Murine typhus
| Murine typhus | |
|---|---|
| Other names: Endemic typhus, flea-borne typhus | |
 | |
| Chest X-ray of a 40 yr old with acute respiratory distress syndrome as a complication of murine typhus | |
| Specialty | Infectious disease |
| Symptoms | Fever, muscle pain, nausea, vomiting, rash[1] |
| Complications | Bronchiolitis, pneumonia, meningitis, septic shock[2][3] |
| Causes | Rickettsia typhi[1] |
| Diagnostic method | Blood test[1] PCR, biopsy[4] |
| Differential diagnosis | Epidemic typhus, scrub typhus, rickettsialpox, African tick typhus[5] |
| Prevention | Insect repellent[6][7] |
| Treatment | Doxycycline[1] |
| Frequency | Fewer than 100 cases reported in US annually.[8][9] |
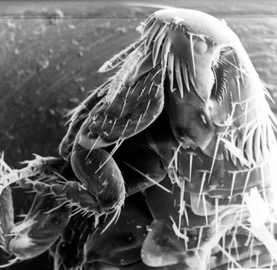
Murine typhus, also known as endemic typhus or flea-borne typhus, is a form of typhus spread by fleas (Xenopsylla cheopis), usually on rats, in contrast to epidemic typhus which is usually spread by lice.[1][10][11]
It is often under-recognized, confused with viral illnesses. Most people who are infected do not realize that they have been bitten by fleas.[5]
The historically term "hunger-typhus" was used by British POWs in Germany at the end of World War I when they described conditions in Germany.[12]
Signs and symptoms
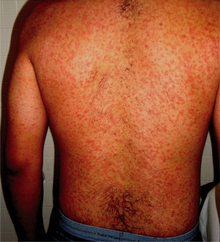
Symptoms may resemble those of measles, rubella, or possibly Rocky Mountain spotted fever. These symptoms are likely caused by a vasculitis caused by the rickettsia.Symptoms of endemic typhus include the following:[1][12][13]
- Headache
- Fever
- Muscle pain
- Joint pain
- Nausea
- Vomiting
- Rash (40–50% - six days after onset of signs)
- Neurological signs (45%)
- Confusion
- Stupor
- Seizures
Complications
Among possible complications of Murine typhus we find the following:[2][3]
Causes
It is caused by the bacterium Rickettsia typhi, and is transmitted by the fleas that infest rats. While rat fleas are the most common vectors, cat fleas and mouse fleas are less common modes of transmission. These fleas are not affected by the infection. Human infection occurs because of flea-fecal contamination of the bites on human skin. Rats, cats, maintain the rickettsia colonization by providing it with a host for its entire life cycle. Rats can develop the infection, and spread the infection to other fleas that infect them, and help multiply the number of infected fleas that can then infect humans.[14][15][16]
Less often, endemic typhus is caused by Rickettsia felis and transmitted by fleas carried by opossums.[4]
-
Rattus norvegicus
-
Rickettsia typhi bacteria
-
Common flea can carry Rickettsia felis bacteria
Mechanism

In terms of the mechanism of Murine typhus we find that it shares the same pathophysiology as epidemic typhus(but milder).[18]
Rickettsia enter endothelial cells of blood vessels, and then begin to spread and cause endothelial cellular expansion which results in multiorgan vasculitis. [18]
The aforementioned process can cause thrombosis, and small nodules due to, leukocytes, macrophages . Gangrene may occur due to thrombosis which ultimately affects extremities, nose, ear lobes, because of blood supply issues. This vasculitic process may in the end result in organ failure[18]
Diagnosis
As of 2014[update], early diagnosis continued to be based on clinical suspicion, and treatment of the disease is indicated even before laboratory results confirm its presence. Because of the lag between the onset of infection and the appearance of antibodies in a blood test, serologic tests are merely confirmatory and retrospective. [19][20]
Weil-Felix agglutination reactions are not sensitive to the disease. Indirect fluorescence antibody assays that are specific to R. typhi antigens are the recommended route for detection and diagnosis: diagnostic titers are present in half of all cases within the first week of infection and in nearly all cases by day-15. The sharing of antigens by rickettsiae means routine serologic evaluation will not distinguish between murine typhus and epidemic typhus. Bacterial cultures are rarely performed because although they are highly accurate for diagnosis, the biohazard risk of generating them is often considered too high.[19][20]
Differential diagnosis
The DDx for Murine typhus is as follows:[5]
- Rocky Mountain spotted fever
- Epidemic typhus
- Scrub typhus
- Rickettsialpox
- African tick typhus
Treatment

The disease can be fatal if left untreated, but endemic typhus is highly treatable with antibiotics.[1] [21]
