Prurigo nodularis
| Prurigo nodularis | |
|---|---|
| Other names: Hyde prurigo nodularis, picker's nodules, atypical nodular form of neurodermatitis circumscripta, lichen corneus obtusus | |
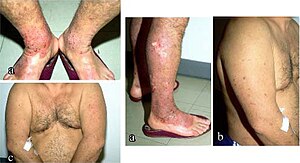 | |
| Pruritic papules and scattered nodules can be seen (a) on the legs, (b) on the arms and (c) on the trunk of this patient with prurigo nodularis. | |
| Diagnostic method | Skin biopsy[1] |
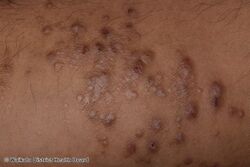
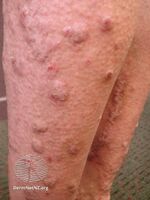
Prurigo nodularis (PN), also known as nodular prurigo, is a skin disease characterised by very itchy widespread bumps in the skin.[1] There are typically multiple scratch marks and abrasions, particularly on the upper trunk, and outer parts of arms and legs.[1]
Diagnosis is by excluding other causes of itchy rashes and confirmed by skin biopsy.[1] Treatment usually includes topical corticosteroids and antihistamines, but have limited effectiveness.[1]
Signs and symptoms
- Nodules are discrete, generally symmetric, hyperpigmented or purpuric, and firm. They are greater than 0.5 cm in both width and depth (as opposed to papules which are less than 0.5 cm). They can appear on any part of the body, but generally begin on the arms and legs.[citation needed]
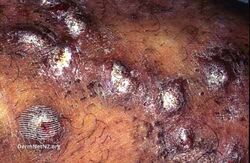
- Excoriated lesions are often flat, umbilicated, or have a crusted top.[citation needed]
- Nodules may appear to begin in the hair follicles.[citation needed]
- Nodule pattern may be follicular.[citation needed]
- In true prurigo nodularis, a nodule forms before itching begins. Typically, these nodules are extremely pruritic and are alleviated only by steroids.[citation needed]
-
Prurigo nodularis
-
Prurigo nodularis
-
Prurigo nodularis
Causes
The cause of prurigo nodularis is unknown, although other conditions may induce PN. PN has been linked to Becker's nevus,[2] linear IgA disease, an autoimmune condition,[3] liver disease[4] and T cells.[5] Systemic pruritus has been linked to cholestasis, thyroid disease, polycythaemia rubra vera, uraemia, Hodgkins disease, HIV and other immunodeficiency diseases.[6][7] Internal malignancies, liver failure, kidney failure, and psychiatric illnesses have been considered to induce PN, although more recent research has refuted a psychiatric cause for PN. Patients report an ongoing battle to distinguish themselves from those with psychiatric disorders, such as delusions of parasitosis and other psychiatric conditions.[8][9]
Pathophysiology
Chronic and repetitive scratching, picking, or rubbing of the nodules may result in permanent changes to the skin, including nodular lichenification, hyperkeratosis, hyperpigmentation, and skin thickening. Unhealed, excoriated lesions are often scaly, crusted or scabbed. Many patients report a lack of wound healing even when medications relieve the itching and subsequent scratching.[citation needed]
Patients often:[citation needed]
- seek treatment during middle-age, although PN can occur at any age.
- have a history of chronic severe pruritus.
- have a significant medical history for unrelated conditions.
- suffer from liver or kidney dysfunctions.
- suffer from secondary skin infections.
- have a personal or family history of atopic dermatitis.
- have other autoimmune disorders.
- have low vitamin D levels.
Diagnosis
Diagnosis is based on visual examination and the presence of itching. A skin biopsy is often performed to exclude other diseases. Lesion biopsies usually show light inflammation, sometimes with increased numbers of eosinophils.[10] A culture of at least one lesion will rule out staphylococcus infection, which has been significantly linked to atopic dermatitis.[11][12][13]
Treatment
Prurigo nodularis is very hard to treat, but current therapies include steroids, vitamins, cryosurgery, thalidomide and UVB light. In the event that staphylococcus or other infection is present, antibiotics have proven effective, but tend to cause more harm than good for this particular disease. A physician may administer a strong dose of prednisone, which will almost immediately stop the itch/scratch cycle. However, cessation of steroids allows relapse to occur, usually within a few weeks. Horiuchi et al recently reported significant improvement in PN with antibiotic therapy.[14]
Another drug a physician may administer is Apo-Azathioprine. Azathioprine, also known by its brand name Imuran, is an immunosuppressive drug used in organ transplantation and autoimmune diseases and belongs to the chemical class of purine analogues.[citation needed]
History
Prurigo nodularis was first described by Hyde and Montgomery in 1909.[15]
See also
Notes
- ↑ 1.0 1.1 1.2 1.3 1.4 Wakelin, Sarah H. (2020). "22. Dermatology". In Feather, Adam; Randall, David; Waterhouse, Mona (eds.). Kumar and Clark's Clinical Medicine (10th ed.). Elsevier. p. 664. ISBN 978-0-7020-7870-5. Archived from the original on 2021-12-11. Retrieved 2021-12-11.
