Opicapone
 | |
| Names | |
|---|---|
| Trade names | Ongentys |
| Other names | BIA 9-1067 |
| |
| Clinical data | |
| Drug class | Catechol-O-methyltransferase (COMT) inhibitor[1] |
| Main uses | Parkinson's disease[1][2] |
| Side effects | Difficulty controlling movement (dyskinesia), constipation, low blood pressure, weight loss, muscle breakdown[2] |
| Pregnancy category |
|
| Routes of use | By mouth (capsules) |
| Duration of action | >24 hours |
| External links | |
| AHFS/Drugs.com | Monograph |
| Legal | |
| License data | |
| Legal status | |
| Pharmacokinetics | |
| Bioavailability | ~20% |
| Protein binding | 99.9% |
| Metabolism | Mainly sulfation, also reduction, glucuronidation, methylation |
| Elimination half-life | 0.7 to 3.2 hours |
| Excretion | Feces (67%), urine (13%) |
| Chemical and physical data | |
| Formula | C15H10Cl2N4O6 |
| Molar mass | 413.17 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
Opicapone, sold under the brand name Ongentys, is a medication used with levodopa/carbidopa for Parkinson's disease.[1][2] Specifically it is used for fluctuation in motor function before the next dose of levodopa.[6] Benefits are similar to entacapone.[2] It is taken by mouth.[1]
Common side effects include difficulty controlling movement (dyskinesia).[1] Other side effects may include constipation, low blood pressure, weight loss, and muscle breakdown.[2] It works by enhancing the effects of levodopa and thus dopamine in the parts of the brain that control movement and coordination.[1] It does this by blocks an enzyme involved in the breakdown of levodopa called catechol-O-methyltransferase (COMT).[1]
Opicapone was approved for medical use in Europe in 2016 and the United States in 2020.[1][2] In the United Kingdom a month of medication costs the NHS about £94 as of 2021.[6] This amount in the United States costs about 630 USD.[7]
Medical uses
In the EU, opicapone is indicated as adjunctive therapy to preparations of levodopa/ DOPA decarboxylase inhibitors (DDCI) in adults with Parkinson's disease and end-of-dose motor fluctuations who cannot be stabilised on those combinations.[1]
In the US, opicapone is indicated as adjunctive treatment to levodopa/carbidopa in patients with Parkinson's disease (PD) experiencing "off" episodes.[5][8]
The COMT inhibitor opicapone is used as an additive to a combination of levodopa and a DOPA decarboxylase inhibitor to treat people with Parkinson's disease experiencing end-of-dose motor fluctuations, if they cannot be stabilised with this drug combination.[9]
Dosage
It is taken at a dose of 50 mg at bedtime.[6]
Contraindications
This drug is contraindicated in people with cancers that secrete catecholamines (for example epinephrine), such as phaeochromocytoma or paraganglioma, because as a COMT inhibitor it blocks catecholamine degradation. Other contraindications are a history of neuroleptic malignant syndrome (NMS) or non-traumatic rhabdomyolysis, and combination with monoamine oxidase inhibitors that are not used as antiparkinsonians, because of possible drug interactions.[9]
NMS and associated rhabdomyolysis have been rarely observed under the older COMT inhibitors tolcapone and entacapone. This typically occurs shortly after the beginning of a COMT inhibitor add-on therapy when the levodopa dose has been reduced, or after discontinuation of a COMT inhibitor.[10]
Opicapone is contraindicated in people with concomitant use of non-selective monoamine oxidase (MAO) inhibitors or people with pheochromocytoma, paraganglioma, or other catecholamine secreting neoplasms.[5][1]
Side effects
People taking opicapone very commonly (18%) experience dyskinesia. Other common side effects (in 1 to 10% of patients) include dizziness, strange dreams, hallucinations, constipation, dry mouth, orthostatic hypotension (low blood pressure), and muscle spasms.[9] Apart from spasms, these side effects are also known from tolcapone and entacapone.[10]
As with entacapone, no relevant liver toxicity has been found in studies. This is in contrast to the first COMT inhibitor tolcapone, which could cause – in some cases lethal – liver insufficiency.[10][11]
Overdose
No specific antidote is known.[9]
Interactions
Monoamine oxidase inhibitors (MAO inhibitors) are another class of drugs blocking catecholamine degradation. Therefore, their combination with opicapone can result in increased catecholamine concentrations in the body and corresponding adverse effects. Combining the antiparkinson MAO inhibitors selegiline or rasagiline with opicapone is considered safe. Potentially, there are also interactions with drugs being metabolised by COMT (for example isoprenaline, epinephrine, dopamine, or dobutamine), tricyclic antidepressants and antidepressants of the norepinephrine reuptake inhibitor type. Possible pharmacokinetic interactions are with substrates of the liver enzyme CYP2C8, such as repaglinide, and the transporter protein SLCO1B1, such as simvastatin.[9]
