Alveolar hydatid disease
| Aveolar Hydatid Disease | |
|---|---|
| Other names: Alveolar echinococcosis Alveolar colloid of the liver, Alveolococcosis, Multilocular echinococcosis | |
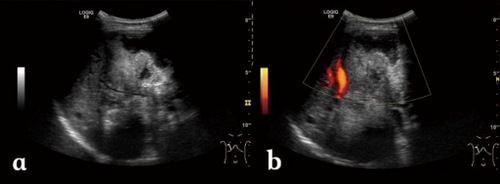 | |
| a) Irregular type heterogeneous mass lesion b)no obvious blood flow signal | |
| Causes | infection of larval stage Echinococcus multilocularis |
Alveolar hydatid disease (AHD), is a form of echinococcosis, or a disease that originates from a parasitic flatworm. AHD is caused by an infection of the flatworm species Echinococcus multilocularis.[1] Although alveolar echinococcosis is rarely diagnosed in humans and is not as widespread as cystic echinococcosis (caused by Echinococcus granulosus), it is also still a serious disease that has a significantly high fatality rate.[2] It is considered one of the most life-threatening helminthic infections humans can have.[2]
It is mostly popular in China, Eastern France, Switzerland, Austria, Bulgaria, Turkey, Iran, Japan, Afghanistan, and Russia, and is mostly confined to the Northern hemisphere, south to around the 40th or 45th degree of Northern latitude, save some cases reported in Northern Africa.[2][3][4][5][6]
Signs and symptoms
As the larvae grow in the liver, they create lesions.[2] If untreated, this progresses into abdominal mass and/or pain, jaundice, and finally liver failure.[7]
Cause
AHD is caused by the larval stage of E. mulitilocularis, a species of flatworm found in the Northern Hemisphere.[2] Humans make poor intermediate hosts for the worm, as they play no role in their life cycle.[5] However, when exposed the worms will still infect them. A major risk factor is when their domesticated dogs and cats eat wild, infected (typically arvicolid) rodents.[5][8][9] Their feces then will contain the worms' eggs, which have fully developed larval worms inside.[5] Humans become infected after eating food or water contaminated by embryonated eggs, or by handling an infected host like dogs and cats or by skinning infected foxes.[8][10]
Pathophysiology
Once ingested by humans, "the oncospheres hatch in the stomach or small intestine, become activated, penetrate the epithelial layer, and migrate via blood and lymphatic vessels to the visceral organs, primarily the liver, where they develop to another larval stage, the metacestode."[5] The larval growth resembles a slow-moving liver tumor and it is able to destroy both the liver parenchyma and its function.[2]
Diagnosis
Due to its infiltration into biliary and vascular liver tissue, it can be difficult to differentiate AHD and liver cancer.[2]
Management
Early detection and treatment and radical surgery is key to preventing fatality from AHD.[2] Treatment may include liver resection to remove the larvae and chemotherapy using benzimidazoles.[7] Chemotherapy must continue for many years, sometimes for the remainder of the patient's life.[11] Failure to comply with these expensive and difficult treatments will likely result in death for the patient.[7]
Prognosis
The disease is often progressive and destructive.[12] The growth happens slow, and so many people do not get symptoms until the later stages.[6] Central necrotic cavities are common in advanced stages of the disease.[13]
Epidemiology
AHD is not as common as diseases caused by other flatworms, but it is still prevalent in the Northern hemisphere. It is not uncommon in China, with some communities having a 5% or more infection rate.[14][15] In Europe, it is considered an emerging disease.[7] The increasing fox populations of Europe correlate with heightened reported cases.[16]
History
In 1855, Rudolf Virchow, the German pathologist, recognized that the disorder that was at the time known as colloid carcinoma of the liver, which was known for its tumor-like lesions in the liver, were actually caused by an Echinococcus species. For 100 year it was debated whether the species was E. granulosus or a different species. It was finally settled by two publications between 1954-1955, the former from Alaska and the latter from Germany.[5]
Society and culture
AHD is confined to the Northern hemisphere.[3] There are about 18,235 reported cases every year with 95% hailing from China.[17]
Research directions
Wildlife research is working to detect the parasite in new areas.[18]
References
- ↑ Wilson JF, Rausch RL, Wilson FR (March 1995). "Alveolar hydatid disease. Review of the surgical experience in 42 cases of active disease among Alaskan Eskimos". Annals of Surgery. 221 (3): 315–23. doi:10.1097/00000658-199503000-00015. PMC 1234575. PMID 7717785.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Malik AA, ul Bari S (2019). "Alveolar Hydatid Disease". In Malik AA, ul Bari S (eds.). Human Abdominal Hydatidosis. Singapore: Springer. pp. 63–72. doi:10.1007/978-981-13-2152-8_6. ISBN 978-981-13-2152-8.
- ↑ 3.0 3.1 Schantz PM (1988). "Echinococcosis (Hydatid Disease)". Laboratory Diagnosis of Infectious Diseases. New York, NY: Springer New York. pp. 836–849.
