Swimmer's itch
| Swimmer's itch | |
|---|---|
| Other names: Schistosome dermatitis,[1] cercarial dermatitis,[2] duck itch[3] | |
 | |
| Cercarial dermatitis on lower legs, four days after spending a day in the shallows of a lake | |
| Specialty | Dermatology |
| Symptoms | Itchy skin, red bumps, small blisters[2] |
| Complications | Secondary bacterial skin infection[2] |
| Usual onset | Minutes to days of exposure[2] |
| Duration | Up to 3 week[3] |
| Causes | Schistosome[1] |
| Risk factors | Shallow warm water[3] |
| Diagnostic method | Based on symptoms[3] |
| Differential diagnosis | Insect bites, contact dermatitis, seabather's eruption, seaweed dermatitis[4][3] |
| Treatment | Hydrocortisone cream, baking soda, Epsom salts, colloidal oatmeal baths[2] |
| Prognosis | Good[1] |
Swimmer's itch is an allergic reation due to certain microscopic parasites.[2] Symptoms include itchy skin, red bumps, and small blisters; involving skin directly exposed to water.[2][3] Onset occurs within minutes to days of exposure.[2] Symptoms may last for up to a few weeks.[2][3] Complications may include a secondary bacterial skin infection.[2] Repeated exposure may result in worse symptoms.[2]
It occurs due to water-borne schistosome, a type of flatworms.[1] The parasite's life cycle involves snails as well as birds and certain mammals.[2] It generally occurs as a result of swimming in infested fresh or salt water.[2] The condition has also been seen among rice farmers.[4] It is not spread between people.[2] Diagnosis is generally based on symptoms.[3]
Treatments that may help include hydrocortisone cream, baking soda, Epsom salts, and colloidal oatmeal baths.[2] Antihistamines may be taken by mouth.[4] There are no permanent effects.[1] Efforts to prevent the condition include toweling off after exiting the water and avoiding shallow warm water.[4][3]
Swimmer's itch occurs globally.[2] Children are more commonly affected than adults.[2] Rates of disease appear to be increasing; either due to it occurring in more regions or being better reported.[4] The cause of the condition was determined in 1928.[4] Outbreaks may affect tourism.[4] It is regarded as emerging infectious disease.[4]
Signs and symptoms
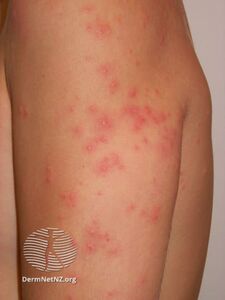
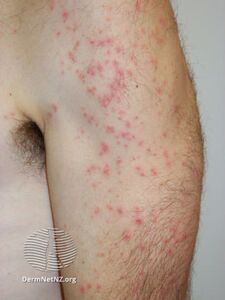
The main symptom is itchy papules (raised skin) that commonly occur within 2 days of infection. Initially, wheals develop quickly, then turn into maculae in about half an hour. Within 10–12 hours these turn into very itchy papules that reach their worst by the second or third day. The papules disappear in 1–2 weeks but secondary effects from scratching can continue longer. The intense itching, which peaks after 48–72 hours, is associated with pain and swelling of the affected areas.[5] People repeatedly exposed to cercariae develop heavier symptoms with faster onset.[6]
Rarely swollen lymph nodes, nausea, diarrhea, or fever may occur.[4] The skin involved is typically that directly exposed to water, rather than that covered by the swimsuit.[3]
-
Swimmers itch
-
Swimmers itch
Cause

Swimmer's itch probably has been around as long as humans. The condition was known to exist as early as the 1800s, but it was not until 1928 that a biologist found that the dermatitis was caused by the larval stage of a group of flatworm parasites in the family Schistosomatidae.[7] The genera most commonly associated with swimmer's itch in humans are Trichobilharzia[6] and Gigantobilharzia. It can also be caused by schistosome parasites of non-avian vertebrates, such as Schistosomatium douthitti, which infects snails and rodents. Other taxa reported to cause the reaction include Bilharziella polonica and Schistosoma bovis. In marine habitats, especially along the coasts, swimmer's itch can occur as well.[8]
These parasites use both freshwater snails and vertebrates as hosts in their parasitic life cycles as follows:
- Once a schistosome egg is immersed in water, a short-lived, non-feeding, free-living stage known as the miracidium emerges. The miracidium uses cilia to follow chemical and physical cues thought to increase its chances of finding the first intermediate host in its life cycle, a freshwater snail.
