Neurogenic shock
| Neurogenic shock | |
|---|---|
| Other names: Vasogenic shock[1] | |
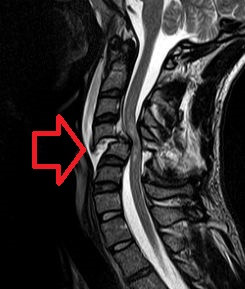 | |
| Cervical spine MRI showing a C4 fracture and dislocation resulting in spinal cord compression | |
| Specialty | Spinal surgery |
| Symptoms | Low blood pressure, low heart rate, warm skin, abnormal body temperature[1] |
| Complications | Organ dysfunction[2] |
| Duration | 4 to 12 weeks[3] |
| Causes | Spinal cord injury above T4, spinal anesthesia, Guillain-Barre syndrome, autonomic nervous system toxins, transverse myelitis, other neuropathies[2][1] |
| Diagnostic method | Based on symptoms and medical imaging after ruling out other possible cases[1] |
| Differential diagnosis | Spinal shock, hypovolemic shock, other types of circulatory shock[1] |
| Treatment | Intravenous fluids, C-spine motion restriction, norepinephrine[1] |
| Frequency | Relatively uncommon[4] |
Neurogenic shock is a type of shock due to spinal cord injury.[1] Symptoms may include low blood pressure, low heart rate, warm skin, and abnormal body temperature.[1] It starts at the time of injury and may last for 4 to 12 weeks.[3] Complications can include organ dysfunction.[2]
The cause is generally a spinal cord injury above the fourth thoracic vertebrae.[2] Other causes may include spinal anesthesia, Guillain-Barre syndrome, autonomic nervous system toxins, transverse myelitis, and other neuropathies.[1] The underlying mechanism involves loss of sympathetic tone.[1] It is a type of distributive shock.[2] Diagnosis is based on symptoms and medical imaging after ruling out other possible cases.[1] It differs from spinal shock, which refers to loss of sensation, reflexes, and motor function, though may be associated with neurogenic shock.[1]
The initial treatment is generally with intravenous fluids and C-spine motion restriction.[1] If this is not sufficient norepinephrine is often used to keep the mean arterial pressure greater than 90 mmHg.[1] The slow heart rate may be treated with atropine.[1] Surgery may be required to stabilize the spine.[1] Neurogenic shock is relatively uncommon.[4] It occurs in about 19% of cervical and 7% of thoracic spinal cord injuries.[1][3]
Signs and symptoms
- Instantaneous hypotension due to sudden, massive vasodilation and decrease in blood saturation
- Warm, flushed skin due to vasodilation and inability to constrict blood vessels.
- Priapism, also due to vasodilation
- The patient will be unable to get tachycardic, and may become bradycardic
- If the injury is below C5, the patient will exhibit diaphragmatic breathing due to loss of nervous control of the intercostal muscles (which are required for thoracic breathing).
- The patient will go into respiratory arrest immediately following the injury, due to loss of nervous control of the diaphragm.
Causes
Neurogenic shock can result from severe central nervous system damage (brain injury, cervical or high thoracic spinal cord).[5] In more simple terms: the trauma causes a sudden loss of background sympathetic stimulation to the blood vessels. This causes them to relax (vasodilation)[6] resulting in a sudden decrease in blood pressure (secondary to a decrease in peripheral vascular resistance).
Neurogenic shock results from damage to the spinal cord above the level of the 6th thoracic vertebra.[7] It is found in about half of people who suffer spinal cord injury within the first 24 hours, and usually doesn't go away for one to three weeks.[7]
Diagnosis
Neurogenic shock is diagnosed based on a person's symptoms and blood pressure levels. Neurogenic shock's presentation includes:[9][10]warm and pink skin,labored breathing , low blood pressure , dizziness, anxiety, history of trauma to head or upper spine, if the injury is to the head or neck, hoarseness or difficulty swallowing may occur.
