Nephrogenic systemic fibrosis
| Nephrogenic systemic fibrosis | |
|---|---|
| Other names: NSF | |
| Causes | iatrogenic disease caused by exposure to gadolinium-based contrast agents |
| Risk factors | impaired kidney function is the major risk factor |
Nephrogenic systemic fibrosis is a rare syndrome that involves fibrosis of skin, joints, eyes, and internal organs. NSF is caused by exposure to gadolinium in gadolinium-based MRI contrast agents (GBCAs) in patients with impaired kidney function.[1][2] Epidemiological studies suggest that the incidence of NSF is unrelated to gender or ethnicity and it is not thought to have a genetic basis.[2][3] After GBCAs were identified as a cause of the disorder in 2006,[4] and screening and prevention measures put in place, it is now considered rare.[5]
Signs and symptoms
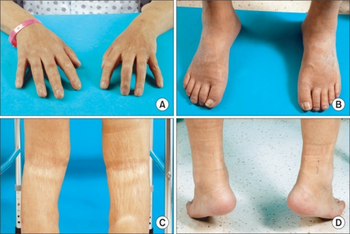
Clinical features of NSF develop within days to months following exposure to GBCA. The main symptoms are the thickening and hardening of the skin associated with brawny hyperpigmentation, typically presenting in a symmetric fashion. The skin gradually becomes fibrotic and adheres to the underlying fascia.[6][7] The symptoms initiate distally in the limbs and progress proximally, sometimes involving the trunk.[6] Joint contractures of the fingers, elbows and knees can develop secondary to skin involvement and can severely impair physical function.[6][8] While skin involvement is on the foreground, the process may involve any organ, e.g., the eye,[8] heart, diaphragm, pleura, pericardium, and kidneys,[6][9] as well as the lungs and liver.[10][11]
Causes
NSF is an iatrogenic disease caused by exposure to gadolinium-based contrast agents used in magnetic resonance imaging.[12]
Risk factors
Impaired kidney function reduces the clearance of GBCAs and is the major risk factor for the development of NSF. The etiology or duration of renal failure seems not to be relevant, but NSF risk greatly depends on the residual kidney function.[7] The majority of NSF cases have been identified in patients with stage 5 CKD,[8] but NSF has also developed in patients with stage 4 and 3 CKD, and those with acute kidney injury, even if kidney function subsequently returned to normal following GBCA administration.[13][14] Thus NSF should be considered as a differential diagnosis in any patient who has been exposed to a GBCA, regardless of the kidney function level.[8]
Three GBCAs have been principally implicated in NSF: gadodiamide, gadopentetate dimeglumine, and gadoversetamide, though cases have been reported with majority of GBCAs on the market.[15] High doses in individual GBCA administrations and high cumulative doses of GBCA over the lifetime of patients with renal dysfunction are associated with increased risk of NSF.[7]
Mechanism
De-chelation of Gd(III) is responsible for the toxicity associated with gadolinium complexes such as GBCAs, and the toxicity appears to be a consequence of Zn2+, Cu2+, and Ca2+ transmetallation in vivo.[12][15] This hypothesis is supported by acute toxicity experiments, which demonstrate that despite a 50-fold range of LDse values for four Gd(III) complexes, all become lethally toxic when they release precisely the same quantity of Gd(III).[16] It is also supported by subchronic rodent toxicity experiments, which demonstrate a set of gross and microscopic findings similar to those known to be caused by Zn2+ deficiency.[16] Under the transmetallation hypothesis, we can expect that subtle changes in formulation can affect the intrinsic safety of gadolinium complexes, which is indeed observed.[12][15]
Diagnosis
There is no specific imaging finding for NSF, and the diagnosis is a clinicopathological one, based on presentation and histological findings.[7]
Microscopic pathology
At the microscopic level, NSF shows a proliferation of dermal fibroblasts and dendritic cells, thickened collagen bundles, increased elastic fibers, and deposits of mucin.[17] More recent case reports have described the presence of sclerotic bodies (also known as elastocollagenous balls) in skin biopsies from NSF patients. While not universally present, this finding is believed to be unique to patients exposed to gadolinium, although not necessarily limited to areas involved by NSF.[18][19][20]
Differential diagnosis
