Isotretinoin
 | |
 | |
| Names | |
|---|---|
| Pronunciation | See note at tretinoin |
| Trade names | Accutane, Roaccutane, others[1] |
| Other names | 13-cis-retinoic acid |
| |
| Clinical data | |
| Drug class | Retinoid[2] |
| Main uses | Acne[2] |
| Side effects | Inflammed lips, high blood triglycerides, joint pain, muscle pain[2] |
| Pregnancy category |
|
| Routes of use | By mouth, topical |
| External links | |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a681043 |
| Legal | |
| License data |
|
| Legal status | |
| Pharmacokinetics | |
| Bioavailability | Variable |
| Protein binding | 99.9% |
| Metabolism | Liver |
| Elimination half-life | 10–20 hours |
| Excretion | Kidney and fecal |
| Chemical and physical data | |
| Formula | C20H28O2 |
| Molar mass | 300.442 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
Isotretinoin, sold under the brand name Accutane among others, is a medication primarily used to treat severe acne.[2] Specifically it is used for acne that is nodular and has not improved with other treatments.[2] Other uses include psoriasis, ichthyosis, and certain cancers.[2] It is taken by mouth or applied to the skin.[2][3]
Common side effects include inflammed lips, high blood triglycerides, joint pain, and muscle pain.[2] Other side effects may include sexual problems, increased susceptibility to sunburn, hair loss, and mental health problems.[3] Isotretinoin is known to cause birth defects and effective birth control is required starting a month before beginning treatment.[3] It is a retinoid, meaning it is related to vitamin A and tretinoin.[2] It is believed to work via altering sebaceous gland function.[2]
It was patented in 1969 and approved for medical use in 1982.[4] While it remains avaliable under a number of generic names the original brand name was discontinued in 2009 due to a combination of low sales and multiple lawsuits over side effects.[5] In the United States and United Kingdom special programs are in place to decrease the risk of women becoming pregnant while using the medication.[2][3] In the United Kingdom 20 mg per day for a month costs the NHS about 17 pounds.[3]
Medical uses
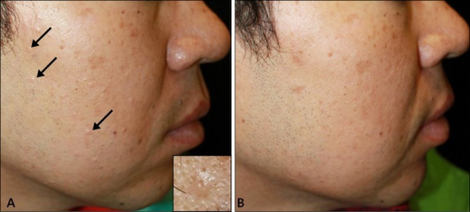
Isotretinoin is used primarily for severe cystic acne and acne that has not responded to other treatments.[6][7][8][9] Many dermatologists also support its use for treatment of lesser degrees of acne that prove resistant to other treatments, or that produce physical or psychological scarring.[10] Isotretinoin is not indicated for treatment of prepubertal acne and is not recommended in children less than 12 years of age.[11]
It is also somewhat effective for hidradenitis suppurativa and some cases of severe rosacea.[12] It can also be used to help treat harlequin ichthyosis, lamellar ichthyosis and is used in xeroderma pigmentosum cases to relieve keratoses. Isotretinoin has been used to treat the extremely rare condition fibrodysplasia ossificans progressiva. It is also used for treatment of neuroblastoma, a form of nerve cancer.
Isotretinoin therapy has furthermore proven effective against genital warts in experimental use, but is rarely used for this indication as there are more effective treatments. Isotretinoin may represent an efficacious and safe alternative systemic form of therapy for recalcitrant condylomata acuminata (RCA) of the cervix. In most countries this therapy is currently unapproved and only used if other therapies failed.[13][14]
Acne may worsen in the first few weeks of treatment but generally is better after a month to month and a half.[2]
Dosage
It is generally used at a dose of 0.5 mg per kg per day for 4 to 6 months by mouth.[3] Doses of up to 1 mg per kg may be used.[3] Doses of 20mg per day; however, appear to work as well as higher doses with less side effects.[15]
The topical form may be applied to the skin once to twice per day.[3]
Side effects
Increasingly higher dosages will result in higher toxicity, resembling vitamin A toxicity. Side effects include:[16]
|
Type of disorders |
Very common (≥ 1/10) |
Common (≥ 1/100, < 1/10) |
Rare (≥ 1/10 000,< 1/1000) |
Very rare (≤ 1/10 000) |
Unknown Frequency |
|---|---|---|---|---|---|
| Infections |
bacterial infection |
||||
| Blood and lymphatic system |
|
|
|||
| Immune system |
|
||||
| Metabolism | |||||
| Psychiatric |
|
|
|||
| Nervous system |
|
||||
| Eye |
|
|
|||
| Ear |
|
||||
| Vascular |
|
||||
| Respiratory, thoracic and mediastinal |
|
|
|||
| Gastrointestinal |
|
||||
| Hepatobiliary |
|
||||
| Skin and |
|
|
|||
| Musculo-skeletal and |
|
and tendons)
|
|||
| Kidney and urinary |
| ||||
| Reproductive system and breast disorders |
| ||||
| General |
|
||||
| Investigation[clarification needed] |
|
|
|
Prescribing restrictions
Isotretinoin is a teratogen; there is about a 20–35% risk for congenital defects in infants exposed to the drug in utero, and about 30–60% of children exposed to isotretinoin prenatally have been reported to show neurocognitive impairment.[17] Because of this, there are strict controls on prescribing isotretinoin to women who may become pregnant and women who become pregnant while taking isotretinoin are strongly advised to terminate their pregnancies.[17]
In most countries, isotretinoin can only be prescribed by dermatologists or specialist physicians; some countries also allow limited prescription by general practitioners and family doctors. In the United Kingdom[18] and Australia,[19][20] isotretinoin may be prescribed only by or under the supervision of a consultant dermatologist. Because severe cystic acne has the potential to cause permanent scarring over a short period, restrictions on its more immediate availability have proved contentious.[21] In New Zealand, isotretinoin can be prescribed by any doctor but subsidised only when prescribed by a vocationally-registered general practitioner, dermatologist or nurse practitioner.[22]
In the United States, since March 2006 the dispensing of isotretinoin is run through a website called iPLEDGE. The FDA required the companies marketing the drug in the US, which at the time that iPLEDGE was launched were Roche, Mylan, Barr, and Ranbaxy, to put this website in place as a risk evaluation and mitigation strategy. These companies formed a group called the Isotretinoin Products Manufacturing Group, and it hired Covance to run the website.[23][24] Prescribers, pharmacists, and all people to whom the drug is prescribed need to register on the site and log information into it. Women with child-bearing potential must commit to using two forms of effective contraception simultaneously for the duration of isotretinoin therapy and for a month immediately preceding and a month immediately following therapy. Additionally they must have two negative pregnancy tests 30 days apart and have negative pregnancy tests before each prescription is written.[25][26]
Possible permanent effects