- ↑ Rausch RL, Wilson JF, Schantz PM (June 1990). "A programme to reduce the risk of infection by Echinococcus multilocularis: the use of praziquantel to control the cestode in a village in the hyperendemic region of Alaska". Annals of Tropical Medicine and Parasitology. 84 (3): 239–50. doi:10.1080/00034983.1990.11812463. PMID 2222026.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Ammann RW, Eckert J (1996-09-01). "CESTODES: Echinococcus". Gastroenterology Clinics of North America. 25 (3): 655–689. doi:10.1016/S0889-8553(05)70268-5. ISSN 0889-8553. PMID 8863045.
- ↑ 6.0 6.1 Bhatia JK, Ravikumar R, Naidu CS, Sethumadhavan T (December 2016). "Alveolar hydatid disease of the liver: A rare entity in India". Medical Journal, Armed Forces India. 72 (Suppl 1): S126–S129. doi:10.1016/j.mjafi.2015.12.005. PMC 5192168. PMID 28050091.
- ↑ 7.0 7.1 7.2 7.3 Torgerson PR, Keller K, Magnotta M, Ragland N (June 2010). "The global burden of alveolar echinococcosis". PLOS Neglected Tropical Diseases. 4 (6): e722. doi:10.1371/journal.pntd.0000722. PMC 2889826. PMID 20582310.
- ↑ 8.0 8.1 Kantarci M, Pirimoglu B, Kizrak Y (2014-03-28). "Diagnostic imaging and interventional procedures in a growing problem: Hepatic alveolar echinococcosis". World Journal of Surgical Procedures. 4 (1): 13–20. doi:10.5412/wjsp.v4.i1.13.
- ↑ Knapp J, Combes B, Umhang G, Aknouche S, Millon L (2016). "Could the domestic cat play a significant role in the transmission of Echinococcus multilocularis? A study based on qPCR analysis of cat feces in a rural area in France". Parasite. 23: 42. doi:10.1051/parasite/2016052. PMC 5782850. PMID 27739398.
- ↑ Morris DL, Richards KS (1992). Hydatid disease : current medical and surgical management. Oxford [England]: Butterworth-Heinemann. ISBN 0-7506-1379-3. OCLC 24538737. Archived from the original on 2021-11-15. Retrieved 2021-10-03.
- ↑ Torgerson PR, Schweiger A, Deplazes P, Pohar M, Reichen J, Ammann RW, et al. (July 2008). "Alveolar echinococcosis: from a deadly disease to a well-controlled infection. Relative survival and economic analysis in Switzerland over the last 35 years". Journal of Hepatology. 49 (1): 72–7. doi:10.1016/j.jhep.2008.03.023. PMID 18485517.
- ↑ Amir-Jahed AK, Fardin R, Farzad A, Bakshandeh K (November 1975). "Clinical echinococcosis". Annals of Surgery. 182 (5): 541–6. doi:10.1097/00000658-197511000-00001. PMC 1344034. PMID 1190858.
- ↑ Gottstein B (July 1992). "Molecular and immunological diagnosis of echinococcosis". Clinical Microbiology Reviews. 5 (3): 248–61. doi:10.1128/cmr.5.3.248. PMC 358243. PMID 1498767.
- ↑ Craig PS, Deshan L, MacPherson CN, Dazhong S, Reynolds D, Barnish G, et al. (October 1992). "A large focus of alveolar echinococcosis in central China". Lancet. 340 (8823): 826–31. doi:10.1016/0140-6736(92)92693-a. PMID 1357252. S2CID 31696615.
- ↑ Budke CM, Jiamin Q, Zinsstag J, Qian W, Torgerson PR (July 2004). "Use of disability adjusted life years in the estimation of the disease burden of echinococcosis for a high endemic region of the Tibetan plateau". The American Journal of Tropical Medicine and Hygiene. 71 (1): 56–64. doi:10.4269/ajtmh.2004.71.56. PMID 15238690.
- ↑ Schweiger A, Ammann RW, Candinas D, Clavien PA, Eckert J, Gottstein B, et al. (June 2007). "Human alveolar echinococcosis after fox population increase, Switzerland". Emerging Infectious Diseases. 13 (6): 878–82. doi:10.3201/eid1306.061074. PMC 2792858. PMID 17553227.
- ↑ Nunnari G, Pinzone MR, Gruttadauria S, Celesia BM, Madeddu G, Malaguarnera G, et al. (April 2012). "Hepatic echinococcosis: clinical and therapeutic aspects". World Journal of Gastroenterology. 18 (13): 1448–58. doi:10.3748/wjg.v18.i13.1448. PMC 3319940. PMID 22509076.
- ↑ Romig T, Dinkel A, Mackenstedt U (January 2006). "The present situation of echinococcosis in Europe". Parasitology International. 55 Suppl: S187-91. doi:10.1016/j.parint.2005.11.028. PMID 16352465.
External links
| Classification |
|---|