Pancreatic mucinous cystic neoplasm
| Pancreatic mucinous cystic neoplasm | |
|---|---|
| Other names: MCN | |
| Specialty | Gastroenterology |
| Complications | Pancreatic cancer |
| Usual onset | 40-60 years of age |
| Risk factors | Female gender, older age |
| Treatment | Surgical resection |
Pancreatic mucinous cystic neoplasm (MCN) is a type of cystic lesion that occurs in the pancreas. Amongst individuals undergoing surgical resection of a pancreatic cyst, about 23 percent were mucinous cystic neoplasms. These lesions are benign, though there is a high rate of progression to cancer. As such, surgery should be pursued when feasible. The rate of malignancy present in MCN is about 10 percent.[1] If resection is performed before invasive malignancy develops, prognosis is excellent. The extent of invasion is the single most important prognostic factor in predicting survival.[2]
Signs and symptoms
The clinical presentation of Pancreatic mucinous cystic neoplasm is the following:[3]
- Abdominal pain
- Weight loss
- Acute pancreatitis
- Fatigue
Pathology
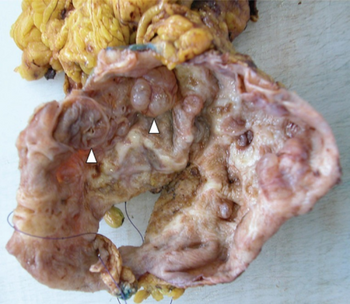
Histologic evaluation of MCNs shows mucin-producing columnar epithelial lining, which is surrounded by ovarian-like stroma.[1] Calcification may be present. Factors that predict malignancy include loculated appearance, mural nodules, papillary projections, p53 immunoreactivity, and loss of ovarian-like stroma.[2]
Diagnosis
The diagnosis of pancreatic MCN is typically achieved with imaging. If the results of imaging (CT/MRI) are unclear, then endoscopic ultrasound with fine needle aspiration (EUS-FNA) of the cyst may be necessary.[1] Cyst fluid analysis may help distinguis potentially premalignant mucinous cysts (MCNs and IPMNs), from benign non-mucinous cysts.[1] However, cyst fluid analysis cannot rule out the presence of pancreatic cancer or high grade dysplasia.[1]
Management
Where possible, surgical resection of mucinous cystic neoplasms is preferable. In individuals who are eligible to undergo surgery, who are found to have asymptomatic cysts that appear to be benign MCNs or IPMNs, then surveillance imaging may be considered.[1]
Following surgery, if resected tissue consists only of MCN without cancer, then further postoperative surveillance imaging is not necessary.[1]
In individuals unable to undergo surgery, there may be a role for endoscopic ultrasound (EUS) guided ablation with alcohol lavage with paclitaxel injection. EUS guided therapy has been performed successfully, though more data is necessary, particularly prospective study.[4][5] An EUS-guided approach appears more effective with smaller sized MCNs.[6]
Epidemiology

MCNs are much more common in women.[8] A study in 2012 found that amongst individuals undergoing surgical resection of a pancreatic cyst, about 23 percent were mucinous cystic neoplasms.[9] The rate of malignancy present in MCN is about 10 percent.[1] Malignancy is more often present in older individuals.[10]
See also
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Elta, GH; Enestvedt, BK; Sauer, BG; Lennon, AM (April 2018). "ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts". The American Journal of Gastroenterology. 113 (4): 464–479. doi:10.1038/ajg.2018.14. PMID 29485131. S2CID 3584079.
- ↑ 2.0 2.1 Zamboni, G; Scarpa, A; Bogina, G; Iacono, C; Bassi, C; Talamini, G; Sessa, F; Capella, C; Solcia, E; Rickaert, F; Mariuzzi, GM; Klöppel, G (April 1999). "Mucinous cystic tumors of the pancreas: clinicopathological features, prognosis, and relationship to other mucinous cystic tumors". The American Journal of Surgical Pathology. 23 (4): 410–22. doi:10.1097/00000478-199904000-00005. PMID 10199470.
- ↑ Babiker, Hani M.; Hoilat, Gilles J.; Mukkamalla, Shiva Kumar R. (2022). "Mucinous Cystic Pancreatic Neoplasms". StatPearls. StatPearls Publishing. Archived from the original on 1 February 2022. Retrieved 28 September 2022.
- ↑ Gan, SI; Thompson, CC; Lauwers, GY; Bounds, BC; Brugge, WR (May 2005). "Ethanol lavage of pancreatic cystic lesions: initial pilot study". Gastrointestinal Endoscopy. 61 (6): 746–52. doi:10.1016/s0016-5107(05)00320-2. PMID 15855986.
- ↑ Oh, HC; Seo, DW; Lee, TY; Kim, JY; Lee, SS; Lee, SK; Kim, MH (April 2008). "New treatment for cystic tumors of the pancreas: EUS-guided ethanol lavage with paclitaxel injection". Gastrointestinal Endoscopy. 67 (4): 636–42. doi:10.1016/j.gie.2007.09.038. PMID 18262182.
- ↑ Oh, HC; Seo, DW; Song, TJ; Moon, SH; Park, DH; Soo Lee, S; Lee, SK; Kim, MH; Kim, J (January 2011). "Endoscopic ultrasonography-guided ethanol lavage with paclitaxel injection treats patients with pancreatic cysts". Gastroenterology. 140 (1): 172–9. doi:10.1053/j.gastro.2010.10.001. PMID 20950614.
- ↑ Wang Y, Miller FH, Chen ZE, Merrick L, Mortele KJ, Hoff FL; et al. (2011). "Diffusion-weighted MR imaging of solid and cystic lesions of the pancreas". Radiographics. 31 (3): E47-64. doi:10.1148/rg.313105174. PMID 21721197.
{{cite journal}}: CS1 maint: multiple names: authors list (link)
Diagram by Mikael Häggström, M.D. - ↑ Reddy, RP; Smyrk, TC; Zapiach, M; Levy, MJ; Pearson, RK; Clain, JE; Farnell, MB; Sarr, MG; Chari, ST (November 2004). "Pancreatic mucinous cystic neoplasm defined by ovarian stroma: demographics, clinical features, and prevalence of cancer". Clinical Gastroenterology and Hepatology. 2 (11): 1026–31. doi:10.1016/s1542-3565(04)00450-1. PMID 15551256.
- ↑ Valsangkar, NP; Morales-Oyarvide, V; Thayer, SP; Ferrone, CR; Wargo, JA; Warshaw, AL; Fernández-del Castillo, C (September 2012). "851 resected cystic tumors of the pancreas: a 33-year experience at the Massachusetts General Hospital". Surgery. 152 (3 Suppl 1): S4-12. doi:10.1016/j.surg.2012.05.033. PMC 3806101. PMID 22770958.
- ↑ Crippa, Stefano; Salvia, Roberto; Warshaw, Andrew L.; Domínguez, Ismael; Bassi, Claudio; Falconi, Massimo; Thayer, Sarah P.; Zamboni, Giuseppe; Lauwers, Gregory Y.; Mino-Kenudson, Mari; Capelli, Paola; Pederzoli, Paolo; Castillo, Carlos Fernández-del (April 2008). "Mucinous Cystic Neoplasm of the Pancreas is Not an Aggressive Entity". Annals of Surgery. 247 (4): 571–579. doi:10.1097/SLA.0b013e31811f4449. PMC 3806104. PMID 18362619.