Isotretinoin may stop long bone growth in young people who are still growing.[9] Premature epiphyseal closure can occur in people with acne receiving recommended doses[27] of Accutane.[28][29][30]
Generally though, premature epiphyseal closure seems to be primarily related to:
- high doses of isotretinoin beyond the recommended dose of 1mg/kg/day
- long duration beyond the usual course of what is required for an acne patient for treatment (usually 5-7 months)
- early onset of treatment (young teenage age 12-14 or younger)[31]
Isotretinoin is known to cause meibomian gland dysfunction which causes persistent keratoconjunctivitis sicca (dry eye).[32] Problems with the meibomian and salivary glands are likely due to the non-selective apoptosis of the cells of the exocrine glands.[33] Decreased night vision has been reported to persist in some people after discontinuation of isotretinoin therapy.[34]
Skin
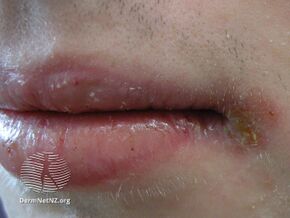
The most common side effects are mucocutaneous: dry lips, skin and nose. Other common mucocutaneous side effects are inflammation and chapping of the lips (cheilitis), redness of the skin (erythema), rashes, peeling, eczema (dermatitis), itching (pruritus) and nose bleeds (epistaxis).[35] Absence of dryness of the lips is considered an indication of non-compliance with treatment (not taking the drug as advised), as it occurs in almost all people who take it.[35]
Regular use of lip balm and moisturizer is recommended throughout a course of treatment to reduce these problems. The dose may need to be decreased to reduce the severity of these side effects.[36] The skin becomes more fragile—especially to frictional forces—and may not heal as quickly as normal. Wound healing is delayed. For this reason elective surgery, waxing of hair, tattooing, tattoo removal, piercings, dermabrasion, exfoliation, etc., are not recommended. Treatment of acne scars is generally deferred until 12 months after completion of a course of isotretinoin.
Acne usually flares up 2–3 weeks into the treatment and is usually mild and tolerable. Occasionally this flare-up is severe, necessitating oral antiobiotics such as erythromycin. A short course of oral prednisolone may be required. Some dermatologists favour a few weeks of pre-treatment with oral antibiotics before commencing isotretinoin to reduce the chance of a severe flare. A "stepped" course may also be used to reduce the chance of this initial flare, by which the initial dose is low (e.g. 0.5 mg/kg) and subsequently increased throughout the course.
Isotretinoin use can rarely lead to a more severe form of acne, acne fulminans.
Pregnancy
Isotretinoin is a teratogen highly likely to cause birth defects if taken by women during pregnancy or even a short time before conception. A few of the more common birth defects this drug can cause are hearing and visual impairment, missing or malformed earlobes, facial dysmorphism, and abnormalities in brain function. Isotretinoin is classified as FDA Pregnancy Category X and ADEC Category X, and use is contraindicated in pregnancy.[12] In the EU, isotretinoin (oral) is contraindicated in pregnancy and must not be taken by women able to have children unless the conditions of a pregnancy prevention programme are met.[37]
The manufacturer recommends pregnancy be ruled out two weeks prior to commencement of isotretinoin, and women should use two simultaneous forms of effective contraception at least one month prior to commencement, during, and for at least one month following isotretinoin therapy.[38]
In the U.S., around 2000 women became pregnant while taking the drug between 1982 and 2000, with most pregnancies ending in abortion or miscarriage. About 160 babies with birth defects were born. After the FDA put the more strict iPLEDGE program in place for the companies marketing the drug in the US, in 2011, 155 pregnancies occurred among 129,544 women of childbearing potential taking isotrentinoin (0.12%).[39]
People taking isotretinoin are not permitted to donate blood during and for at least one month after discontinuation of therapy due to its teratogenicity.[40]
Psychological
Rare psychological side effects may include depression, worsening of pre-existing depression, aggressive tendencies, irritable mood and anxiety. Very rare effects include abnormal behaviour, psychosis, suicidal ideation, suicide attempts and suicide.[8][41][42][43] In a total of 5577 adverse reactions reported to the UK's MHRA up to 31 March 2017, the plurality (1207, or 22%) concerned psychiatric effects.[44] There were 85 reports of suicidal ideation, 56 of completed suicide and 43 of suicide attempts.[44]
The association between isotretinoin use and psychopathology has been controversial. Beginning in 1983, isolated case reports emerged suggesting mood change, particularly depression, occurring during or soon after isotretinoin use.[45] A number of studies have been conducted since then of the drug's effect on depression, psychosis, suicidal thoughts and other psychological effects.[45]
Depression and suicidality
Isotretinoin is the only non-psychiatric drug on the FDA's top 10 list of drugs associated with depression[42][46] and is also within the top 10 for suicide attempts.[47] A black box warning for suicide, depression and psychosis has been present on isotretinoin's packaging in the United States since 2005.[46] In March 2018, European Medicines Agency issued a warning on a possible risk of neuropsychiatric disorders (such as depression, anxiety and mood changes) following the use of oral retinoids, including isotretinoin. [37]
In 2012, a systematic review covering all articles in the literature related to isotretinoin, depression and suicide, as well as articles related to class effect, dose response, and biologic plausibility found that the literature reviewed was consistent with an association of isotretinoin administration and depression and with suicide in a subgroup of vulnerable individuals.[41] Following this systematic review, in a 2014 review a group of Australian dermatologists and psychiatrists collaborated on a set of recommendations for safe prescribing of isotretinoin.[48] However, whether isotretinoin use is causally associated with mental illness remains controversial.[48]
Evidence for depression being causally associated with isotretinoin use includes 41 reports of positive challenge/dechallenge/rechallenge with isotretinoin, involving administering isotretinoin, withdrawing the drug and then re-administering it.[41] The majority of these cases had no psychiatric history.[41] There is also a temporal relationship between development of depression and initiation of isotretinoin treatment, with most cases developing after 1–2 months of treatment.[41] Further, higher doses of isotretinoin increases the risk of developing depression, with 25% of people showing depression on a dose of 3 mg/kg/day as compared with 3–4% at normal doses.[41] Studies have uncovered several biological processes which may credibly explain the affective changes induced by isotretinoin.
