Sydenham's chorea
| Sydenham's chorea | |
|---|---|
| Other names: Rheumatic chorea[1], Chorea minor, St Vitus' dance | |
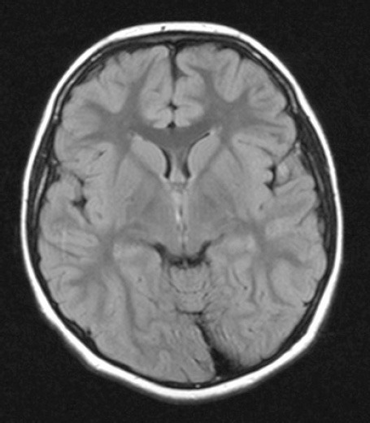 | |
| MRI of individual with Sydenham chorea. | |
Sydenham's chorea, also known as chorea minor and historically and occasionally referred to as St Vitus' dance, is a disorder characterized by rapid, uncoordinated jerking movements primarily affecting the face, hands and feet.[2] Sydenham's chorea is an autoimmune disease that results from childhood infection with Group A beta-haemolytic Streptococcus. It is reported to occur in 20–30% of people with acute rheumatic fever and is one of the major criteria for it, although it sometimes occurs in isolation. The disease occurs typically a few weeks, but up to 6 months, after the acute infection, which may have been a simple sore throat (pharyngitis).
Sydenham's chorea is more common in females than males and most cases affect children between the ages of 5 and 15 years of age. Adult onset of Sydenham's chorea is comparatively rare, and the majority of the adult cases are recurrences following childhood Sydenham's chorea.
Signs and symptoms
Sydenham's chorea is characterized by the abrupt onset (sometimes within a few hours) of neurologic symptoms, classically chorea, which are non-rhythmic, writhing or explosive involuntary movements. Usually all four limbs are affected, but there are cases reported where just one side of the body is affected (hemichorea). Typical chorea includes repeated wrist hyperextension, grimacing, lip pouting. The fingers can move as if playing the piano. There may be tongue fasciculations ("bag of worms") and motor impersistence for example the "milk maid sign" (grip strength fluctuates, as if hand milking), or inability to sustain tongue protrusion or eye closure. There is usually loss of fine motor control, particularly obvious in handwriting if the child is of school age. Speech is often affected (dysarthria), as is walking; legs will suddenly give way or flick out to one side, giving an irregular gait and the appearance of skipping or dancing. Underlying the abnormal movements is often low tone (hypotonia) which may not become obvious until treatment is started to suppress the chorea. In severe cases, the loss of tone and weakness predominate (chorea paralyticum).
The severity of the condition can vary from just some instability on walking and difficulty with hand writing, to the extreme of being wholly unable to walk, talk, or feed yourself.
Movements cease during sleep. The eye muscles are not affected, curiously.[citation needed]
It is a neuropsychiatric disorder, so besides the motor problems there is classically emotional lability (mood swings, or inappropriate mood), anxiety, attention deficit. These can precede the motor symptoms.[3]
Non-neurologic manifestations of acute rheumatic fever may be present, namely carditis (up to 70% of cases, often subclinical, so echocardiography required), arthritis, erythema marginatum, and subcutaneous nodules.

Differentiating these signs from other involuntary movements such as tics and stereotypies can be difficult, and since these things are not uncommon they can potentially co-exist. Diagnosis is often delayed and attributed to another condition such as tic disorder or conversion disorder. The controversial PANDAS (pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections) hypothesis has overlapping clinical features but Sydenham's chorea is one of the exclusion criteria. PANDAS can present with chorea but more typically there are tics, stereotypies with a psychological component (e.g., OCD).[4][5][6]
Pathology
One of the important manifestations of acute rheumatic fever, Sydenham's chorea is similarly caused by an autoimmune response following infection by group A β-hemolytic streptococci.[7]
Two cross reactive streptococcal antigens have been identified, the M protein and N-acetyl-beta-D-glucosamine, whereby infection leads to autoantibodies being produced against host tissues (molecular mimicry) causing a variety of streptococcal related diseases including Sydenham's chorea but also rheumatic heart disease and nephritic syndrome.[8] Autoantibodies against basal ganglia proteins have been found in Sydenham's chorea but these are non-specific.[9] Dopamine receptor autoantibodies have been reported to correlate with clinical symptoms.[10] Whether these antibodies represent an epi-phenomenon or are pathogenic, remains to be proven.[citation needed]
Diagnosis
Chorea is distinctive, if the health care provider is familiar with it. The diagnosis is then made by the typical acute onset in the weeks following a sore throat or other minor infection, plus evidence of inflammation (raised CRP and/or ESR) and evidence of recent streptococcal infection.
