MELAS syndrome
| Mitochondrial myopathy, encephalomyopathy, lactic acidosis, and stroke-like episodes | |
|---|---|
 | |
| Basal ganglia calcification, cerebellar atrophy, increased lactate; a CT image of a person diagnosed with MELAS | |
| Frequency | 1 in 4000[1] |
Mitochondrial encephalopathy, lactic acidosis, and stroke-like episodes (MELAS) is one of the family of mitochondrial diseases, which also include MERRF syndrome, and Leber's hereditary optic neuropathy. It was first characterized under this name in 1984.[2] A feature of these diseases is that they are caused by defects in the mitochondrial genome which is inherited purely from the female parent.[3]
Signs and symptoms
MELAS is a condition that affects many of the body's systems, particularly the brain and nervous system (encephalo-) and muscles (myopathy). In most cases, the signs and symptoms of this disorder appear in childhood following a period of normal development.[4] Children with MELAS often have normal early psychomotor development until the onset of symptoms between 2 and 10 years old. Though less common, infantile onset may occur and may present as failure to thrive, growth retardation and progressive deafness. Onset in older children typically presents as recurrent attacks of a migraine-like headache, anorexia, vomiting, and seizures. Children with MELAS are also frequently found to have short stature.[1]
Most people with MELAS have a buildup of lactic acid in their bodies, a condition called lactic acidosis. Increased acidity in the blood can lead to vomiting, abdominal pain, extreme tiredness (fatigue), muscle weakness, loss of bowel control, and difficulty breathing. Less commonly, people with MELAS may experience involuntary muscle spasms (myoclonus), impaired muscle coordination (ataxia), hearing loss, heart and kidney problems, diabetes, epilepsy, and hormonal imbalances.[citation needed]
Genetics
MELAS is mostly caused by mutations in the genes in mitochondrial DNA, but it can also be caused by mutations in the nuclear DNA.[citation needed]
NADH dehydrogenase
Some of the genes (MT-ND1, MT-ND5) affected in MELAS encode proteins that are part of NADH dehydrogenase (also called complex I) in mitochondria, that helps convert oxygen and simple sugars to energy.[5]
Transfer RNAs
Other genes (MT-TH, MT-TL1, and MT-TV) encode mitochondrial specific transfer RNAs (tRNAs).[citation needed]
Mutations in MT-TL1 cause more than 80 percent of all cases of MELAS. They impair the ability of mitochondria to make proteins, use oxygen, and produce energy. Researchers have not determined how changes in mitochondrial DNA lead to the specific signs and symptoms of MELAS. They continue to investigate the effects of mitochondrial gene mutations in different tissues, particularly in the brain.[citation needed]
Inheritance
This condition is inherited in a mitochondrial pattern, which is also known as maternal inheritance and heteroplasmy. This pattern of inheritance applies to genes contained in mitochondrial DNA. Because egg cells, but not sperm cells, contribute mitochondria to the developing embryo, only females pass mitochondrial conditions to their children. Mitochondrial disorders can appear in every generation of a family and can affect both males and females, but fathers do not pass mitochondrial traits to their children. In most cases, people with MELAS inherit an altered mitochondrial gene from their mother. Less commonly, the disorder results from a new mutation in a mitochondrial gene and occurs in people with no family history of MELAS.[citation needed]
Diagnosis
MRI: Multifocal infarct-like cortical areas in different stages of ischemic evolution, areas that do not conform to any known vascular territory. Initial lesions often occur in the occipital or parietal lobes with eventual involvement of the cerebellum, cerebral cortex, basal ganglia, and thalamus.[citation needed]
Lactate levels are often elevated in serum and cerebrospinal fluid. MR spectroscopy may show an elevated lactate peak in affected and even unaffected brain areas. Muscle biopsy shows ragged red fibers. However, genetic evaluation should be done first, which eliminates the need for muscle biopsy in most cases. Diagnosis may be molecular or clinical:[citation needed]
- Stroke-like episodes before 40 years old
- Encephalopathy with seizures or dementia
- Blood lactic acidosis* or ragged red fibers on muscle biopsy