Psychosis
Isotretinoin has also been linked to psychosis.[16] Many of the side effects of isotretinoin mimic hypervitaminosis A, which has been associated with psychotic symptoms.[41] The dopamine hypothesis of schizophrenia and psychosis suggests that an increase in dopaminergic stimulation or sensitivity in the limbic system causes psychotic symptoms.[49]
It has been suggested that dysregulation of retinoid receptors by retinoids such as isotretinoin may cause schizophrenia.[50][51] The evidence for this is threefold: transcriptional activation of the dopamine D2 receptor – in addition to serotonin and glutamate receptors – is regulated by retinoic acid;[50] schizophrenia and the retinoid cascade have been linked to the same gene loci;[50] and retinoid dysfunction causes congenital anomalies identical to those observed in people with schizophrenia.[50] Further, the expression of dopamine receptors has indeed been shown to be regulated by retinoic acid.[52][53]
Musculoskeletal
Isotretinoin has a number of muscoloskeletal effects. Myalgia (muscular pain) and arthralgia (joint pain) are rare side effects.[35] Retinoids, such as high dose etretinate, are well known to cause bone changes, the most common type of which is hyperostotic changes (excessive bone growth), especially in growing children and adolescents.[35] Other problems include premature epiphyseal closure and calcification of tendons and ligaments.[35] The bones of the spine and feet are most commonly affected. Risk factors for skeletal effects include older age, greater dosage and longer course of treatment. Most bone changes cause no symptoms and may only be noticed using X-ray imaging.[35]
Gastrointestinal
Isotretinoin may cause non-specific gastrointestinal symptoms including nausea, diarrhea and abdominal pain.[35] The drug is associated with inflammatory bowel disease (IBD)—ulcerative colitis, but not Crohn's disease.[54] There are also reports of people developing irritable bowel syndrome (IBS) and worsening of existing IBS.[55]
Eyes
Isotretinoin and other retinoids are well known to affect the eyes. Dry eyes are very common during treatment and is caused by isotretinoin's apoptotic effect on the meibomian glands. Some people develop contact lens intolerance as a result.[35] In some people, these changes are long-lasting or irreversible and represent Meibomian Gland Dysfunction (MGD).[32] Other common effects on the eyes include inflammation of the eyelid (blepharitis), red eye caused by conjunctivitis and irritation of the eye. More rare ocular side effects include blurred vision, decreased night vision (which may be permanent), colour blindness, development of corneal opacities, inflammation of the cornea (keratitis), swelling of the optic disk (papilloedema, associated with IIH), photophobia and other visual disturbances.[8]
Sexual
Isotretinoin is also associated with sexual side effects, namely erectile dysfunction and reduced libido.[16] In October 2017, the UK MHRA issued a Drug Safety Update to physicians in response to reports of these problems.[56] This was in response to an EU review, published in August 2017, which states that a plausible physiological explanation of these side effects "may be a reduction in plasma testosterone".[11] The review also stated that "the product information should be updated to include ‘sexual dysfunction including erectile dysfunction and decreased libido’ as an undesirable effect with an unknown frequency".[57] There have also been reports of spermatogenesis disorders, such as oligospermia. 27 cases of sexual dysfunction report either negative dechallenge or positive dechallenge.[clarification needed][11]
Pharmacology
Mechanism of action
Isotretinoin's exact mechanism of action is unknown, but several studies have shown that isotretinoin induces apoptosis (programmatic cell death) in various cells in the body. Cell death may be instigated in the meibomian glands,[33][58] hypothalamic cells,[59] hippocampus cells[60][61] and—important for treatment of acne—in sebaceous gland cells.[62][63] Isotretinoin has a low affinity for retinoic acid receptors (RAR) and retinoid X receptors (RXR), but may be converted intracellularly to metabolites that act as agonists of RAR and RXR nuclear receptors.[7]
One study suggests the drug amplifies production of neutrophil gelatinase-associated lipocalin (NGAL) in the skin, which has been shown to reduce sebum production by inducing apoptosis in sebaceous gland cells, while exhibiting an antimicrobial effect on Cutibacterium acnes.[64][65][66] The drug decreases the size and sebum output of the sebaceous glands.[67] Isotretinoin is the only available acne drug that affects all four major pathogenic processes in acne, which distinguishes it from alternative treatments (such as antibiotics) and accounts for its efficacy in severe, nodulocystic cases.[68] The effect of Isotretinoin on sebum production can be temporary,[9] or remission of the disease can be "complete and prolonged."[67][69][70]
Isotretinoin has been speculated to down-regulate the enzyme telomerase and hTERT, inhibiting "cellular immortalization and tumorigenesis."[71] In a 2007 study, Isotretinoin was proven to inhibit the action of the metalloprotease MMP-9 (gelatinase) in sebum without any influence in the action of TIMP1 and TIMP2 (the tissue inhibitors of metalloproteases).[72] It is already known that metalloproteases play an important role in the pathogenesis of acne.[73]
CNS activities
A possible biological basis for the case reports of depression involves decreased metabolism in the orbitofrontal cortex (OFC) of the frontal lobe.[41] It has also been found that decreased OFC metabolism was correlated with headaches.[41] People reporting headache as a side effect often report comorbid neuropsychiatric symptoms, especially depression; a statistically significant relationship between headache and depression has been established.[74] It is suggested that people sensitive to isotretinoin-induced CNS effects may also be susceptible to other psychiatric side effects such as depression.[41]
Studies in mice and rats have found that retinoids, including isotretinoin, bind to dopaminergic receptors in the central nervous system.[42][75][76] Isotretinoin may affect dopaminergic neurotransmission by disrupting the structure of dopamine receptors and decreasing dopaminergic activity.[43] The dopaminergic system is implicated in numerous psychological disorders, including depression. Isotretinoin is also thought to affect the serotonergic system – it increases expression of 5-HT1A receptors in the pre-synaptic neuron, which inhibit serotonin secretion.[43] Isotretinoin also directly and indirectly increases the translation of the serotonin transporter protein (SERT), leading to increased reuptake and consequently reduced synaptic availability of serotonin.[43]
Inhibition of hippocampal neurogenesis may also play a role in the development of isotretinoin-induced depression.[41] A further effect of isotretinoin on the brain involves retinoic acid function in the hypothalamus, the hormone regulatory centre of the brain and part of the hypothalamus-pituitary-adrenal axis, a key part of the body's stress response.[41] Other brain regions regulated by retinoic acid and potentially disrupted by isotretinoin include the frontal cortex and the striatum.[41]
Pharmacokinetics and pharmacodynamics
Oral Isotretinoin is best absorbed when taken with a high-fat meal, because it has a high level of lipophilicity.[77] The efficacy of isotretinoin doubles when taken after a high-fat meal compared to when taken without food.[78] Due to Isotretinoin's molecular relationship to Vitamin A, it should not be taken with Vitamin A supplements due to the danger of toxicity through cumulative overdosing.[79] Accutane also negatively interacts with tetracycline, another class of acne drug, and with micro-dosed ('mini-pill') progesterone preparations, norethisterone/ethinylestradiol ('OrthoNovum 7/7/7'), St. John's Wort, phenytoin, and systemic corticosteroids.
