Nevus of Ota
| Nevus of Ota | |
|---|---|
| Other names: Congenital melanosis bulbi,[1] nevus fuscoceruleus ophthalmomaxillaris, oculodermal melanocytosis,[2]: 700 oculomucodermal melanocytosis[1] | |
 | |
| Symptoms | Blue-brown area of skin typically on the forehead and cheeks from birth[3] |
| Frequency | Females>males[3] |
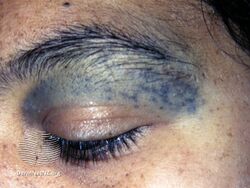
Nevus of Ota is a blue-brown area of skin made up of many flat spots merged together, typically on the forehead and cheeks, and present from birth.[3]
Females are affected more frequently than males.[3] It is more common than nevus of Ito.[4] Masao Ōta of Japan first described the condition in 1939.[4]
Signs and symptoms
-
Nevus of Ota
-
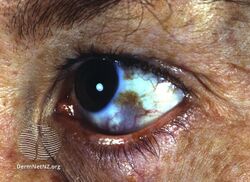
Nevus of Ota
-
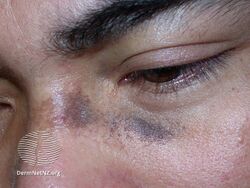
Nevus of Ota
Cause
Nevus of Ota is caused by the entrapment of melanocytes in the upper third of the dermis. It is found only on the face, most commonly unilaterally, rarely bilaterally and involves the first two branches of the trigeminal nerve. The sclera is involved in two-thirds of cases (causing an increased risk of glaucoma). It should not be confused with Mongolian spot, which is a birthmark caused by entrapment of melanocytes in the dermis but is located in the lumbosacral region.[5]
Treatment
A Q-switched 1064 nm laser has been successfully used to treat the condition.[6][7] The Q-Switched Lasers (694 nm Ruby, 755 nm Alexandrite or 1064 nm Nd-YAG) with their high peak power and pulse width in nano second range are best suited to treat various epidermal, junctional, mixed and dermal lesions The Q-switched 1064 nm Nd-YAG is an ideal choice to treat dermal pigment as in nevus of Ota and in darker skin types, as it reduces the risk of epidermal injury and pigmentary alterations. The pigment clearance may be expected to be near total. Usually a number of treatment sessions with an interval of minimum six weeks are required to achieve total or near total clearance. The number of treatments depend mainly on the severity of the lesion. Darker the lesion, more are the treatments required. It also depends to some extent on the quality of the laser system used and its energy output. Last but not the least, experience of the laser surgeon plays a significant role in achieving early and good clearance.[8]
Epidemiology
Females are nearly five times more likely to be affected than males, and it is rare among Caucasians.[5]
History
Masao Ōta of Japan first described the condition in 1939.[4]
See also
References
- ↑ 1.0 1.1 Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph (2007). Dermatology: 2-Volume Set. St. Louis, Missouri: Mosby. pp. 1720–22. ISBN 978-1-4160-2999-1.
- ↑ James, William D.; Berger, Timothy G. (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Philadelphia, Pennsylvania: Saunders Elsevier. ISBN 0-7216-2921-0.
- ↑ 3.0 3.1 3.2 3.3 Johnstone, Ronald B. (2017). "32. Lentigines and melanomase". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 544. ISBN 978-0-7020-6830-0. Archived from the original on 2023-07-01. Retrieved 2023-06-29.
- ↑ 4.0 4.1 4.2 DE, Elder; D, Massi; RA, Scolyer; R, Willemze (2018). "2. Melanocytic tumours: Naevus of Ito and naevus of Ota". WHO Classification of Skin Tumours. Vol. 11 (4th ed.). Lyon (France): World Health Organization. p. 131. ISBN 978-92-832-2440-2. Archived from the original on 2022-07-11. Retrieved 2022-08-20.
- ↑ 5.0 5.1 Sancton, Julian (September 2011). "Daniela Ruah Officially Checks In". Esquire. New York City: Hearst Corporation. Archived from the original on December 15, 2017. Retrieved June 9, 2016.
- ↑ Geronemus, Roy G. (December 1992). "Q-switched ruby laser therapy of nevus of Ota". Archives of Dermatology. Chicago, Illinois: American Medical Association. 128 (12): 1618–22. Bibcode:1992SPIE.1643..284G. doi:10.1001/archderm.1992.04530010056008. PMID 1456756.
- ↑ Watanabe, Shinichi; Takahashi, Hisashi (December 1, 1994). "Treatment of nevus of Ota with the Q-switched ruby laser". New England Journal of Medicine. Waltham, Massachusetts: Massachusetts Medical Society. 331 (26): 1745–50. doi:10.1056/NEJM199412293312604. PMID 7984195.
- ↑ Patil, Uddhav A.; Dhami, Lakshyajit D. (October 2008). "Overview of Lasers". Indian Journal of Plastic Surgery. Mumbai, India: Medknow Publications. 41 (Supplement): 101–113. doi:10.1055/S-0039-1700481. PMC 2825126. Archived from the original on 2021-08-28. Retrieved 2021-02-28.
| Classification | |
|---|---|
| External resources |