Skin cancer
| Skin cancer | |
|---|---|
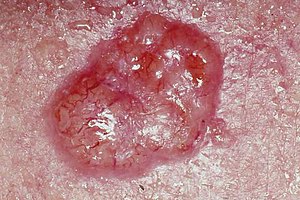 | |
| A basal-cell skin cancer. Note the pearly appearance and telangiectasia. | |
| Specialty | Oncology and dermatology |
| Symptoms | Basal-cell: painless raised area of skin that may be shiny with small blood vessel running over it or ulceration[1] Squamous-cell: hard lump with a scaly top[2] Melanoma: mole that has changed in size, shape, color, or has irregular edges[3] |
| Types | Basal-cell skin cancer (BCC), squamous-cell skin cancer (SCC), melanoma[1] |
| Causes | Ultraviolet radiation from the Sun or tanning beds[4] |
| Risk factors | Light skin, poor immune function[1][5] |
| Diagnostic method | Tissue biopsy[3] |
| Prevention | Decreasing exposure to ultraviolet radiation, sunscreen[6][7] |
| Treatment | Surgery, radiation therapy, fluorouracil[1] |
| Frequency | 5.6 million (2015)[8] |
| Deaths | 111,700 (2015)[9] |
Skin cancers are cancers that arise from the skin. They are due to the development of abnormal cells that have the ability to invade or spread to other parts of the body.[10] There are three main types of skin cancers: basal-cell skin cancer (BCC), squamous-cell skin cancer (SCC) and melanoma.[1] The first two, along with a number of less common skin cancers, are known as nonmelanoma skin cancer (NMSC).[5][11] Basal-cell cancer grows slowly and can damage the tissue around it but is unlikely to spread to distant areas or result in death.[5] It often appears as a painless raised area of skin that may be shiny with small blood vessels running over it or may present as a raised area with an ulcer.[1] Squamous-cell skin cancer is more likely to spread.[5] It usually presents as a hard lump with a scaly top but may also form an ulcer.[2] Melanomas are the most aggressive. Signs include a mole that has changed in size, shape, color, has irregular edges, has more than one color, is itchy or bleeds.[3]
More than 90% of cases are caused by exposure to ultraviolet radiation from the Sun.[4] This exposure increases the risk of all three main types of skin cancer.[4] Exposure has increased, partly due to a thinner ozone layer.[5][12] Tanning beds are another common source of ultraviolet radiation.[4] For melanomas and basal-cell cancers, exposure during childhood is particularly harmful.[6] For squamous-cell skin cancers, total exposure, irrespective of when it occurs, is more important.[4] Between 20% and 30% of melanomas develop from moles.[6] People with lighter skin are at higher risk[1][13] as are those with poor immune function such as from medications or HIV/AIDS.[5][14] Diagnosis is by biopsy.[3]
Decreasing exposure to ultraviolet radiation and the use of sunscreen appear to be effective methods of preventing melanoma and squamous-cell skin cancer.[6][7] It is not clear if sunscreen affects the risk of basal-cell cancer.[7] Nonmelanoma skin cancer is usually curable.[5] Treatment is generally by surgical removal but may, less commonly, involve radiation therapy or topical medications such as fluorouracil.[1] Treatment of melanoma may involve some combination of surgery, chemotherapy, radiation therapy and targeted therapy.[3] In those people whose disease has spread to other areas of the body, palliative care may be used to improve quality of life.[3] Melanoma has one of the higher survival rates among cancers, with over 86% of people in the UK and more than 90% in the United States surviving more than 5 years.[15][16]
Skin cancer is the most common form of cancer, globally accounting for at least 40% of cancer cases.[5][17] The most common type is nonmelanoma skin cancer, which occurs in at least 2–3 million people per year.[6][18] This is a rough estimate, however, as good statistics are not kept.[1] Of nonmelanoma skin cancers, about 80% are basal-cell cancers and 20% squamous-cell skin cancers.[11] Basal-cell and squamous-cell skin cancers rarely result in death.[6] In the United States, they were the cause of less than 0.1% of all cancer deaths.[1] Globally in 2012, melanoma occurred in 232,000 people and resulted in 55,000 deaths.[6] White people in Australia, New Zealand and South Africa have the highest rates of melanoma in the world.[6][19] The three main types of skin cancer have become more common in the last 20 to 40 years, especially in those areas with mostly White people.[5][6]
Classification
There are three main types of skin cancer: basal-cell skin cancer (basal-cell carcinoma) (BCC), squamous-cell skin cancer (squamous-cell carcinoma) (SCC) and malignant melanoma.
