Sgarbossa's criteria
| Sgarbossa's criteria | |
|---|---|
| Other names: Smith-modified Sgarbossa criteria,[1] modified Sgarbossa criteria[2] | |
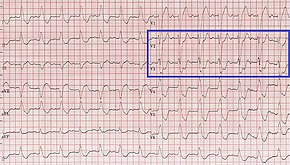 An ECG showing 3 to 4 mm of ST depression in the same direction as the QRS complex in leads V2 and V3[3] | |
| Calculator | MDCalc |
| Purpose | Identify acute myocardial infarction in LBBB or right ventricular pacing[4] |
| Based on | ECG[4] |
Sgarbossa criteria are specific electrocardiographic (ECG) changes, in the presence of a left bundle branch block (LBBB) or right ventricular pacing (RVP), that are equivalent to an ST elevation myocardial infarction (STEMI).[4] They represent a sudden blockage of a coronary artery.[4]
In LBBB an acute MI is present when there is 1) ST elevation of at least 1 mm in the same direction as the QRS in at least one lead 2) ST depression of at least 1 mm in the same direction as the QRS in one of leads V1 to V3 3) ST elevation in the opposite direction of the QRS that is at least 25% the size of the S wave in one lead.[4] In RVP the second criteria can be applied to leads V1 to V6.[2]
Reperfusion efforts, such as percutaneous coronary intervention (PCI) or fibrinolysis, are recommended if the person has a suspected MI based on symptom and is hemodynamically unstable, has positive Sgarbossa criteria, or has an ultrasound of the heart that shows a STEMI.[5] If one of the three Sgarbossa criteria is present it generally indicate an acute MI, while their absence indicates that the risk is low.[4]
The criteria were first descried by the cardiologist Elena Sgarbossa in 1996.[1][6] Modifications to the third criteria were proposed by Smith in 2012.[4] While historically, a presumed new LBBB was considered a STEMI equivalent, this is no longer the case as of 2013.[5]
Criteria
Smith modification
Smith modified Sgarbossa's original criteria by adjusting the third criteria.[7]
Smith modified Sgarbossa rule:
- ST elevation ≥1 mm in a lead with a positive QRS complex (i.e.: concordance) (Sgarbossa criterion 1) or
- concordant ST depression ≥1 mm in lead V1, V2, or V3 (Sgarbossa criterion 2) or
- proportionally excessively discordant ST elevation in V1-V4, as defined by an ST/S ratio of equal to or more than 0.20 and at least 2 mm of STE. (this replaces Sgarbossa criterion 3 which uses an absolute of 5mm)
Original
Three criteria are included in the original Sgarbossa's criteria:[6]
- ST elevation ≥1 mm in a lead with a positive QRS complex (i.e.: concordance) - 5 points
- concordant ST depression ≥1 mm in lead V1, V2, or V3 - 3 points
- ST elevation ≥5 mm in a lead with a negative (discordant) QRS complex - 2 points
≥3 points = 90% specificity of STEMI (sensitivity of 36%)[6]
A high take-off of the ST segment in leads V1 to V3 is well-described with uncomplicated LBBB, such as in the setting of left ventricular hypertrophy. In a substudy from the ASSENT 2 and 3 trials, the third criteria added little diagnostic or prognostic value.[8]
A Sgarbossa score of ≥3 was specific but not sensitive (36%) in the validation sample in the original report.[6] A subsequent meta-analysis of 10 studies consisting of 1614 patients showed that a Sgarbossa score of ≥3 had a specificity of 98% and sensitivity of 20%.[9] The sensitivity may increase if serial or previous ECGs are available.[10]
Other
Wackers et al. correlated ECG changes in LBBB with localization of the infarct by thallium scintigraphy.[11] The most useful ECG criteria were:
- Serial ECG changes — 67 percent sensitivity
- ST segment elevation — 54 percent sensitivity
- Abnormal Q waves — 31 percent sensitivity
- Cabrera's sign — 27 percent sensitivity, 47 percent for anteroseptal MI
- Initial positivity in V1 with a Q wave in V6 — 20 percent sensitivity but 100 percent specificity for anteroseptal MI
See also
References
- ↑ 1.0 1.1 Cadogan, Mike; Buttner, Robert; Buttner, Mike Cadogan and Robert (1 August 2020). "Sgarbossa Criteria". Life in the Fast Lane • LITFL. Archived from the original on 17 August 2022. Retrieved 20 December 2022.
