Membranous nephropathy
| Membranous nephropathy | |
|---|---|
| Other names: Membranous glomerulonephritis[1] | |
 | |
| Micrograph of membranous nephropathy showing prominent glomerular basement membrane spikes. Jones' stain. | |
| Specialty | Nephrology |
| Symptoms | Foamy urine, swelling[1][2] |
| Complications | Kidney failure, high blood pressure, high cholesterol, blood clots[1][2] |
| Usual onset | 40 to 60 years old[2] |
| Types | Stage 1 to 4[2] |
| Causes | Unknown, lupus, hepatitis B, hepatitis C, cancer[1] |
| Diagnostic method | Confirmed by kidney biopsy[1] |
| Differential diagnosis | Membranoproliferative glomerulonephritis, diabetic nephropathy, focal segmental glomerulosclerosis, minimal change disease[2] |
| Treatment | Corticosteroids, ACE inhibitors, ARBs [1] |
| Frequency | 1 in 100,000 people per year[2] |
Membranous nephropathy, previously known as membranous glomerulonephritis, is a form of kidney disease that results in foamy urine and swelling.[1][2] Over decades kidney failure occurs in about 30%.[1] Other complications may include high blood pressure, high cholesterol and blood clots.[1][2]
In 75% of cases the cause is unknown while in the other 25% of cases it occur as a result of lupus, hepatitis B, hepatitis C, certain medications, or cancer.[1] The underlying mechanism involves the build up of IgG and complement C3 in the kidney.[1] It is a type of glomerular disease.[2] Diagnosis may be suspected based on a large amount of protein in the urine and confirmed by kidney biopsy.[1]
How to best treat the condition is unclear.[1] Corticosteroids, ACE inhibitors, or ARBs may be used.[1] Other recommended measures may include a low salt diet or blood thinners.[2] About 20% of people recover without treatment.[1] Dialysis or a kidney transplant may be required in those who developed kidney failure.[2]
Membranous nephropathy newly affects about 1 in 100,000 people per year.[2] Onset is most common between the ages of 40 and 60.[2] Males are more commonly affected than females.[2] It is the second most common cause of nephrotic syndrome in adults, after diabetic nephropathy.[1] The condition was initially described by Bell in 1946.[3]
Signs and symptoms
Some people may present as nephrotic syndrome with proteinuria, edema with or without kidney failure. Others may not have symptoms and may be picked up on screening or urinalysis as having high amounts of protein loss in the urine. A definitive diagnosis of membranous nephropathy requires a kidney biopsy.
Causes
Primary
85% of MGN cases are classified as primary membranous glomerulonephritis—that is to say, the cause of the disease is idiopathic (of unknown origin or cause). This can also be referred to as idiopathic membranous nephropathy. One study has identified antibodies to an M-type phospholipase A2 receptor in 70% (26 of 37) cases evaluated.[4] In 2014, a second autoantigen was discovered, the thrombospondin type 1 domain-containing 7A (THSD7A) system that might account for an additional 5-10% of membranous nephropathy cases.[5] Other studies have implicated neutral endopeptidase and cationic bovine serum albumin as antigens.[6]
Secondary
The remainder is secondary due to:
- autoimmune conditions (e.g., systemic lupus erythematosus[7]).
- infections (e.g., syphilis, malaria, hepatitis B, hepatitis C, HIV).[8]
- drugs (e.g., captopril, NSAIDs, penicillamine, probenecid, Bucillamine, Anti-TNF therapy, Tiopronin).[9]
- inorganic salts (e.g. gold, mercury).[10]
- tumors, frequently solid tumors of the lung and colon; hematological malignancies such as chronic lymphocytic leukemia are less common.[11]
Pathogenesis
MGN is caused by immune complex formation in the glomerulus. The immune complexes are formed by binding of antibodies to antigens in the glomerular basement membrane. The antigens may be part of the basement membrane, or deposited from elsewhere by the systemic circulation.
The immune complex serves as an activator that triggers a response from the C5b - C9 complements, which form a membrane attack complex (MAC) on the glomerular epithelial cells. This, in turn, stimulates release of proteases and oxidants by the mesangial and epithelial cells, damaging the capillary walls and causing them to become "leaky". In addition, the epithelial cells also seem to secrete an unknown mediator that reduces nephrin synthesis and distribution.
Within membranous glomerulonephritis, especially in cases caused by viral hepatitis, serum C3 levels are low.[12]
Similar to other causes of nephrotic syndrome (e.g., focal segmental glomerulosclerosis or minimal change disease), membranous nephropathy is known to predispose affected individuals to develop blood clots such as pulmonary emboli. Membranous nephropathy in particular is known to increase this risk more than other causes of nephrotic syndrome though the reason for this is not yet clear.