Isotretinoin is primarily (99.9%) bound to plasma proteins, mostly albumin. Three metabolites of Isotretinoin are detectable in human plasma after oral administration: 4-oxo-isotretinoin, retinoid acid (tretinoin), and 4-oxo-retinoic acid (4-oxo-tretinoin). Isotretinoin also oxidizes, irreversibly, to 4-oxo-isotretinoin—which forms its geometric isomer 4-oxo-tretinoin. After an orally-administered, 80 mg dose of liquid suspension 14C-isotretinoin, 14C-activity in blood declines with a half-life of 90 hours.[77] The metabolites of isotretinoin and its conjugates are then excreted in the subject's urine and faeces in relatively equal amounts.[77] After a single, 80 mg oral dose of Isotretinoin to 74 healthy adult subjects under fed conditions, the mean ±SD elimination half-life (t1/2) of isotretinoin and 4-oxo-isotretinoin were 21.0 ± 8.2 hours and 24.0 ± 5.3 hours, respectively.[77] After both single and multiple doses, the observed accumulation ratios of isotretinoin ranged from 0.90 to 5.43 in people with cystic acne.[77]
History
The compound 13-cis retinoic acid was first studied in the 1960s at Roche Laboratories in Switzerland by Werner Bollag as a treatment for skin cancer. Experiments completed in 1971 showed that the compound was likely to be ineffective for cancer and, surprisingly, that it could be useful to treat acne. However, they also showed that the compound was likely to cause birth defects, so in light of the events around thalidomide, Roche abandoned the product. In 1975, Gary Peck and Frank Yoder independently rediscovered the drug's use as a treatment of cystic acne while studying it as a treatment for lamellar ichthyosis, and published that work. Roche resumed work on the drug. In clinical trials, subjects were carefully screened to avoid including women who were or might become pregnant. Roche's New Drug Application for isotretinoin for the treatment of acne included data showing that the drug caused birth defects in rabbits. The FDA approved the application in 1982.
Scientists involved in the clinical trials published articles warning of birth defects at the same time the drug was launched in the US, but nonetheless isotretinoin was taken up quickly and widely, both among dermatologists and general practitioners. Cases of birth defects showed up in the first year, leading the FDA to begin publishing case reports and to Roche sending warning letters to doctors and placing warning stickers on drug bottles, and including stronger warnings on the label. Lawsuits against Roche started to be filed. In 1983 the FDA's advisory committee was convened and recommended stronger measures, which the FDA took and were that time unprecedented: warning blood banks not to accept blood from people taking the drug, and adding a warning to the label advising women to start taking contraceptives a month before starting the drug. However use of the drug continued to grow, as did the number of babies born with birth defects. In 1985 the label was updated to include a boxed warning. In early 1988 the FDA called for another advisory committee, and FDA employees prepared an internal memo estimating that around 1,000 babies had been born with birth defects due to isotretinoin, that up to around 1,000 miscarriages had been caused, and that between 5,000 and 7,000 women had had abortions due to isotretinoin. The memo was leaked to the New York Times[80] a few days before the meeting, leading to a storm of media attention. In the committee meeting, dermatologists and Roche each argued to keep the drug on the market but to increase education efforts; pediatricians and the CDC argued to withdraw the drug from the market. The committee recommended to restrict physicians who could prescribe the drug and to require a second opinion before it could be prescribed. The FDA, believing it did not have authority under the law to restrict who had the right to prescribe the drug, kept the drug on the market but took further unprecedented measures: it required to Roche to make warnings yet more visible and graphic, provide doctors with informed consent forms to be used when prescribing the drug, and to conduct follow up studies to test whether the measures were reducing exposure of pregnant women to the drug. Roche implemented those measures, and offered to pay for contraception counseling and pregnancy testing for women prescribed the drug; the program was called the "Pregnancy Prevention Program".