To confirm recent streptococcal infection:
- Throat culture
- Anti-DNAse B titre (peaks at 8–12 weeks after infection)
- Anti-streptolysin O titre (peaks at 3–5 weeks)
None of these tests are 100% reliable, particularly when the infection was some months previously.
Further testing is directed more towards alternative diagnoses and other manifestations of rheumatic fever:
- Echocardiography
- EEG
- Lumbar puncture
- Magnetic resonance imaging or computed tomography scan of the brain (alterations in caudate nucleus and putaminal enlargement have been described in some patients)[11][12]
Differential diagnosis
Other disorders that may be accompanied by chorea include benign hereditary chorea, bilateral striatal necrosis, abetalipoproteinemia, ataxia–telangiectasia, biotin-thiamine-responsive basal ganglia disease, Fahr disease, familial dyskinesia–facial myokymia (Bird–Raskind syndrome) due to an ADCY5 gene mutation, glutaric aciduria, Lesch–Nyhan syndrome, mitochondrial disorders, Huntington's disease, Wilson disease, hyperthyroidism, lupus erythematosus, pregnancy (chorea gravidarum), drug intoxication and side effects of certain anticonvulsants (e.g. phenytoin) or psychotropic agents. Although some of these can similarly present in an acute way, there will typically be other neurological signs (such as ataxia or cognitive impairment), or other disease manifestations, or positive family history, which will help distinguish between them.[13]
Management
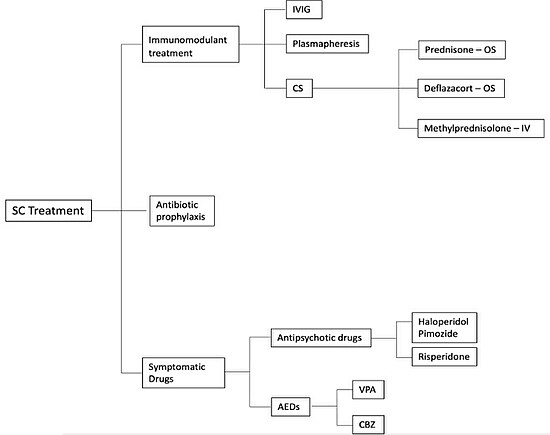
Management of Sydenham's chorea is based on the following principles:
- Eliminate the streptococcus – it may not be of any use for the index patient but further spread of that specific clone will be prevented.
- Treat the movement disorder
- Immunosuppression
- Prevention of relapses and further cardiac damage
- Manage the disability
There is a UFMG rating scale Archived 2021-10-08 at the Wayback Machine for Sydenham's chorea, from Brazilian Universidade Federal de Minas Gerais (UFMG), for research purposes, but it only looks at motor function not psychiatric/behavioural symptoms.

Occupational therapy and physiotherapy is useful for maintaining function and muscle tone.
Treatment with sodium valproate is effective for controlling symptoms, but it doesn’t speed up recovery. Haloperidol was used previously, but caused serious side effects e.g. tardive dyskinesia. Case reports exist to support carbamazepine and levetiracetam; other drugs tried include pimozide, clonidine, and phenobarbitone.
Immunosuppression
Immunosuppression is used inconsistently in Sydenham's chorea. The model of an autoimmune disorder would support its use. One randomized controlled trial of steroids from Paz, Brazil in 2006 (22 cases) showed remission reduced to 54 days from 119 days.[15] Various other reports of use of oral or IV steroids from Israel, Italy and Brazil .[16][17][18] Immunoglobulin has been used in Holland and South Africa.[19][20] Some improvement can be seen within a few days of IV steroids. In Italy, prednisolone reduced average duration of symptoms from 9 weeks to 4 weeks, and these were severe cases.[16] South African group found less neuropsychiatric complications at 6 months with IVIG treatment (IVIG preferred due to fear of TB reactivation).[21]
A course of penicillin is usually given at diagnosis to definitively clear any remaining streptococci, but there is no evidence that this is an effective treatment. Active infection is usually cleared by diagnosis. Penicillin prophylaxis, on the other hand, is essential to treat cardiac features of rheumatic fever, even if subclinical (American Heart Association guideline).[22] If the case is of isolated chorea, it is arguable whether cardiac risk justifies prophylaxis or not, however it is likely to reduce recurrence.