-
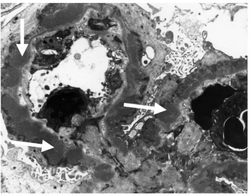
Subepithelial dense deposits and basement membrane reaction arrows
-
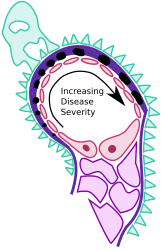
Immune complexes (black) are deposited in a thickened basement membrane creating a "spike and dome" appearance on electron microscopy.
Diagnosis
Diagnosis is by a kidney biopsy.[1] The defining point of MGN is the presence of subepithelial immunoglobulin-containing deposits along the glomerular basement membrane (GBM).
- By light microscopy, the basement membrane is observed to be diffusely thickened. Using Jones' stain, the GBM appears to have a "spiked" or "holey" appearance.
- On electron microscopy, subepithelial deposits that nestle against the glomerular basement membrane seems to be the cause of the thickening. Also, the podocytes lose their foot processes. As the disease progresses, the deposits will eventually be cleared, leaving cavities in the basement membrane. These cavities will later be filled with basement membrane-like material, and if the disease continues even further, the glomeruli will become sclerosed and finally hyalinized.
- Immunofluorescence microscopy will reveal typical granular deposition of immunoglobulins and complement along the basement membrane.[13]
Although it usually affects the entire glomerulus, it can affect parts of the glomerulus in some cases.[14]
Treatment
Treatment of secondary membranous nephropathy is guided by the treatment of the original disease. For treatment of idiopathic membranous nephropathy, the treatment options include immunosuppressive drugs and non-specific anti-proteinuric measures. Recommended first line therapy often includes: cyclophosphamide alternating with a corticosteroid.[15]
Immunosuppressants
- Corticosteroids: They have been tried with mixed results, with one study showing prevention of progression to kidney failure without improvement in proteinuria.
- Chlorambucil
- Cyclosporine[16]
- Tacrolimus
- Cyclophosphamide
- Mycophenolate mofetil
- Rituximab
Perhaps the most difficult aspect of membranous glomerulonephritis is deciding which people to treat with immunosuppressive therapy as opposed to simple "background" or anti-proteinuric therapies. A large part of this difficulty is due to a lack of ability to predict which people will progress to end-stage kidney disease, or kidney disease severe enough to require dialysis. Because the above medications carry risk, treatment should not be initiated without careful consideration as to risk/benefit profile. Of note, corticosteroids (typically Prednisone) alone are of little benefit. They should be combined with one of the other 5 medications, each of which, along with prednisone, has shown some benefit in slowing down progression of membranous nephropathy. It must be kept in mind, however, that each of the 5 medications also carry their own risks, on top of prednisone.
The twin aims of treating membranous nephropathy are first to induce a remission of the nephrotic syndrome and second to prevent the development of end-stage kidney failure. A meta-analysis of four randomized controlled trials comparing treatments of membranous nephropathy showed that regimes comprising chlorambucil or cyclophosphamide, either alone or with steroids, were more effective than symptomatic treatment or treatment with steroids alone in inducing remission of the nephrotic syndrome.
Prognosis
About a third of untreated patients have spontaneous remission, another third progress to require dialysis and the last third continue to have proteinuria, without progression of kidney failure.[citation needed]
Terminology
The closely related terms membranous nephropathy (MN)[17] and membranous glomerulopathy[18] both refer to a similar constellation but without the assumption of inflammation.
Membranous nephritis (in which inflammation is implied, but the glomerulus not explicitly mentioned) is less common, but the phrase is occasionally encountered.[19] These conditions are usually considered together.
By contrast, membranoproliferative glomerulonephritis has a similar name, but is considered a separate condition with a distinctly different causality. Membranoproliferative glomerulonephritis involves the basement membrane and mesangium, while membranous glomerulonephritis involves the basement membrane but not the mesangium. (Membranoproliferative glomerulonephritis has the alternate name "mesangiocapillary glomerulonephritis", to emphasize its mesangial character.)
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 "Glomerular Diseases | NIDDK". National Institute of Diabetes and Digestive and Kidney Diseases. Archived from the original on 28 August 2021. Retrieved 24 January 2021.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 Alok, A; Yadav, A (January 2020). "Membranous Nephropathy". PMID 32644595.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Liu, Wenbin; Gao, Chang; Dai, Haoran; Zheng, Yang; Dong, Zhaocheng; Gao, Yu; Liu, Fei; Zhang, Zihan; Liu, Zhiyuan; Liu, Weijing; Liu, Baoli; Liu, Qingquan; Shi, Jialan (6 August 2019). "Immunological Pathogenesis of Membranous Nephropathy: Focus on PLA2R1 and Its Role". Frontiers in Immunology. 10: 1809. doi:10.3389/fimmu.2019.01809.