Symptoms of neurogenic shock are differentiated from other forms of shock, by the lack of signs of the compensatory mechanisms triggered by the sympathetic nervous system on other forms of shock via the release of epinephrine and norepinephrine. Signs caused by these neurotransmitters are typically lacking in where shock is of neurogenic origin include: increased heart rate, faster breathing, and sweating, and adaptive vasoconstriction, which serves in other forms of shock to shunt blood away from the extremities and to the vital organs.
In neurogenic shock, the body loses its ability to activate the sympathetic nervous system so that only parasympathetic tone remains. The resulting loss of sympathetic tone, which plays a major role in other forms of shock is responsible for the unique and atypical features mentioned above.[9]
Treatment
- Dopamine (medication) is often used either alone or in combination with other inotropic agents.
- Vasopressin[11]
- Certain vasopressors (ephedrine, norepinephrine (medication)). Phenylephrine may be used as a first line treatment, or secondarily in people who do not respond adequately to dopamine.
- Atropine is administered for slowed heart rate.[12]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 Dave, S; Cho, JJ (January 2020). "Neurogenic Shock". PMID 29083597.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 2.0 2.1 2.2 2.3 2.4 "Shock - Critical Care Medicine". Merck Manuals Professional Edition. Archived from the original on 27 November 2020. Retrieved 5 January 2021.
- ↑ 3.0 3.1 3.2 Chhabra, Harvinder Singh (2015). ISCoS Textbook on Comprehensive management of Spinal Cord Injuries. Wolters kluwer india Pvt Ltd. p. 784. ISBN 978-93-5129-440-5. Archived from the original on 2021-08-28. Retrieved 2021-01-06.
- ↑ 4.0 4.1 Standl, T; Annecke, T; Cascorbi, I; Heller, AR; Sabashnikov, A; Teske, W (9 November 2018). "The Nomenclature, Definition and Distinction of Types of Shock". Deutsches Arzteblatt international. 115 (45): 757–768. doi:10.3238/arztebl.2018.0757. PMID 30573009.
- ↑ 4. Guly HR, Bouamra O, Lecky FE. The incidence of neurogenic shock in patients with isolated spinal cord injury in the emergency department. Resuscitation (2008) 76, 57-62
- ↑ "Dorlands Medical Dictionary:neurogenic shock". Archived from the original on 2009-05-09. Retrieved 2022-03-04.
- ↑ 7.0 7.1 Newman, Mark F.; Fleisher, Lee A.; Fink, Mitchell P. (2008). Perioperative Medicine: Managing for Outcome. Elsevier Health Sciences. p. 348. ISBN 978-1-4160-2456-9.
- ↑ Grigorean, VT; Sandu, AM; Popescu, M; Iacobini, MA; Stoian, R; Neascu, C; Popa, F (4 April 2009). "Cardiac dysfunctions following spinal cord injury". Journal of Medicine and Life. 2 (2). Retrieved 28 October 2022.
- ↑ 9.0 9.1 Mallek JT; Inaba K; et al. (2012). "The Incidence of Neurogenic Shock after Spinal Cord Injury in Patients Admitted to a High-Volume Level I Trauma Center". The American Surgeon. 78 (5): 623–626.
- ↑ Axelrad A, Pandya P, et al. (2013). "The Significance of Neurogenic Shock and Acute Spinal Cord Injury (Poster Session)". Critical Care Medicine. The Society of Critical Care Medicine and Lippincott Williams & Wilkins. doi:10.1097/01.ccm.0000439365.59627.b5.
- ↑ "Hypotension & Shock Treatment | health.am". Archived from the original on 2012-03-14. Retrieved 2011-01-18.
- ↑ Holtz, Anders; Levi, Richard (6 July 2010). Spinal Cord Injury. Oxford University Press. p. 63–4. ISBN 978-0-19-970681-5.
External links
| Classification |
|---|