Onycholysis
| Onycholysis | |
|---|---|
 | |
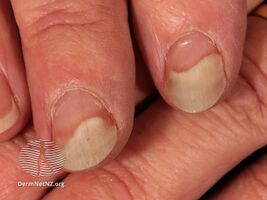
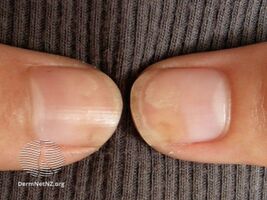
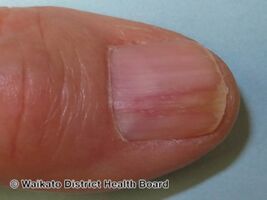
| Left hand onycholysis: ring and little fingers affected | |
| Pronunciation | |
Onycholysis is a common medical condition characterized by the painless detachment of the nail from the nail bed, usually starting at the tip and/or sides.[1] It may be complicated by P. aeruginosa.[2]
Onycholysis may occur in psoriasis, contact dermatitis, fungal infections of the nail, following trauma, with nail bed tumors, and with some medicines such as doxycycline.[2] In thyrotoxicosis, it is thought to be due to sympathetic overactivity.[3] It may also be seen in infections or trauma.[4]
Causes
- Unknown
- Trauma, excessive manicuring
- Infection: especially fungal
- Skin disease: psoriasis, dermatitis
- Impaired peripheral circulation, e.g. Raynaud's syndrome
- Systemic disease: hyperthyroidism, hypothyroidism, reactive arthritis, porphyria cutanea tarda
- Reaction to detergents (e.g. washing dishes with bare hands, using detergent-based shampoos or soaps).[5][6][7]
- Patients with hepatocellular dysfunction may develop hair-thinning or hair loss and nail changes such as clubbing, leukonychia (whitening), or onycholysis, affecting the nails of the hands and feet.[8]
- Onychomycosis (tinea)
- It is common in ballet dancers[9]
- Chemotherapy (cytotoxic agents like taxanes, vinca alkaloids and others)
Treatment
Most instances of onycholysis without a clear cause will heal spontaneously within a few weeks. The most commonly recommended treatment is to keep the nail dry as much as possible and allow the nail to slowly reattach. Trimming away as much loose nail as can be done comfortably will prevent the nail from being pried upwards. Cleaning under the nail is not recommended as this only serves to separate the nail further. Bandages are also to be avoided.[10] When kept dry and away from further trauma, the nail will reattach from the base upward (i.e., from proximal to distal).
If the underlying cause of the condition is not found and the nail continues to detach despite conservative treatment, the nail bed may begin to form a granular layer of abnormal cells on its surface. After six months of detachment, this layer is likely to prevent the adhesion of any new nail tissue, possibly leading to permanent deformity.[11]
Etymology
The word onycholysis comes from onycho-, from Ancient Greek ὄνυξ ónuks 'nail', and Ancient Greek λύσις lúsis 'a loosening'.
Additional images
-
Psoriatic onycholysis
-
Drug-induced onycholysis
-
Erythronychia, onycholysis
See also
References
- ↑ Bolognia, Jean L.; Schaffer, Julie V.; Duncan, Karynne O.; Ko, Christine (2021). "58. Nail disorders". Dermatology Essentials (2nd ed.). Elsevier. pp. 564–565. ISBN 978-0-323-62453-4. Archived from the original on 2024-01-20. Retrieved 2024-01-17.
- ↑ 2.0 2.1 Saavedra, Arturo; Roh, Ellen K.; Mikailov, Anar (2023). "32.Disorders of the nail apparatus". Fitzpatrick's Color Atlas and Synopsis of Clinical Dermatology (9th ed.). New York: McGraw Hill Professional. pp. 849–872. ISBN 978-1-264-27801-5. Archived from the original on 2023-12-31. Retrieved 2024-01-18.
- ↑ Talley&O'Connor (2006). Clinical Examination A Systematic Guide to Physical Diagnosis (5th ed.). Elsevier. p. 262. ISBN 978-0-7295-3762-9.
- ↑ Weber&Kelley (2010). Health Assessment in Nursing (4th ed.). Wolters Kluwer Health and Lippincott, Williams & Wilkins. pp. 193. ISBN 978-0-7817-8160-2.
- ↑ Mayon-White, R. T.; Hodgson, G. (1971-08-07). "Acute onychia and onycholysis due to an enzyme detergent". Br Med J. 3 (5770): 352. doi:10.1136/bmj.3.5770.352. ISSN 0007-1447. PMC 1798590. PMID 5558190.
- ↑ Al-Kathiri, Lutfi; Al-Asmaili, Abla (2016). "Diclofenac-Induced Photo-Onycholysis". Oman Medical Journal. 31 (1): 65–68. doi:10.5001/omj.2016.12. ISSN 1999-768X. PMC 4720947. PMID 26816569.
- ↑ Alevizos, Alevizos; Gregoriou, Stamatis; Larios, George; Rigopoulos, Dimitris (2008-02-01). "Acute and Chronic Paronychia". American Family Physician. 77 (3): 339–346. ISSN 0002-838X. PMID 18297959. Archived from the original on 2020-08-11. Retrieved 2021-02-26.
- ↑ Hazin, Ribhi; Tamimi, Tarek I. Abu-Rajab; Abuzetun, Jamil Y.; Zein, Nizar N. (October 2009). "Recognizing and treating cutaneous signs of liver disease". Cleveland Clinic Journal of Medicine. 76 (10): 599–606. doi:10.3949/ccjm.76A.08113. ISSN 0891-1150. PMID 19797460. Archived from the original on 2020-01-09. Retrieved 2021-02-26.
- ↑ Shah, Selina (April 2010). "Pointe shoes complicate biomechanics of ballet". Lower Extremity Review Magazine. Archived from the original on 2021-08-28. Retrieved 2021-02-26.
- ↑ "Onycholysis". American Osteopathic College of Dermatology. Archived from the original on 30 December 2016. Retrieved 29 December 2016.
- ↑ Richard K. Scherr (1 December 1997). "The Nail Doctor: Onycholysis, or Nail Separation, Has Different Varieties". Nails Magazine. Archived from the original on 2 July 2018. Retrieved 26 February 2021.
External links
| Classification |
|---|