34 (4): 247–50. doi:10.1259/dmfr/19689789. PMID 15961601.
- ↑ 8.0 8.1 8.2 8.3 8.4 "Tonsil Stones (Tonsilloliths)". WebMD.com. Archived from the original on 4 September 2012. Retrieved 6 March 2016.
{{cite web}}: More than one of|archivedate=and|archive-date=specified (help); More than one of|archiveurl=and|archive-url=specified (help) - ↑ Stoodley, P; Debeer, D; Longwell, M; Nistico, L; Hall-Stoodley, L; Wenig, B; Krespi, YP (September 2009). "Tonsillolith: not just a stone but a living biofilm". Otolaryngology–Head and Neck Surgery. 141 (3): 316–21. doi:10.1016/j.otohns.2009.05.019. PMID 19716006.
- ↑ Padmanabhan TK, Chandra Dutt GS, Vasudevan DM, Vijayakumar (May–June 1984). "Giant tonsillolith simulating tumour of the tonsil – a case report". Indian J Cancer. 21 (2): 90–1. PMID 6530236.
- ↑ Silvestre-Donat F, Pla-Mocholi A, Estelles-Ferriol E, Martinez-Mihi V (2005). "Giant tonsillolith: report of a case" (PDF). Medicina Oral, Patología Oral y Cirugía Bucal. 10 (3): 239–42. PMID 15876967. Archived (PDF) from the original on 5 July 2017. Retrieved 17 April 2007.
{{cite journal}}: More than one of|accessdate=and|access-date=specified (help); More than one of|archivedate=and|archive-date=specified (help); More than one of|archiveurl=and|archive-url=specified (help) - ↑ "Images". Archived from the original on 3 December 2012. Retrieved 28 November 2007.
{{cite web}}: More than one of|archivedate=and|archive-date=specified (help); More than one of|archiveurl=and|archive-url=specified (help) - ↑ Darrow DH, Siemens C (August 2002). "Indications for tonsillectomy and adenoidectomy". Laryngoscope. 112 (8 Pt 2 Suppl 100): 6–10. doi:10.1002/lary.5541121404. PMID 12172229.
- ↑ S. G. Nour; Mafee, Mahmood F.; Valvassori, Galdino E.; Galdino E. Valbasson; Minerva Becker (2005). Imaging of the head and neck. Stuttgart: Thieme. p. 716. ISBN 1-58890-009-6.
External links
| Classification |
|---|