| Cancer | Description | Illustration |
|---|---|---|
| Basal-cell carcinoma | Note the pearly translucency to fleshy color, tiny blood vessels on the surface, and sometimes ulceration which can be characteristics. The key term is translucency. | 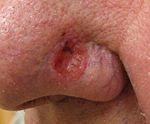 |
| Squamous-cell skin carcinoma | Commonly presents as a red, crusted, or scaly patch or bump. Often a very rapidly growing tumor. |  |
| Malignant melanoma | These are commonly asymmetrical in shape and/or pigment distribution, with an irregular border, color variation, and often greater than 6 mm diameter.[20] |  |
Basal-cell carcinomas are most commonly present on sun-exposed areas of the skin, especially the face. They rarely metastasize and rarely cause death. They are easily treated with surgery or radiation. Squamous-cell skin cancers are also common, but much less common than basal-cell cancers. They metastasize more frequently than BCCs. Even then, the metastasis rate is quite low, with the exception of SCC of the lip, ear, and in people who are immunosuppressed. Melanoma are the least frequent of the three common skin cancers. They frequently metastasize, and potentially cause death once they spread.
Less common skin cancers include: dermatofibrosarcoma protuberans, Merkel cell carcinoma, Kaposi's sarcoma, keratoacanthoma, spindle cell tumors, sebaceous carcinomas, microcystic adnexal carcinoma, Paget's disease of the breast, atypical fibroxanthoma, leiomyosarcoma, and angiosarcoma.
BCC and SCC often carry a UV-signature mutation indicating that these cancers are caused by UVB radiation via direct DNA damage. However malignant melanoma is predominantly caused by UVA radiation via indirect DNA damage. The indirect DNA damage is caused by free radicals and reactive oxygen species. Research indicates that the absorption of three sunscreen ingredients into the skin, combined with a 60-minute exposure to UV, leads to an increase of free radicals in the skin, if applied in too little quantity and too infrequently.[21] However, the researchers add that newer creams often do not contain these specific compounds, and that the combination of other ingredients tends to retain the compounds on the surface of the skin. They also add that frequent re-application reduces the risk of radical formation.
Signs and symptoms
There are a variety of different skin cancer symptoms. These include changes in the skin that do not heal, ulcering in the skin, discolored skin, and changes in existing moles, such as jagged edges to the mole and enlargement of the mole.
Basal-cell skin cancer
Basal-cell skin cancer (BCC) usually presents as a raised, smooth, pearly bump on the sun-exposed skin of the head, neck, torso or shoulders. Sometimes small blood vessels (called telangiectasia) can be seen within the tumor. Crusting and bleeding in the center of the tumor frequently develops. It is often mistaken for a sore that does not heal. This form of skin cancer is the least deadly, and with proper treatment can be completely eliminated, often without significant scarring.
Squamous-cell skin cancer
Squamous-cell skin cancer (SCC) is commonly a red, scaling, thickened patch on sun-exposed skin. Some are firm hard nodules and dome shaped like keratoacanthomas. Ulceration and bleeding may occur. When SCC is not treated, it may develop into a large mass. Squamous-cell is the second most common skin cancer. It is dangerous, but not nearly as dangerous as a melanoma.
Melanoma
Most melanoma consist of various colours from shades of brown to black. A small number of melanoma are pink, red or fleshy in colour; these are called amelanotic melanoma and tend to be more aggressive. Warning signs of malignant melanoma include change in the size, shape, color or elevation of a mole. Other signs are the appearance of a new mole during adulthood or pain, itching, ulceration, redness around the site, or bleeding at the site. An often-used mnemonic is "ABCDE", where A is for "asymmetrical", B for "borders" (irregular: "Coast of Maine sign"), C for "color" (variegated), D for "diameter" (larger than 6 mm – the size of a pencil eraser) and E for "evolving."[22][23]
Other
Merkel cell carcinomas are most often rapidly growing, non-tender red, purple or skin colored bumps that are not painful or itchy. They may be mistaken for a cyst or another type of cancer.[24]
Causes
Ultraviolet radiation from sun exposure is the primary environmental cause of skin cancer.[25][26][27] This can occur in professions such as farming. Other risk factors that play a role include:
- Light skin color [26]
- Age [26]
- Smoking tobacco[26]
- HPV infections increase the risk of squamous-cell skin cancer.[26]
- Some genetic syndromes[26] including congenital melanocytic nevi syndrome which is characterized by the presence of nevi (birthmarks or moles) of varying size which are either present at birth, or appear within 6 months of birth. Nevi larger than 20 mm (3/4") in size are at higher risk for becoming cancerous.
- Chronic non-healing wounds.[26] These are called Marjolin's ulcers based on their appearance, and can develop into squamous-cell skin cancer.