A CDC report published in 2000[81] showed problems with the Pregnancy Prevention Program and showed that the increase in prescriptions was from off-label use, and prompted Roche to revamp its program, renaming it the "Targeted Pregnancy Prevention Program" and adding label changes like requirements for two pregnancy tests, two kinds of contraception, and for doctors to provide pharmacists with prescriptions directly; providing additional educational materials, and providing free pregnancy tests. The FDA had another advisory meeting in late 2000 that again debated how to prevent pregnant women from being exposed to the drug; dermatologists testified about the remarkable efficacy of the drug, the psychological impact of acne, and demanded autonomy to prescribe the drug; others argued that the drug be withdrawn or much stricter measures be taken. In 2001 the FDA announced a new regulatory scheme called SMART (the System to Manage Accutane Related Teratogenicity) that required Roche to provide defined training materials to doctors, and for doctors to sign and return a letter to Roche acknowledging that they had reviewed the training materials, for Roche to then send stickers to doctors, which doctors would have to place on prescriptions they give people after they have confirmed a negative pregnancy test; prescriptions could only be written for 30 days and could not be renewed, thus requiring a new pregnancy test for each prescription.[citation needed]
In February 2002, Roche's patents for isotretinoin expired, and there are now many other companies selling cheaper generic versions of the drug. On June 29, 2009, Roche Pharmaceuticals, the original creator and distributor of isotretinoin, officially discontinued both the manufacture and distribution of their Accutane brand in the United States due to what the company described as business reasons related to low market share (below 5%), coupled with the high cost of defending personal-injury lawsuits brought by some people who took the drug.[82] Generic isotretinoin will remain available in the United States through various manufacturers. Roche USA continues to defend Accutane and claims to have treated over 13 million people since its introduction in 1982. F. Hoffmann-La Roche Ltd. apparently will continue to manufacture and distribute Roaccutane outside of the United States.[83]
Among others, actor James Marshall sued Roche over allegedly Accutane-related disease that resulted in removal of his colon.[84] The jury, however, decided that James Marshall had a pre-existing bowel disease.[85]
Several trials over inflammatory bowel disease claims have been held in the United States thus far, with many of them resulting in multimillion-dollar judgments against the makers of isotretinoin.[86]
Society and culture
Brands
As of 2017 isotretinoin was marketed under many brand names worldwide: A-Cnotren, Absorica, Accuran, Accutane, Accutin, Acne Free, Acnecutan, Acnegen, Acnemin, Acneone, Acneral, Acnestar, Acnetane, Acnetin A, Acnetrait, Acnetrex, Acnogen, Acnotin, Acnotren, Acretin, Actaven, Acugen, Acutret, Acutrex, Ai Si Jie, Aisoskin, Aknal, Aknefug Iso, Aknenormin, Aknesil, Aknetrent, Amnesteem, Atlacne, Atretin, Axotret, Casius, Ciscutan, Claravis, Contracné, Curacne, Curacné, Curakne, Curatane, Cuticilin, Decutan, Dercutane, Effederm, Epuris, Eudyna, Farmacne, Flexresan, Flitrion, I-Ret, Inerta, Inflader, Inotrin, Isac, Isdiben, Isoacne, Isobest, Isocural, Isoderm, Isoface, IsoGalen, Isogeril, Isolve, Isoprotil, Isoriac, Isosupra, Isosupra Lidose, Isotane, Isotina, Isotinon, Isotren, Isotret, Isotretinoin, Isotretinoina, Isotretinoína, Isotretinoine, Isotretinoïne, Isotrétinoïne, Isotretinoinum, Isotrex, Isotrin, Isotroin, Izotek, Izotziaja, Lisacne, Locatret, Mayesta, Myorisan, Neotrex, Netlook, Nimegen, Noitron, Noroseptan, Novacne, Oralne, Oraret, Oratane, Piplex, Policano, Procuta, Reducar, Retin A, Roaccutan, Roaccutane, Roacnetan, Roacta, Roacutan, Rocne, Rocta, Sotret, Stiefotrex, Tai Er Si, Teweisi, Tretin, Tretinac, Tretinex, Tretiva, Tufacne, Zenatane, Zerocutan, Zonatian ME, and Zoretanin.[1]
As of 2017 it was marketed as a topical combination drug with erythromycin under the brand names Isotrex Eritromicina, Isotrexin, and Munderm.[1]
Cost
In the United Kingdom 20 mg per day for a month costs the NHS about 17 pounds.[3]
-
Isotretinoin costs (US)
-
Isotretinoin prescriptions (US)
Research
While excessive bone growth has been raised a possible side effect, a 2006 review found little evidence for this.[87]
See also
References
- ↑ 1.0 1.1 1.2 "Isotretinoin international brands". Drugs.com. Archived from the original on 16 July 2018. Retrieved 1 June 2017.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 "Isotretinoin Monograph for Professionals". Drugs.com. Archived from the original on 13 August 2020. Retrieved 5 October 2020.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 BNF 79. London: Pharmaceutical Press. March 2020. p. 1308. ISBN 978-0857113658.
- ↑ Fischer, Jnos; Ganellin, C. Robin (2006). Analogue-based Drug Discovery. John Wiley & Sons. p. 476. ISBN 978-3-527-60749-5. Archived from the original on 2021-08-28. Retrieved 2020-09-19.
- ↑ DeNoon, Daniel J. "Acne Drug Accutane No Longer Sold". WebMD. Archived from the original on 29 September 2020. Retrieved 5 October 2020.
- ↑ Merritt B, Burkhart CN, Morrell DS (June 2009). "Use of isotretinoin for acne vulgaris". Pediatric Annals. 38 (6): 311–20. doi:10.3928/00904481-20090512-01. PMID 19588674.
- ↑ 7.0 7.1 Layton A (May 2009). "The use of isotretinoin in acne". Dermato-Endocrinology. 1 (3): 162–9. doi:10.4161/derm.1.3.9364. PMC 2835909. PMID 20436884.
- ↑ 8.0 8.1 8.2 "Roaccutane 20mg Soft Capsules - Summary of Product Characteristics". UK Electronic Medicines Compendium. 1 July 2015. Archived from the original on 29 December 2017. Retrieved 19 September 2020.
- ↑ 9.0 9.1 9.2 US Label (PDF) (Report). FDA. 22 October 2010 [January 2010]. Archived (PDF) from the original on 27 February 2017. Retrieved 1 June 2017. See FDA Index page for NDA 018662 Archived 2020-10-20 at the Wayback Machine for updates
- ↑ Strauss JS, Krowchuk DP, Leyden JJ, Lucky AW, Shalita AR, Siegfried EC, Thiboutot DM, Van Voorhees AS, Beutner KA, Sieck CK, Bhushan R (April 2007). "Guidelines of care for acne vulgaris management". Journal of the American Academy of Dermatology. 56 (4): 651–63. doi:10.1016/j.jaad.2006.08.048. PMID 17276540.
- ↑ 11.0 11.1 11.2 11.3 "Isotretinoin (oral formulations): CMDH scientific conclusions – Scientific conclusions and grounds for the variation to the terms of the Marketing Authorisation(s)" (PDF). European Medicines Agency. August 2017. Archived (PDF) from the original on 17 May 2019. Retrieved 17 May 2019.
- ↑ 12.0 12.1 Klasco RK, editor. Drugdex system, vol. 128. Greenwood Village (CO): Thomson Micromedex; 2006.[page needed]
- ↑ Georgala S, Katoulis AC, Georgala C, Bozi E, Mortakis A (June 2004). "Oral isotretinoin in the treatment of recalcitrant condylomata acuminata of the cervix: a randomised placebo controlled trial". Sexually Transmitted Infections. 80 (3): 216–8. doi:10.1136/sti.2003.006841. PMC 1744851. PMID 15170007.
