Transient global amnesia
| Transient global amnesia | |
|---|---|
 | |
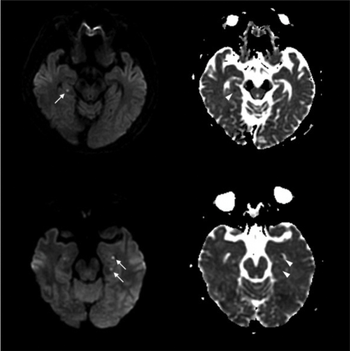
| Abnormal hippocampus findings consistent with transient global amnesia on MRI | |
| Specialty | Neurology |
| Usual onset | Sudden[1] |
| Duration | Up to 24 hrs[1] |
| Causes | Unknown[1] |
| Risk factors | Migraines, family history[1] |
| Diagnostic method | Based on symptoms after ruling out other possible causes[1][2] |
| Differential diagnosis | Toxins, stroke, seizure, migraine, concussion, encephalitis[1] |
| Treatment | Observation[1] |
| Prognosis | Good[1] |
| Frequency | 7 per 100,000 per year[1] |
Transient global amnesia (TGA) is a condition of sudden onset, were people are unable to form new memories.[1] There may also be problems remembering recent past memories.[1] No other signs of neurological problems are generally present and the condition lasts less than 24 hours.[1]
The cause is unclear.[1] Risk factors include a history of migraines and a family history.[1] Triggers may include emotional or physical stress.[1] Diagnosis is based on symptoms after ruling out other potential causes including: stroke, epilepsy, encephalitis, migraine, and concussion.[1][3][2]
Treatment generally involves observation with repeated examinations until the ability to form new memories returns.[1] Though the period of memory loss generally does not return.[1] Outcomes are good; however, up to 5% of people may have another episode within a year.[1]
Transient global amnesia affects about 7 per 100,000 people a year.[1] It most commonly occurs in those over the age of 50.[1] Males and females are affected with similar frequency.[1] It was first clearly described in the 1950s.[1]
Signs and symptoms
A person having TGA has almost no capacity to establish new memories, but generally appears otherwise mentally alert and normal, possessing full knowledge of self-identity and identity of close family, and maintaining intact perceptual skills and a wide repertoire of complex learned behavior. The individual simply cannot recall anything since the onset that happened outside the last few minutes, while memory for more temporally distant events may be largely intact.[4][5] The degree of amnesia is profound, and, in the interval during which the individual is aware of his or her condition, is often accompanied by anxiety.[6]
The diagnostic criteria include:[5]
- The attack was witnessed by a capable observer and reported as being a definite loss of recent memory (anterograde amnesia).
- There was an absence of clouding of consciousness or other cognitive impairment other than amnesia.
- There were no focal neurological signs or deficits during or after the attack.
- There were no features off epilepsy, or active epilepsy in the past two years, and the patient did not have any recent head injury.
- The attack resolved within 24 hours.
Often people repeatedly ask the same question, despite having the question answered.[1]
Progression
This onset of TGA is generally fairly rapid, and its duration varies but generally lasts between 2 and 8 hours.[5] A person experiencing TGA typically has memory only of the past few minutes or less, and cannot retain new information beyond that period of time. One of its bizarre features is perseveration, in which the victim of an attack faithfully and methodically repeats statements or questions, complete with profoundly identical intonation and gestures "as if a fragment of a sound track is being repeatedly rerun."[7] This is found in almost all TGA attacks and is sometimes considered a defining characteristic of the condition.[5][8][9] The individual experiencing TGA retains social skills and older significant memories, almost always including knowing his or her own identity and the identity of family members, and the ability to perform various complex learned tasks including driving and other learned behavior; one individual "was able to continue putting together the alternator of his car."[5] Though outwardly appearing to be normal, a person with TGA is disoriented in time and space, perhaps knowing neither the year nor where they reside. Although confusion is sometimes reported, others consider this an imprecise observation,[9] but an elevated emotional state (compared to patients experiencing Transient Ischemic Attack, or TIA) is common.[10] In a large survey, 11% of individuals in a TGA state were described as exhibiting "emotionalism" and 14% "fear of dying".[11] The attack lessens over a period of hours, with older memories returning first, and the repetitive fugue slowly lengthening so that the victim retains short-term memory for longer periods. While seemingly back to normal within 24 hours, there are subtle effects on memory that can persist longer.[12][13] In the majority of cases there are no long-term effects other than a complete lack of recall for this period of the attack and an hour or two before its onset.[5][14] There is emerging evidence for observable impairments in a minority of cases weeks or even years following a TGA attack.[12][15][16]
There is also evidence that the victim is aware that something is not quite right, even though they can't pinpoint it. Persons suffering from the attack may vocalize signs that 'they just lost their memory', or that they believed they had a stroke, although they aren't aware of the other signs that they are displaying. The main sign of this condition is the repetitive actions of something that is not usually repeated.[citation needed]
