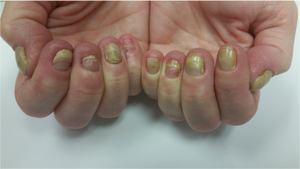
Yellow nail syndrome
| Yellow nail syndrome | |
|---|---|
| Other names: Primary lymphedema associated with yellow nails and pleural effusion | |
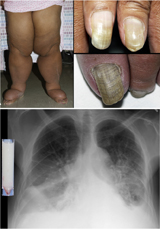 | |
| Yellow nail syndrome: This patient has a 20-year history of severe lymphedema of her legs; thick, ridged, yellowish, hypercurved thumbnails (top right); similarly affected, yellow-green to brown toenails (bottom right); and bilateral, chylous pleural effusions. A sample of her chylous pleural fluid is shown to the left of the radiograph. | |
| Causes | Unknown[1] |
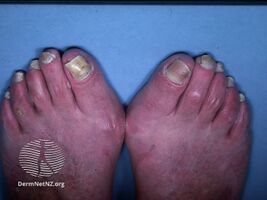
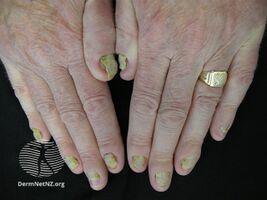
Yellow nail syndrome is a condition that presents with thick yellow nails, lymphedema, and lung disease; though these symptoms may not all occur at the same time.[2][3] Generally, two of the three features are required to make the diagnosis.[4] All the nails are generally affected and they do not grow.[5] Over half of cases have respiratory symptoms; the most common being cough and pleural effusion, and less frequently bronchiectasis, pneumonia, sinusitis, and lung fibrosis.[4] The lymphedema typically occurs in both legs, with or without pitting.[4]
The cause of yellow nail syndrome is uknown.[1] Diagnosis is generally not helped by lung function tests and lung biopsies.[4] When the lymphedema is associated with pitting and pleural effusion, a diagnosis of heart failure may be incorrectly made.[4]
It is a very rare medical syndrome.[6] Approximately 40% will also have bronchiectasis. It usually affects adults.[7][5][8] The condition was first reported by Heller in 1927 and the first case series was described in a publication in 1964 by London physicians Peter Samman and William White.[3][9][4]
Signs and symptoms
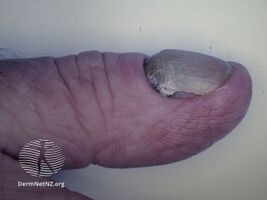
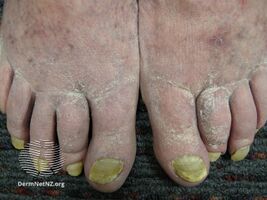
The nails are markedly thickened with yellow to yellow-green discoloration of the nails.[2][10] They grow slowly, at a rate of 0.25 mm/week or less. The nails may have ridges and increased side-to-side curvature, reduction of the white crescent and detachment of the nail from the nailbed.[8] These nail abnormalities may also change over time.[8]
Most people with yellow nail syndrome (four fifths) have lymphedema; it is symmetrical and typically affects both legs. It is the first symptom of the condition in about a third. Involvement of the arms and face is more unusual, as is lymphedema of the abdomen with ascites (fluid collection in the abdominal cavity) and fluid collection around the heart.[8]
Various lung problems can occur in people with yellow nail syndrome. Many experience cough and shortness of breath. Forty percent of cases develop pleural effusions, which are collections of fluid in the pleural cavity (the space that contains the lungs and normally only has a minimal amount of fluid in it).[8] About half of all people with yellow nail syndrome have either recurrent chest infections or a chronic lung condition known as bronchiectasis which causes chronic production of sputum with episodes of worsening. Forty percent of people with yellow nail syndrome have chronic sinusitis.[8]
Yellow nail syndrome has been associated with some drugs, e.g. penicillamine, bucillamine and gold sodium thiomalate.[11]
It has also been associated with exposure to titanium from dental implants.[12]
-
Yellow nail syndrome
-
Yellow nail syndrome
-
Yellow nail syndrome
-
Yellow nail syndrome
-
Yellow nail syndrome
-
Yellow nail syndrome
-
Yellow nail syndrome
Genetics
Although it has been described in families, it has been suggested that it might not have a genetic link.[13]
Diagnosis
The diagnosis is based on the combination of the symptoms. Generally, people are diagnosed with yellow nail syndrome if they have two or three of the three classical symptoms (yellow nails, lymphedema and pleural effusion). The nail changes are considered essential for the diagnosis, but they can be subtle.[8]