- Ionizing radiation such as X-rays, environmental carcinogens, and artificial UV radiation (e.g. tanning beds).[26] It is believed that tanning beds are the cause of hundreds of thousands of basal and squamous-cell skin cancer.[28] The World Health Organization now places people who use artificial tanning beds in its highest risk category for skin cancer.[29] Alcohol consumption, specifically excessive drinking increase the risk of sunburns.[30]
- The use of many immunosuppressive medications increases the risk of skin cancer. Cyclosporin A, a calcineurin inhibitor for example increases the risk approximately 200 times, and azathioprine about 60 times.[31]
Pathophysiology
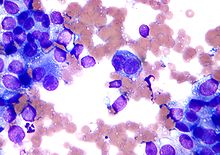
A malignant epithelial tumor that primarily originates in the epidermis, in squamous mucosa or in areas of squamous metaplasia is referred to as a squamous-cell carcinoma.[32]
Macroscopically, the tumor is often elevated, fungating, or may be ulcerated with irregular borders. Microscopically, tumor cells destroy the basement membrane and form sheets or compact masses which invade the subjacent connective tissue (dermis). In well differentiated carcinomas, tumor cells are pleomorphic/atypical, but resembling normal keratinocytes from prickle layer (large, polygonal, with abundant eosinophilic (pink) cytoplasm and central nucleus).[32]
Their disposal tends to be similar to that of normal epidermis: immature/basal cells at the periphery, becoming more mature to the centre of the tumor masses. Tumor cells transform into keratinized squamous cells and form round nodules with concentric, laminated layers, called "cell nests" or "epithelial/keratinous pearls". The surrounding stroma is reduced and contains inflammatory infiltrate (lymphocytes). Poorly differentiated squamous carcinomas contain more pleomorphic cells and no keratinization.[32]
A molecular factor involved in the disease process is mutation in gene PTCH1 that plays an important role in the Sonic hedgehog signaling pathway.[33]
Diagnosis
Diagnosis is by biopsy and histopathological examination.[3]
Non-invasive skin cancer detection methods include photography, dermatoscopy, sonography, confocal microscopy, Raman spectroscopy, fluorescence spectroscopy, terahertz spectroscopy, optical coherence tomography, the multispectral imaging technique, thermography, electrical bio-impedance, tape stripping and computer-aided analysis.[34]
Dermatoscopy may be useful in diagnosing basal cell carcinoma in addition to skin inspection.[35]
There is insufficient evidence that optical coherence tomography (OCT) is useful in diagnosing melanoma or squamous cell carcinoma. OCT may have a role in diagnosing basal cell carcinoma but more data is needed to support this.[36]
Computer-assisted diagnosis devices have been developed that analyze images from a dermatoscope or spectroscopy and can be used by a diagnostician to aid in the detection of skin cancer. CAD systems have been found to be highly sensitive in the detection of melanoma, but have a high false-positive rate. There is not yet enough evidence to recommend CAD as compared to traditional diagnostic methods.[37]
High-frequency ultrasound (HFUS) is of unclear usefulness in the diagnosis of skin cancer.[38] There is insufficient evidence for reflectance confocal microscopy to diagnose basal cell or squamous cell carcinoma or any other skin cancers.[39]
Prevention
Sunscreen is effective and thus recommended to prevent melanoma[40] and squamous-cell carcinoma.[41] There is little evidence that it is effective in preventing basal-cell carcinoma.[42] Other advice to reduce rates of skin cancer includes avoiding sunburning, wearing protective clothing, sunglasses and hats, and attempting to avoid sun exposure or periods of peak exposure.[43] The U.S. Preventive Services Task Force recommends that people between 9 and 25 years of age be advised to avoid ultraviolet light.[44]
The risk of developing skin cancer can be reduced through decreasing indoor tanning and mid day sun exposure, increasing the use of sunscreen,[44] and avoiding the use of tobacco products.
There is insufficient evidence either for or against screening for skin cancers.[45] Vitamin supplements and antioxidant supplements have not been found to have an effect in prevention.[46] Evidence for reducing melanoma risk from dietary measures is tentative, with some supportive epidemiological evidence, but no clinical trials.[47]
Zinc oxide and titanium oxide are often used in sun screen to provide broad protection from UVA and UVB ranges.[48]
Eating certain foods may decrease the risk of sunburns but this is much less than the protection provided by sunscreen.[49]
A meta-analysis of skin cancer prevention in high risk individuals found evidence that topical application of T4N5 liposome lotion reduced the rate of appearance of basal cell carcinomas in people with xeroderma pigmentosum, and that acitretin taken by mouth may have a skin protective benefit in people following kidney transplant.[50]
Treatment
Treatment is dependent on the specific type of cancer, location of the cancer, age of the person, and whether the cancer is primary or a recurrence. For a small basal-cell cancer in a young person, the treatment with the best cure rate (Mohs surgery or CCPDMA) might be indicated. In the case of an elderly frail man with multiple complicating medical problems, a difficult to excise basal-cell cancer of the nose might warrant radiation therapy (slightly lower cure rate) or no treatment at all. Topical chemotherapy might be indicated for large superficial basal-cell carcinoma for good cosmetic outcome, whereas it might be inadequate for invasive nodular basal-cell carcinoma or invasive squamous-cell carcinoma.[citation needed] In general, melanoma is poorly responsive to radiation or chemotherapy.