The differential diagnoses for NSF include diffuse cutaneous or limited cutaneous systemic sclerosis, scleromyxedema, lipodermatosclerosis, scleroedema diabeticorum, graft versus host disease, eosinophilic fasciitis; eosinophilia-myalgia syndrome; porphyria cutanea tarda, and other disorders. The nearly universal absence of facial skin involvement in NSF, presence of yellow plaques on the sclera of the eyes, absence of Raynaud’s phenomenon, and other differences in presentation can aid the proper diagnosis. History of exposure to GBCAs would favor NSF as the differential diagnosis.[6][8]
Prevention
The only known measure for prevention of NSF is the non-use or cautious use of GBCAs in patients with renal impairment, including preferential use of safer, macrocyclic GBCAs. Performing dialysis immediately after the MRI exam is recommended for patients already in dialysis treatment, but there is no evidence for introducing dialysis in non-dialytic patients for prevention of NSF.[6] Screening for impaired kidney function is routinely conducted and has drastically reduced the incidence of NSF.[5]
Treatment
Multiple therapies for NSF have been attempted, with variable clinical improvement. None have been as effective as restoration of kidney function. Restoration of kidney function by treating the underlying disease process, recovery from acute kidney injury (AKI), or performing a kidney transplant can slow or hold the progression of NSF. A few cases of curative kidney transplantation have been reported, and it is appropriate to consider transplantation as treatment.[6][7]
Epidemiology
NSF affects males and females in approximately equal numbers and has been reported in patients of different ethnic and geographic regions. It most often affects middle-aged individuals, but there are reports of cases occurring from childhood to senescence.[6][7]
History
This condition was originally termed “nephrogenic fibrosing dermopathy” as initially only skin involvement in patients with impaired kidney function was observed, and later renamed “nephrogenic systemic fibrosis” to better describe its systemic nature.[12] The term "gadolinium-associated systemic fibrosis" has also been proposed to reflect the fact that impaired kidney function is not in itself the cause of NSF.[12]
The first cases of NSF were identified in 1997,[21] but it was first described as an independent disease entity in 2000.[22] In 2006, the link between NSF and gadolinium-based MRI contrast agents was made.[4][23][24] As a result, restrictions on use of GBCAs in patients with an estimated glomerular filtration rate (a measure of kidney function) under 60 and especially under 30 mL/min/1.73 m2 have been recommended and NSF is now considered rare.[5]
After several years of controversy, during which up to 100 Danish patients suffered gadolinium poisoning after use of the contrast agent Omniscan, the Norwegian medical company Nycomed admitted that they were aware of some dangers from using gadolinium-based agents in their product.[25]
With both Gadopentetic acid (gadopentetate dimegulumine (Magnevist)) and Gadodiamide (Omniscan) the risk was considered to outweigh the benefits and, as a result, the EMA recommended the licence for intravenous gadopentetic acid and Gadodiamide be suspended.[26]
Following a legally binding decision issued by The European Commission and applicable in all EU Member States (Commission decision date: 23/11/2017), Intravenous Magnevist and Omniscan is now no longer authorised for use in Europe. Magnavist is, however, still authorised in Europe as an intra-articular MR contrast medium. The authorised indication for the use of linear chelated media gadobenic acid (also known as gadobenate dimeglumine; MultiHance) and gadoxetic acid (Primovist) has been limited to delayed phase liver imaging only. [27]
References
- ↑ Thomsen HS, Morcos SK, Almén T, Bellin MF, Bertolotto M, Bongartz G, Clement O, Leander P, Heinz-Peer G, Reimer P, Stacul F, van der Molen A, Webb JA (February 2013). "Nephrogenic systemic fibrosis and gadolinium-based contrast media: updated ESUR Contrast Medium Safety Committee guidelines". European Radiology. 23 (2): 307–18. doi:10.1007/s00330-012-2597-9. PMID 22865271. S2CID 10493284.
- ↑ 2.0 2.1 Thomsen HS (September 2009). "Nephrogenic systemic fibrosis: history and epidemiology". Radiologic Clinics of North America. 47 (5): 827–31, vi. doi:10.1016/j.rcl.2009.05.003. PMID 19744597.