Pharmacology
Mechanism of action
Opicapone blocks the enzyme catechol-O-methyltransferase (COMT) effectively (>90% at therapeutic doses), selectively and reversibly, and only outside the central nervous system. It dissociates slowly from COMT, resulting in a duration of action longer than 24 hours despite its short blood plasma half-life.[9][11] As COMT and DOPA decarboxylase are the main enzymes for degrading levodopa, blocking the two effectively increases its concentrations in the bloodstream. More levodopa reaches the brain, where it is activated to dopamine.[12]
Pharmacokinetics
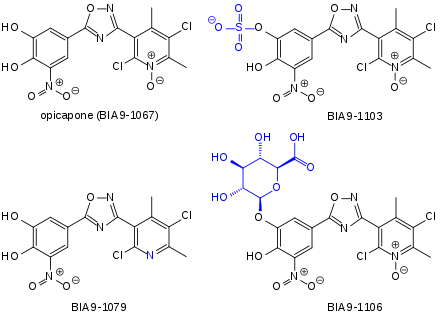
The substance is quickly absorbed from the gut, but only to about 20% of the applied dose. Highest blood plasma concentrations are reached after 1 to 2.5 hours. When in the bloodstream, it is almost completely (99.9%) bound to plasma proteins, but apparently to different binding sites than warfarin, digoxin and other drugs with high plasma protein affinity. It is mainly metabolised to the sulfate, which accounts for 67% of the circulating drug after a single dose, and a methylated derivative, which accounts for 21%. Minor metabolites are a reduced derivative (<10%) and a glucuronide. All of these metabolites are inactive except the reduced derivative. Opicapone is eliminated with a terminal half-life of 0.7 to 3.2 hours. It is mainly excreted via the faeces (67%), and in form of the glucuronide also via the kidney (13%). The sulfate has a much longer half-life of 94 to 122 hours.[9][11][13]
Opicapone sulfate is transported by SLCO1B1; the possibility that it blocks this transporter has not been excluded. Opicapone itself and the sulfate are also transported by a number of other proteins, but given the low concentrations of the free substances in the blood plasma, this is very unlikely to give rise to drug interactions. Opicapone is a weak inhibitor of the liver enzymes CYP1A2, CYP2B6, CYP2C8, and CYP2C9. The only CYP interaction found in studies that is somewhat likely to be relevant is that with repaglinide, which is metabolised by CYP2C8. The metabolism of warfarin, a CYP2C9 substrate, is not measurably affected.[9]
History
Opicapone was authorised for medical use in the European Union in June 2016.[1][14]
In February 2017, its developer Bial sold exclusive marketing rights for the United States and Canada to Neurocrine Biosciences for an initial payment of US$30 million.[15]
Opicapone was authorised for medical use in the United States in April 2020.[16][8][14]
Opicapone was approved based on evidence from two clinical trials (Trial 1/ NCT01568073, and Trial 2/NCT01227655) of 522 participants with Parkinson's disease (PD) whose symptoms were not well controlled while receiving their regular PD treatment.[8] Trial 1 was conducted at 104 sites in 19 European countries, and Trial 2 was conducted at 69 sites in Argentina, Australia, Belgium, Chile, Czech Republic, Estonia, India, Israel, South Korea, Russia, South Africa and UK.[8]
There were two 12-week trials conducted in Parkinson's disease (PD) participants with inadequate control of their Parkinson's symptom ("off" time) while receiving carbidopa/levodopa PD medications.[8] Participants were randomly selected to receive either opicapone or a placebo capsule once a day.[8] Neither the participants nor the health care providers knew which treatment was being given until the trial was completed.[8]
In all of the trials, the participants kept daily diaries of the number of hours of "off" time for the three days before the evaluation visit.[8] The benefit was evaluated by measuring the change from baseline in total daily "off" time in opicapone- and placebo-receiving participants.[8]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 "Ongentys EPAR". European Medicines Agency. Archived from the original on 9 May 2020. Retrieved 28 April 2020. Text was copied from this source which is © European Medicines Agency. Reproduction is authorized provided the source is acknowledged.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 "Opicapone Monograph for Professionals". Drugs.com. Archived from the original on 22 June 2020. Retrieved 8 November 2021.
- ↑ "Archive copy" (PDF). Archived (PDF) from the original on 13 June 2021. Retrieved 13 June 2021.