For low-risk disease, radiation therapy (external beam radiotherapy[51] or brachytherapy), topical chemotherapy (imiquimod or 5-fluorouracil) and cryotherapy (freezing the cancer off) can provide adequate control of the disease; all of them, however, may have lower overall cure rates than certain type of surgery. Other modalities of treatment such as photodynamic therapy, topical chemotherapy, electrodesiccation and curettage can be found in the discussions of basal-cell carcinoma and squamous-cell carcinoma.
Mohs' micrographic surgery (Mohs surgery) is a technique used to remove the cancer with the least amount of surrounding tissue and the edges are checked immediately to see if tumor is found. This provides the opportunity to remove the least amount of tissue and provide the best cosmetically favorable results. This is especially important for areas where excess skin is limited, such as the face. Cure rates are equivalent to wide excision. Special training is required to perform this technique. An alternative method is CCPDMA and can be performed by a pathologist not familiar with Mohs surgery.
In the case of disease that has spread (metastasized), further surgical procedures or chemotherapy may be required.[52]
Treatments for metastatic melanoma include biologic immunotherapy agents ipilimumab, pembrolizumab, and nivolumab; BRAF inhibitors, such as vemurafenib and dabrafenib; and a MEK inhibitor trametinib.[53]
Reconstruction
Currently, surgical excision is the most common form of treatment for skin cancers. The goal of reconstructive surgery is restoration of normal appearance and function. The choice of technique in reconstruction is dictated by the size and location of the defect. Excision and reconstruction of facial skin cancers is generally more challenging due to presence of highly visible and functional anatomic structures in the face.
When skin defects are small in size, most can be repaired with simple repair where skin edges are approximated and closed with sutures. This will result in a linear scar. If the repair is made along a natural skin fold or wrinkle line, the scar will be hardly visible. Larger defects may require repair with a skin graft, local skin flap, pedicled skin flap, or a microvascular free flap. Skin grafts and local skin flaps are by far more common than the other listed choices.
Skin grafting is patching of a defect with skin that is removed from another site in the body. The skin graft is sutured to the edges of the defect, and a bolster dressing is placed atop the graft for seven to ten days, to immobilize the graft as it heals in place. There are two forms of skin grafting: split thickness and full thickness. In a split thickness skin graft, a shaver is used to shave a layer of skin from the abdomen or thigh. The donor site regenerates skin and heals over a period of two weeks. In a full thickness skin graft, a segment of skin is totally removed and the donor site needs to be sutured closed.[54]
Split thickness grafts can be used to repair larger defects, but the grafts are inferior in their cosmetic appearance. Full thickness skin grafts are more acceptable cosmetically. However, full thickness grafts can only be used for small or moderate sized defects.
Local skin flaps are a method of closing defects with tissue that closely matches the defect in color and quality. Skin from the periphery of the defect site is mobilized and repositioned to fill the deficit. Various forms of local flaps can be designed to minimize disruption to surrounding tissues and maximize cosmetic outcome of the reconstruction. Pedicled skin flaps are a method of transferring skin with an intact blood supply from a nearby region of the body. An example of such reconstruction is a pedicled forehead flap for repair of a large nasal skin defect. Once the flap develops a source of blood supply form its new bed, the vascular pedicle can be detached.[55]
Prognosis
The mortality rate of basal-cell and squamous-cell carcinoma is around 0.3%, causing 2000 deaths per year in the US. In comparison, the mortality rate of melanoma is 15–20% and it causes 6500 deaths per year.[56]: 29, 31 Even though it is much less common, malignant melanoma is responsible for 75% of all skin cancer-related deaths.[57]
The survival rate for people with melanoma depends upon when they start treatment. The cure rate is very high when melanoma is detected in early stages, when it can easily be removed surgically. The prognosis is less favorable if the melanoma has spread to other parts of the body.[58] As of 2003 the overall five-year cure rate with Mohs' micrographic surgery was around 95 percent for recurrent basal cell carcinoma.[59]
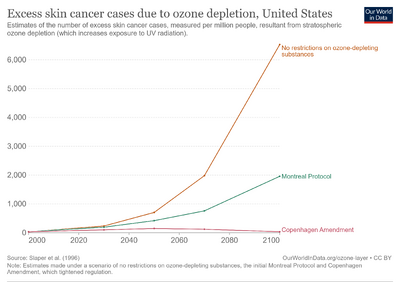