- After infecting a snail, it develops into a mother sporocyst, which in turn undergoes asexual reproduction, yielding large numbers of daughter sporocysts, which asexually produce another short-lived, free-living stage, the cercaria.
- Cercariae use a tail-like appendage (often forked in genera causing swimmer's itch) to swim to the surface of the water; and use various physical and chemical cues in order to locate the next and final (definitive) host in the life cycle, a bird. These larvae can accidentally come into contact with the skin of a swimmer. The cercaria penetrates the skin and dies in the skin immediately. The cercariae cannot infect humans, but they cause an inflammatory immune reaction. This reaction causes initially mildly itchy spots on the skin. Within hours, these spots become raised papules which are intensely itchy. Each papule corresponds to the penetration site of a single parasite.
- After locating a bird, the parasite penetrates through the skin (usually the feet), dropping the forked tail in the process. Inside the circulatory system, the immature worms (schistosomula) develop into mature male and female worms, mate and migrate through the host's circulatory system (or nervous system in case of T. regenti) to the final location (veins feeding the gastrointestinal tract) within the host body. There they lay eggs in the small veins in the intestinal mucosa from which they make their way into the lumen of the gut, and are dumped into the water when the bird defecates. One European species, Trichobilharzia regenti, instead infects the bird host's nasal tissues and larvae hatch from the eggs directly in the tissue during drinking/feeding of the infected birds.[9]
Risk factors

Humans usually become infected after swimming in lakes or other bodies of slow-moving fresh water. Some laboratory evidence indicates snails shed cercariae most intensely in the morning and on sunny days, and exposure to water in these conditions may therefore increase risk. Duration of swimming is positively correlated with increased risk of infection in Europe[10] and North America,[11] and shallow inshore waters may harbour higher densities of cercariae than open waters offshore. Onshore winds are thought to cause cercariae to accumulate along shorelines.[12] Studies of infested lakes and outbreaks in Europe and North America have found cases where infection risk appears to be evenly distributed around the margins of water bodies[10] as well as instances where risk increases in endemic swimmer's itch "hotspots".[12] Children may become infected more frequently and more intensely than adults but this probably reflects their tendency to swim for longer periods inshore, where cercariae also concentrate.[13] Stimuli for cercarial penetration into host skin include unsaturated fatty acids, such as linoleic and linolenic acids. These substances occur naturally in human skin and are found in sun lotions and creams based on plant oils.[citation needed]
Prevention

Various strategies targeting the mollusc and avian hosts of schistosomes have been used by lakeside residents in recreational areas of North America to deal with outbreaks of swimmer's itch. In Michigan, for decades, authorities used copper sulfate as a molluscicide to reduce snail host populations and thereby the incidence of swimmer's itch.[citation needed] The results with this agent have been inconclusive, possibly because:
- Snails become tolerant
- Local water chemistry reduces the molluscicide's efficacy
- Local currents diffuse it
- Adjacent snail populations repopulate a treated area[14]
More importantly, perhaps, copper sulfate is toxic to more than just molluscs, and the effects of its use on aquatic ecosystems are not well understood.[citation needed]
Another method targeting the snail host, mechanical disturbance of snail habitat, has been also tried in some areas of North America[12] and Lake Annecy in France, with promising results. Some work in Michigan suggests that administering praziquantel to hatchling waterfowl can reduce local swimmer's itch rates in humans.[15] Work on schistosomiasis showed that water-resistant topical applications of the common insect repellent DEET prevented schistosomes from penetrating the skin of mice.[16] Public education of risk factors, a good alternative to the aforementioned interventionist strategies, can also reduce human exposure to cercariae.[17]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 "With warm weather, Swimmers Itch makes annual appearance". dnr.wi.gov. Archived from the original on 2016-03-08. Retrieved 2016-03-07.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 Prevention, CDC-Centers for Disease Control and (18 September 2020). "CDC - Cercarial Dermatitis - Frequently Asked Questions (FAQs)". www.cdc.gov. Archived from the original on 10 June 2021. Retrieved 21 July 2022.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 3.9 "Swimmer's itch | DermNet NZ". dermnetnz.org. Archived from the original on 13 December 2021. Retrieved 21 July 2022.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 Horák, Petr; Mikeš, Libor; Lichtenbergová, Lucie; Skála, Vladimír; Soldánová, Miroslava; Brant, Sara Vanessa (January 2015). "Avian schistosomes and outbreaks of cercarial dermatitis". Clinical Microbiology Reviews. 28 (1): 165–190. doi:10.1128/CMR.00043-14. ISSN 1098-6618. PMC 4284296. PMID 25567226.
