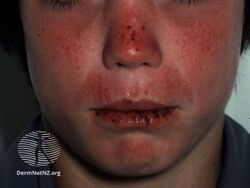
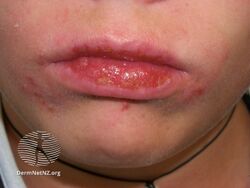
Actinic prurigo
| Actinic prurigo | |
|---|---|
 | |
| Membrane/cytoplasmic reaction of anti-CD117 in tissue with Actinic prurigo | |
| Specialty | Dermatology |
Actinic prurigo is a rare sunlight-induced, pruritic, papular or nodular skin eruption. Some medical experts use the term actinic prurigo to denote a rare photodermatosis that develops in childhood and is chronic and persistent; this rare photodermatosis, associated with the human leukocyte antigen HLA-DR4, is often called "Familial polymorphous light eruption of American Indians" or "Hereditary polymorphous light eruption of American Indians" but some experts consider it to be a variant of the syndrome known as polymorphous light eruption (PMLE).[1] Some experts use the term actinic prurigo for Hutchinson's summer prurigo[2] (aka hydroa aestivale) and several other photodermatoses that might, or might not, be distinct clinical entities.[3][4][5]
Signs and symptoms
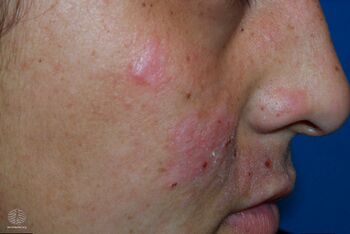
AP is characterized by itchy, inflamed papules, nodules, and plaques on the skin. Lesions typically appear hours or days after exposure of the skin to UV light, and follow a general pattern of sun-exposed areas. The face, neck, arms, hands, and legs are often affected, although lesions sometimes appear on skin that is covered by clothing and thus not exposed to UV light, thus making AP somewhat difficult to diagnose.
AP is a chronic disease, and symptoms usually worsen in the spring and summer as the day lengthens and exposure to sunlight increases.
Causes
The cause for actinic prurigo is unknown, however researchers believe that protein in our bodies may be a cause to the condition also: •UV-A and UV-B light seem to be the main provoking agents. This observation is supported by the fact that most patients live at high altitudes (>1000 m above sea level), and the condition improves in many patients when they move to lower altitudes. However, some patients who are affected already live at sea level.18,19,27 •Some authors are considering a food photosensitizer or a nutritional selective deficiency as a cause; however, no evidence proves this theory.27
Diagnosis
The diagnosis of Actinic prurigo is based on the following:[6]
- Medical history
- Physical exam
- Skin photo-testing
- Histologic evaluation
- Genetic test
Treatment
Currently there is no cure for actinic prurigo, and treatment focuses on relieving the dermatologic symptoms, by way of topical steroid creams or systemic immunosuppressants.
Prescribed treatments include:
- topical creams such as Tacrolimus and Betamethasone.
- systemic immunosuppressants such as Prednisone.
- In some cases, Thalidomide has proven to be effective in controlling the symptoms of actinic prurigo.
All patients with AP are encouraged to minimize sun exposure, and to use strong sunscreen throughout the year, and even on cloudy or overcast days, as UVA light, unlike UVB light, is able to penetrate cloud cover and remains constant throughout the day.
Alternative treatment methods might include UV Hardening, Meditation and/or cognitive behavioral therapy. UV-A desensitization phototherapy has also been shown to be effective in cases.
History
Actinic prurigo (AP) was first described by Escalona in Mexico, in 1954.
See also
- Photosensitivity with HIV infection
- List of human leukocyte antigen alleles associated with cutaneous conditions
- Hydroa vacciniforme
References
- ↑ Draelos, Zoe Kececioglu; Hansen, Ronald C. (November 1986). "Polymorphic Light Eruption in Pediatric Patients with American Indian Ancestry". Pediatric Dermatology. 3 (5): 384–389. doi:10.1111/j.1525-1470.1986.tb00546.x. PMID 3809022. S2CID 11347509.
- ↑ Hutchinson, Jonathan (1879). "Summer Prurigo". Lectures on Clinical Surgery. Vol. 1. J. & A. Churchill. pp. 130–131. Archived from the original on 2022-02-24. Retrieved 2021-01-23.
- ↑ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. p. 1336. ISBN 978-1-4160-2999-1.
- ↑ Lim, H. W.; Honigsmann, H.; Hawk, J. L., eds. (2007). Photodermatology. CRC Press. p. 149. ISBN 9781420019964.
- ↑ Lehmann, Percy; Schwarz, Thomas (4 March 2011). "Photodermatoses". Deutsches Ärzteblatt Online. 108 (9): 135–41. doi:10.3238/arztebl.2011.0135. PMC 3063367. PMID 21442060.
- ↑ Pile, Hannah D.; Crane, Jonathan S. (2022). "Actinic Prurigo". StatPearls. StatPearls Publishing. Archived from the original on 24 February 2022. Retrieved 23 February 2022.
External links
- http://dermnetnz.org/reactions/actinic-prurigo.html Archived 2016-07-20 at the Wayback Machine
- Actinic Prurigo at eMedicine
- Torres-Alvarez, B; Baranda, L; Fuentes, C; Delgado, C; Santos-Martinez, L; Portales-Perez, D; Moncada, B; Gonzalez-Amaro, R (January 1998). "An immunohistochemical study of UV-induced skin lesions in actinic prurigo. Resistance of langerhans cells to UV light". European Journal of Dermatology. 8 (1): 24–8. PMID 9649710. INIST:2157125.
- Polymorphous light eruption – Mayo Clinic Archived 2017-01-24 at the Wayback Machine