Causes
The underlying cause of TGA remains unclear.[1]
The leading hypotheses are some form of epileptic event, a problem with blood circulation around, to or from the brain, or some kind of migraine-like phenomenon.[10][17][18][19] The differences are sufficiently meaningful that transient amnesia may be considered a heterogeneous clinical syndrome[5] with multiple etiologies, corresponding mechanisms, and differing prognoses.[11]
Precipitating events
TGA attacks are associated with some form of precipitating event in at least one-third of cases.[20] The most commonly cited precipitating events include vigorous exercise (including sexual intercourse), swimming in cold water or enduring other temperature changes, and emotionally traumatic or stressful events.[5] There are reports of TGA-like conditions following certain medical procedures and disease states.[18] One study reports two cases of familial incidence (in which two members of the same family experienced TGA), out of 114 cases considered.[5] This indicates the possibility that there could be a slight familial incidence.
If the definition of a precipitating event is widened to include events days or weeks earlier, and to take in emotionally stressful burdens such as money worries, attending a funeral or exhaustion due to overwork or unusual childcare responsibilities, a large majority, over 80%, of TGA attacks are said to correlate with precipitating events.[11]
The role of psychological co-factors has been addressed by some research. It is the case that people in a state of TGA exhibit measurably elevated levels of anxiety and/or depression.[6] Emotional instability may leave some people vulnerable to stressful triggers and thus be associated with TGA.[11] Individuals who have experienced TGA, compared with similar people with TIA, are more likely to have some kind of emotional problem (such as depression or phobias) in their personal or family history[21] or to have experienced some kind of phobic or emotionally challenging precipitating event.[22]
Vascular hypotheses
Cerebral ischemia is a frequently disputed possible cause, at least for some segment of the TGA population, and until the 1990s it was generally thought that TGA was a variant of transient ischemic attack (TIA) secondary to some form of cerebrovascular disease.[10][19] Those who argue against a vascular cause point to evidence that those experiencing TGA are no more likely than the general population to have subsequent cerebral vascular disease.[10] In fact, "in comparison with TIA patients, TGA patients had a significantly lower risk of combined stroke, myocardial infarct, and death."[21]
Other vascular origins remain a possibility, however, according to research of jugular vein valve insufficiency in patients with TGA. In these cases TGA has followed vigorous exertion. One current hypothesis is that TGA may be due to venous congestion of the brain,[23] leading to ischemia of structures involved with memory, such as the hippocampus.[24] It has been shown that performing a Valsalva maneuver (involving "bearing down" and increasing breath pressure against a closed glottis, which occurs frequently during exertion) may be related to retrograde flow of blood in the jugular vein, and therefore, presumably, cerebral blood circulation, in patients with TGA.[23][25][26][27][28]
Migraine
A history of migraine is a statistically significant risk factor identified in the medical literature.[10][11] "When comparing TGA patients with normal control subjects… the only factor significantly associated with an increased risk for TGA was migraine."[19] Fourteen percent of people with TGA had a history of migraine in one study,[20] and approximately a third of the participants in another clinical study reported such a history.[5]
However, migraine does not appear to occur simultaneously with TGA nor serve as a precipitating event. Headache frequently occurs during TGA, as does nausea, both symptoms often associated with migraine, but it appears that these do not indicate migraine in patients during a TGA event. The connection remains conceptual, and muddied further by a lack of consensus about the definition of migraine itself, and by the differences in age, gender, and psychological characteristics of migraine sufferers when compared to those variables in the TGA cohort.[11]
Epilepsy
Amnesia is often a symptom in epilepsy, and for that reason people with known epilepsy are disqualified from most studies of TGA. In a study where strict criteria were applied to TGA diagnosis, no epileptic features were seen in EEGs of over 100 patients with TGA.[11] However, despite the fact that EEG readings are usually normal during a TGA attack, and other usual symptoms of epilepsy are not observed with TGA,[19] it has been speculated that some initial epileptic attacks present as TGA.[5] The observation that 7% of people who experience TGA will develop epilepsy calls into question whether those case are, in fact, TGA or transient epileptic amnesia (TEA).[10] TEA attacks tend to be short (under one hour) and tend to recur, so that a person who has experienced both repeated attacks of temporary amnesia resembling TGA and if those events lasted less than one hour is very likely to develop epilepsy.[5]