There are several historical case series reporting successful treatment of Sydenham's chorea by inducing fever.[23][24]
Prognosis
Motor problems including chorea settle within an average of 2–3 months.
Recurrence seen in 16–40% of cases. Recurrence is more likely with poor compliance with penicillin prophylaxis. Intramuscular penicillin is given every 2–3 weeks superior to 4 weekly regime, and oral penicillin is also prescribed. Recurrences are sometimes associated with rise in ASO titre or other evidence of new streptococcal infection. There is no obvious clinical parameter that might predict those at risk of recurrence. More likely if failure to remit in initial 6 months, can recur with pregnancy (chorea gravidorum).
Higher recurrence rates seen in longest follow up – can recur up to 10 years after the initial episode, so might be underestimated by series with shorter follow up.
Recurrence is usually only chorea, even if the original case was associated with rheumatic fever. There are two total reports of heart disease worsening after recurrence of chorea. The Thailand study also had 2 cases where carditis, which had improved after initial diagnosis, came back again. Some suggest that recurrent chorea is a different disease altogether.[25]
10% reported long term tremor in one study (10 years follow up). Long term neuropsychiatric difficulties are increasingly recognized (49 studies so far, especially obsessive-compulsive disorder but also attention-deficit hyperactivity disorder, affective disorders, tic disorders, executive function disturbances, psychotic features, and language impairment).[26]
Heart involvement improves in about a third of cases (whether silent or not).[PMID 22734303]
Epidemiology
As with rheumatic fever, Sydenham's chorea is seen more often in less affluent communities, whether in the developing world or in aboriginal communities in the global North. High rates of impetigo are a marker for widespread streptococcal transmission.
History
The incidence of acute rheumatic fever and rheumatic heart disease is not declining. Recent figures quote the incidence of Acute Rheumatic Fever as 0.6–0.7/1,000 population in the United States and Japan compared with 15–21/1,000 population in Asia and Africa.[27] The prevalence of Acute Rheumatic Fever and Sydenham's Chorea has declined progressively in developed countries over the last decades.[28][29]
Etymology
It is named after British physician Thomas Sydenham (1624–1689).[27][30] The alternate eponym, "Saint Vitus Dance", is in reference to Saint Vitus, a Christian saint who was persecuted by Roman emperors and died as a martyr in AD 303. Saint Vitus is considered to be the patron saint of dancers, with the eponym given as homage to the manic dancing that historically took place in front of his statue during the feast of Saint Vitus in Germanic and Latvian cultures.[31]
References
- ↑ "Sydenham Chorea - Symptoms, Causes, Treatment | NORD". rarediseases.org. Archived from the original on 2023-09-30. Retrieved 2024-03-06.
- ↑ "Sydenham Chorea Information Page | National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. Archived from the original on 1 March 2021. Retrieved 2 March 2021.
- ↑ Oosterveer, Daniëlla M.; Overweg-Plandsoen, Wilhelmina C.T.; Roos, Raymund A.C. (July 2010). "Sydenham's Chorea: A Practical Overview of the Current Literature". Pediatric Neurology. 43 (1): 1–6. doi:10.1016/j.pediatrneurol.2009.11.015. PMID 20682195. Archived from the original on 11 January 2022. Retrieved 2 March 2021.
- ↑ Wilbur C, Bitnun A, Kronenberg S, Laxer RM, Levy DM, Logan WJ, Shouldice M, Yeh EA (May 2019). "PANDAS/PANS in childhood: Controversies and evidence". Paediatr Child Health. 24 (2): 85–91. doi:10.1093/pch/pxy145. PMC 6462125. PMID 30996598.
- ↑ Sigra S, Hesselmark E, Bejerot S (March 2018). "Treatment of PANDAS and PANS: a systematic review". Neurosci Biobehav Rev. 86: 51–65. doi:10.1016/j.neubiorev.2018.01.001. PMID 29309797. S2CID 40827012. Archived from the original on 2022-01-11. Retrieved 2021-12-06.
- ↑ Swedo SE, Leonard HL, Garvey M, et al. (February 1998). "Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections: clinical description of the first 50 cases". The American Journal of Psychiatry. 155 (2): 264–71. doi:10.1176/ajp.155.2.264 (inactive 31 October 2021). PMID 9464208. Archived from the original on 27 March 2020. Retrieved 6 December 2021.