Pulmonary function testing can show obstruction of the airways. People with pleural effusions may show evidence of restriction in lung volumes due to the fluid. Analysis of the fluid in pleural effusions generally shows high levels of protein but low levels of cholesterol and lactate dehydrogenase, but about 30% of effusions are chylous (chylothorax) in that they have the characteristics of lymph.[8]
A lymphogram may be performed in people with lymphedema. This can show both under developed (hypoplastic) lymphatic ducts and dilated ducts. Dye may be found in the skin months after the initial test. Scintigraphy of lymph flow (lymphoscintigraphy) shows delays in drainage of lymph (sometimes asymmetrically), although this test can also be normal.[8]
Treatment
Normal treatment for swelling and any respiratory problems is appropriate. Nutritional supplementation with Vitamin E in some studies has been shown to be effective in controlling nail changes.[7]
Prognosis
People with yellow nail syndrome have been found to have a moderately reduced lifespan compared to people without the condition.[8]
Epidemiology
The condition is thought to be rare, with approximately 150 cases described in the medical literature.[8]
History
The condition was first described in 1964 by London physicians Peter Samman and William White.[14] Earlier cases may have been recorded in 1927 and 1962.[8]
References
- ↑ 1.0 1.1 Tosti, Antonella (2020). "413. Diseases of hair and nails". In Goldman, Lee; Schafer, Andrew I. (eds.). Goldman-Cecil Medicine. Vol. 2 (26th ed.). Philadelphia: Elsevier. pp. 2661–2662. ISBN 978-0-323-53266-2. Archived from the original on 2023-07-01. Retrieved 2023-05-31.
- ↑ 2.0 2.1 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "33. Diseases of the skin appendages". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 790. ISBN 978-0-323-54753-6. Archived from the original on 2023-06-30. Retrieved 2024-01-19.
- ↑ 3.0 3.1 Baran, Robert L.; Vignes, Stefane (2021). "1. Yellow Nail Syndrome". In Baran, Robert L. (ed.). Advances in Nail Disease and Management. Switzerland: Springer. pp. 1–4. ISBN 978-3-030-59996-6. Archived from the original on 2023-07-02. Retrieved 2023-05-14.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Cheslock, Megan; Harrington, Douglas W. (2023). "Yellow Nail Syndrome". StatPearls. StatPearls Publishing. Archived from the original on 2023-07-05. Retrieved 2024-01-19.
- ↑ 5.0 5.1 Saavedra, Arturo; Roh, Ellen K.; Mikailov, Anar (2023). "32.Disorders of the nail apparatus". Fitzpatrick's Color Atlas and Synopsis of Clinical Dermatology (9th ed.). New York: McGraw Hill Professional. pp. 849–872. ISBN 978-1-264-27801-5. Archived from the original on 2023-12-31. Retrieved 2024-01-18.
- ↑ "Yellow nail syndrome | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program". rarediseases.info.nih.gov. Archived from the original on 2018-04-18. Retrieved 2018-04-17.
- ↑ 7.0 7.1 "Yellow nail syndrome. DermNet NZ". Archived from the original on 2013-11-15. Retrieved 2008-03-19.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 8.11 Maldonado, Fabien; Ryu, Jay H (July 2009). "Yellow nail syndrome". Current Opinion in Pulmonary Medicine. 15 (4): 371–375. doi:10.1097/MCP.0b013e32832ad45a. PMID 19373089.
- ↑ Samman, PD; White, WF (April 1964). "The "yellow nail" syndrome". The British Journal of Dermatology. 76 (4): 153–7. doi:10.1111/j.1365-2133.1964.tb14499.x. PMID 14140738. S2CID 35463634.
- ↑ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. p. 1020. ISBN 978-1-4160-2999-1.
- ↑ Nanda S; Dorville F (2009). "Yellow nail syndrome". Canadian Medical Association Journal. 181 (9): 614. doi:10.1503/cmaj.080255. PMC 2764757. PMID 19770240.
- ↑ Berglund, F; Carlmark, B (2010). "Titanium, Sinusitis, and the Yellow Nail Syndrome". Biological Trace Element Research. 143 (1): 1–7. doi:10.1007/s12011-010-8828-5. PMC 3176400. PMID 20809268.
- ↑ Hoque SR, Mansour S, Mortimer PS (June 2007). "Yellow nail syndrome: not a genetic disorder? Eleven new cases and a review of the literature". Br. J. Dermatol. 156 (6): 1230–4. doi:10.1111/j.1365-2133.2007.07894.x. PMID 17459037.
- ↑ Samman, PD; White, WF (April 1964). "The "yellow nail" syndrome". The British Journal of Dermatology. 76 (4): 153–7. doi:10.1111/j.1365-2133.1964.tb14499.x. PMID 14140738.
External links
| Classification | |
|---|---|
| External resources |