There is additional speculation that atypical cases of TEA in the form of nonconvulsive status epilepticus may present with duration similar to TGA.[29] This may constitute a distinct subgroup of TGA. TEA, as opposed to "pure" TGA, is also characterized by "two unusual forms of memory deficit …: (i) accelerated long-term forgetting (ALF): the excessively rapid loss of newly acquired memories over a period of days or weeks and (ii) remote autobiographical memory loss: a loss of memories for salient, personally experienced events of the past few decades."[8]
Whether an amnestic event is TGA or TEA thus presents a diagnostic challenge,[18] especially in light of the recently published descriptions of possible long-term cognitive deficits with (presumably correctly diagnosed) TGA.
Other associations
There have been assertions of a possible link between TGA and the use of statins (a class of drug used in treating cholesterol).[30][31] En bloc memory loss which is total, permanent, and irrecoverable can occur as an alcoholic "black out," usually lasting longer than an hour and up to 2–5 days. Marijuana intoxication, Halogenated hydroxyquinolines such as Clioquinol, PDE inhibitors such as sildenafil, Digitalis and scopolamine intoxication, and general anaesthesia have been reported with TGA.
Diagnosis
Unless there are concerning features, limited testing is required.[1] Medical imaging and lumbar puncture are generally not required.[1]
Differential diagnosis
A differential diagnosis should include:[32]
- Stroke (basilar artery, posterior cerebral artery, Lacunar syndromes)
- Complex partial seizures (temporal lobe epilepsy, frontal lobe epilepsy)
- Migraine variants
- Encephalopathy including Wernicke encephalopathy[3]
- Syncope and related paroxysmal spells
If the event lasts less than one hour, transient epileptic amnesia (TEA) might be implicated.[5][33]
If the condition lasts longer than 24 hours, it is not considered TGA by definition. A diagnostic investigation would then probably focus on some form of undetected ischemic attack or cranial bleed.[34][35]
Both TGA and anterograde amnesia deal with disruptions of short-term memory. However, a TGA episode generally lasts no more than 2 to 8 hours before people returns to normal with the ability to form new memories. A person with anterograde amnesia may not be able to form new memories indefinitely.[5]
Treatment
Treatment involves observing the individual until they are back to normal.[1] As those with ongoing memory problems do not have capacity to leave against medical advise, they may be held against their wises.[1]
Prognosis
The prognosis of "pure" TGA is very good. It does not affect mortality or morbidity[32] and unlike earlier understanding of the condition, TGA is not a risk factor for stroke or ischemic disease.[10] Rates of recurrence are variously reported, with one systematic calculation suggesting the rate is under 6% per year.[21] TGA "is universally felt to be a benign condition which requires no further treatment other than reassurance to the patient and his or her family."[34] "The most important part of management after diagnosis is looking after the psychological needs of the patient and his or her relatives. Seeing a once competent and healthy partner, sibling or parent become incapable of remembering what was said only a minute ago is very distressing, and hence it is often the relatives who will require reassurance."[36]
TGA may have multiple etiologies and prognoses.[11] Atypical presentations may masquerade as epilepsy[10] and be more properly considered TEA. In addition to such probable TEA cases, some people experiencing amnestic events diverging from the diagnostic criteria articulated above may have a less benign prognosis than those with "pure" TGA.[5]
Recently, moreover, both imaging and neurocognitive testing studies question whether TGA is as benign as has been thought. MRI scans of the brain in one study showed that among people who had experienced TGA, all had cavities in the hippocampus, and these cavities were far more numerous, larger, and more suggestive of pathological damage than in either healthy controls or a large control group of people with tumor or stroke.[15] Verbal and cognitive impairments have been observed days after TGA attacks, of such severity that the researchers estimated the effects would be unlikely to resolve within a short time frame.[16] A large neurocognitive study of patients more than a year after their attack has shown persistent effects consistent with amnestic mild cognitive impairment (MCI-a) in a third of the people who had experienced TGA.[37] In another study, "selective cognitive dysfunctions after the clinical recovery" were observed, suggesting a prefrontal impairment.[13] These dysfunctions may not be in memory per se but in retrieval, in which speed of access is part of the problem among people who have had TGA and experience ongoing memory problems.[12]
Epidemiology
The estimated annual incidence of TGA varies from a minimum of 2.9 cases per 100,000 population (in Spain) and 5.2 per 100,000 (in the US),[32] but among people aged over 50, the rate of TGA incidence is reported to range from approximately 23 per 100,000 (in a US population) to 32 per 100,000 (in a population in Scandinavia).[20][38]
TGA is most common in people between age 56 and 75,[11] with the average age of a person experiencing TGA being approximately 62.[10]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 Faust, JS; Nemes, A (August 2016). "Transient Global Amnesia: Emergency Department Evaluation And Management". Emergency medicine practice. 18 (8): 1–20. PMID 27416582. Archived from the original on 2021-09-23. Retrieved 2021-09-18.