{{cite journal}}: CS1 maint: DOI inactive as of October 2021 (link) - ↑ Swedo SE, Leonard HL, Shapiro MB (1993). "Sydenham's Chorea:Physical and Psychological Symptoms of St Vitus Dance". Pediatrics. 91 (4): 706–713. PMID 8464654.
- ↑ Cunningham, Madeleine W. (2 August 2019). "Molecular Mimicry, Autoimmunity, and Infection: The Cross-Reactive Antigens of Group A Streptococci and their Sequelae". Microbiology Spectrum. 7 (4). doi:10.1128/microbiolspec.GPP3-0045-2018. PMC 6684244. PMID 31373269.
- ↑ Dale RC, Merheb V, Pillai S, et al. (2012). "Antibodies to surface dopamine-2 receptor in autoimmune movement and psychiatric disorders". Brain. 135 (11): 3453–3468. doi:10.1093/brain/aws256. PMID 23065479.
- ↑ Ben-Pazi H, Stoner JA, Cunningham MW (2013). "Dopamine receptor autoantibodies correlate with symptoms in Sydenham's chorea". PLOS ONE. 8 (9): e73516. Bibcode:2013PLoSO...873516B. doi:10.1371/journal.pone.0073516. PMC 3779221. PMID 24073196.
- ↑ "Sydenham chorea: MedlinePlus Medical Encyclopedia". Archived from the original on 2021-12-14. Retrieved 2021-12-06.
- ↑ Faustino PC, Terreri MT, Rocha AJ, et al. (2003). "Clinical, laboratory, psychiatric and magnetic resonance findings in patients with sydenham chorea". Neuroradiology. 45 (7): 456–462. doi:10.1007/s00234-003-0999-8. PMID 12811441. S2CID 23605799.
- ↑ Zomorrodi A, Wald ER (2006). "Sydenham's Chorea in Western Pennsylvania". Pediatrics. 117 (4): 675–679. doi:10.1542/peds.2005-1573. PMID 16533893. S2CID 32478765. Archived from the original on 2022-01-11. Retrieved 2021-12-06.
- ↑ Depietri, Greta; Carli, Niccolo; Sica, Attilio; Oliviero, Domenico; Costagliola, Giorgio; Striano, Pasquale; Bonuccelli, Alice; Frisone, Flavia; Peroni, Diego; Consolini, Rita; Foiadelli, Thomas; Orsini, Alessandro (2021). "Therapeutic aspects of Sydenham's Chorea: an update". Acta Bio Medica : Atenei Parmensis. 92 (Suppl 4): e2021414. doi:10.23750/abm.v92iS4.12663. ISSN 0392-4203.
- ↑ Paz, José A.; Silva, Clovis A.A.; Marques-Dias, Maria J. (April 2006). "Randomized Double-Blind Study With Prednisone in Sydenham's Chorea". Pediatric Neurology. 34 (4): 264–269. doi:10.1016/j.pediatrneurol.2005.08.028. PMID 16638499.
- ↑ 16.0 16.1 Fusco, Carlo; Ucchino, Valentina; Frattini, Daniele; Pisani, Francesco; Della Giustina, Elvio (July 2012). "Acute and chronic corticosteroid treatment of ten patients with paralytic form of Sydenham's chorea". European Journal of Paediatric Neurology. 16 (4): 373–378. doi:10.1016/j.ejpn.2011.12.005. PMID 22197452.
- ↑ Fusco, C.; Spagnoli, C. (March 2018). "Corticosteroid treatment in Sydenham's chorea". European Journal of Paediatric Neurology. 22 (2): 327–331. doi:10.1016/j.ejpn.2017.11.011. PMID 29287833.
- ↑ Teixeira Jr., Antônio L.; Maia, Débora P.; Cardoso, Francisco (August 2005). "Treatment of acute Sydenham's chorea with methyl-prednisolone pulse-therapy". Parkinsonism & Related Disorders. 11 (5): 327–330. doi:10.1016/j.parkreldis.2005.02.007. PMID 15878690.
- ↑ Boersma, Nienke Anne; Schippers, Herman; Kuijpers, Taco; Heidema, Jojanneke (27 January 2016). "Successful treatment of Sydenham's chorea with intravenous immunoglobulin". BMJ Case Reports. 2016: bcr2015211673. doi:10.1136/bcr-2015-211673. PMC 4746543. PMID 26837939.
