Monoarthritis
| Monoarthritis | |
|---|---|
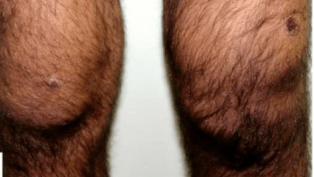 | |
| Left knee monoarthritis. | |
Monoarthritis (or Monoarticular Arthritis[1]) is inflammation (arthritis) of one joint at a time. It is usually caused by trauma, infection, or crystalline arthritis.
Signs and symptoms

The clinical presentation of Monoarthritis is consistent with:[2]
- Joint pain
- Warm skin over the joint
- Stiffness
Causes
Septic arthritis
Septic arthritis is due to a bacterial infection to the joint. It requires urgent joint washout in the operating room followed by intravenous antibiotic therapy for large joints. Small joints or children can be treated with repeated aspirations and intravenous antibiotics.
Gout
In gout, the acute inflammatory arthritis is caused by excess uric acid caused by either overproduction or under-excretion. Before the age of menopause, women have a lower incidence than males, but the rates are equal above this age. Gout can cause mono- or polyarthritis, but usually results in monoarthritis first.
Pseudogout
When monoarthritis is caused by pseudogout (calcium pyrophosphate deposition disease, CPPD), the inflammation usually lasts days to weeks, and involves the knees in half of all attacks. Like gout, attacks can occur spontaneously or with physical trauma or metabolic stress. Patients may feel well in between pseudogout attacks, and 5% present with pseudo-rheumatoid symptoms.
Osteoarthritis
Osteoarthritis is a degenerative disease commonly involving the knees and hips. It results from erosion of the cartilage protecting the bones from rubbing together. Osteoarthritis is, in fact, a polyarthritis, but it starts initially in one joint before the involvement of other joints, hence, mimicking monoarthritis.
Psoriatic arthritis
Occurs in 5-10% of patients who have psoriasis. Classic presentation involves the DIP(distal interphalangeal joints). Morning stiffness is present. Deformity of involved joints, dactylitis and nail involvement are common. Well demarcated red plaques with silvery scaling - the classic lesions of psoriasis are seen on the dorsum of the hand.
Diagnosis
When faced with monoarthritis, one of the main decisions to make is whether to perform a joint aspirate by inserting a needle into the affected joint and removing some fluid for microscopic analysis. This decision is largely taken on inflammatory markers in blood tests (e.g. CRP), fever and the clinical picture. The main use of aspiration is to detect bacteria and neutrophil granulocytes (in septic arthritis) and crystals (crystal arthropathies).
Treatment
The management of Monoarthritis is based on the following:[2]
- Antimicrobial therapy
- Systemic steroids
- Anti-inflammatory drugs
See also
References
- ↑ Scutellari, P. N.; Orzincolo, C.; Castaldi, G.; Franceschini, F. (December 1995). "[Monoarthritis]". La Radiologia Medica. 90 (6): 689–698. ISSN 0033-8362. Archived from the original on 27 September 2022. Retrieved 22 September 2022.
- ↑ 2.0 2.1 Abraham, Sherly; Patel, Shama (2022). "Monoarticular Arthritis". StatPearls. StatPearls Publishing. Archived from the original on 11 December 2021. Retrieved 22 September 2022.
External links
| Classification |
|---|