Australia and New Zealand exhibit one of the highest rates of skin cancer incidence in the world, almost four times the rates registered in the United States, the UK and Canada. Around 434,000 people receive treatment for non-melanoma skin cancers and 10,300 are treated for melanoma. Melanoma is the most common type of cancer in people between 15–44 years in both countries. The incidence of skin cancer has been increasing.[60] The incidence of melanoma among Auckland residents of European descent in 1995 was 77.7 cases per 100,000 people per year, and was predicted to increase in the 21st century because of "the effect of local stratospheric ozone depletion and the time lag from sun exposure to melanoma development."[61]
Epidemiology

| no data <0.7 0.7–1.4 1.4–2.1 2.1–2.8 2.8–3.5 3.5–4.2 | 4.2–4.9 4.9–5.6 5.6–6.3 6.3–7 7–7.7 >7.7 |
Skin cancers result in 80,000 deaths a year as of 2010, 49,000 of which are due to melanoma and 31,000 of which are due to non-melanoma skin cancers.[63] This is up from 51,000 in 1990.[63]
More than 3.5 million cases of skin cancer are diagnosed annually in the United States, which makes it the most common form of cancer in that country. One in five Americans will develop skin cancer at some point of their lives. The most common form of skin cancer is basal-cell carcinoma, followed by squamous cell carcinoma. Unlike for other cancers, there exists no basal and squamous cell skin cancers registry in the United States.[64]
Melanoma
In the US in 2008, 59,695 people were diagnosed with melanoma, and 8,623 people died from it.[65] In Australia more than 12,500 new cases of melanoma are reported each year, out of which more than 1,500 die from the disease. Australia has the highest per capita incidence of melanoma in the world.[66]
Although the rates of many cancers in the United States is falling, the incidence of melanoma keeps growing, with approximately 68,729 melanomas diagnosed in 2004 according to reports of the National Cancer Institute.[67]
Melanoma is the fifth most common cancer in the UK (around 13,300 people were diagnosed with melanoma in 2011), and the disease accounts for 1% all cancer deaths (around 2,100 people died in 2012).[68]
Non-melanoma
Approximately 2,000 people die from basal or squamous cell skin cancers (non-melanoma skin cancers) in the United States each year. The rate has dropped in recent years. Most of the deaths happen to people who are elderly and might not have seen a doctor until the cancer had spread; and people with immune system disorders.[64]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 "Skin Cancer Treatment (PDQ®)". NCI. 25 October 2013. Archived from the original on 5 July 2014. Retrieved 30 June 2014.
- ↑ 2.0 2.1 Dunphy, Lynne M (2011). Primary Care: The Art and Science of Advanced Practice Nursing. F.A. Davis. p. 242. ISBN 9780803626478. Archived from the original on 20 May 2016.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 "General Information About Melanoma". NCI. 17 April 2014. Archived from the original on 5 July 2014. Retrieved 30 June 2014.
- ↑ 4.0 4.1 4.2 4.3 4.4 Gallagher RP, Lee TK, Bajdik CD, Borugian M (2010). "Ultraviolet radiation". Chronic Diseases in Canada. 29 Suppl 1: 51–68. PMID 21199599.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 Cakir BÖ, Adamson P, Cingi C (November 2012). "Epidemiology and economic burden of nonmelanoma skin cancer". Facial Plastic Surgery Clinics of North America. 20 (4): 419–22. doi:10.1016/j.fsc.2012.07.004. PMID 23084294.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 6.8 World Cancer Report 2014. World Health Organization. 2014. pp. Chapter 5.14. ISBN 978-9283204299.
- ↑ 7.0 7.1 7.2 Jou PC, Feldman RJ, Tomecki KJ (June 2012). "UV protection and sunscreens: what to tell patients". Cleveland Clinic Journal of Medicine. 79 (6): 427–36. doi:10.3949/ccjm.79a.11110. PMID 22660875.
- ↑ GBD 2015 Disease Injury Incidence Prevalence Collaborators (October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ↑ GBD 2015 Mortality Causes of Death Collaborators (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ↑ "Defining Cancer". National Cancer Institute. 17 September 2007. Archived from the original on 25 June 2014. Retrieved 10 June 2014.
- ↑ 11.0 11.1 Marsden, edited by Sajjad Rajpar, Jerry (2008). ABC of skin cancer. Malden, Mass.: Blackwell Pub. pp. 5–6. ISBN 9781444312508. Archived from the original on 29 April 2016.
- ↑ Maverakis E, Miyamura Y, Bowen MP, Correa G, Ono Y, Goodarzi H (May 2010). "Light, including ultraviolet". Journal of Autoimmunity. 34 (3): J247-57. doi:10.1016/j.jaut.2009.11.011. PMC 2835849. PMID 20018479.
- ↑ Leiter U, Garbe C (2008). "Epidemiology of melanoma and nonmelanoma skin cancer--the role of sunlight". Advances in Experimental Medicine and Biology. 624: 89–103. doi:10.1007/978-0-387-77574-6_8. ISBN 978-0-387-77573-9. PMID 18348450.
- ↑ Chiao EY, Krown SE (September 2003). "Update on non-acquired immunodeficiency syndrome-defining malignancies". Current Opinion in Oncology. 15 (5): 389–97. doi:10.1097/00001622-200309000-00008. PMID 12960522.
