Podoconiosis
| Podoconiosis | |
|---|---|
| Other names: Nonfilarial elephantiasis | |
 | |
| Bilateral lower extremity swelling and "mossy" hyperkeratotic papillomata characteristic of podoconiosis | |
| Specialty | Toxicology |
Podoconiosis, also known as nonfilarial elephantiasis,[1] is a disease of the lymphatic vessels of the lower extremities that is caused by chronic exposure to irritant soils. It is the second most common cause of tropical lymphedema after lymphatic filariasis,[2] and it is characterized by prominent swelling of the lower extremities, which leads to disfigurement and disability. Methods of prevention include wearing shoes and using floor coverings. Mainstays of treatment include daily foot hygiene, compression bandaging, and when warranted, surgery of overlying nodules.
Signs and symptoms
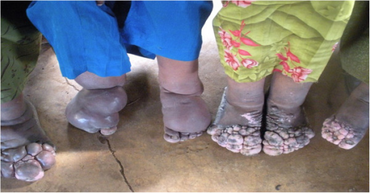
Podoconiosis causes bilateral yet asymmetrical leg swelling with overlying firm nodules. Early on, symptoms may include itching, tingling, widening of the forefoot, and swelling which then progress to soft edema, skin fibrosis, papillomatosis, and nodule formation resembling moss, giving rise to the disease's alternate name of "mossy foot" in some regions of the world.[3] As with other forms of tropical lymphedema, chronic disease can lead to rigid toes, ulceration, and bacterial superinfection. During acute episodes of adenolymphangitis, patients may develops fevers, extremity warmth, redness, and pain. These episodes are extremely debilitating and account for many days of activity and productivity loss each year.[4]
Psychological consequences
As a result of its appearance, podoconiosis can cause social stigmatization and discrimination.[5] People with podoconiosis also report a lower quality of life than people in similar neighborhood circumstances except without podoconiosis[6] and also higher levels of mental distress[7] and depression.[8]
Pathophysiology
According to the World Health Organization "Evidence suggests that podoconiosis is the result of a genetically determined abnormal inflammatory reaction to mineral particles in irritant red clay soils derived from volcanic deposits".[9]
The pathophysiology of podoconiosis is a combination of genetic susceptibility, possibly through associations with HLA-DQA1, HLA-DQB1, and HLA-DRB1 variants, and a cumulative exposure to irritant soil.[10][11] In susceptible individuals, irritant soil particles penetrate the feet and collect in lymphatic vessels.[12] Over time, chronic inflammation within the lymphatic vessels leads to fibrosis and occlusion.[13]
Diagnosis
Differential diagnosis
The differential diagnosis for podoconiosis includes other causes of tropical lymphedema, such as filariasis or leprosy, and mycetoma pedis.[3][12]
While filariasis is generally unilateral, podoconiosis affects the legs bilaterally albeit asymmetrically and in an ascending manner. Podoconiosis very rarely affects the groin while filariasis frequently involves the groin: a high ratio of lymphoedema/hydrocele cases in an area suggests podoconiosis as the dominant cause of lymphedema. In some cases, the history and clinical presentation alone are unable to differentiate between the two causes of tropical lymphedema. Local epidemiology can also be a clue to diagnosis, as podoconiosis is typically found in higher altitude areas with volcanic soils while filariasis is common in low-lying areas where mosquitos are prevalent. Blood smears for identification of microfilariae and antigen detection techniques can be helpful in the diagnosis of lymphatic filariasis.[citation needed]
Lepromatous lymphedema can also mimic podoconiosis clinically, but the former will have loss of sensation in the toes and feet, thickened nerves, and trophic ulcers. Other causes of lymphedema include Kaposi sarcoma, mycetoma, and elephantiasis nostras verrucosa.[14]
Prevention
Elimination of podoconiosis relies on prevention with widespread shoe implementation, stringent foot hygiene, and floor coverings. Community-based initiatives are crucial to achieving elimination of this disease. In Ethiopia, The Mossy Foot Treatment and Prevention Association (now Mossy Foot International) works to transform patients into community podoconiosis agents who in turn visit patients, teach basic treatment techniques such as foot hygiene, and educate families about the disease.[15] This model has been adapted by several other non-government groups as they have started programs in other regions of Ethiopia.[16][17]
Treatment