- ↑ Mayr M, Burkhalter F, Bongartz G (December 2009). "Nephrogenic systemic fibrosis: clinical spectrum of disease". Journal of Magnetic Resonance Imaging. 30 (6): 1289–97. doi:10.1002/jmri.21975. PMID 19937929.
- ↑ 4.0 4.1 Grobner T (April 2006). "Gadolinium--a specific trigger for the development of nephrogenic fibrosing dermopathy and nephrogenic systemic fibrosis?". Nephrology, Dialysis, Transplantation. 21 (4): 1104–8. doi:10.1093/ndt/gfk062. PMID 16431890.
- ↑ 5.0 5.1 5.2 Schieda N, Blaichman JI, Costa AF, Glikstein R, Hurrell C, James M, Jabehdar Maralani P, Shabana W, Tang A, Tsampalieros A, van der Pol CB, Hiremath S (2018). "Gadolinium-Based Contrast Agents in Kidney Disease: A Comprehensive Review and Clinical Practice Guideline Issued by the Canadian Association of Radiologists". Canadian Journal of Kidney Health and Disease. 5: 2054358118778573. doi:10.1177/2054358118778573. PMC 6024496. PMID 29977584.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 Igreja AC, Mesquita K, Cowper SE, Costa IM (2012). "Nephrogenic systemic fibrosis: concepts and perspectives". Anais Brasileiros de Dermatologia. 87 (4): 597–607. doi:10.1590/S0365-05962012000400013. PMID 22892775.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 Daftari Besheli L, Aran S, Shaqdan K, Kay J, Abujudeh H (July 2014). "Current status of nephrogenic systemic fibrosis". Clinical Radiology. 69 (7): 661–8. doi:10.1016/j.crad.2014.01.003. PMID 24582176.
- ↑ 8.0 8.1 8.2 8.3 8.4 Bernstein EJ, Schmidt-Lauber C, Kay J (August 2012). "Nephrogenic systemic fibrosis: a systemic fibrosing disease resulting from gadolinium exposure". Best Practice & Research. Clinical Rheumatology. 26 (4): 489–503. doi:10.1016/j.berh.2012.07.008. PMID 23040363.
- ↑ Haneder S, Kucharczyk W, Schoenberg SO, Michaely HJ (February 2015). "Safety of magnetic resonance contrast media: a review with special focus on nephrogenic systemic fibrosis". Topics in Magnetic Resonance Imaging. 24 (1): 57–65. doi:10.1097/RMR.0b013e3182a14e79. PMID 25654421. S2CID 27945913.
- ↑ Kucher C, Steere J, Elenitsas R, Siegel DL, Xu X (February 2006). "Nephrogenic fibrosing dermopathy/nephrogenic systemic fibrosis with diaphragmatic involvement in a patient with respiratory failure". Journal of the American Academy of Dermatology. 54 (2 Suppl): S31–4. doi:10.1016/j.jaad.2005.04.024. PMID 16427988.
- ↑ Krous HF, Breisch E, Chadwick AE, Pinckney L, Malicki DM, Benador N (2007). "Nephrogenic systemic fibrosis with multiorgan involvement in a teenage male after lymphoma, Ewing's sarcoma, end-stage renal disease, and hemodialysis". Pediatric and Developmental Pathology. 10 (5): 395–402. doi:10.2350/06-05-0093.1. PMID 17929984. S2CID 32160877.
- ↑ 12.0 12.1 12.2 12.3 12.4 Wagner B, Drel V, Gorin Y (July 2016). "Pathophysiology of gadolinium-associated systemic fibrosis". American Journal of Physiology. Renal Physiology. 311 (1): F1–F11. doi:10.1152/ajprenal.00166.2016. PMC 4967166. PMID 27147669.
- ↑ Kalb RE, Helm TN, Sperry H, Thakral C, Abraham JL, Kanal E (March 2008). "Gadolinium-induced nephrogenic systemic fibrosis in a patient with an acute and transient kidney injury". The British Journal of Dermatology. 158 (3): 607–10. doi:10.1111/j.1365-2133.2007.08369.x. PMID 18076707.
- ↑ Bhaskaran A, Kashyap P, Kelly B, Ghera P (January 2010). "Nephrogenic systemic fibrosis following acute kidney injury and exposure to gadolinium". Indian Journal of Medical Sciences. 64 (1): 33–6. doi:10.4103/0019-5359.92485. PMID 22301807.
