Subacute bacterial endocarditis
| Subacute bacterial endocarditis | |
|---|---|
| Other names: Endocarditis lenta | |
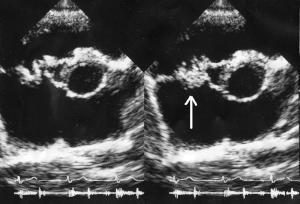 | |
| Vegetation of tricuspid valve by ECHO | |
| Symptoms | Malaise, weakness[1] |
| Causes | Streptococcus mutans, mitis, sanguis or milleri bacteria[2][3] |
| Diagnostic method | Blood culture specimens over 24-hour period/analysis[4] |
| Treatment | Intravenous penicillin[2] |
Subacute bacterial endocarditis, abbreviated SBE, is a type of endocarditis (more specifically, infective endocarditis).[5] Subacute bacterial endocarditis can be considered a form of type III hypersensitivity.[6]
Signs and symptoms

Among the signs ands symptoms of subacute bacterial endocarditis are the folowing:[1][7]
Causes
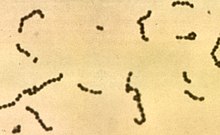
It is usually caused by a form of Viridans group streptococcus bacteria that normally live in the mouth[3] (Streptococcus mutans, mitis, sanguis or milleri).[2]
Other strains of streptococci can cause subacute endocarditis as well. These include streptococcus intermedius, which can cause acute or subacute infection (about 15% of cases pertaining to infective endocarditis).[8]
Enterococci from urinary tract infections and coagulase negative staphylococci can also be causative agents.[5]
Mechanism
The mechanism of subacute bacterial endocarditis could be due to malformed stenotic valves which in the company of bacteremia, become infected, via adhesion and subsequent colonization of the surface area. This causes an inflammatory response, with recruitment of matrix metalloproteinases, and destruction of collagen.[9]
Underlying structural valve disease is usually present in patients before developing subacute endocarditis, and is less likely to lead to septic emboli than is acute endocarditis, but subacute endocarditis has a relatively slow process of infection and, if left untreated, can worsen for up to one year before it is fatal.[medical citation needed] In cases of subacute bacterial endocarditis, the causative organism (streptococcus viridans) needs a previous heart valve disease to colonize.[10] On the other hand, in cases of acute bacterial endocarditis, the organism can colonize on the healthy heart valve, causing the disease.[11]
Diagnosis
Diagnosis of subacute bacterial endocarditis can be done by collecting three blood culture specimens over a 24-hour period for analysis,[4] also it can usually be indicated by the existence of:
Treatment
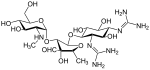
The standard treatment is with a minimum of four weeks of high-dose intravenous penicillin with an aminoglycoside such as gentamicin. The use of high-dose antibiotics is largely based upon animal models.[2]
Leo Loewe of Brooklyn Jewish Hospital was the first to successfully treat subacute bacterial endocarditis with penicillin. Loewe reported at the time seven cases of subacute bacterial endocarditis in 1944.[15]
References
- ↑ 1.0 1.1 Jefferson, James W. (2012-12-06). Neuropsychiatric Features of Medical Disorders. Springer Science & Business Media. p. 28. ISBN 9781468439205. Archived from the original on 2016-06-23. Retrieved 2021-07-18.
- ↑ 2.0 2.1 2.2 2.3 Verhagen, DW; Vedder, AC; Speelman, P; van der Meer, JT (2006). "Antimicrobial treatment of infective endocarditis caused by viridans streptococci highly susceptible to penicillin: historic overview and future considerations". The Journal of Antimicrobial Chemotherapy. 57 (5): 819–24. doi:10.1093/jac/dkl087. PMID 16549513.
- ↑ 3.0 3.1 deWit, Susan C.; Kumagai, Candice K. (2014-04-14). Medical-Surgical Nursing: Concepts & Practice. Elsevier Health Sciences. p. 101. ISBN 9780323293211. Archived from the original on 2016-06-03. Retrieved 2021-07-18.
- ↑ 4.0 4.1 Engelkirk, Paul G.; Duben-Engelkirk, Janet L. (2008-01-01). Laboratory Diagnosis of Infectious Diseases: Essentials of Diagnostic Microbiology. Lippincott Williams & Wilkins. p. 446. ISBN 9780781797016. Archived from the original on 2021-09-01. Retrieved 2021-07-18.
- ↑ 5.0 5.1 "Infective Endocarditis. Information; prevention of endocarditis | Patient". Patient. Archived from the original on 2019-05-22. Retrieved 2015-08-28.
- ↑ Keogan, Mary; Wallace, Eleanor M.; O'Leary, Paula (2006-04-18). Concise Clinical Immunology for Healthcare Professionals. Routledge. p. 106. ISBN 9781134428021. Archived from the original on 2016-05-11. Retrieved 2021-07-18.
- ↑ Sethi, Karishna; Buckley, Jim; de Wolff, Jacob (September 2013). "Splinter haemorrhages, Osler's nodes, Janeway lesions and Roth spots: the peripheral stigmata of endocarditis". British Journal of Hospital Medicine (London, England: 2005). 74 (9): C139–142. ISSN 1750-8460. Archived from the original on 12 May 2021. Retrieved 1 September 2021.
- ↑ "Endocarditis". The Lecturio Medical Concept Library. Archived from the original on 18 July 2021. Retrieved 18 July 2021.
- ↑ Pathology of Infectious Endocarditis at eMedicine
- ↑ Pommerville, Jeffrey C. (2012-01-15). Alcamo's Fundamentals of Microbiology: Body Systems Edition. Jones & Bartlett Publishers. p. 768. ISBN 9781449605940. Archived from the original on 2016-06-10. Retrieved 2021-07-18.
- ↑ Copstead-Kirkhorn, Lee-Ellen C.; Banasik, Jacquelyn L. (2014-06-25). Pathophysiology. Elsevier Health Sciences. p. 395. ISBN 9780323293174. Archived from the original on 2020-08-11. Retrieved 2021-07-18.
- ↑ Kahan, Scott (2008-03-01). Signs and Symptoms. Lippincott Williams & Wilkins. p. 234. ISBN 9780781770439. Archived from the original on 2016-05-02. Retrieved 2021-07-18.
- ↑ Diepenbrock, Nancy H. (2011-02-15). Quick Reference to Critical Care. Lippincott Williams & Wilkins. p. 391. ISBN 9781608314645. Archived from the original on 2016-05-29. Retrieved 2021-07-18.
- ↑ Clubbing of the Nails~clinical at eMedicine
- ↑ Loewe, Leo (1944). "Combined penicillin and heparin therapy of subacute bacterial endocarditis". Journal of the American Medical Association. 124 (3): 270–272. doi:10.1001/jama.1944.02850030012003. PMC 1871521. PMID 19312479.
Further references
- Goolsby, Mary Jo; Grubbs, Laurie (2011-04-28). Advanced Assessment: Interpreting Findings and Formulating Differential Diagnoses. F.A. Davis. ISBN 9780803625174. Archived from the original on 2016-05-10. Retrieved 2021-07-18.
- Silverman, Sol; Eversole, Lewis R.; Truelove, Edmond L. (2002-01-01). Essentials of Oral Medicine. PMPH-USA. ISBN 9781550091465. Archived from the original on 2016-05-12. Retrieved 2021-07-18.
- Kiefer, TL; Bashore, TM (2012). "Infective endocarditis: a comprehensive overview". Reviews in Cardiovascular Medicine. 13 (2–3): e105–20. PMID 23160159.
External links
| Classification |
|---|