Pearly penile papules
| Pearly penile papules | |
|---|---|
| Other names: Papillomatosis corona penis, corona capillitii, hirsuties coronae glandis, papillae coronis glandis, hirsutoid papillomas, hirsuties coronae glandis[1][2] | |
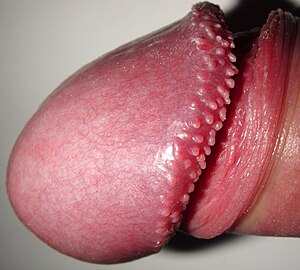 | |
| Glans penis with pearly penile papules | |
| Specialty | Dermatology |
| Symptoms | Painless small bumps on ridge of glans of the penis[2] |
| Usual onset | Age 20-30 years[3] |
| Diagnostic method | Examination[3] |
| Differential diagnosis | Genital warts, molluscum contagiosum, sebaceous hyperplasia, lichen nitidus[2] |
| Treatment | Reassurance, generally no treatment necessary[3] |
| Prognosis | Not harmful, regress spontaneously, recurrence rare[3] |
| Frequency | Up to half of young males[1] |
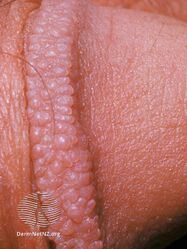
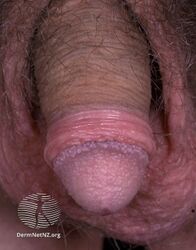
Pearly penile papules (PPPs) are normal small bumps that can occur on the penis.[2][3] They vary in size from 1 - 4 mm, are white or flesh-colored, smooth and dome-topped, and appear in one or several rows around the ridge of the head of the penis and sometimes on the shaft.[2][4] In a Black person, they generally appear whitish.[5] They are painless, non-cancerous, and harmless.[2]
They are a type of angiofibroma, whose function is not well-understood.[3][1] They are sometimes described as remnants of penile spines, a sensitive feature found in the same location in other primates.[6] PPPs secrete oil that moistens the head of the penis.[7] Diagnosis is by visualization.[3] On dermoscopy, they appear in a cobblestone-like pattern, with a central dotted or comma-shaped blood vessels, and without scaling.[1] Examination of a tissue biopsy shows dense connective tissue, fibroblasts, and many blood vessels.[4] They are sometimes mistaken for genital warts, molluscum contagiosum, sebaceous hyperplasia, or lichen nitidus.[8][2]
Generally, reassurance is given and no treatment is needed.[3] Following counselling, cryotherapy, laser therapy, or shave excision may be options for cosmetic reasons.[9][3] Some home remedies involving corrosive substances can be damaging.[10] They do not spread and often spontaneously regress.[11]
PPPs are common, occurring in up to half of young males.[1][2] They are more common in uncircumcised people.[2] They were first described in 1700 and the term "pearly penile papules" was coined in 1964.[1] Some find them distressing to look at, owing to their resemblance to some sexually transmitted infections.[1][12]
Signs and symptoms
PPPs are small bumps on the human penis.[2] They vary in size from 1 - 4 mm, are pearly or flesh-colored, smooth and dome-topped or filiform, and appear in one or several rows around the corona, the ridge of the glans and sometimes on the penile shaft.[2][4] In a black person, the bumps may appear whitish.[5] They are painless, non-cancerous and not harmful.[2]
-
Pearly penile papules
-
Pearly penile papules
-
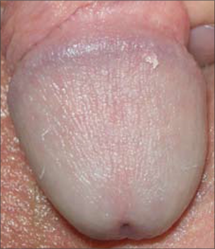
Single pearly penile papule on glans
Cause and mechanism
PPPs are a type of angiofibroma.[3] Their function is not well-understood.[1][13] They are sometimes described as vestigial remnants of penile spines, sensitive features found in the same location in other primates.[6] PPPs secrete oil that moistens the glans of the penis.[7] They do not spread and often regress spontaneously.[11] Along with Fordyce glands PPPs secrete oils to keep the skin of the head of penis in good condition.[7] Smegma can accumulate if these oils are produced in excess or there is inadequate washing under the foreskin.[7] There is no association with human papilloma virus[1] The bumps are analogous to vestibular papillomatosis in women.[14]'
Diagnosis

Diagnosis is by visualisation.[3] On dermoscopy, the white-pink papules appear in a cobblestone-like pattern and contain a central dotted or comma-shaped blood vessels. There is no scale.[1] PPPs are sometimes mistaken for genital warts due to a perceived similarity in appearance.[8] They can also appear similar to molluscum contagiosum, sebaceous hyperplasia and lichen nitidus.[2] Histopathology shows dense connective tissue, fibroblasts and many blood vessels.[4]
Treatment

Generally, reassurance is given and no treatment is needed.[3][15] Laser or cryotherapy may be considered for men who find PPPs distressing to look at or feel excessive embarrassment.[1]
Carbon dioxide laser generally has good outcomes with skin healing within 7 days.[1] The procedure requires anaesthesia, may need to be performed more than once, and has a risk of bleeding, scarring and colour changes.[1] Another procedure involves a hyfrecator.[16]