Most people recover fully, but death may occur in the elderly, severely disabled or patients with a depressed immune system.[1] [21]
The most effective antibiotics include tetracycline and chloramphenicol, in United States, CDC recommends doxycycline.[1][21]
Epidemiology
Historically, thousands of murine typhus cases were reported in the United States every year;[22][8] however, the disease experienced a sudden decline in incidence in the 1940s with the implementation of pest control programs to remove the flea and rodent reservoirs responsible for rickettsial transmission in urban dwellings.[22][9] Murine typhus infections in the present are more sporadic and infrequent, with fewer than 100 cases reported in the US annually.[8][9] Nevertheless, R. typhi is still regarded as a bacterium of considerable public health significance, and outbreaks are commonly reported in the Southern US, Southern Europe, Asia, Africa, and Australia.[22][8] It is estimated that R. typhi prevalence is actually higher than the measured value, since murine typhus is often underreported and misdiagnosed because of its non-specific and mild clinical presentation.[8][23] Undiagnosed infections are predicted to outnumber reported cases by 4:1.[9] A recent study presented a clinical case of a patient that works in the Brazilian Amazon and presented an unspecific febrile illness probably caused by Rickettsia typhi since the patient presented specific antibodies to this bacteria. This shows that the R. typhi, geographical distribution can be wider than expected.[24]
In the United States of America, murine typhus is found most commonly in southern California,[25] Texas and Hawaii. In some studies, up to 13% of children were found to have serological evidence of infection.[26]
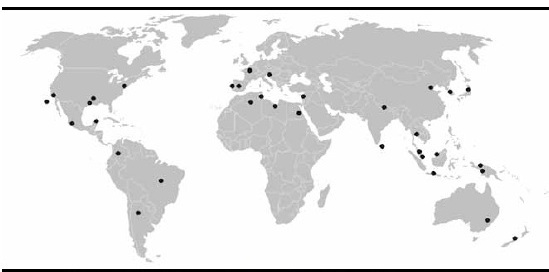
-
Worldwide distribution of R. typhi in the XXI century
-
Southern california
See also
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 "Flea-borne (murine) typhus | CDC". Centers for Disease Control and Prevention. 13 November 2020. Archived from the original on 26 March 2017. Retrieved 19 July 2023.
- ↑ 2.0 2.1 Afzal, Zeeshan; Kallumadanda, Sunand; Wang, Feng; Hemmige, Vagish; Musher, Daniel (August 2017). "Acute Febrile Illness and Complications Due to Murine Typhus, Texas, USA1,2". Emerging Infectious Diseases. 23 (8): 1268–1273. doi:10.3201/eid2308.161861. ISSN 1080-6059. PMC 5547806. PMID 28726607.
- ↑ 3.0 3.1 Moraru, Gail Miriam; II, Jerome Goddard (4 March 2019). The Goddard Guide to Arthropods of Medical Importance. CRC Press. ISBN 978-1-351-63014-6. Archived from the original on 24 July 2023. Retrieved 23 July 2023.Google books offers no page number
- ↑ 4.0 4.1 "Murine (Endemic) Typhus - Infectious Diseases". Merck Manuals Professional Edition. Archived from the original on 3 June 2023. Retrieved 19 July 2023.
- ↑ 5.0 5.1 5.2 "Overview of Rickettsial and Related Infections - Infectious Diseases". MSD Manual Professional Edition. Archived from the original on 10 May 2023. Retrieved 25 July 2023.
- ↑ "Rickettsial Diseases | CDC Yellow Book 2024". wwwnc.cdc.gov. Archived from the original on 6 June 2023. Retrieved 28 July 2023.
- ↑ US EPA, OCSPP (9 July 2013). "Repellents: Protection against Mosquitoes, Ticks and Other Arthropods". www.epa.gov. Archived from the original on 10 July 2023. Retrieved 19 July 2023.
- ↑ 8.0 8.1 8.2 8.3 8.4 Whiteford, Sarah F.; Taylor, Jeffery P.; Dumler, J. Stephen (1 March 2001). "Clinical, Laboratory, and Epidemiologic Features of Murine Typhus in 97 Texas Children". Archives of Pediatrics & Adolescent Medicine. 155 (3): 396–400. doi:10.1001/archpedi.155.3.396. ISSN 1072-4710. PMID 11231808. Archived from the original on 17 June 2022. Retrieved 20 July 2023.
- ↑ 9.0 9.1 9.2 9.3 Azad, A F (January 1990). "Epidemiology of Murine Typhus". Annual Review of Entomology. 35 (1): 553–570. doi:10.1146/annurev.en.35.010190.003005. ISSN 0066-4170. PMID 2105686. Archived from the original on 17 June 2022. Retrieved 20 July 2023.
- ↑ Li, Li; Li, Guiying (2015), Li, Hongjun (ed.), "Epidemic and Endemic Typhus", Radiology of Infectious Diseases: Volume 2, Dordrecht: Springer Netherlands, pp. 89–94, doi:10.1007/978-94-017-9876-1_8, ISBN 978-94-017-9876-1, archived from the original on 2021-10-18, retrieved 2021-02-27
- ↑ "Epidemic typhus". Centers for Disease Control and Prevention. 2020-11-13. Archived from the original on 2017-03-26. Retrieved 2021-02-27.
