Video:Hypertension
| Hypertension (Tutorial) | |
|---|---|
| On Commons | |
| Steps for video creation | |
| Step 1 | Preview my changes (10 sec) |
| Step 2 | Upload to Commons (10 min) |
Overview
Hypertension, also known as high blood pressure, is a long-term medical condition where the blood pressure in the arteries is chronically elevated.[1]

Epidemiology
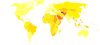
High blood pressure is very common, and affects between 16 and 37% of the population. [2] In 2010, it was a factor in 9.4 million deaths globally.[3]

Symptoms and risks
High blood pressure typically does not cause symptoms,[4] but is a major risk factor for many life threatening conditions, including coronary artery disease, stroke, heart failure, atrial fibrillation, peripheral vascular disease, vision loss, chronic kidney disease, and dementia.[5][6][7][8]

Classification
High blood pressure is classified as either primary, or secondary hypertension.[2] Primary high blood pressure is also known as essential hypertension.

Causes
Roughly 90 to 95% of people with high blood pressure, have the primary type. This is high blood pressure caused by nonspecific lifestyle, and genetic factors.[2][9]

Most common causes
Lifestyle factors that increase the risk of primary hypertension include smoking, being overweight, too much salt in the diet, and excessive alcohol use.[4][2]

Less common causes
The remaining 5 to 10% of cases are secondary hypertension, where an identifiable cause can be found, such as the use of birth control pills, chronic kidney disease, narrowing of the arteries to the kidneys, or an endocrine disorder like hyperthyroidism.[2]

Diagnosis
Blood pressure is expressed by two measurements. The systolic number, which is the maximum pressure, and the diastolic number, which is the minimum pressure.[4]

Typical reading
For instance, a blood pressure of 120 over 70 would be normal, in most people when they are at rest. [10]

Normal values
For most adults, when they are resting, a normal maximum (or systolic) blood pressure is between 100 and 130 mmHg, and the minimum (or diastolic) pressure is between 60 and 80 mmHg.[11]

High blood pressure values
A high blood pressure is present when the resting blood pressure is persistently at, or above, 130 over 80, or 140 over 90 mmHg.[2][11] It is important to realize, children have much different numbers that depend on their age, and size.[12]

Ambulatory blood pressure monitoring
Measuring the blood pressure outside of an office, over a 24 hour period, appears to be more accurate than office-based blood pressure measurement.[2][1]
Pregnancy
Hypertension occurs in approximately 8 to 10% of pregnancies.[13] This is called gestational hypertension. Two blood pressure measurements, six hours apart, of greater than 140 over 90 mmHg, are diagnostic of hypertension in pregnancy, and should be immediately addressed.[14]

Treatment of moderate hypertension
Research is clear that the treatment of moderately high blood pressure (defined as more than 160 over 100 mmHg), is associated with an improved life expectancy.[15]

Low to moderate blood pressure
The research is less clear on the effect of treatment of blood pressure between the ranges of 130 and 160 mmHg systolic, and 80 to 100 mmHg diastolic. Some reviews find benefit,[11][16][17] and others do not.[18][19][20]

Effect of lifestyle
Lifestyle changes and medications can lower blood pressure, and decrease the risk of health complications.[21]

Lifestyle changes
Lifestyle changes include weight loss, physical exercise, decreased salt intake, reducing alcohol intake, and a healthy diet.[2]

Treatment with medication
If lifestyle changes are not sufficient, then blood pressure medications are used.[21] Up to three different medications can control hypertension, in 90% of people.[2]