{{cite web}}: CS1 maint: archived copy as title (link) - ↑ "Ongentys 50 mg hard capsules - Summary of Product Characteristics (SmPC)". (emc). 18 July 2019. Archived from the original on 4 June 2020. Retrieved 28 April 2020.
- ↑ 5.0 5.1 5.2 "Ongentys- opicapone capsule". DailyMed. 24 April 2020. Archived from the original on 25 October 2021. Retrieved 30 September 2020.
- ↑ 6.0 6.1 6.2 BNF 81: March-September 2021. BMJ Group and the Pharmaceutical Press. 2021. p. 433. ISBN 978-0857114105.
- ↑ "Ongentys Prices, Coupons & Patient Assistance Programs". Drugs.com. Retrieved 8 November 2021.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 8.8 "Drug Trials Snapshots: Ongentys". U.S. Food and Drug Administration (FDA). 24 April 2020. Archived from the original on 21 September 2020. Retrieved 13 May 2020.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 "Ongentys: EPAR – Product Information" (PDF). European Medicines Agency (EMA). 28 January 2020. Archived (PDF) from the original on 7 October 2018. Retrieved 13 June 2021.
- ↑ 10.0 10.1 10.2 Haberfeld H, ed. (2017). Austria-Codex (in Deutsch). Vienna: Österreichischer Apothekerverlag. Comtan, Tasmar.
- ↑ 11.0 11.1 11.2 Annus Á, Vécsei L (2017). "Spotlight on opicapone as an adjunct to levodopa in Parkinson's disease: design, development and potential place in therapy". Drug Design, Development and Therapy. 11: 143–151. doi:10.2147/DDDT.S104227. PMC 5234693. PMID 28123288.
- ↑ Mutschler E, Schäfer-Korting M (2001). Arzneimittelwirkungen (in Deutsch) (8th ed.). Stuttgart: Wissenschaftliche Verlagsgesellschaft. p. 315. ISBN 3-8047-1763-2.
- ↑ 13.0 13.1 Rocha JF, Almeida L, Falcão A, Palma PN, Loureiro AI, Pinto R, et al. (November 2013). "Opicapone: a short lived and very long acting novel catechol-O-methyltransferase inhibitor following multiple dose administration in healthy subjects". British Journal of Clinical Pharmacology. 76 (5): 763–75. doi:10.1111/bcp.12081. PMC 3853535. PMID 23336248.
- ↑ 14.0 14.1 "Neurocrine Biosciences Announces FDA Approval of Once-Daily Ongentys (opicapone) as an Add-On Treatment for Patients with Parkinson's Disease Experiencing "Off" Episodes". Neurocrine Biosciences (Press release). 27 April 2020. Archived from the original on 28 April 2020. Retrieved 28 April 2020.
- ↑ "Brief: Neurocrine and Bial reports exclusive North American licensing agreement for opicapone". Reuters. 9 February 2017. Archived from the original on 8 August 2019. Retrieved 13 June 2021.
- ↑ "Ongentys: FDA-Approved Drugs". U.S. Food and Drug Administration (FDA). Archived from the original on 28 April 2020. Retrieved 28 April 2020.
External links
- Rodrigues FB, Ferreira JJ (March 2017). "Opicapone for the treatment of Parkinson's disease" (PDF). Expert Opin Pharmacother. 18 (4): 445–453. doi:10.1080/14656566.2017.1294683. PMID 28234566. S2CID 5251815. Archived (PDF) from the original on 25 October 2021. Retrieved 13 June 2021.
- Scott LJ (September 2016). "Opicapone: A Review in Parkinson's Disease". Drugs. 76 (13): 1293–1300. doi:10.1007/s40265-016-0623-y. PMID 27498199. S2CID 5787752.
| External sites: | |
|---|---|
| Identifiers: |
|
- Pages using duplicate arguments in template calls
- Pages with non-numeric formatnum arguments
- CS1 maint: archived copy as title
- Wikipedia articles incorporating the PD-notice template
- CS1 Deutsch-language sources (de)
- Use dmy dates from April 2017
- Articles with invalid date parameter in template
- Use list-defined references from April 2017
- Use British English from April 2017
- Drugs with non-standard legal status
- Chemical articles with unknown parameter in Infobox drug
- Chemical articles without CAS registry number
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Chemical pages without DrugBank identifier
- Articles without KEGG source
- Articles without UNII source
- Drugs missing an ATC code
- Drug has EMA link
- Articles containing unverified chemical infoboxes
- Amine oxides
- Catechol-O-methyltransferase inhibitors
- Catechols
- Nitrophenols
- Oxadiazoles
- RTT