- ↑ Beck LH, Bonegio RG, Lambeau G, Beck DM, Powell DW, Cummins TD, Klein JB, Salant DJ (July 2009). "M-type phospholipase A2 receptor as target antigen in idiopathic membranous nephropathy". The New England Journal of Medicine. 361 (1): 11–21. doi:10.1056/NEJMoa0810457. PMC 2762083. PMID 19571279.
- ↑ Tomas NM, Beck LH, Meyer-Schwesinger C, Seitz-Polski B, Ma H, Zahner G, Dolla G, Hoxha E, Helmchen U, Dabert-Gay AS, Debayle D, Merchant M, Klein J, Salant DJ, Stahl RA, Lambeau G (December 2014). "Thrombospondin type-1 domain-containing 7A in idiopathic membranous nephropathy". The New England Journal of Medicine. 371 (24): 2277–2287. doi:10.1056/NEJMoa1409354. PMC 4278759. PMID 25394321.
- ↑ Ronco P, Debiec H (February 2012). "Pathogenesis of membranous nephropathy: recent advances and future challenges". Nature Reviews. Nephrology. 8 (4): 203–13. doi:10.1038/nrneph.2012.35. PMID 22371247.
- ↑ "Renal Pathology". Archived from the original on 2007-01-22. Retrieved 2008-11-25.
- ↑ "UpToDate". www.uptodate.com. Archived from the original on 2019-12-11. Retrieved 2019-05-11.
- ↑ "UpToDate". www.uptodate.com. Archived from the original on 2019-12-11. Retrieved 2019-05-11.
- ↑ "UpToDate". www.uptodate.com. Archived from the original on 2019-12-11. Retrieved 2019-05-11.
- ↑ Ziakas PD, Giannouli S, Psimenou E, Nakopoulou L, Voulgarelis M (July 2004). "Membranous glomerulonephritis in chronic lymphocytic leukemia". American Journal of Hematology. 76 (3): 271–4. doi:10.1002/ajh.20109. PMID 15224365.
- ↑ Menon S, Valentini RP (August 2010). "Membranous nephropathy in children: clinical presentation and therapeutic approach". Pediatric Nephrology. 25 (8): 1419–28. doi:10.1007/s00467-009-1324-5. PMC 2887508. PMID 19908069.
- ↑ "Renal Pathology". Archived from the original on 2018-08-20. Retrieved 2008-11-25.
- ↑ Obana M, Nakanishi K, Sako M, Yata N, Nozu K, Tanaka R, Iijima K, Yoshikawa N (July 2006). "Segmental membranous glomerulonephritis in children: comparison with global membranous glomerulonephritis". Clinical Journal of the American Society of Nephrology. 1 (4): 723–9. doi:10.2215/CJN.01211005. PMID 17699279.
- ↑ Chen Y, Schieppati A, Chen X, Cai G, Zamora J, Giuliano GA, Braun N, Perna A (October 2014). "Immunosuppressive treatment for idiopathic membranous nephropathy in adults with nephrotic syndrome". The Cochrane Database of Systematic Reviews (10): CD004293. doi:10.1002/14651858.CD004293.pub3. PMC 6669245. PMID 25318831.
- ↑ Goumenos DS, Katopodis KP, Passadakis P, Vardaki E, Liakopoulos V, Dafnis E, Stefanidis I, Vargemezis V, Vlachojannis JG, Siamopoulos KC (2007). "Corticosteroids and ciclosporin A in idiopathic membranous nephropathy: higher remission rates of nephrotic syndrome and less adverse reactions than after traditional treatment with cytotoxic drugs". American Journal of Nephrology. 27 (3): 226–31. doi:10.1159/000101367. PMID 17389782.
- ↑ Passerini P, Ponticelli C (July 2003). "Corticosteroids, cyclophosphamide, and chlorambucil therapy of membranous nephropathy". Seminars in Nephrology. 23 (4): 355–61. doi:10.1016/S0270-9295(03)00052-4. PMID 12923723.
- ↑ Markowitz GS (May 2001). "Membranous glomerulopathy: emphasis on secondary forms and disease variants". Advances in Anatomic Pathology. 8 (3): 119–25. doi:10.1097/00125480-200105000-00001. PMID 11345236.
- ↑ Hallegua D, Wallace DJ, Metzger AL, Rinaldi RZ, Klinenberg JR (2016). "Cyclosporine for lupus membranous nephritis: experience with ten patients and review of the literature". Lupus. 9 (4): 241–51. doi:10.1191/096120300680198935. PMID 10866094.
External links
| Classification | |
|---|---|
| External resources |