- ↑ Gregorowski, Claire; Lochner, Christine; Martin, Lindi; Simmons, Candice; Kidd, Martin; Walker, Kathleen; Wilmshurst, Jo M.; Seedat, Soraya (1 February 2016). "Neuropsychological manifestations in children with Sydenham's chorea after adjunct intravenous immunoglobulin and standard treatment". Metabolic Brain Disease. 31 (1): 205–212. doi:10.1007/s11011-015-9681-1. PMID 25987537. S2CID 3234882.
- ↑ Dean, Shannon L.; Singer, Harvey S. (1 June 2017). "Treatment of Sydenham's Chorea: A Review of the Current Evidence". Tremor and Other Hyperkinetic Movements. 7: 456. doi:10.7916/d8w95gj2. PMC 5459984. PMID 28589057.
- ↑ Kumar, Raman Krishna; Antunes, Manuel J.; Beaton, Andrea; Mirabel, Mariana; Nkomo, Vuyisile T.; Okello, Emmy; Regmi, Prakash Raj; Reményi, Boglarka; Sliwa-Hähnle, Karen; Zühlke, Liesl Joanna; Sable, Craig; American Heart Association Council on Lifelong Congenital Heart Disease Heart Health in the Young; Council on Cardiovascular Stroke Nursing; Council on Clinical Cardiology (17 November 2020). "Contemporary Diagnosis and Management of Rheumatic Heart Disease: Implications for Closing the Gap: A Scientific Statement From the American Heart Association". Circulation. 142 (20): e337–e357. doi:10.1161/CIR.0000000000000921. PMID 33073615. S2CID 224783747.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Sutton, LP; Dodge, KG (1933). "The treatment of chorea by induced fever". The Journal of Pediatrics. 3 (6): 813–26. doi:10.1016/s0022-3476(33)80151-x.
- ↑ Sutton, LP; Dodge, KG (1936). "Fever therapy in chorea and in rheumatic carditis with and without chorea". The Journal of Laboratory and Clinical Medicine. 21 (6): 619–28.
- ↑ Gurkas, E; Karalok, ZS; Taskin, BD; Aydogmus, U; Guven, A; Degerliyurt, A; Bektas, O; Yilmaz, C (October 2016). "Predictors of recurrence in Sydenham's chorea: Clinical observation from a single center". Brain & Development. 38 (9): 827–34. doi:10.1016/j.braindev.2016.04.010. PMID 27209549. S2CID 2614986.
- ↑ Punukollu, M; Mushet, N; Linney, M; Hennessy, C; Morton, M (January 2016). "Neuropsychiatric manifestations of Sydenham's chorea: a systematic review". Developmental Medicine and Child Neurology. 58 (1): 16–28. doi:10.1111/dmcn.12786. PMID 25926089. S2CID 31037155.
- ↑ 27.0 27.1 Walker K, Lawrenson J, Wilmshurst JM (2006). "Sydenham's Chorea-clinical and therapeutic update 320 years down the line". South African Medical Journal. 96 (9): 906–912.
- ↑ Nausieda PA, Grossman BJ, Koller WC, et al. (1980). "Sydenham's Chorea:An update". Neurology. 30 (3): 331–334. doi:10.1212/wnl.30.3.331. PMID 7189038. S2CID 21035716.
- ↑ Eshel E, Lahat E, Azizi E, et al. (1993). "Chorea as a manifestation of rheumatic fever-a 30-year survey". European Journal of Pediatrics. 152 (8): 645–646. doi:10.1007/bf01955239. PMID 8404967. S2CID 29611352.
- ↑ "Sydenham's chorea". Whonamedit. Archived from the original on 2017-03-12. Retrieved 2011-09-16.
- ↑ "St. Vitus Information Page - Star Quest Production Network". Saints.sqpn.com. 2009-01-07. Archived from the original on 2019-07-26. Retrieved 2011-09-16.
Further reading
- Martino D, Tanner A, Defazio G, et al. (May 2005). "Tracing Sydenham's chorea: historical documents from a British paediatric hospital". Archives of Disease in Childhood. 90 (5): 507–11. doi:10.1136/adc.2004.057679. PMC 1720385. PMID 15851434.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 maint: DOI inactive as of October 2021
- CS1 maint: multiple names: authors list
- Articles with hatnote templates targeting a nonexistent page
- All articles with unsourced statements
- Articles with unsourced statements from May 2021
- Articles with invalid date parameter in template
- Articles with unsourced statements from December 2020
- Webarchive template wayback links
- Neurological disorders