- ↑ 2.0 2.1 Arena, JE; Rabinstein, AA (February 2015). "Transient global amnesia". Mayo Clinic proceedings. 90 (2): 264–72. doi:10.1016/j.mayocp.2014.12.001. PMID 25659242.
- ↑ 3.0 3.1 Nehring, SM; Spurling, BC; Kumar, A (January 2021). "Transient Global Amnesia". PMID 28723030.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Logan, W; Sherman, D (1983). "Transient global amnesia". Stroke. 14 (6): 1005–7. doi:10.1161/01.STR.14.6.1005. PMID 6658982.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 Hodges; Warlow, CP (1990). "Syndromes of transient amnesia: towards a classification. A study of 153 cases". Journal of Neurology, Neurosurgery, and Psychiatry. 53 (10): 834–43. doi:10.1136/jnnp.53.10.834. PMC 488242. PMID 2266362.
- ↑ 6.0 6.1 Noel, A.; Quinette, P.; Guillery-Girard, B.; Dayan, J.; Piolino, P.; Marquis, S.; De La Sayette, V.; Viader, F.; et al. (2008). "Psychopathological factors, memory disorders and transient global amnesia". The British Journal of Psychiatry. 193 (2): 145–51. doi:10.1192/bjp.bp.107.045716. PMID 18670000.
- ↑ Frederiks, J (1993). "Transient global amnesia". Clinical Neurology and Neurosurgery. 95 (4): 265–83. doi:10.1016/0303-8467(93)90102-M. PMID 8299284. Archived from the original on 2021-09-23. Retrieved 2021-09-18.
- ↑ 8.0 8.1 Butler, C. R.; Zeman, A. Z. (2008). "Recent insights into the impairment of memory in epilepsy: transient epileptic amnesia, accelerated long-term forgetting and remote memory impairment". Brain. 131 (Pt 9): 2243–63. doi:10.1093/brain/awn127. PMID 18669495.
- ↑ 9.0 9.1 Owen, D; Paranandi, B; Sivakumar, R; Seevaratnam, M (2007). "Classical diseases revisited: transient global amnesia". Postgraduate Medical Journal. 83 (978): 236–9. doi:10.1136/pgmj.2006.052472. PMC 2600033. PMID 17403949.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 10.7 10.8 Hodges, John R.; Warlow, Charles P. (1990). "The Aetiology of Transient Global Amnesia". Brain. 113 (3): 639–57. CiteSeerX 10.1.1.1009.4172. doi:10.1093/brain/113.3.639. PMID 2194627.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 Quinette, P.; Guillery-Girard, B; Dayan, J; De La Sayette, V; Marquis, S; Viader, F; Desgranges, B; Eustache, F (2006). "What does transient global amnesia really mean? Review of the literature and thorough study of 142 cases". Brain. 129 (Pt 7): 1640–58. doi:10.1093/brain/awl105. PMID 16670178.