Due to mitochondrial heteroplasmy, urine and blood testing is preferable to blood alone.[1] PCR and ARMS-PCR are commonly used, reliable, rapid, and cost-effective techniques for the diagnosis of MELAS.[6]
-
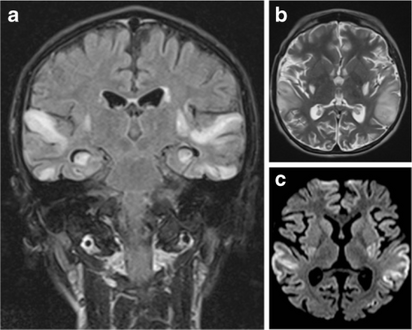
a)Symmetrical high signal intensities lesions in multiple arterial territories b)high signal cortical and subcortical lesions bilaterally in the edematous superior temporal gyri c)high signal areas in the same regions
-
Muscle biopsy of a person diagnosed with MELAS but carrying no known mutation. (a) Modified Gomori trichrome stain showing several ragged red fibers (arrowhead). (b) Cytochrome c oxidase stain showing Type-1 lightly stained and Type II fibers, darker fibers, and a few fibers with abnormal collections of mitochondria (arrowhead). Note cytochrome c oxidase negative fibers as usually seen in mitochondrial encephalopathy, lactic acidosis and stroke-like episodes (MELAS). (c) Succinate dehydrogenase staining showing a few ragged blue fibers and intense staining in the mitochondria of the blood vessels (arrow). (d) Electron microscopy showing abnormal collection of mitochondria with paracrystalline inclusions (arrowhead), osmiophilic inclusions (large arrowhead) and mitochondrial vacuoles (small arrowhead).[7]
Differential diagnosis
The presentation of some cases is similar to that of Kearns–Sayre syndrome.[8][1]
Myoclonus epilepsy associated with ragged red fibers (MERRF) may be confused with MELAS as they both involve seizures, mental deterioration, and myopathy with ragged red fibers on biopsy. MERRF patients may also have hearing loss, visual disturbance secondary to optic atrophy, and short stature. The characteristic myoclonic seizure in MERRF may help to narrow diagnosis, but genetic testing should be considered to distinguish the 2 conditions.[1]
Leigh syndrome may also present with progressive neurological deterioration, seizures, and vomiting mainly in young children.[1]
Treatment
There is no curative treatment. The disease remains progressive and fatal.[9][10]
Patients are managed according to what areas of the body are affected at a particular time. Enzymes, amino acids, antioxidants and vitamins have been used.
Also the following supplements may help:
- CoQ10 has been helpful for some MELAS patients.[11] Nicotinamide has been used because complex l accepts electrons from NADH and ultimately transfers electrons to CoQ10.
- Riboflavin has been reported to improve the function of a patient with complex l deficiency and the 3250T-C mutation.[12]
- The administration of L-arginine during the acute and interictal periods may represent a potential new therapy for this syndrome to reduce brain damage due to impairment of vasodilation in intracerebral arteries due to nitric oxide depletion.[13][14]
Epidemiology
The exact incidence of MELAS is unknown.[15] It is one of the more common conditions in a group known as mitochondrial diseases.[15] Together, mitochondrial diseases occur in about 1 in 4,000 people.[15]
See also
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Pia S, Lui F (2020). "Melas Syndrome". Statpearls. Treasure Island (FL): StatPearls Publishing. PMID 30422554. Archived from the original on 2022-04-08. Retrieved 2022-01-30.
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License Archived 2017-10-16 at the Wayback Machine.
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License Archived 2017-10-16 at the Wayback Machine.
- ↑ Pavlakis SG, Phillips PC, DiMauro S, De Vivo DC, Rowland LP (October 1984). "Mitochondrial myopathy, encephalopathy, lactic acidosis, and strokelike episodes: a distinctive clinical syndrome". Annals of Neurology. 16 (4): 481–488. doi:10.1002/ana.410160409. PMID 6093682. S2CID 41412358.
- ↑ Hirano M, Pavlakis SG (January 1994). "Mitochondrial myopathy, encephalopathy, lactic acidosis, and strokelike episodes (MELAS): current concepts". Journal of Child Neurology. 9 (1): 4–13. doi:10.1177/088307389400900102. PMID 8151079. S2CID 31329972.
- ↑ MELAS syndrome at NLM Genetics Home Reference
- ↑ Tranchant C, Anheim M (2016). "Movement disorders in mitochondrial diseases". Revue Neurologique. 172 (8–9): 524–529. doi:10.1016/j.neurol.2016.07.003. PMID 27476418.
- ↑ Bulduk BK, Kiliç HB, Bekircan-Kurt CE, Haliloğlu G, Erdem Özdamar S, Topaloğlu H, Kocaefe YÇ (March 2020). "A Novel Amplification-Refractory Mutation System-PCR Strategy to Screen MT-TL1 Pathogenic Variants in Patient Repositories". Genetic Testing and Molecular Biomarkers. 24 (3): 165–170. doi:10.1089/gtmb.2019.0079. PMID 32167396. S2CID 212693790.