Epidemiology
PPPs are common and occur in around up to 48% of young males.[1][2] They are more common in uncircumcised males.[2]
History
PPPs were first described by Alexis Littré in 1700 and the term pearly penile papules was coined in 1964.[1]
Society and culture
Although it is not related to any disease, PPPs are occasionally mistaken for HPV warts.[1] There are also home remedies for "curing" it, despite the fact that the papules are neither infectious nor detrimental to one's health and may have beneficial functions.[7][12] Some of the "home remedies" found on the Internet and elsewhere use mild ointments or creams to soften the papules, but others are physically dangerous techniques for papule removal which can result in permanent genital mutilation.[10]
With safe, effective ways to remove the papules if desired, home remedies involving corrosive substances or self-surgery can be damaging.[10]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 Aldahan, Adam S.; Brah, Tara K.; Nouri, Keyvan (May 2018). "Diagnosis and Management of Pearly Penile Papules". American Journal of Men's Health. 12 (3): 624–627. doi:10.1177/1557988316654138. ISSN 1557-9883. PMID 27316776. Archived from the original on 2021-02-12. Retrieved 2021-09-25.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 Love, Lauren W.; Badri, Talel; Ramsey, Michael L. (2021). "Pearly Penile Papule". StatPearls. StatPearls Publishing. Archived from the original on 2020-11-11. Retrieved 2021-09-23.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "28. Dermal and subcutaneous tumors". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. p. 616. ISBN 978-0-323-54753-6. Archived from the original on 2021-10-19. Retrieved 2021-10-19.
- ↑ 4.0 4.1 4.2 4.3 Johnstone, Ronald B. (2017). "34. Fibrous tumors and tumor-like proliferations". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 614. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2021-09-24.
- ↑ 5.0 5.1 Passos, Mauro Romero Leal (2017). "11. Differential diagnosis". Atlas of Sexually Transmitted Diseases: Clinical Aspects and Differential Diagnosis. Springer. p. 383. ISBN 978-3-319-57470-7. Archived from the original on 2022-06-10. Retrieved 2022-06-06.
- ↑ 6.0 6.1 Kumar P, Das A, Savant SS (2015). "Multiple Shiny Papules on the Shaft of the Penis". Indian Journal of Dermatology. 60 (3): 325. doi:10.4103/0019-5154.156491. PMC 4458986. PMID 26120199.
- ↑ 7.0 7.1 7.2 7.3 7.4 French, Kathy (2009). Sexual Health. Chichester: Wiley-Blackwell. pp. 31–32. ISBN 978-1-4051-6831-1. Archived from the original on 2021-09-25. Retrieved 2021-09-24.
- ↑ 8.0 8.1 Li H (28 August 2015). Radiology of Infectious Diseases:. Springer. p. 405. ISBN 9789401798822.
- ↑ Honigman, AD; Dubin, DP; Chu, J; Lin, MJ (2020). "Management of Pearly Penile Papules: A Review of the Literature". Journal of cutaneous medicine and surgery. 24 (1): 79–85. doi:10.1177/1203475419887730. PMID 31690111.
- ↑ 10.0 10.1 10.2 Rapini RP, Bolognia JL, Jorizzo JL (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 1-4160-2999-0.
- ↑ 11.0 11.1 Brown, Clarence W (8 July 2020). "Pearly Penile Papules: Background, Pathophysiology, Etiology". Medscape. Archived from the original on 20 October 2021. Retrieved 20 October 2021.
- ↑ 12.0 12.1 Pattman R, Snow M, Handy P, Elawad B. Oxford handbook of genitourinary medicine, HIV, and AIDS. Vol. 13.
- ↑ Agrawal, Subhav Kumar; Bhattacharya, Sambit Nath; Singh, Navjeevan (March 2004). "Pearly penile papules: a review". International Journal of Dermatology. 43 (3): 199–201. doi:10.1111/j.1365-4632.2004.02057.x. ISSN 0011-9059. PMID 15009391.
- ↑ Sanchez, Isabella; Raffi, Jodie; Kraus, Christina N. (23 February 2022). "Vulvar Neoplasms (Part II)". Urology: S0090–4295(22)00151–0. doi:10.1016/j.urology.2022.02.007. ISSN 1527-9995. PMID 35218865. Archived from the original on 27 February 2022. Retrieved 6 June 2022.
- ↑ Paller, Amy S.; Mancini, Anthony J. (2020). "9. Cutaneous tumors and tumor syndromes". Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence (6th ed.). St Louis, Missouri: Elsevier. p. 251. ISBN 978-0-323-54988-2. Archived from the original on 2021-09-25. Retrieved 2021-09-25.
- ↑ Marwah, Deepak (2019). Final Edge: Image-based Questions (3rd ed.). New Delhi: Jaypee Brothers Medical Publishers. p. 358. ISBN 978-93-5270-431-6. Archived from the original on 2021-09-25. Retrieved 2021-09-25.
External links
| Classification | |
|---|---|
| External resources |