- ↑ 12.0 12.1 12.2 Guillery-girard, B.; Quinette, P.; Desgranges, B.; Piolino, P.; Viader, F.; De La Sayette, V.; Eustache, F. (2006). "Long-term memory following transient global amnesia: an investigation of episodic and semantic memory". Acta Neurologica Scandinavica. 114 (5): 329–33. doi:10.1111/j.1600-0404.2006.00625.x. PMID 17022781.
- ↑ 13.0 13.1 Le Pira; Giuffrida, S; Maci, T; Reggio, E; Zappalà, G; Perciavalle, V (2005). "Cognitive findings after transient global amnesia: role of prefrontal cortex". Applied Neuropsychology. 12 (4): 212–7. doi:10.1207/s15324826an1204_5. PMID 16422663.
- ↑ Landres, Bruce (13 April 2003). "Clinical Vignette: Transient Global Amnesia". Archived from the original on 9 March 2012. Retrieved 18 October 2009.
- ↑ 15.0 15.1 Nakada; Kwee, IL; Fujii, Y; Knight, RT (2005). "High-field, T2 reversed MRI of the hippocampus in transient global amnesia". Neurology. 64 (7): 1170–4. doi:10.1212/01.WNL.0000156158.48587.EA. PMID 15824342.
- ↑ 16.0 16.1 Kessler, Josef; Markowitsch, Hans; Rudolf, Jobst; Heiss, Wolf-Dieter (2001). "Continuing Cognitive Impairment After Isolated Transient Global Amnesia". International Journal of Neuroscience. 106 (3–4): 159–68. doi:10.3109/00207450109149746. PMID 11264917.
- ↑ Enzinger, C.; Thimary, F.; Kapeller, P.; Ropele, S.; Schmidt, R.; Ebner, F.; Fazekas, F. (2008). "Transient Global Amnesia: Diffusion-Weighted Imaging Lesions and Cerebrovascular Disease". Stroke. 39 (8): 2219–25. doi:10.1161/STROKEAHA.107.508655. PMID 18583561.
- ↑ 18.0 18.1 18.2 Bauer, G.; Benke, T; Unterberger, I; Schmutzhard, E; Trinka, E (2005). "Transient global amnesia or transient epileptic amnesia?". QJM. 98 (5): 383, author reply 383–4. doi:10.1093/qjmed/hci060. PMID 15833772.
- ↑ 19.0 19.1 19.2 19.3 Zorzon, Marino; Antonutti, L; Masè, G; Biasutti, E; Vitrani, B; Cazzato, G (1995). "Transient Global Amnesia and Transient Ischemic Attack : Natural History, Vascular Risk Factors, and Associated Conditions". Stroke. 26 (9): 1536–42. doi:10.1161/01.STR.26.9.1536. PMID 7660394.
- ↑ 20.0 20.1 20.2 Miller, J. W.; Petersen, R; Metter, E; Millikan, C; Yanagihara, T (1987). "Transient global amnesia: Clinical characteristics and prognosis". Neurology. 37 (5): 733–7. doi:10.1212/wnl.37.5.733. PMID 3574671. Archived from the original on 2009-09-12. Retrieved 2021-09-18.
- ↑ 21.0 21.1 21.2 Pantoni; Bertini, E; Lamassa, M; Pracucci, G; Inzitari, D (2005). "Clinical features, risk factors, and prognosis in transient global amnesia: a follow-up study". European Journal of Neurology. 12 (5): 350–6. doi:10.1111/j.1468-1331.2004.00982.x. PMID 15804264.
- ↑ Inzitari; Pantoni, L; Lamassa, M; Pallanti, S; Pracucci, G; Marini, P (1997). "Emotional arousal and phobia in transient global amnesia". Archives of Neurology. 54 (7): 866–73. doi:10.1001/archneur.1997.00550190056015. PMID 9236576.
- ↑ 23.0 23.1 Lewis, S (1998). "Aetiology of transient global amnesia". The Lancet. 352 (9125): 397–9. doi:10.1016/S0140-6736(98)01442-1. PMID 9717945.
- ↑ Chung, C. -P.; Hsu, HY; Chao, AC; Chang, FC; Sheng, WY; Hu, HH (2006). "Detection of intracranial venous reflux in patients of transient global amnesia". Neurology. 66 (12): 1873–7. doi:10.1212/01.wnl.0000219620.69618.9d. PMID 16801653.
