Yersiniosis
| Yersinia enterocolitica | |
|---|---|
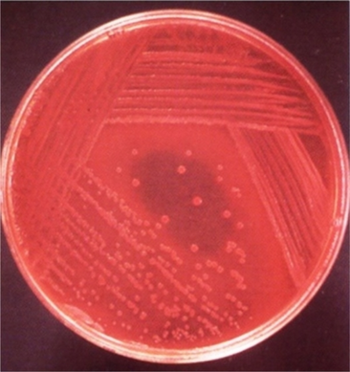 | |
| Colony of Yersinia enterocolitica on Cefsoludin-Irgasan-Novobiocin (CIN) agar | |
| Specialty | Infectious disease |
Yersiniosis is an infectious disease caused by a bacterium of the genus Yersinia.[1] In the United States, most yersiniosis infections among humans are caused by Yersinia enterocolitica.
Infection with Y. enterocolitica occurs most often in young children.[citation needed] The infection is thought to be contracted through the consumption of undercooked meat products, unpasteurized milk, or water contaminated by the bacteria. It has been also sometimes associated with handling raw chitterlings.[2][3]
Another bacterium of the same genus, Yersinia pestis, is the cause of Plague.
Signs and symptoms
Infection with Y. enterocolitica can cause a variety of symptoms depending on the age of the person infected. Common symptoms in children are fever, abdominal pain, and diarrhea, which is often bloody. Symptoms typically develop 4 to 7 days after exposure and may last 1 to 3 weeks or longer. In older children and adults, right-sided abdominal pain and fever may be the predominant symptoms, and may be confused with appendicitis. In a small proportion of cases, complications such as skin rash, joint pains, ileitis, erythema nodosum, and sometimes sepsis, acute arthritis[4] or the spread of bacteria to the bloodstream (bacteremia) can occur.
Cause
The etiology of Yersiniosis is Yersinia enterocolitica, humans are hosts who do not contribute to the pathogens life cycle [5] Most people become infected by eating contaminated food, especially raw or undercooked pork, or through contact with a person who has prepared a pork product, such as chitlins.[6] For example, babies and infants can be infected if their caretakers handle contaminated food and then do not wash their hands properly before handling the child or the child's toys, bottles, or pacifiers.[6] People occasionally become infected after drinking contaminated milk or untreated water, or after contact with infected animals or their feces.[6] On rare occasions, people become infected through person-to-person contact.[6] For example, caretakers can become infected if they do not wash their hands properly after changing the diaper of a child with yersiniosis.[6] Even more rarely, people may become infected through contaminated blood during a transfusion.[6]
Diagnosis
Phage typing of bacterial culture or antibodies for F-antigen.
Treatment
Treatment for gastroenteritis due to Y. enterocolitica is not needed in the majority of cases. Severe infections with systemic involvement (sepsis or bacteremia) often requires aggressive antibiotic therapy; the drugs of choice are doxycycline and an aminoglycoside. Alternatives include cefotaxime, fluoroquinolones, and co-trimoxazole.[7][8]
Prevalence
The Centers for Disease Control and Prevention estimates that infections with Yersinia enterocolitica cause almost 117,000 illnesses, 640 hospitalizations, and 35 deaths in the United States every year.[6] In 2011, there were 7,017 diagnosed cases of yersiniosis in the European Union.[1] This was a 3.5% increase compared to the prior year.[1] In 2011, there were 257 diagnosed cases of yersiniosis in Poland.[1] In 2012 in Poland, there was a drop to 231 reported yersiniosis cases.[1] Children are infected more often than adults, and the infection is more common in the winter.[6]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 Bancerz-Kisiel, Agata; Szweda, Wojciech (4 September 2015). "Yersiniosis – zoonotic foodborne disease of relevance to public health". Annals of Agricultural and Environmental Medicine. 22 (3): 397–402. doi:10.5604/12321966.1167700. PMID 26403101.
- ↑ Jones TF (August 2003). "From pig to pacifier: chitterling-associated yersiniosis outbreak among black infants". Emerging Infectious Diseases. 9 (8): 1007–9. doi:10.3201/eid0908.030103. PMC 3020614. PMID 12967503.
- ↑ Lee, LA.; Gerber, AR.; Lonsway, DR.; Smith, JD.; Carter, GP.; Puhr, ND.; Parrish, CM.; Sikes, RK.; Finton, RJ.; Tauxe, RV. (1990). " Yersinia enterocolitica O:3 infections in infants and children, associated with the household preparation of chitterlings". New England Journal of Medicine. 322 (14): 984–987. doi:10.1056/NEJM199004053221407. PMID 2314448.
- ↑ "Yersiniosis". Medical Dictionary. Archived from the original on 2018-12-21. Retrieved 2013-01-28.
- ↑ Aziz, Muhammad; Yelamanchili, Varun S. (2023). "Yersinia Enterocolitica". StatPearls. StatPearls Publishing. Archived from the original on 3 February 2023. Retrieved 28 April 2023.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 "Questions and Answers". Centers for Disease Control and Prevention. 1 August 2019. Archived from the original on 22 April 2023. Retrieved 30 April 2023.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ Torok E. Oxford MHandbook of Infect Dis and Microbiol, 2009
- ↑ Collins FM (1996). Baron S; et al. (eds.). Pasteurella, and Francisella. In: Barron's Medical Microbiology (4th ed.). Univ of Texas Medical Branch. ISBN 0-9631172-1-1. (via NCBI Bookshelf).
External links
| Classification | |
|---|---|
| External resources |