- ↑ 15.0 15.1 15.2 Fraum TJ, Ludwig DR, Bashir MR, Fowler KJ (August 2017). "Gadolinium-based contrast agents: A comprehensive risk assessment". Journal of Magnetic Resonance Imaging. 46 (2): 338–353. doi:10.1002/jmri.25625. PMID 28083913. S2CID 28114440.
- ↑ 16.0 16.1 Cacheris WP, Quay SC, Rocklage SM (1990). "The relationship between thermodynamics and the toxicity of gadolinium complexes". Magnetic Resonance Imaging. 8 (4): 467–81. doi:10.1016/0730-725X(90)90055-7. PMID 2118207.
- ↑ Scheinfeld NS, Cowper S, Kovarik CL, Butler DF (2019-02-02). "Nephrogenic Systemic Fibrosis". Emedicine. Archived from the original on 2008-10-19. Retrieved 2021-01-01.
- ↑ Bhawan J, Perez-Chua TA, Goldberg L (September 2013). "Sclerotic bodies beyond nephrogenic systemic fibrosis". Journal of Cutaneous Pathology. 40 (9): 812–7. doi:10.1111/cup.12187. PMID 23808625.
- ↑ Bhawan J, Swick BL, Koff AB, Stone MS (May 2009). "Sclerotic bodies in nephrogenic systemic fibrosis: a new histopathologic finding". Journal of Cutaneous Pathology. 36 (5): 548–52. doi:10.1111/j.1600-0560.2008.01111.x. PMID 19476523.
- ↑ Wiedemeyer K, Kutzner H, Abraham JL, Thakral C, Carlson JA, Tran TA, Hausser I, Hartschuh W (October 2009). "The evolution of osseous metaplasia in localized cutaneous nephrogenic systemic fibrosis: a case report". The American Journal of Dermatopathology. 31 (7): 674–81. doi:10.1097/dad.0b013e3181a1fb55. PMID 19633532. S2CID 5483217.
- ↑ Cowper SE (November 2003). "Nephrogenic fibrosing dermopathy: the first 6 years". Current Opinion in Rheumatology. 15 (6): 785–90. doi:10.1097/00002281-200311000-00017. PMID 14569211. S2CID 11768872.
- ↑ Cowper SE, Robin HS, Steinberg SM, Su LD, Gupta S, LeBoit PE (September 2000). "Scleromyxoedema-like cutaneous diseases in renal-dialysis patients". Lancet. 356 (9234): 1000–1. doi:10.1016/S0140-6736(00)02694-5. PMID 11041404. S2CID 8746227.
- ↑ Marckmann P, Skov L, Rossen K, Dupont A, Damholt MB, Heaf JG, Thomsen HS (September 2006). "Nephrogenic systemic fibrosis: suspected causative role of gadodiamide used for contrast-enhanced magnetic resonance imaging". Journal of the American Society of Nephrology. 17 (9): 2359–62. doi:10.1681/ASN.2006060601. PMID 16885403.
- ↑ Centers for Disease Control and Prevention (CDC) (February 2007). "Nephrogenic fibrosing dermopathy associated with exposure to gadolinium-containing contrast agents--St. Louis, Missouri, 2002-2006". MMWR. Morbidity and Mortality Weekly Report. 56 (7): 137–41. PMID 17318112.
- ↑ "Nyhedsavisen: Medicinalfirma fortiede at stof var farligt". Archived from the original on 2011-07-22. Retrieved 2010-11-05.
- ↑ "Gadolinium-containing contrast agents". 2018-09-17. Archived from the original on 2018-08-01. Retrieved 2022-03-14.
- ↑ "Gadolinium-containing contrast agents: Removal of Omniscan and iv Magnevist, restrictions to the use of other linear agents". Archived from the original on 2020-11-09. Retrieved 2021-01-01.
Further reading
- Cheong BY, Muthupillai R (2010). "Nephrogenic systemic fibrosis: a concise review for cardiologists". Texas Heart Institute Journal. 37 (5): 508–15. PMC 2953218. PMID 20978560.
External links
| Classification |
|---|