- ↑ "SEER Stat Fact Sheets: Melanoma of the Skin". NCI. Archived from the original on 6 July 2014. Retrieved 18 June 2014.
- ↑ "Release: Cancer Survival Rates, Cancer Survival in England, Patients Diagnosed 2005–2009 and Followed up to 2010". Office for National Statistics. 15 November 2011. Archived from the original on 17 October 2014. Retrieved 30 June 2014.
- ↑ Dubas LE, Ingraffea A (February 2013). "Nonmelanoma skin cancer". Facial Plastic Surgery Clinics of North America. 21 (1): 43–53. doi:10.1016/j.fsc.2012.10.003. PMID 23369588.
- ↑ "How common is skin cancer?". World Health Organization. Archived from the original on 27 September 2010. Retrieved 30 June 2014.
- ↑ Harris, Randall E. (2013). Epidemiology of Chronic Disease. Jones & Bartlett Publishers. p. 271. ISBN 9780763780470. Archived from the original on 28 September 2018. Retrieved 27 September 2018.
- ↑ "Malignant Melanoma: eMedicine Dermatology". 31 January 2019. Archived from the original on 7 October 2010.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Hanson KM, Gratton E, Bardeen CJ (October 2006). "Sunscreen enhancement of UV-induced reactive oxygen species in the skin" (PDF). Free Radical Biology & Medicine. 41 (8): 1205–12. doi:10.1016/j.freeradbiomed.2006.06.011. PMID 17015167. Archived (PDF) from the original on 14 March 2020. Retrieved 23 September 2019.
- ↑ "What You Need To Know About: Melanoma and Other Skin Cancers" (PDF). National Cancer Institute. Archived (PDF) from the original on 18 March 2013.
- ↑ "Melanoma Skin Cancer" (PDF). American Cancer Society. 2012. Archived (PDF) from the original on 9 September 2013.
- ↑ Bickle K, Glass LF, Messina JL, Fenske NA, Siegrist K (March 2004). "Merkel cell carcinoma: a clinical, histopathologic, and immunohistochemical review". Seminars in Cutaneous Medicine and Surgery. 23 (1): 46–53. doi:10.1016/s1085-5629(03)00087-7. PMID 15095915.
- ↑ Narayanan DL, Saladi RN, Fox JL (September 2010). "Ultraviolet radiation and skin cancer". International Journal of Dermatology. 49 (9): 978–86. doi:10.1111/j.1365-4632.2010.04474.x. PMID 20883261.
- ↑ 26.0 26.1 26.2 26.3 26.4 26.5 26.6 26.7 Saladi RN, Persaud AN (January 2005). "The causes of skin cancer: a comprehensive review". Drugs of Today. 41 (1): 37–53. doi:10.1358/dot.2005.41.1.875777. PMID 15753968.
- ↑ Gordon R (August 2013). "Skin cancer: an overview of epidemiology and risk factors". Seminars in Oncology Nursing. 29 (3): 160–9. doi:10.1016/j.soncn.2013.06.002. PMID 23958214.
- ↑ Wehner MR, Shive ML, Chren MM, Han J, Qureshi AA, Linos E (October 2012). "Indoor tanning and non-melanoma skin cancer: systematic review and meta-analysis". BMJ. 345: e5909. doi:10.1136/bmj.e5909. PMC 3462818. PMID 23033409.
- ↑ Arndt KA (2010). Skin Care and Repair. Chestnut Hill, MA: Harvard Health Publications.
- ↑ Saladi RN, Nektalova T, Fox JL (January 2010). "Induction of skin carcinogenicity by alcohol and ultraviolet light". Clinical and Experimental Dermatology. 35 (1): 7–11. doi:10.1111/j.1365-2230.2009.03465.x. PMID 19778305.
- ↑ Kuschal C, Thoms KM, Schubert S, Schäfer A, Boeckmann L, Schön MP, Emmert S (January 2012). "Skin cancer in organ transplant recipients: effects of immunosuppressive medications on DNA repair". Experimental Dermatology. 21 (1): 2–6. doi:10.1111/j.1600-0625.2011.01413.x. PMID 22151386.
- ↑ 32.0 32.1 32.2 "Squamous cell carcinoma (epidermoid carcinoma) – skin". Atlas of Pathology (3rd ed.). Universitatii St., Iasi, Romania. Archived from the original on 10 March 2009. Retrieved 21 July 2007.
- ↑ Kormi SM, Ardehkhani S (2012). "Non-melanoma Skin Cancer: Mini Review". Cancer. 166 (5): 1069–80. doi:10.15562/tcp.40.
- ↑ Narayanamurthy V, Padmapriya P, Noorasafrin A, Pooja B, Hema K, Nithyakalyani K, Samsuri F (2018). "Skin cancer detection using non-invasive techniques". RSC Advances. 8 (49): 28095–28130. doi:10.1039/c8ra04164d.