- ↑ Sehgal VN, Srivastava G, Sardana K (June 2006). "Isotretinoin--unapproved indications/uses and dosage: a physician's reference". International Journal of Dermatology. 45 (6): 772–7. doi:10.1111/j.1365-4632.2006.02830.x. PMID 16796650.
- ↑ Moe, Samantha (14 March 2016). "#158 Is less more with isotretinoin and acne?". CFPCLearn. Archived from the original on 30 January 2023. Retrieved 16 June 2023.
- ↑ 16.0 16.1 16.2 "Isotretinoin 20mg capsules - - (eMC)". www.medicines.org.uk. Archived from the original on 2017-12-28. Retrieved 2017-12-27.
- ↑ 17.0 17.1 Choi JS, Koren G, Nulman I (March 2013). "Pregnancy and isotretinoin therapy". Canadian Medical Association Journal. 185 (5): 411–3. doi:10.1503/cmaj.120729. PMC 3602257. PMID 23296582.
- ↑ Joint Formulary Committee. British National Formulary (47th ed.). London: British Medical Association and Royal Pharmaceutical Society of Great Britain. ISBN 978-0-85369-584-4.[page needed]
- ↑ "Fresh call for GPs to prescribe Roaccutane". AustralianDoctor. 19 June 2012. Archived from the original on 12 April 2017. Retrieved 19 September 2020.
- ↑ Specifically, doctors who are fellows of the Australasian College of Dermatologists (FACD); cf. Pharmaceutical Services Branch, Guide to poisons and therapeutic goods legislation for medical practitioners and dentists, Sydney: NSW Department of Health; 2006.[page needed]
- ↑ James M (June 1996). "Isotretinoin for severe acne". Lancet. 347 (9017): 1749–50. doi:10.1016/S0140-6736(96)90814-4. PMID 8656912. S2CID 28756302.
- ↑ "Acne, Isotretinoin, and Depression". MEDSAFE (New Zealand Ministry of Health). June 2013 [June 2005]. Archived from the original on 22 February 2014. Retrieved 7 February 2014.
- ↑ Thiboutot, D. M.; Cockerell, C. J. (1 August 2006). "iPLEDGE: A Report from the Front Lines of Dermatologic Practice". AMA Journal of Ethics. 8 (8): 524–528. doi:10.1001/virtualmentor.2006.8.8.pfor1-0608. ISSN 1937-7010. PMID 23234692.
- ↑ Darves, Bonnie (March 9, 2006). "Dermatologists Frustrated With Problematic iPledge Program". Medscape. Archived from the original on November 28, 2020. Retrieved September 19, 2020.
- ↑ "iPledge (About iPledge)". Archived from the original on 2017-07-29. Retrieved 2020-09-19.
- ↑ "Isotretinoin (marketed as Accutane) Capsule Information". U.S. Food and Drug Administration (FDA). 2018-11-03. Archived from the original on 2019-04-23. Retrieved 2020-09-19.
- ↑ "Isotretinoin 20mg capsules - - (eMC)". www.medicines.org.uk. Archived from the original on 2017-12-28. Retrieved 2018-01-10.
- ↑ David M, Hodak E, Lowe NJ (1988). "Adverse effects of retinoids". Medical Toxicology and Adverse Drug Experience. 3 (4): 273–88. doi:10.1007/bf03259940. PMID 3054426. S2CID 12432684.
- ↑ DiGiovanna JJ (November 2001). "Isotretinoin effects on bone". Journal of the American Academy of Dermatology. 45 (5): S176-82. doi:10.1067/mjd.2001.113721. PMID 11606950.
- ↑ Ellis CN, Madison KC, Pennes DR, Martel W, Voorhees JJ (1984). "Isotretinoin therapy is associated with early skeletal radiographic changes". Journal of the American Academy of Dermatology. 10 (6): 1024–9. doi:10.1016/S0190-9622(84)80329-1. PMID 6588057.
- ↑ "Isotretinoin risks in acne treatment: Page 3 of 4". October 2014. Archived from the original on 2019-06-09. Retrieved 2020-09-19.
- ↑ 32.0 32.1 Moy A, McNamara NA, Lin MC (September 2015). "Effects of Isotretinoin on Meibomian Glands". Optometry and Vision Science. 92 (9): 925–30. doi:10.1097/OPX.0000000000000656. PMID 26154692. S2CID 205905994. Archived from the original on 2020-10-21. Retrieved 2020-09-19.
- ↑ 33.0 33.1 Lambert RW, Smith RE (March 1989). "Effects of 13-cis-retinoic acid on the hamster meibomian gland". The Journal of Investigative Dermatology. 92 (3): 321–5. doi:10.1111/1523-1747.ep12277122. PMID 2918239.
- ↑ Fraunfelder FT, Fraunfelder FW, Edwards R (September 2001). "Ocular side effects possibly associated with isotretinoin usage". American Journal of Ophthalmology. 132 (3): 299–305. doi:10.1016/S0002-9394(01)01024-8. PMID 11530040.
- ↑ 35.0 35.1 35.2 35.3 35.4 35.5 35.6 35.7 Brelsford M, Beute TC (September 2008). "Preventing and managing the side effects of isotretinoin". Seminars in Cutaneous Medicine and Surgery. 27 (3): 197–206. doi:10.1016/j.sder.2008.07.002. PMID 18786498. Archived from the original on 2019-11-17. Retrieved 2020-09-19.
- ↑ Scheinfeld N, Bangalore S (May 2006). "Facial edema induced by isotretinoin use: a case and a review of the side effects of isotretinoin". Journal of Drugs in Dermatology. 5 (5): 467–8. PMID 16703787.
- ↑ 37.0 37.1 "Updated measures for pregnancy prevention during retinoid use". European Medicines Agency. 21 June 2018. Archived from the original on 23 November 2020.
- ↑ Roche Products Pty Ltd. Roaccutane (Australian Approved Product Information). Dee Why (NSW): Roche; 2005.[page needed]
- ↑ Leyden JJ, Del Rosso JQ, Baum EW (February 2014). "The use of isotretinoin in the treatment of acne vulgaris: clinical considerations and future directions". The Journal of Clinical and Aesthetic Dermatology. 7 (2 Suppl): S3–S21. PMC 3970835. PMID 24688620.