The cornerstone of prevention and treatment of podoconiosis is avoidance of exposure to irritant soils. Wearing shoes in the presence of irritant soils is the primary method of exposure reduction. In Rwanda, a country of high disease prevalence, the government has banned walking barefoot in public,[18] in order to prevent podoconiosis and other soil-borne diseases. Increasing the availability of footwear must be coupled with education on the benefits of wearing shoes as cultural influences, such as barefoot traditions, can hinder widespread use of footwear.[19]
Once the disease has developed, rigorous foot hygiene including daily washing with soap and water, application of an emollient, and nightly elevation of the affected extremity has been shown to reduce frequency of acute attacks.[16] Nodules will not resolve with these conservative measures, although surgical removal of the nodules can be performed.[20]
Epidemiology
Podoconiosis is most frequently seen in the highland areas of Africa, India, and Central America. The highest prevalence is seen in Uganda, Tanzania, Kenya, Rwanda, Burundi, Sudan, and Ethiopia.[12] A recent review has summarized the global distribution of podoconiosis.[21] In some areas of Ethiopia, the prevalence is as high as 4%.[22] The incidence of podoconiosis increases with age, likely due to cumulative exposure to irritant soil. It is very rare to see podoconiosis in the 0–5 year old age group, and the incidence rapidly rises from 6 to 20 years of age, with the highest prevalence after 45 years of age. Podoconiosis is most commonly seen in higher altitude areas with volcanic soil,[12] and it is estimated to affect 4 million people worldwide.[2] Productivity losses associated with the disease are significant. In Ethiopia (where 1.6 million people are estimated to be affected),[23] the condition is thought to have caused US $200 million in lost productivity per year in 2004.[24]
History
After parasitic filariae were discovered to be an important cause of tropical lymphedema in the 19th century, early investigators assumed that filariae were the sole cause of lymphedema in the tropics. It was later discovered that the distribution of tropical lymphedema and filariasis did not perfectly overlap, and researchers began to recognize that some forms of tropical lymphedema were not associated with filariasis.[12] Ernest W Price, a British surgeon living in Ethiopia, discovered the true etiology of podoconiosis in the 1970s and 1980s by studying the lymph nodes and vessels of those afflicted with the disease.[25] Using light microscopy, he observed macrophage cells laden with micro-particles in lymph nodes of the affected extremity. After examining the same tissue using electron microscopy, he was able to identify the presence of silicon, aluminum, and other soil metals both in the phagosomes of macrophages and adhered to the surface of lymphocytes.[26] Price demonstrated that the lymphatic vessels of these patients experienced subendothelial edema and eventual collagenization of the lumen leading to complete blockage.[13] He wrote a monograph on podoconiosis which was published after his death in 1990.[27]
Society and culture
Podoconiosis is now recognised as one of the WHO Neglected Tropical Diseases,[28] its importance as a public health problem is well recognised in Ethiopia.[29] Footwork[30] is a charity which bring together public and private partners to support prevention and treatment of podoconiosis. There is an active research group led by Gail Davey[31] at the Wellcome Trust Brighton and Sussex Centre for Global Health Research[32] which co-ordinates research worldwide. A recent article in the Lancet includes some excellent illustrations.[33]
References
- ↑ "Podoconiosis: endemic non-filarial elephantiasis". World Health Organization. Archived from the original on April 28, 2016. Retrieved March 20, 2018.
- ↑ 2.0 2.1 Molyneux DH (March 2012). "Tropical lymphedemas--control and prevention" (PDF). The New England Journal of Medicine. 366 (13): 1169–71. doi:10.1056/NEJMp1202011. PMID 22455411. Archived (PDF) from the original on 2018-07-19. Retrieved 2021-12-13.
- ↑ 3.0 3.1 Korevaar DA, Visser BJ (June 2012). "Podoconiosis, a neglected tropical disease". The Netherlands Journal of Medicine. 70 (5): 210–4. PMID 22744921. Archived from the original on 2020-08-07. Retrieved 2021-12-13.
- ↑ Bekele K, Deribe K, Amberbir T, Tadele G, Davey G, Samuel A (September 2016). "Burden assessment of podoconiosis in Wayu Tuka woreda, east Wollega zone, western Ethiopia: a community-based cross-sectional study". BMJ Open. 6 (9): e012308. doi:10.1136/bmjopen-2016-012308. PMC 5051403. PMID 27670520.