- ↑ Dinnes J, Deeks JJ, Chuchu N, Matin RN, Wong KY, Aldridge RB, et al. (Cochrane Skin Group) (December 2018). "Visual inspection and dermoscopy, alone or in combination, for diagnosing keratinocyte skin cancers in adults". The Cochrane Database of Systematic Reviews. 12: CD011901. doi:10.1002/14651858.CD011901.pub2. PMC 6516870. PMID 30521688.
- ↑ Ferrante di Ruffano L, Dinnes J, Deeks JJ, Chuchu N, Bayliss SE, Davenport C, et al. (Cochrane Skin Group) (December 2018). "Optical coherence tomography for diagnosing skin cancer in adults". The Cochrane Database of Systematic Reviews. 12: CD013189. doi:10.1002/14651858.CD013189. PMC 6516952. PMID 30521690.
- ↑ Ferrante di Ruffano L, Takwoingi Y, Dinnes J, Chuchu N, Bayliss SE, Davenport C, et al. (December 2018). "Computer-assisted diagnosis techniques (dermoscopy and spectroscopy-based) for diagnosing skin cancer in adults". The Cochrane Database of Systematic Reviews. 12: CD013186. doi:10.1002/14651858.cd013186. PMC 6517147. PMID 30521691.
- ↑ Dinnes J, Bamber J, Chuchu N, Bayliss SE, Takwoingi Y, Davenport C, et al. (December 2018). "High-frequency ultrasound for diagnosing skin cancer in adults". The Cochrane Database of Systematic Reviews. 12: CD013188. doi:10.1002/14651858.cd013188. PMC 6516989. PMID 30521683.
- ↑ Dinnes J, Deeks JJ, Chuchu N, Saleh D, Bayliss SE, Takwoingi Y, et al. (Cochrane Skin Group) (December 2018). "Reflectance confocal microscopy for diagnosing keratinocyte skin cancers in adults". The Cochrane Database of Systematic Reviews. 12: CD013191. doi:10.1002/14651858.CD013191. PMC 6516892. PMID 30521687.
- ↑ Kanavy HE, Gerstenblith MR (December 2011). "Ultraviolet radiation and melanoma". Seminars in Cutaneous Medicine and Surgery. 30 (4): 222–8. doi:10.1016/j.sder.2011.08.003. PMID 22123420.
- ↑ Burnett ME, Wang SQ (April 2011). "Current sunscreen controversies: a critical review". Photodermatology, Photoimmunology & Photomedicine. 27 (2): 58–67. doi:10.1111/j.1600-0781.2011.00557.x. PMID 21392107.
- ↑ Kütting B, Drexler H (December 2010). "UV-induced skin cancer at workplace and evidence-based prevention". International Archives of Occupational and Environmental Health. 83 (8): 843–54. doi:10.1007/s00420-010-0532-4. PMID 20414668.
- ↑ Balk SJ (March 2011). "Ultraviolet radiation: a hazard to children and adolescents". Pediatrics. 127 (3): 588–97. doi:10.1542/peds.2010-3501. PMID 21357336.
- ↑ 44.0 44.1 Lin JS, Eder M, Weinmann S (February 2011). "Behavioral counseling to prevent skin cancer: a systematic review for the U.S. Preventive Services Task Force". Annals of Internal Medicine. 154 (3): 190–201. CiteSeerX 10.1.1.690.6405. doi:10.7326/0003-4819-154-3-201102010-00009. PMID 21282699.
- ↑ Bibbins-Domingo K, Grossman DC, Curry SJ, Davidson KW, Ebell M, Epling JW, et al. (July 2016). "Screening for Skin Cancer: US Preventive Services Task Force Recommendation Statement". JAMA. 316 (4): 429–35. doi:10.1001/jama.2016.8465. PMID 27458948.
- ↑ Chang YJ, Myung SK, Chung ST, Kim Y, Lee EH, Jeon YJ, et al. (2011). "Effects of vitamin treatment or supplements with purported antioxidant properties on skin cancer prevention: a meta-analysis of randomized controlled trials". Dermatology. 223 (1): 36–44. doi:10.1159/000329439. PMID 21846961.
- ↑ Jensen JD, Wing GJ, Dellavalle RP (November–December 2010). "Nutrition and melanoma prevention". Clinics in Dermatology. 28 (6): 644–9. doi:10.1016/j.clindermatol.2010.03.026. PMID 21034988.
- ↑ Smijs TG, Pavel S (October 2011). "Titanium dioxide and zinc oxide nanoparticles in sunscreens: focus on their safety and effectiveness". Nanotechnology, Science and Applications. 4: 95–112. doi:10.2147/NSA.S19419. PMC 3781714. PMID 24198489.
- ↑ Stahl W, Sies H (November 2012). "β-Carotene and other carotenoids in protection from sunlight". The American Journal of Clinical Nutrition. 96 (5): 1179S–84S. doi:10.3945/ajcn.112.034819. PMID 23053552.
