Thymoma
| Thymoma | |
|---|---|
| Other names: | |
| Specialty | Oncology, cardiothoracic surgery |
| Usual onset | Adulthood |
| Treatment | surgical removal, chemotherapy (in malignant cases). |
| Frequency | 013-0.26 per 100,000 people per year[1] |
A thymoma is a tumor originating from the epithelial cells of the thymus.[1] It may be associated with myasthenia gravis.[2]
They are classified mainly by their appearance under the miscroscope.[2] Types include type A and AB thymomas which are distinct from B1 to B3 thymomas.[2] Both groups belong to a spectrum of tumors, and are considered genomically completely distinct from thymoma carcinoma.[2] Other types include micronodular thymoma with lymphoid stroma, and metaplastic thymoma.[2]
It is considered a rare malignancy.
Signs and symptoms
A third of all people with a thymoma have symptoms caused by compression of the surrounding organs by an expansive mass. These problems may take the form of superior vena cava syndrome, dysphagia (difficulty swallowing), cough, or chest pain.[3]
One-third of patients have their tumors discovered because they have an associated autoimmune disorder. As mentioned earlier, the most common of those conditions is myasthenia gravis (MG); 10–15% of patients with MG have a thymoma and, conversely, 30–45% of patients with thymomas have MG. Additional associated autoimmune conditions include thymoma-associated multiorgan autoimmunity, pure red cell aplasia and Good syndrome (thymoma with combined immunodeficiency and hypogammaglobulinemia). Other reported disease associations are with acute pericarditis, agranulocytosis, alopecia areata, ulcerative colitis, Cushing's disease, hemolytic anemia, limbic encephalopathy, myocarditis, nephrotic syndrome, panhypopituitarism, pernicious anemia, polymyositis, rheumatoid arthritis, sarcoidosis, scleroderma, sensorimotor radiculopathy, stiff person syndrome, systemic lupus erythematosus and thyroiditis.[3][4]
One-third to one-half of all persons with thymoma have no symptoms at all, and the mass is identified on a chest X-ray or CT/CAT scan performed for an unrelated problem.[3]
Classification and pathology
Thymoma originates from the epithelial cell population in the thymus.[2] They are classified mainly by their appearance under the miscroscope; immunohistochemistry is rarely required.[2] Types include type A thymoma (including an atypical variant), AB thymoma, type B thymoma (separated into B1, B2, and B3 thymomas), micronodular thymoma with lymphoid stroma, and metaplastic thymoma.[2] Type A and AB thymomas are distinct from B1 to B3 thymomas.[2] Both groups belong to a spectrum of tumors, and are considered genomically completely distinct from thymoma carcinoma.[2]
Thymic cortical epithelial cells have abundant cytoplasm, vesicular nucleus with finely divided chromatin and small nucleoli and cytoplasmic filaments contact adjacent cells. Thymic medullary epithelial cells in contrast are spindle shaped with oval dense nucleus and scant cytoplasm thymoma if recapitulates cortical cell features more, is thought to be less benign.
Diagnosis


When a thymoma is suspected, a CT/CAT scan is generally performed to estimate the size and extent of the tumor, and the lesion is sampled with a CT-guided needle biopsy. Increased vascular enhancement on CT scans can be indicative of malignancy, as can be pleural deposits.[3] Limited[clarification needed] biopsies are associated with a very small risk of pneumomediastinum or mediastinitis and an even-lower risk of damaging the heart or large blood vessels. Sometimes thymoma metastasize for instance to the abdomen.[5]
The diagnosis is made via histologic examination by a pathologist, after obtaining a tissue sample of the mass. Final tumor classification and staging is accomplished pathologically after formal[clarification needed] surgical removal of the thymic tumor.
Selected laboratory tests can be used to look for associated problems or possible tumor spread. These include: full blood count, protein electrophoresis, antibodies to the acetylcholine receptor (indicative of myasthenia), electrolytes, liver enzymes and renal function.[3]
Staging
The Masaoka Staging System is used widely and is based on the anatomic extent of disease at the time of surgery:[6]
- I: Completely encapsulated
- IIA: Microscopic invasion through the capsule into surrounding fatty tissue
- IIB: Macroscopic invasion into capsule
- III: Macroscopic invasion into adjacent organs
- IVA: Pleural or pericardial implants
- IVB: Lymphogenous or hematogenous metastasis to distant (extrathoracic) sites
Treatment
Surgery is the mainstay of treatment for thymoma. If the tumor is apparently invasive and large, preoperative (neoadjuvant) chemotherapy and/or radiotherapy may be used to decrease the size and improve resectability, before surgery is attempted. When the tumor is an early stage (Masaoka I through IIB), no further therapy is necessary. Removal of the thymus in adults does not appear to induce immune deficiency. In children, however, postoperative immunity may be abnormal and vaccinations for several infectious agents are recommended. Invasive thymomas may require additional treatment with radiotherapy and chemotherapy (cyclophosphamide, doxorubicin and cisplatin).[3][citation needed].[7] Recurrences of thymoma are described in 10-30% of cases up to 10 years after surgical resection, and in the majority of cases also pleural recurrences can be removed. Recently, surgical removal of pleural recurrences can be followed by hyperthermic intrathoracic perfusion chemotherapy or intrathoracic hyperthermic perfused chemotherapy (ITH).
Once diagnosed, thymomas may be removed surgically. In the rare case of a malignant tumor, chemotherapy may be used.