- ↑ Lockshin BN, Brogan B, Billings S, Billings S (2006). "Eczematous dermatitis and prurigo nodularis confined to a Becker's nevus". Int. J. Dermatol. 45 (12): 1465–1466. doi:10.1111/j.1365-4632.2006.02971.x. PMID 17184268.
- ↑ Torchia D, Caproni M, Del Bianco E, Cozzani E, Ketabchi S, Fabbri P (2006). "Linear IgA disease presenting as prurigo nodularis". Br. J. Dermatol. 155 (2): 479–80. doi:10.1111/j.1365-2133.2006.07315.x. PMID 16882196.
- ↑ Hazin R, Abu-Rajab Tamimi TI, Abuzetun JY, Zein NN (October 2009). "Recognizing and treating cutaneous signs of liver disease". Cleve Clin J Med. 76 (10): 599–606. doi:10.3949/ccjm.76A.08113. PMID 19797460.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Sonkoly E, Muller A, Lauerma AI, et al. (2006). "IL-31: a new link between T cells and pruritus in atopic skin inflammation". J. Allergy Clin. Immunol. 117 (2): 411–7. doi:10.1016/j.jaci.2005.10.033. PMID 16461142.
- ↑ Hiramanek N (2004). "Itch: a symptom of occult disease". Australian Family Physician. 33 (7): 495–9. PMID 15301165.
- ↑ Berger TG, Hoffman C, Thieberg MD (1995). "Prurigo nodularis and photosensitivity in AIDS: treatment with thalidomide". J. Am. Acad. Dermatol. 33 (5 Pt 1): 837–8. doi:10.1016/0190-9622(95)91846-9. PMID 7593791.
- ↑ Kieć-Swierczyńska M, Dudek B, Krecisz B, et al. (2006). "[The role of psychological factors and psychiatric disorders in skin diseases]" [The role of psychological factors and psychiatric disorders in skin diseases]. Med Pr (in polski). 57 (6): 551–5. PMID 17533993.
- ↑ Vargas Laguna E, Peña Payero ML, Vargas Márquez A (Dec 2006). "[Influence of anxiety in diverse cutaneous diseases]" [Influence of anxiety in diverse cutaneous diseases]. Actas Dermosifiliogr (in español). 97 (10): 637–43. doi:10.1016/s0001-7310(06)73484-6. PMID 17173825.[permanent dead link]
- ↑ Johansson O, Liang Y, Marcusson JA, Reimert CM (2000). "Eosinophil cationic protein- and eosinophil-derived neurotoxin/eosinophil protein X-immunoreactive eosinophils in prurigo nodularis". Arch. Dermatol. Res. 292 (8): 371–8. doi:10.1007/s004030000142. PMID 10994770.
- ↑ Gong JQ, Lin L, Lin T, et al. (Oct 2006). "Skin colonization by Staphylococcus aureus in patients with eczema and atopic dermatitis and relevant combined topical therapy: a double-blind multicentre randomized controlled trial". Br J Dermatol. 155 (4): 680–7. doi:10.1111/j.1365-2133.2006.07410.x. PMID 16965415.
- ↑ Lin YT, Wang CT, Chiang BL (Dec 2007). "Role of bacterial pathogens in atopic dermatitis". Clin Rev Allergy Immunol. 33 (3): 167–77. doi:10.1007/s12016-007-0044-5. PMID 18163223.
- ↑ Guzik TJ, Bzowska M, Kasprowicz A, et al. (Apr 2005). "Persistent skin colonization with Staphylococcus aureus in atopic dermatitis: relationship to clinical and immunological parameters". Clin Exp Allergy. 35 (4): 448–55. doi:10.1111/j.1365-2222.2005.02210.x. PMID 15836752.
- ↑ Horiuchi Y, Bae S, Katayama I (2006). "Uncontrollable prurigo nodularis effectively treated by roxithromycin and tranilast". Journal of Drugs in Dermatology. 5 (4): 363–5. PMID 16673805.
- ↑ Hyde JN, Montgomery FH: A practical treatise on disease of the skin for the use of students and practitioners. 1909; 174–175.
External links
| Classification | |
|---|---|
| External resources |
- DermNet NZ: Prurigo nodularis Archived 2012-05-17 at the Wayback Machine
- DermAtlas -2016053621
- Pages with script errors
- CS1 maint: multiple names: authors list
- CS1 polski-language sources (pl)
- CS1 español-language sources (es)
- All articles with dead external links
- Articles with dead external links from April 2018
- Articles with invalid date parameter in template
- Articles with permanently dead external links
- All articles with unsourced statements
- Articles with unsourced statements from December 2020
- Webarchive template wayback links
- Pruritic skin conditions
- Ailments of unknown cause