- ↑ Abu-Amero KK, Al-Dhalaan H, Bohlega S, Hellani A, Taylor RW (October 2009). "A patient with typical clinical features of mitochondrial encephalopathy, lactic acidosis and stroke-like episodes (MELAS) but without an obvious genetic cause: a case report". Journal of Medical Case Reports. 3: 77. doi:10.1186/1752-1947-3-77. PMC 2783076. PMID 19946553.
- ↑ Hirano M, Ricci E, Koenigsberger MR, Defendini R, Pavlakis SG, DeVivo DC, et al. (1992). "Melas: an original case and clinical criteria for diagnosis". Neuromuscular Disorders. 2 (2): 125–135. doi:10.1016/0960-8966(92)90045-8. PMID 1422200. S2CID 45634693.
- ↑ Quinn NM, Stone G, Brett F, Caro-Dominguez P, Neylon O, Lynch B (September 2016). "MELAS (Mitochondrial Encephalomyopathy, Lactic Acidosis, Stroke) - a Diagnosis Not to be Missed". Irish Medical Journal. 109 (8): 455. PMID 28124854. Archived from the original on 2021-07-20. Retrieved 2022-01-30.
- ↑ Muñoz-Guillén N, León-López R, Ferrer-Higueras MJ, Vargas-Vaserot FJ, Dueñas-Jurado JM (August 2009). "[Arreflexic coma and MELAS syndrome]" [Arreflexic coma and MELAS syndrome]. Revista Clinica Espanola (in español). 209 (7): 337–341. doi:10.1016/s0014-2565(09)71818-1. PMID 19709537.
- ↑ Rodriguez MC, MacDonald JR, Mahoney DJ, Parise G, Beal MF, Tarnopolsky MA (February 2007). "Beneficial effects of creatine, CoQ10, and lipoic acid in mitochondrial disorders". Muscle & Nerve. 35 (2): 235–242. doi:10.1002/mus.20688. PMID 17080429. S2CID 28962906.
- ↑ Ogle RF, Christodoulou J, Fagan E, Blok RB, Kirby DM, Seller KL, et al. (January 1997). "Mitochondrial myopathy with tRNA(Leu(UUR)) mutation and complex I deficiency responsive to riboflavin". The Journal of Pediatrics. 130 (1): 138–145. doi:10.1016/S0022-3476(97)70323-8. PMID 9003864.
- ↑ Koga Y, Akita Y, Nishioka J, Yatsuga S, Povalko N, Katayama K, Matsuishi T (2007). "MELAS and L-arginine therapy". Mitochondrion. 7 (1–2): 133–139. doi:10.1016/j.mito.2006.11.006. PMID 17276739.
- ↑ Hirata K, Akita Y, Povalko N, Nishioka J, Yatsuga S, Matsuishi T, Koga Y (April 2008). "Effect of L-arginine on synaptosomal mitochondrial function". Brain & Development. 30 (4): 238–245. doi:10.1016/j.braindev.2007.08.007. PMID 17889473. S2CID 46238939.
- ↑ 15.0 15.1 15.2 "MELAS". Genetics Home Reference. December 2013. Archived from the original on 19 September 2020. Retrieved 11 April 2017.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- Webarchive template wayback links
- CS1 español-language sources (es)
- Wikipedia articles incorporating the PD-notice template
- All articles with unsourced statements
- Articles with unsourced statements from September 2021
- Articles with invalid date parameter in template
- Mitochondrial diseases
- Genodermatoses
- Syndromes
![Muscle biopsy of a person diagnosed with MELAS but carrying no known mutation. (a) Modified Gomori trichrome stain showing several ragged red fibers (arrowhead). (b) Cytochrome c oxidase stain showing Type-1 lightly stained and Type II fibers, darker fibers, and a few fibers with abnormal collections of mitochondria (arrowhead). Note cytochrome c oxidase negative fibers as usually seen in mitochondrial encephalopathy, lactic acidosis and stroke-like episodes (MELAS). (c) Succinate dehydrogenase staining showing a few ragged blue fibers and intense staining in the mitochondria of the blood vessels (arrow). (d) Electron microscopy showing abnormal collection of mitochondria with paracrystalline inclusions (arrowhead), osmiophilic inclusions (large arrowhead) and mitochondrial vacuoles (small arrowhead).[7]](https://upload.wikimedia.org/wikipedia/commons/thumb/4/44/Modified_Gomori_trichrome_stain_showing_several_ragged_red_fibers.jpg/398px-Modified_Gomori_trichrome_stain_showing_several_ragged_red_fibers.jpg)