- ↑ Tora A, Franklin H, Deribe K, Reda AA, Davey G (2014). "Extent of podoconiosis-related stigma in Wolaita Zone, Southern Ethiopia: a cross-sectional study". SpringerPlus. 3: 647. doi:10.1186/2193-1801-3-647. PMC 4233027. PMID 25485190.
- ↑ Mousley E, Deribe K, Tamiru A, Davey G (July 2013). "The impact of podoconiosis on quality of life in Northern Ethiopia". Health and Quality of Life Outcomes. 11: 122. doi:10.1186/1477-7525-11-122. PMC 3726315. PMID 23866905.
- ↑ Mousley E, Deribe K, Tamiru A, Tomczyk S, Hanlon C, Davey G (January 2015). "Mental distress and podoconiosis in Northern Ethiopia: a comparative cross-sectional study". International Health. 7 (1): 16–25. doi:10.1093/inthealth/ihu043. PMC 4236095. PMID 25062906.
- ↑ Bartlett J, Deribe K, Tamiru A, Amberbir T, Medhin G, Malik M, Hanlon C, Davey G (March 2016). "Depression and disability in people with podoconiosis: a comparative cross-sectional study in rural Northern Ethiopia". International Health. 8 (2): 124–31. doi:10.1093/inthealth/ihv037. PMC 4604655. PMID 26113669.
- ↑ "Podoconiosis: endemic non-filarial elephantiasis". Neglected tropical diseases. World Health Organization. Archived from the original on October 15, 2011. Retrieved 27 April 2014.
- ↑ Tekola Ayele F, Adeyemo A, Finan C, Hailu E, Sinnott P, Burlinson ND, Aseffa A, Rotimi CN, Newport MJ, Davey G (March 2012). "HLA class II locus and susceptibility to podoconiosis". The New England Journal of Medicine. 366 (13): 1200–8. doi:10.1056/NEJMoa1108448. PMC 3350841. PMID 22455414.
- ↑ Lewis, Ricki. "Vanquishing "Mossy Foot" with Genetic Epidemiology and Shoes". Scientific American. Archived from the original on 28 February 2021. Retrieved 25 March 2021.
- ↑ 12.0 12.1 12.2 12.3 12.4 Davey G, Tekola F, Newport MJ (December 2007). "Podoconiosis: non-infectious geochemical elephantiasis". Transactions of the Royal Society of Tropical Medicine and Hygiene. 101 (12): 1175–80. doi:10.1016/j.trstmh.2007.08.013. PMID 17976670.
- ↑ 13.0 13.1 Price EW (1975). "The mechanism of lymphatic obstruction in endemic elephantiasis of the lower legs". Transactions of the Royal Society of Tropical Medicine and Hygiene. 69 (2): 177–80. doi:10.1016/0035-9203(75)90150-9. PMID 1166487.
- ↑ Arellano, Javier; Gonzalez, Ruben; Corredoira, Yamile; Nuñez, Roxana (2020). "Diagnosis of elephantiasis nostras verrucosa as a clinical mani-festation of Kaposi's sarcoma". Medwave. 20 (1): e7767. doi:10.5867/medwave.2020.01.7767. PMID 31999679.
- ↑ Davey G, Burridge E (May 2009). "Community-based control of a neglected tropical disease: the mossy foot treatment and prevention association". PLOS Neglected Tropical Diseases. 3 (5): e424. doi:10.1371/journal.pntd.0000424. PMC 2682702. PMID 19479039.
- ↑ 16.0 16.1 Negussie H, Kassahun MM, Fegan G, Njuguna P, Enquselassie F, McKay A, Newport M, Lang T, Davey G (July 2015). "Podoconiosis treatment in northern Ethiopia (GoLBet): study protocol for a randomised controlled trial". Trials. 16: 307. doi:10.1186/s13063-015-0818-7. PMC 4504163. PMID 26177812.
- ↑ Tomczyk S, Tamiru A, Davey G (2012). "Addressing the neglected tropical disease podoconiosis in Northern Ethiopia: lessons learned from a new community podoconiosis program". PLOS Neglected Tropical Diseases. 6 (3): e1560. doi:10.1371/journal.pntd.0001560. PMC 3302806. PMID 22428078.
- ↑ Banks T (December 1, 2011). "Rwanda: From Nightmare Past to Hopeful Future". International Reporting Project. Archived from the original on 22 December 2015. Retrieved 15 December 2015.