- ↑ BNF, edition 57[page needed]
- ↑ 41.00 41.01 41.02 41.03 41.04 41.05 41.06 41.07 41.08 41.09 41.10 41.11 41.12 Bremner JD, Shearer KD, McCaffery PJ (January 2012). "Retinoic acid and affective disorders: the evidence for an association". The Journal of Clinical Psychiatry (Systematic Review). 73 (1): 37–50. doi:10.4088/JCP.10r05993. PMC 3276716. PMID 21903028.
- ↑ 42.0 42.1 42.2 Kontaxakis VP, Skourides D, Ferentinos P, Havaki-Kontaxaki BJ, Papadimitriou GN (January 2009). "Isotretinoin and psychopathology: a review". Annals of General Psychiatry. 8: 2. doi:10.1186/1744-859X-8-2. PMC 2637283. PMID 19154613.
- ↑ 43.0 43.1 43.2 43.3 Borovaya A, Olisova O, Ruzicka T, Sárdy M (September 2013). "Does isotretinoin therapy of acne cure or cause depression?". International Journal of Dermatology. 52 (9): 1040–52. doi:10.1111/ijd.12169. PMID 23962262.
- ↑ 44.0 44.1 "Interactive Drug Analysis Profile - Isotretinoin". mhra.gov.uk. Medicines & Healthcare Products Regulatory Agency. 31 March 2017. Archived from the original on 29 December 2017.
- ↑ 45.0 45.1 Goodfield MJ, Cox NH, Bowser A, McMillan JC, Millard LG, Simpson NB, Ormerod AD (June 2010). "Advice on the safe introduction and continued use of isotretinoin in acne in the U.K. 2010". The British Journal of Dermatology. 162 (6): 1172–9. doi:10.1111/j.1365-2133.2010.09836.x. PMID 21250961.
- ↑ 46.0 46.1 Ludot M, Mouchabac S, Ferreri F (June 2015). "Inter-relationships between isotretinoin treatment and psychiatric disorders: Depression, bipolar disorder, anxiety, psychosis and suicide risks". World Journal of Psychiatry. 5 (2): 222–7. doi:10.5498/wjp.v5.i2.222. PMC 4473493. PMID 26110123.
- ↑ Wysowski DK, Pitts M, Beitz J (October 2001). "An analysis of reports of depression and suicide in patients treated with isotretinoin". Journal of the American Academy of Dermatology. 45 (4): 515–9. doi:10.1067/mjd.2001.117730. PMID 11568740. Archived (PDF) from the original on 2021-08-28. Retrieved 2020-09-19.
- ↑ 48.0 48.1 Rowe C, Spelman L, Oziemski M, Ryan A, Manoharan S, Wilson P, Daubney M, Scott J (May 2014). "Isotretinoin and mental health in adolescents: Australian consensus". The Australasian Journal of Dermatology (Review). 55 (2): 162–7. doi:10.1111/ajd.12117. PMID 24283385. S2CID 29178483.
- ↑ Palha JA, Goodman AB (June 2006). "Thyroid hormones and retinoids: a possible link between genes and environment in schizophrenia" (PDF). Brain Research Reviews. 51 (1): 61–71. doi:10.1016/j.brainresrev.2005.10.001. hdl:1822/3943. PMID 16325258. S2CID 30773986. Archived (PDF) from the original on 2021-06-29. Retrieved 2020-09-19.
- ↑ 50.0 50.1 50.2 50.3 Goodman AB (March 1994). "Retinoid dysregulation as a cause of schizophrenia". The American Journal of Psychiatry. 151 (3): 452–3. doi:10.1176/ajp.151.3.452b. PMID 8109664.
- ↑ Goodman AB (May 1996). "Congenital anomalies in relatives of schizophrenic probands may indicate a retinoid pathology". Schizophrenia Research. 19 (2–3): 163–70. doi:10.1016/0920-9964(96)88523-9. PMID 8789914. S2CID 12089905.
- ↑ Goodman AB (July 2005). "Microarray results suggest altered transport and lowered synthesis of retinoic acid in schizophrenia". Molecular Psychiatry. 10 (7): 620–1. doi:10.1038/sj.mp.4001668. PMID 15838536.
- ↑ Samad TA, Krezel W, Chambon P, Borrelli E (December 1997). "Regulation of dopaminergic pathways by retinoids: activation of the D2 receptor promoter by members of the retinoic acid receptor-retinoid X receptor family". Proceedings of the National Academy of Sciences of the United States of America. 94 (26): 14349–54. Bibcode:1997PNAS...9414349S. doi:10.1073/pnas.94.26.14349. PMC 24972. PMID 9405615.
- ↑ Crockett SD, Porter CQ, Martin CF, Sandler RS, Kappelman MD (September 2010). "Isotretinoin use and the risk of inflammatory bowel disease: a case-control study". The American Journal of Gastroenterology. 105 (9): 1986–93. doi:10.1038/ajg.2010.124. PMC 3073620. PMID 20354506.
- ↑ Lowenstein EB, Lowenstein EJ (2011). "Isotretinoin systemic therapy and the shadow cast upon dermatology's downtrodden hero". Clinics in Dermatology. 29 (6): 652–61. doi:10.1016/j.clindermatol.2011.08.026. PMID 22014987.
- ↑ "Drug Safety Update – Latest advice for medicines users – October 2017" (PDF). Medicines and Healthcare products Regulatory Agency. 3 October 2017. Archived (PDF) from the original on 17 May 2019. Retrieved 17 May 2019.
- ↑ "Pharmacovigilance Risk Assessment Committee (PRAC) – Minutes for the meeting on 3–6 July 2017" (PDF). European Medicines Agency. 1 September 2017. p. 44. Archived (PDF) from the original on 17 May 2019. Retrieved 17 May 2019.
- ↑ Kremer I, Gaton DD, David M, Gaton E, Shapiro A (1994). "Toxic effects of systemic retinoids on meibomian glands". Ophthalmic Research. 26 (2): 124–8. doi:10.1159/000267402. PMID 8196934.
- ↑ Griffin JN, Pinali D, Olds K, Lu N, Appleby L, Doan L, Lane MA (November 2010). "13-Cis-retinoic acid decreases hypothalamic cell number in vitro". Neuroscience Research. 68 (3): 185–90. doi:10.1016/j.neures.2010.08.003. PMID 20708044. S2CID 207152111.