- ↑ 12.0 12.1 Tsioutis, Constantinos; Zafeiri, Maria; Avramopoulos, Asimakis; Prousali, Efthymia; Miligkos, Michael; Karageorgos, Spyridon A. (February 2017). "Clinical and laboratory characteristics, epidemiology, and outcomes of murine typhus: A systematic review". Acta Tropica. 166: 16–24. doi:10.1016/j.actatropica.2016.10.018. ISSN 1873-6254. PMID 27983969. Archived from the original on 25 July 2023. Retrieved 24 July 2023.
- ↑ Doppler, Johannes F.; Newton, Paul N. (14 September 2020). "A systematic review of the untreated mortality of murine typhus". PLOS Neglected Tropical Diseases. 14 (9): e0008641. doi:10.1371/journal.pntd.0008641. ISSN 1935-2735. Archived from the original on 17 June 2022. Retrieved 2 August 2023.
- ↑ Snowden, Jessica; Ladd, Megan; King, Kevin C. (2023). "Rickettsial Infection". StatPearls. StatPearls Publishing. PMID 28613765. Archived from the original on 2023-07-24. Retrieved 2023-07-22.
- ↑ McLeod, MP; Qin, X; Karpathy, SE; Gioia, J; Highlander, SK; Fox, GE; McNeill, TZ; Jiang, H; Muzny, D; Jacob, LS; Hawes, AC; Sodergren, E; Gill, R; Hume, J; Morgan, M; Fan, G; Amin, AG; Gibbs, RA; Hong, C; Yu, XJ; Walker, DH; Weinstock, GM (September 2004). "Complete genome sequence of Rickettsia typhi and comparison with sequences of other rickettsiae". Journal of bacteriology. 186 (17): 5842–55. doi:10.1128/JB.186.17.5842-5855.2004. PMID 15317790. Retrieved 30 July 2023.
- ↑ "Concept 48283". pubchem.ncbi.nlm.nih.gov. Archived from the original on 2 August 2023. Retrieved 31 July 2023.
- ↑ Osterloh, Anke (1 December 2017). "Immune response against rickettsiae: lessons from murine infection models". Medical Microbiology and Immunology. 206 (6): 403–417. doi:10.1007/s00430-017-0514-1. ISSN 1432-1831. Retrieved 25 July 2023.
- ↑ 18.0 18.1 18.2 "Typhus: Background, Pathophysiology, Epidemiology". Medscape. 12 July 2023. Archived from the original on 29 May 2023. Retrieved 21 July 2023.
- ↑ 19.0 19.1 John E. Bennett; Raphael Dolin; Martin J. Blaser (2014-09-02). Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases E-Book. Elsevier Health Sciences. p. 2223. ISBN 978-0-323-26373-3. Archived from the original on 2021-10-18. Retrieved 2021-05-30.
- ↑ 20.0 20.1 Peniche Lara, G; Dzul-Rosado, KR; Zavala Velázquez, JE; Zavala-Castro, J (April 2012). "Murine Typhus: Clinical and epidemiological aspects". Colombia medica (Cali, Colombia). 43 (2): 175–80. PMID 24893060. Archived from the original on 8 April 2023. Retrieved 25 July 2023.
- ↑ 21.0 21.1 21.2 "Typhus Treatment & Management: Medical Care, Activity, Prevention". Medscape. 12 July 2023. Archived from the original on 31 January 2023. Retrieved 26 July 2023.
- ↑ 22.0 22.1 22.2 Eremeeva, Marina E.; Dasch, Gregory A. (1 January 2012). "179 - Other Rickettsia Species". Principles and Practice of Pediatric Infectious Diseases (Fourth ed.). Elsevier. pp. 930–938.e4. ISBN 978-1-4377-2702-9.
- ↑ Schriefer, M E; Sacci, J B; Dumler, J S; Bullen, M G; Azad, A F (April 1994). "Identification of a novel rickettsial infection in a patient diagnosed with murine typhus". Journal of Clinical Microbiology. 32 (4): 949–954. doi:10.1128/jcm.32.4.949-954.1994. PMC 267160. PMID 8027348.
- ↑ Minervino, Antonio H.H.; Labruna, Marcelo B.; Dias, Salatiel R.; Costa, Francisco B.; Martins, Thiago F.; da Silva, Phablo N.S.; Faccini-Martínez, Álvaro A. (September 2020). "Typhus Group Rickettsiosis, Brazilian Amazon". Emerging Infectious Diseases. 26 (9): 2294–2296. doi:10.3201/eid2609.201305. ISSN 1080-6040. PMC 7454102. PMID 32818424. Archived from the original on 2023-07-21. Retrieved 2023-07-20.
- ↑ "Murine (endemic) Typhus" (PDF). California Department of Public Health. Archived from the original (PDF) on 4 February 2012. Retrieved 30 May 2012.
- ↑ The Pediatric Infectious Disease Journal (Impact Factor: 3.57). 07/2000; 19(6):535−8.
External links
| Classification | |
|---|---|
| External resources |