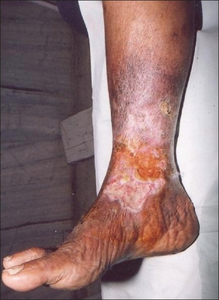
Marjolin's ulcer
| Marjolin's ulcer | |
|---|---|
 | |
| Marjolin's ulcer presenting on arm following a burn | |
Marjolin's ulcer refers to an aggressive ulcerating squamous cell carcinoma presenting in an area of previously traumatized,[1] chronically inflamed,[2] or scarred skin.[3]: 737 [4] They are commonly present in the context of chronic wounds including burn injuries, varicose veins, venous ulcers,[5] ulcers from osteomyelitis,[6] and post radiotherapy scars.
The term was named after French surgeon, Jean-Nicolas Marjolin, who first described the condition in 1828.[7] The term was later coined by J C De Costa.
Signs and symptoms
Slow growth, painlessness (as the ulcer is usually not associated with nerve tissue), and absence of lymphatic spread due to local destruction of lymphatic channels.[8]
-
Chronic venous ulcer with malignant transformation
-
Museum specimen of Marjolin's' ulcer on the sole of a foot
Histology
Histologically, the tumour is a well-differentiated squamous cell carcinoma. This carcinoma is aggressive in nature, spreads locally and is associated with a poor prognosis.[7] The cancer has a 18-38% rate of metastasis.[9] 40% occur on the lower limb and the malignant change is usually painless. This malignant change of the wound happens a long time after initial trauma, usually 10–25 years later. Its edge is everted and not always raised. More recent transcriptional analysis suggests that chronically impeded extracellular matrix turnover and epithelium-to-mesenchyme transitions in neglected scar tissue might give rise to this malignancy.[10]
Diagnosis
Wedge biopsy is the favored method of diagnosis. Tissue specimens obtained should be taken from both the centre and margin of lesion, as the central ulcerated deposits may be necrotic.
Treatment
Treatment is usually surgical, with a wide excision of the lesion; typically a 1 cm margin all around is required.
See also
References
- ↑ Esther RJ, Lamps L, Schwartz HS (1999). "Marjolin ulcers: secondary carcinomas in chronic wounds". J South Orthop Assoc. 8 (3): 181–7. PMID 12132863.
- ↑ Simmons MA, Edwards JM, Nigam A (December 2000). "Marjolin's ulcer presenting in the neck". J Laryngol Otol. 114 (12): 980–2. doi:10.1258/0022215001904545. PMID 11177375.
- ↑ Freedberg, et al. (2003). Fitzpatrick's Dermatology in General Medicine. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0.
- ↑ Phillips TJ, Salman SM, Bhawan J, Rogers GS (May 1998). "Burn scar carcinoma. Diagnosis and management". Dermatol Surg. 24 (5): 561–5. doi:10.1016/S1076-0512(98)00022-3. PMID 9598012.
- ↑ Tibbs, David J. (2013-10-22). Varicose Veins and Related Disorders. ISBN 9781483193762. Archived from the original on 2021-11-08. Retrieved 2020-12-11.
- ↑ Smidt LS, Smidt LF, Chedid MB, Bavaresco CS, Chedid MF (October 2005). "Radical surgical treatment for Marjolin ulcer occurring after chronic osteomyelitis". South. Med. J. 98 (10): 1053. doi:10.1097/01.smj.0000182509.78816.7b. PMID 16295826.
- ↑ 7.0 7.1 Chong AJ, Klein MB (March 2005). "Images in clinical medicine. Marjolin's ulcer". N. Engl. J. Med. 352 (10): e9. doi:10.1056/NEJMicm040020. PMID 15758002.
- ↑ Paredes F (February 1998). "[Marjölin ulcer]". Acta Med Port (in português). 11 (2): 185–7. PMID 9567417.
- ↑ Motley, T., White, K. and Clyde, J. (2014). Squamous cell carcinoma of the foot: A case report. The Foot and Ankle Online Journal, 7(2): 2. [1] Archived 2021-03-03 at the Wayback Machine
- ↑ Sinha S, Su S, Workentine M, Agabalyan N, Cheng M, Gabriel V, Biernaskie J (January 2017). "Transcriptional Analysis Reveals Evidence of Chronically Impeded ECM Turnover and Epithelium-to-Mesenchyme Transition in Scar Tissue Giving Rise to Marjolin's Ulcer". J Burn Care Res. 38 (1): e14–e22. doi:10.1097/BCR.0000000000000432. PMID 27679957.
External links
| Classification |
|---|