- ↑ 2.0 2.1 "Modified Sgarbossa Criteria for Ventricular Paced Rhythms". JournalFeed. 6 August 2021. Archived from the original on 24 September 2022. Retrieved 21 December 2022.
- ↑ "MI Diagnosis in LBBB or paced rhythm". Archived from the original on 20 October 2021. Retrieved 20 December 2022.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Khawaja, M; Thakker, J; Kherallah, R; Ye, Y; Smith, SW; Birnbaum, Y (17 November 2021). "Diagnosis of Occlusion Myocardial Infarction in Patients with Left Bundle Branch Block and Paced Rhythms". Current cardiology reports. 23 (12): 187. doi:10.1007/s11886-021-01613-0. PMID 34791609.
- ↑ 5.0 5.1 "LBBB in Patients With Suspected MI: An Evolving Paradigm". American College of Cardiology. Archived from the original on 10 August 2022. Retrieved 21 December 2022.
- ↑ 6.0 6.1 6.2 6.3 Sgarbossa, Elena B.; Pinski, Sergio L.; Barbagelata, Alejandro; Underwood, Donald A.; Gates, Kathy B.; Topol, Eric J.; Califf, Robert M.; Wagner, Galen S. (1996). "Electrocardiographic Diagnosis of Evolving Acute Myocardial Infarction in the Presence of Left Bundle-Branch Block". New England Journal of Medicine. 334 (8): 481–487. doi:10.1056/NEJM199602223340801. ISSN 0028-4793. PMID 8559200.
- ↑ Smith, Stephen W.; Dodd, Kenneth W.; Henry, Timothy D.; Dvorak, David M.; Pearce, Lesly A. (2012). "Diagnosis of ST-Elevation Myocardial Infarction in the Presence of Left Bundle Branch Block With the ST-Elevation to S-Wave Ratio in a Modified Sgarbossa Rule". Annals of Emergency Medicine. 60 (6): 766–776. doi:10.1016/j.annemergmed.2012.07.119. ISSN 0196-0644. PMID 22939607.
- ↑ Al-Faleh, Hussam; Fu, Yuling; Wagner, Galen; Goodman, Shaun; Sgarbossa, Elena; Granger, Christopher; Van de Werf, Frans; Wallentin, Lars; W. Armstrong, Paul; et al. (2006). "Unraveling the spectrum of left bundle branch block in acute myocardial infarction: Insights from the Assessment of the Safety and Efficacy of a New Thrombolytic (ASSENT 2 and 3) trials". American Heart Journal. 151 (1): 10–15. doi:10.1016/j.ahj.2005.02.043. ISSN 0002-8703. PMID 16368285.
- ↑ Tabas, Jeffrey A.; Rodriguez, Robert M.; Seligman, Hilary K.; Goldschlager, Nora F. (2008). "Electrocardiographic Criteria for Detecting Acute Myocardial Infarction in Patients With Left Bundle Branch Block: A Meta-analysis". Annals of Emergency Medicine. 52 (4): 329–336.e1. doi:10.1016/j.annemergmed.2007.12.006. ISSN 0196-0644. PMID 18342992.
- ↑ E. B. Sgarbossa (2000). "Value of the ECG in suspected acute myocardial infarction with left bundle branch block". Journal of Electrocardiology. 33 Suppl: 87–92. doi:10.1054/jelc.2000.20324. PMID 11265742.
- ↑ F. J. Wackers (August 1987). "The diagnosis of myocardial infarction in the presence of left bundle branch block". Cardiology Clinics. 5 (3): 393–401. doi:10.1016/S0733-8651(18)30529-0. PMID 3690603.
External links
- ECGepedia Archived 2021-10-20 at the Wayback Machine
- EM cases Archived 2022-06-27 at the Wayback Machine