- ↑ Sander, Kerstin; Sander, Dirk (2005). "New insights into transient global amnesia: recent imaging and clinical findings". The Lancet Neurology. 4 (7): 437–44. doi:10.1016/S1474-4422(05)70121-6. PMID 15963447.
- ↑ Moreno-lugris; Martínez-Alvarez, J; Brañas, F; Martínez-Vázquez, F; Cortés-Laiño, JA (1996). "Transient global amnesia. Case-control study of 24 cases". Revista de Neurología. 24 (129): 554–7. PMID 8681172.
- ↑ Nedelmann; Eicke, BM; Dieterich, M (2005). "Increased incidence of jugular valve insufficiency in patients with transient global amnesia". Journal of Neurology. 252 (12): 1482–6. doi:10.1007/s00415-005-0894-9. PMID 15999232.
- ↑ Akkawi NM, Agosti C, Rozzini L, Anzola GP, Padovani A (2001). "Transient global amnesia and venous flow patterns". The Lancet. 357 (9256): 639. doi:10.1016/S0140-6736(05)71434-3. PMID 11558519.
- ↑ Vuilleumier, P.; Despland, P; Regli, F (1996). "Failure to recall (but not to remember): Pure transient amnesia during nonconvulsive status epilepticus". Neurology. 46 (4): 1036–9. doi:10.1212/wnl.46.4.1036. PMID 8780086. Archived from the original on 2005-11-14. Retrieved 2021-09-18.
- ↑ Healy, D.; Morgan, R.; Chinnaswamy, S. (2009). "Transient global amnesia associated with statin intake". Case Reports. 2009: bcr0620080033. doi:10.1136/bcr.06.2008.0033. PMC 3027897. PMID 21686951.
- ↑ Graveline, Duane. "Statins and Amnesia". Archived from the original on 8 November 2009. Retrieved 19 October 2009.
{{cite journal}}: Cite journal requires|journal=(help)[unreliable source?] - ↑ 32.0 32.1 32.2 Sucholeiki, Roy (3 December 2008). "Transient Global Amnesia". eMedicine. Medscape. Archived from the original on 27 September 2009. Retrieved 19 October 2009.
- ↑ Engmann, Birk; Reuter, Mike (2003). "A case history of sudden memory dysfunction – caused by transient epileptic amnesia". Aktuelle Neurologie. 30 (7): 350–353. doi:10.1055/s-2003-41889.
- ↑ 34.0 34.1 Landres B: UCLA Department of Medicine Clinical Vignette: Transient Global Amnesia. Last Revised: Sun, 13-Apr-2003. "Archived copy". Archived from the original on 2012-03-09. Retrieved 2012-07-03.
{{cite web}}: CS1 maint: archived copy as title (link) accessed 9/26/09 - ↑ Monzani; Rovellini, A; Schinco, G; Silani, V (2000). "Transient global amnesia or subarachnoid haemorrhage? Clinical and laboratory findings in a particular type of acute global amnesia". European Journal of Emergency Medicine. 7 (4): 291–3. doi:10.1097/00063110-200012000-00007. PMID 11764138.
- ↑ Magnus Harrison; Mark Williams (2007). "The diagnosis and management of transient global amnesia in the emergency department". Emerg Med J. 24 (6): 444–445. doi:10.1136/emj.2007.046565. PMC 2658295. PMID 17513554.
- ↑ Borroni; Agosti, C; Brambilla, C; Vergani, V; Cottini, E; Akkawi, N; Padovani, A (2004). "Is transient global amnesia a risk factor for amnestic mild cognitive impairment?". Journal of Neurology. 251 (9): 1125–7. doi:10.1007/s00415-004-0497-x. PMID 15372257.
- ↑ Koski; Marttila, RJ (1990). "Transient global amnesia: incidence in an urban population". Acta Neurologica Scandinavica. 81 (4): 358–60. doi:10.1111/j.1600-0404.1990.tb01571.x. PMID 2360405.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 errors: missing periodical
- All articles lacking reliable references
- Articles lacking reliable references from October 2009
- Articles with invalid date parameter in template
- CS1 maint: archived copy as title
- All articles with unsourced statements
- Articles with unsourced statements from February 2010
- Portal templates with all redlinked portals
- Portal-inline template with redlinked portals
- Amnesia
- Episodic and paroxysmal disorders
- Neurological disorders
- RTT
- WHRTT