- ↑ Bath-Hextall F, Leonardi-Bee J, Somchand N, Webster A, Delitt J, Perkins W (October 2007). "Interventions for preventing non-melanoma skin cancers in high-risk groups". The Cochrane Database of Systematic Reviews (4): CD005414. doi:10.1002/14651858.CD005414.pub2. hdl:2123/22258. PMID 17943854. Archived from the original on 23 June 2018. Retrieved 23 June 2018.
- ↑ Hill R, Healy B, Holloway L, Kuncic Z, Thwaites D, Baldock C (March 2014). "Advances in kilovoltage x-ray beam dosimetry". Physics in Medicine and Biology. 59 (6): R183-231. Bibcode:2014PMB....59R.183H. doi:10.1088/0031-9155/59/6/r183. PMID 24584183.
- ↑ Doherty, Gerard M.; Mulholland, Michael W. (2005). Greenfield's Surgery: Scientific Principles And Practice. Baltimore: Williams & Wilkins. ISBN 978-0-7817-5626-6.
- ↑ Maverakis E, Cornelius LA, Bowen GM, Phan T, Patel FB, Fitzmaurice S, et al. (May 2015). "Metastatic melanoma - a review of current and future treatment options". Acta Dermato-Venereologica. 95 (5): 516–24. doi:10.2340/00015555-2035. PMID 25520039. Archived from the original on 19 July 2018. Retrieved 16 May 2018.
- ↑ Khosh, Maurice M (2 February 2019). "Skin Grafts, Full-Thickness". eMedicine. Archived from the original on 9 March 2009.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Skin Cancer Reconstruction Archived 10 July 2011 at archive.today
- ↑ Boring CC, Squires TS, Tong T (1991). "Cancer statistics, 1991". Ca. 41 (1): 19–36. doi:10.3322/canjclin.41.1.19. PMID 1984806.
- ↑ Jerant AF, Johnson JT, Sheridan CD, Caffrey TJ (July 2000). "Early detection and treatment of skin cancer". American Family Physician. 62 (2): 357–68, 375–6, 381–2. PMID 10929700. Archived from the original on 24 July 2008.
- ↑ "Malignant Melanoma Cancer". Archived from the original on 23 March 2010. Retrieved 2 July 2010.
- ↑ Wong CS, Strange RC, Lear JT (October 2003). "Basal cell carcinoma". BMJ. 327 (7418): 794–8. doi:10.1136/bmj.327.7418.794. PMC 214105. PMID 14525881.
- ↑ "Skin Cancer Facts and Figures". Archived from the original on 10 August 2012. Retrieved 1 December 2013.
From 1982 to 2007 melanoma diagnoses increased by around 50%. From 1998 to 2007, GP consultations to treat non-melanoma skin cancer increased by 14%, to reach 950,000 visits each year.
- ↑ Jones WO, Harman CR, Ng AK, Shaw JH (July 1999). "Incidence of malignant melanoma in Auckland, New Zealand: highest rates in the world". World Journal of Surgery. 23 (7): 732–5. doi:10.1007/pl00012378. PMID 10390596. Archived from the original on 3 December 2013.
- ↑ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 11 November 2009. Retrieved 11 November 2009.
- ↑ 63.0 63.1 Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, et al. (December 2012). "Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010" (PDF). Lancet. 380 (9859): 2095–128. doi:10.1016/S0140-6736(12)61728-0. hdl:10536/DRO/DU:30050819. PMID 23245604. Archived (PDF) from the original on 1 August 2020. Retrieved 3 September 2019.
- ↑ 64.0 64.1 "Key statistics for basal and squamous cell skin cancers". www.cancer.org. American Cancer Society. Archived from the original on 10 January 2017. Retrieved 9 January 2017.
- ↑ CDC – Skin Cancer Statistics Archived 8 September 2012 at the Wayback Machine
- ↑ "Melanoma facts and statistics". Melanoma Institute Australia. Archived from the original on 18 May 2014. Retrieved 18 May 2014.
- ↑ "Skin Cancer Facts". Skin Cancer Foundation. Archived from the original on 30 June 2010. Retrieved 2 July 2010.
- ↑ "Skin cancer statistics". Cancer Research UK. Archived from the original on 16 January 2014. Retrieved 28 October 2014.
External links
| Classification | |
|---|---|
| External resources |
- Skin cancer at Curlie
- Skin cancer procedures: text, images and videos Archived 7 December 2013 at the Wayback Machine
- Pages with script errors
- CS1: long volume value
- CS1 errors: missing periodical
- Webarchive template archiveis links
- Webarchive template wayback links
- Use dmy dates from March 2020
- Articles with invalid date parameter in template
- All articles with unsourced statements
- Articles with unsourced statements from January 2010
- Articles with Curlie links
- Integumentary neoplasia
- Sun tanning
- RTT
- Medical mnemonics