References
- ↑ 1.0 1.1 Naish, Jeannette; Court, Denise Syndercombe (2014). Medical sciences (2 ed.). p. 562. ISBN 9780702052491.
{{cite book}}: CS1 maint: url-status (link) - ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Poulter, NR; Prabhakaran, D; Caulfield, M (22 August 2015). "Hypertension". Lancet. 386 (9995): 801–12. doi:10.1016/s0140-6736(14)61468-9. PMID 25832858.
- ↑ Campbell, NR; Lackland, DT; Lisheng, L; Niebylski, ML; Nilsson, PM; Zhang, XH (March 2015). "Using the Global Burden of Disease study to assist development of nation-specific fact sheets to promote prevention and control of hypertension and reduction in dietary salt: a resource from the World Hypertension League". Journal of Clinical Hypertension (Greenwich, Conn.). 17 (3): 165–67. doi:10.1111/jch.12479. PMID 25644474.
- ↑ 4.0 4.1 4.2 "High Blood Pressure Fact Sheet". CDC. 19 February 2015. Archived from the original on 6 March 2016. Retrieved 6 March 2016.
- ↑ Lackland, DT; Weber, MA (May 2015). "Global burden of cardiovascular disease and stroke: hypertension at the core". The Canadian Journal of Cardiology. 31 (5): 569–71. doi:10.1016/j.cjca.2015.01.009. PMID 25795106.
- ↑ Mendis, Shanthi; Puska, Pekka; Norrving, Bo (2011). Global atlas on cardiovascular disease prevention and control (PDF) (1st ed.). Geneva: World Health Organization in collaboration with the World Heart Federation and the World Stroke Organization. p. 38. ISBN 9789241564373. Archived (PDF) from the original on 17 August 2014.
- ↑ Hernandorena, I; Duron, E; Vidal, JS; Hanon, O (July 2017). "Treatment options and considerations for hypertensive patients to prevent dementia". Expert Opinion on Pharmacotherapy (Review). 18 (10): 989–1000. doi:10.1080/14656566.2017.1333599. PMID 28532183.
- ↑ Lau, DH; Nattel, S; Kalman, JM; Sanders, P (August 2017). "Modifiable Risk Factors and Atrial Fibrillation". Circulation (Review). 136 (6): 583–96. doi:10.1161/CIRCULATIONAHA.116.023163. PMID 28784826.
- ↑ Carretero OA, Oparil S; Oparil (January 2000). "Essential hypertension. Part I: definition and etiology". Circulation. 101 (3): 329–35. doi:10.1161/01.CIR.101.3.329. PMID 10645931. Archived from the original on 12 February 2012.
- ↑ Giuseppe, Mancia; Fagard, R; Narkiewicz, K; Redon, J; Zanchetti, A; Bohm, M; Christiaens, T; Cifkova, R; De Backer, G; Dominiczak, A; Galderisi, M; Grobbee, DE; Jaarsma, T; Kirchhof, P; Kjeldsen, SE; Laurent, S; Manolis, AJ; Nilsson, PM; Ruilope, LM; Schmieder, RE; Sirnes, PA; Sleight, P; Viigimaa, M; Waeber, B; Zannad, F; Redon, J; Dominiczak, A; Narkiewicz, K; Nilsson, PM; et al. (July 2013). "2013 ESH/ESC Guidelines for the management of arterial hypertension: The Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC)". European Heart Journal. 34 (28): 2159–219. doi:10.1093/eurheartj/eht151. PMID 23771844.
- ↑ 11.0 11.1 11.2 Paul Whelton; et al. (13 November 2017). "2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults" (PDF). Hypertension. 71 (6): e13–e115. doi:10.1161/HYP.0000000000000065. PMID 29133356.
- ↑ James, PA.; Oparil, S.; Carter, BL.; Cushman, WC.; Dennison-Himmelfarb, C.; Handler, J.; Lackland, DT.; Lefevre, ML.; et al. (Dec 2013). "2014 Evidence-Based Guideline for the Management of High Blood Pressure in Adults: Report From the Panel Members Appointed to the Eighth Joint National Committee (JNC 8)". JAMA. 311 (5): 507–20. doi:10.1001/jama.2013.284427. PMID 24352797.
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedABC - ↑ Harrison's principles of internal medicine (18th ed.). New York: McGraw-Hill. 2011. pp. 55–61. ISBN 9780071748896.
- ↑ Musini, VM; Tejani, AM; Bassett, K; Wright, JM (7 October 2009). "Pharmacotherapy for hypertension in the elderly". The Cochrane Database of Systematic Reviews (4): CD000028. doi:10.1002/14651858.CD000028.pub2. PMID 19821263.
- ↑ Sundström, Johan; Arima, Hisatomi; Jackson, Rod; Turnbull, Fiona; Rahimi, Kazem; Chalmers, John; Woodward, Mark; Neal, Bruce (February 2015). "Effects of Blood Pressure Reduction in Mild Hypertension". Annals of Internal Medicine. 162 (3): 184–91. doi:10.7326/M14-0773. PMID 25531552.
- ↑ Xie, X; Atkins, E; Lv, J; Bennett, A; Neal, B; Ninomiya, T; Woodward, M; MacMahon, S; Turnbull, F; Hillis, GS; Chalmers, J; Mant, J; Salam, A; Rahimi, K; Perkovic, V; Rodgers, A (30 January 2016). "Effects of intensive blood pressure lowering on cardiovascular and renal outcomes: updated systematic review and meta-analysis". Lancet. 387 (10017): 435–43. doi:10.1016/S0140-6736(15)00805-3. PMID 26559744.
- ↑ Diao, D; Wright, JM; Cundiff, DK; Gueyffier, F (Aug 15, 2012). "Pharmacotherapy for mild hypertension". The Cochrane Database of Systematic Reviews. 8 (8): CD006742. doi:10.1002/14651858.CD006742.pub2. PMID 22895954.
- ↑ Garrison, SR; Kolber, MR; Korownyk, CS; McCracken, RK; Heran, BS; Allan, GM (8 August 2017). "Blood pressure targets for hypertension in older adults". The Cochrane Database of Systematic Reviews. 8: CD011575. doi:10.1002/14651858.CD011575.pub2. PMID 28787537.
- ↑ Musini, VM; Gueyffier, F; Puil, L; Salzwedel, DM; Wright, JM (16 August 2017). "Pharmacotherapy for hypertension in adults aged 18 to 59 years". The Cochrane Database of Systematic Reviews. 8: CD008276. doi:10.1002/14651858.CD008276.pub2. PMID 28813123.
- ↑ 21.0 21.1 "How Is High Blood Pressure Treated?". National Heart, Lung, and Blood Institute. 10 September 2015. Archived from the original on 6 April 2016. Retrieved 6 March 2016.