Prognosis
Prognosis is much worse for stage III or IV thymomas as compared with stage I and II tumors. Invasive thymomas uncommonly can also metastasize, generally to pleura, bones, liver or brain in approximately 7% of cases.[3] A study found that slightly over 40% of observed patients with stage III and IV tumors survived for at least 10 years after diagnosis. The median age of these patients at the time of thymoma diagnosis was 57 years. [8]
Patients who have undergone thymectomy for thymoma should be warned of possible severe side effects after yellow fever vaccination. This is probably caused by inadequate T-cell response to live attenuated yellow fever vaccine. Deaths have been reported.[citation needed]
Epidemiology
Men and women are equally affected by thymomas. The typical age at diagnosis is 30–40, although cases have been described in every age group, including children.[3]
Thymomas are frequently associated with neuromuscular disorders such as myasthenia gravis;[3] thymoma is found in 20% of patients with myasthenia gravis.[9]
History
The “type A, AB, B1-B3 thymoma” for the major thymoma types was introduced by Juan Rosai in the 1999 second edition of the WHO Classification and remained so in the 5th edition in 2021.[2]
Gallery
-
An encapsulated cystic thymoma.
-
A locally invasive circumscribed thymoma (mixed lymphocytic and epithelial, mixed polygonal and spindle).
-
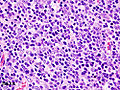
Histopathological image of thymoma type B1. Anterior mediastinal mass surgically resected. Hematoxylin & eosin stain.
-
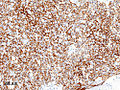
Histopathological image of thymoma type B1. Anterior mediastinal mass surgically resected. Cytokeratin CAM5.2 immunostain.
-
Histopathological image representing a noninvasive thymoma type B1, surgically resected. Hematoxylin & eosin.
-
Thymoma. FNA specimen. Field stain.
See also
References
- ↑ 1.0 1.1 WHO Classification of Tumours Editorial Board (2021). "5. Tumors of the thymus". Thoracic Tumours. Vol. 5 (5th ed.). Lyon (France): World Health Organization. pp. 320–325. ISBN 978-92-832-4506-3. Archived from the original on 2022-05-14. Retrieved 2022-07-26.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 Marx, Alexander; Chan, John K. C.; Chalabreysse, Lara; Dacic, Sanja; Detterbeck, Frank; French, Christopher A.; Hornick, Jason L.; Inagaki, Hiroshi; Jain, Deepali; Lazar, Alexander J.; Marino, Mirella; Marom, Edith M.; Moreira, Andre L.; Nicholson, Andrew G.; Noguchi, Masayuki; Nonaka, Daisuke; Papotti, Mauro G.; Porubsky, Stefan; Sholl, Lynette M.; Tateyama, Hisashi; Thomas de Montpréville, Vincent; Travis, William D.; Rajan, Arun; Roden, Anja C.; Ströbel, Philipp (February 2022). "The 2021 WHO Classification of Tumors of the Thymus and Mediastinum: What Is New in Thymic Epithelial, Germ Cell, and Mesenchymal Tumors?". Journal of Thoracic Oncology: Official Publication of the International Association for the Study of Lung Cancer. 17 (2): 200–213. doi:10.1016/j.jtho.2021.10.010. ISSN 1556-1380. PMID 34695605. Archived from the original on 2022-06-18. Retrieved 2022-07-27.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Thomas CR, Wright CD, Loehrer PJ (July 1999). "Thymoma: state of the art". Journal of Clinical Oncology. 17 (7): 2280–9. doi:10.1200/JCO.1999.17.7.2280. PMID 10561285. Archived from the original on 2022-07-28. Retrieved 2021-12-30.
- ↑ Bernard C, Frih H, Pasquet F, Kerever S, Jamilloux Y, Tronc F, Guibert B, Isaac S, Devouassoux M, Chalabreysse L, Broussolle C, Petiot P, Girard N, Sève P (January 2016). "Thymoma associated with autoimmune diseases: 85 cases and literature review". Autoimmunity Reviews. 15 (1): 82–92. doi:10.1016/j.autrev.2015.09.005. PMID 26408958.
- ↑ van Geffen WH, Sietsma J, Roelofs PM, Hiltermann TJ (December 2011). "A malignant retroperitoneal mass--a rare presentation of recurrent thymoma". BMJ Case Reports. 2011: bcr0920114737. doi:10.1136/bcr.09.2011.4737. PMC 3229325. PMID 22674945.
- ↑ Masaoka A, Monden Y, Nakahara K, Tanioka T (December 1981). "Follow-up study of thymomas with special reference to their clinical stages". Cancer. 48 (11): 2485–92. doi:10.1002/1097-0142(19811201)48:11<2485::AID-CNCR2820481123>3.0.CO;2-R. PMID 7296496.
- ↑ NCCN Thymoma, Guidelines (2016). "NCCN Thymoma Guidelines" (PDF). NCCN Guidelines. Archived (PDF) from the original on 2021-12-14. Retrieved 2021-12-30.
- ↑ Wilkins KB, Sheikh E, Green R, Patel M, George S, Takano M, Diener-West M, Welsh J, Howard S, Askin F, Bulkley GB (October 1999). "Clinical and pathologic predictors of survival in patients with thymoma". Annals of Surgery. 230 (4): 562–72, discussion 572–4. doi:10.1097/00000658-199910000-00012. PMC 1420905. PMID 10522726.
- ↑ Mitchell, Richard Sheppard; Kumar, Vinay; Robbins, Stanley L.; Abbas, Abul K.; Fausto, Nelson (2007). Robbins basic pathology. Saunders/Elsevier. ISBN 978-1-4160-2973-1.[page needed]
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- Wikipedia articles needing page number citations from May 2018
- Articles with invalid date parameter in template
- Wikipedia articles needing clarification from November 2015
- All articles with unsourced statements
- Articles with unsourced statements from November 2007
- Articles with unsourced statements from April 2010
- Rare cancers
- Lymphatic organ neoplasia