- ↑ Kelemework A, Tora A, Amberbir T, Agedew G, Asmamaw A, Deribe K, Davey G (March 2016). "'Why should I worry, since I have healthy feet?' A qualitative study exploring barriers to use of footwear among rural community members in northern Ethiopia". BMJ Open. 6 (3): e010354. doi:10.1136/bmjopen-2015-010354. PMC 4809094. PMID 27006343.
- ↑ Yeshanehe WE, Tamiru A, Fuller LC (October 2017). "Surgical nodulectomies can heal in patients with lymphoedema secondary to podoconiosis in resource-poor settings". The British Journal of Dermatology. 177 (4): e128–e129. doi:10.1111/bjd.15420. PMID 28256715. S2CID 30097328.
- ↑ Deribe K, Cano J, Trueba ML, Newport MJ, Davey G (March 2018). "Global epidemiology of podoconiosis: A systematic review". PLOS Neglected Tropical Diseases. 12 (3): e0006324. doi:10.1371/journal.pntd.0006324. PMC 5849362. PMID 29494642.
- ↑ Deribe K, Brooker SJ, Pullan RL, Sime H, Gebretsadik A, Assefa A, Kebede A, Hailu A, Rebollo MP, Shafi O, Bockarie MJ, Aseffa A, Reithinger R, Cano J, Enquselassie F, Newport MJ, Davey G (January 2015). "Epidemiology and individual, household and geographical risk factors of podoconiosis in Ethiopia: results from the first nationwide mapping". The American Journal of Tropical Medicine and Hygiene. 92 (1): 148–58. doi:10.4269/ajtmh.14-0446. PMC 4288951. PMID 25404069.
- ↑ Deribe K, Cano J, Giorgi E, Pigott DM, Golding N, Pullan RL, et al. (2017). "Estimating the number of cases of podoconiosis in Ethiopia using geostatistical methods". Wellcome Open Research. 2: 78. doi:10.12688/wellcomeopenres.12483.2. PMC 5668927. PMID 29152596.
- ↑ Tekola F, Mariam DH, Davey G (July 2006). "Economic costs of endemic non-filarial elephantiasis in Wolaita Zone, Ethiopia". Tropical Medicine & International Health. 11 (7): 1136–44. doi:10.1111/j.1365-3156.2006.01658.x. PMID 16827714.
- ↑ Vernon, Gervase (2019). "Dr E W Price, the discoverer of podoconiosis". Journal of Medical Biography. Sage publications: 096777201988840. doi:10.1177/0967772019888406. PMID 31735101.
- ↑ Price EW, Henderson WJ (1978). "The elemental content of lymphatic tissues of barefooted people in Ethiopia, with reference to endemic elephantiasis of the lower legs". Transactions of the Royal Society of Tropical Medicine and Hygiene. 72 (2): 132–6. doi:10.1016/0035-9203(78)90048-2. PMID 653784.
- ↑ Price, Dr E W (1990). Podoconiosis. Oxford: Oxford University Press. ISBN 0192620029.
- ↑ Davey, Gail (2007). "Podoconiosis: the most neglected tropical disease?". Lancet. 369 (9565): 888–9. doi:10.1016/S0140-6736(07)60425-5. PMID 17368134. S2CID 35516740. Archived from the original on 10 March 2022. Retrieved 31 May 2019.
- ↑ Deribe, Kebede (2017). "Podoconiosis in Ethiopia: From Neglect to Priority Public Health Problem". Ethiop Med J. 55(Suppl 1): . (Suppl 1): 65–74. PMC 5582632. PMID 28878431.
- ↑ "Footwork". Footwork; the international podoconiosis initiative. Archived from the original on 4 December 2018. Retrieved 31 May 2019.
- ↑ "Professor Gail Davey". Archived from the original on 31 May 2019. Retrieved 31 May 2019.
- ↑ "Wellcome Trust Brighton and Sussex Centre for Global Health Research". Archived from the original on 3 April 2019. Retrieved 31 May 2019.
- ↑ Alexander Kumar Kebede Deribe Nebiyu Negussu Gail Davey (2019). "Picturing health: podoconiosis—stepping out of neglect". The Lancet. 394 (10208): 1499–1512. doi:10.1016/S0140-6736(19)32129-4. PMID 32534625. S2CID 202583049. Archived from the original on 10 March 2022. Retrieved 18 December 2019.