- ↑ Bonamonte, D.; Romita, P.; Vestita, M.; Angelini, G. (2016). "Dermatitis Caused by Aquatic Worms". In Bonamonte, D.; Angelini, G. (eds.). Aquatic Dermatology. Springer. p. 142. doi:10.1007/978-3-319-40615-2_9. ISBN 978-3-319-40615-2.
- ↑ 6.0 6.1 Macháček, Tomáš; Turjanicová, Libuše; Bulantová, Jana; Hrdý, Jiří; Horák, Petr; Mikeš, Libor (2018-10-09). "Cercarial dermatitis: a systematic follow-up study of human cases with implications for diagnostics". Parasitology Research. 117 (12): 3881–3895. doi:10.1007/s00436-018-6095-0. ISSN 0932-0113. PMID 30302587. S2CID 52945883.
- ↑ "Swimmer's Itch in Michigan" (PDF). State of Michigan. 2014. Archived (PDF) from the original on 3 January 2015. Retrieved 5 March 2015.
- ↑ Brant S, Cohen A, James D, Hui L, Hom A, Loker E (2010). "Cercarial Dermatitis Transmitted by Exotic Marine Snail". Emerging Infectious Diseases. 16 (9): 1357–65. doi:10.3201/eid1609.091664. PMC 3294964. PMID 20735918.
- ↑ Horák P., Kolářová L., Dvořák J. (1998). "Trichobilharzia regenti n. sp. (Schistosomatidae, Bilharziellinae), a new nasal schistosome from Europe" (PDF). Parasite. 5 (4): 349–357. doi:10.1051/parasite/1998054349. PMID 9879557. Archived (PDF) from the original on 2020-08-06. Retrieved 2021-06-05.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ 10.0 10.1 Chamot E, Toscani L, Rougemont A (1998). "Public health importance and risk factors for cercarial dermatitis associated with swimming in Lake Leman at Geneva, Switzerland". Epidemiol. Infect. 120 (3): 305–14. doi:10.1017/S0950268898008826. PMC 2809408. PMID 9692609.
- ↑ Lindblade KA (1998). "The epidemiology of cercarial dermatitis and its association with limnological characteristics of a northern Michigan lake". J. Parasitol. 84 (1): 19–23. doi:10.2307/3284521. JSTOR 3284521. PMID 9488332.
- ↑ 12.0 12.1 12.2 Leighton BJ, Zervos S, Webster JM (2000). "Ecological factors in schistosome transmission, and an environmentally benign method for controlling snails in a recreational lake with a record of schistosome dermatitis". Parasitol. Int. 49 (1): 9–17. doi:10.1016/S1383-5769(99)00034-3. PMID 10729712.
- ↑ Verbrugge LM, Rainey JJ, Reimink RL, Blankespoor HD (2004). "Prospective study of swimmer's itch incidence and severity". J. Parasitol. 90 (4): 697–704. doi:10.1645/GE-237R. PMID 15357056. S2CID 43205388.
- ↑ Blankespoor, H. D., Reimink, R. L. (1991). "The control of swimmer's itch in Michigan: Past, present, and future". Michigan Academician. 24 (1): 7–23.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Blankespoor, C. L., Reimink, R. L., Blankespoort, H. D. (2001). "Efficacy of praziquantel in treating natural schistosome infections in common mergansers". Journal of Parasitology. 87 (2): 424–6. doi:10.1645/0022-3395(2001)087[0424:EOPITN]2.0.CO;2. PMID 11318576.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Salafsky, B., Ramaswamy, K., He, Y. X., Li, J., Shibuya, T. (November 1999). "Development and evaluation of LIPODEET, a new long-acting formulation of N, N-diethyl-m-toluamide (DEET) for the prevention of schistosomiasis". Am. J. Trop. Med. Hyg. 61 (5): 743–50. doi:10.4269/ajtmh.1999.61.743. PMID 10586906.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ "Swimmer's Itch Reported at Lakes". Bureau of Land Management. Archived from the original on 2021-04-13. Retrieved 2021-06-05.
External links
| Classification |
|---|
- Pages with script errors
- CS1 maint: multiple names: authors list
- All articles with unsourced statements
- Articles with unsourced statements from June 2021
- Articles with invalid date parameter in template
- Articles with unsourced statements from January 2021
- Parasitic infestations, stings, and bites of the skin
- Inflammations
- Helminthiases
- Zoonoses
- Swimming culture
- RTT