- ↑ Crandall J, Sakai Y, Zhang J, Koul O, Mineur Y, Crusio WE, McCaffery P (April 2004). "13-cis-retinoic acid suppresses hippocampal cell division and hippocampal-dependent learning in mice". Proceedings of the National Academy of Sciences of the United States of America. 101 (14): 5111–6. Bibcode:2004PNAS..101.5111C. doi:10.1073/pnas.0306336101. JSTOR 3371827. PMC 387382. PMID 15051884.
- ↑ Sakai Y, Crandall JE, Brodsky J, McCaffery P (June 2004). "13-cis Retinoic acid (accutane) suppresses hippocampal cell survival in mice". Annals of the New York Academy of Sciences. 1021 (1): 436–40. Bibcode:2004NYASA1021..436S. doi:10.1196/annals.1308.059. PMID 15251924.
- ↑ Nelson AM, Cong Z, Gilliland KL, Thiboutot DM (September 2011). "TRAIL contributes to the apoptotic effect of 13-cis retinoic acid in human sebaceous gland cells". The British Journal of Dermatology. 165 (3): 526–33. doi:10.1111/j.1365-2133.2011.10392.x. PMC 3166444. PMID 21564055.
- ↑ Nelson AM, Gilliland KL, Cong Z, Thiboutot DM (October 2006). "13-cis Retinoic acid induces apoptosis and cell cycle arrest in human SEB-1 sebocytes". The Journal of Investigative Dermatology. 126 (10): 2178–89. doi:10.1038/sj.jid.5700289. PMID 16575387.
- ↑ Wachter K (2009). "Isotretinoin's Mechanism of Action Explored". Skin & Allergy News. 40 (11): 32. doi:10.1016/S0037-6337(09)70553-4.
- ↑ Isotretinoin’s Mechanism of Action Elucidated Archived 2010-04-04 at the Wayback Machine. Medconnect (2009-08-28). Retrieved on 2010-11-13.
- ↑ Nelson AM, Zhao W, Gilliland KL, Zaenglein AL, Liu W, Thiboutot DM (April 2008). "Neutrophil gelatinase-associated lipocalin mediates 13-cis retinoic acid-induced apoptosis of human sebaceous gland cells". The Journal of Clinical Investigation. 118 (4): 1468–78. doi:10.1172/JCI33869. PMC 2262030. PMID 18317594.
- ↑ 67.0 67.1 Peck GL, Olsen TG, Yoder FW, Strauss JS, Downing DT, Pandya M, Butkus D, Arnaud-Battandier J (February 1979). "Prolonged remissions of cystic and conglobate acne with 13-cis-retinoic acid". The New England Journal of Medicine. 300 (7): 329–33. doi:10.1056/NEJM197902153000701. PMID 153472.
- ↑ Shalita A (2001). "The integral role of topical and oral retinoids in the early treatment of acne". Journal of the European Academy of Dermatology and Venereology. 15: 43–9. doi:10.1046/j.0926-9959.2001.00012.x. PMID 11843233.
- ↑ [unreliable medical source?]Farrell LN, Strauss JS, Stranieri AM (December 1980). "The treatment of severe cystic acne with 13-cis-retinoic acid. Evaluation of sebum production and the clinical response in a multiple-dose trial". Journal of the American Academy of Dermatology. 3 (6): 602–11. doi:10.1016/S0190-9622(80)80074-0. PMID 6451637.
- ↑ [unreliable medical source?]Jones H, Blanc D, Cunliffe WJ (November 1980). "13-cis retinoic acid and acne". Lancet. 2 (8203): 1048–9. doi:10.1016/S0140-6736(80)92273-4. PMID 6107678. S2CID 40877032.
- ↑ Pendino F, Flexor M, Delhommeau F, Buet D, Lanotte M, Segal-Bendirdjian E (June 2001). "Retinoids down-regulate telomerase and telomere length in a pathway distinct from leukemia cell differentiation". Proceedings of the National Academy of Sciences of the United States of America. 98 (12): 6662–7. Bibcode:2001PNAS...98.6662P. doi:10.1073/pnas.111464998. JSTOR 3055868. PMC 34517. PMID 11371621.
- ↑ Φαχαντίδης, Παναγιώτης Ε. (2007). Η επίδραση της ισοτρετινοϊνης και των αναστολέων της 5α-αναγωγάσης στις μεταλλοπρωτεάσες του συνδετικού ιστού σε ασθενείς με ακμή [The influence of isotretinoin and 5-a reductase inhibitors in metaloproteases of connective tissue in patients with ance] (in Greek). Aristotle University of Thessaloniki. Archived from the original on 2014-06-02. Retrieved 2020-09-19.
{{cite book}}: CS1 maint: unrecognized language (link)[unreliable medical source?] - ↑ Toyoda M, Nakamura M, Makino T, Kagoura M, Morohashi M (June 2002). "Sebaceous glands in acne patients express high levels of neutral endopeptidase". Experimental Dermatology. 11 (3): 241–7. doi:10.1034/j.1600-0625.2002.110307.x. PMID 12102663. S2CID 23468315.
- ↑ Wysowski DK, Swartz L (May 2005). "Relationship between headache and depression in users of isotretinoin". Archives of Dermatology. 141 (5): 640–1. doi:10.1001/archderm.141.5.640. PMID 15897395.
- ↑ Magin P, Pond D, Smith W (February 2005). "Isotretinoin, depression and suicide: a review of the evidence". The British Journal of General Practice. 55 (511): 134–8. PMC 1463189. PMID 15720936. Archived from the original on 2019-10-30. Retrieved 2020-09-19.
- ↑ Ng CH, Schweitzer I (February 2003). "The association between depression and isotretinoin use in acne". The Australian and New Zealand Journal of Psychiatry. 37 (1): 78–84. doi:10.1046/j.1440-1614.2003.01111.x. PMID 12534661. S2CID 8475675.
- ↑ 77.0 77.1 77.2 77.3 77.4 "FDA information, side effects, and uses / Accutane (isotretinoin)". U. S. Food and Drug Administration (FDA). Archived from the original on 1 February 2014. Retrieved 20 January 2014.
- ↑ "FDA information, side effects, and uses / Accutane (isotretinoin) : Table 2 Pharmacokinetic Parameters of Isotretinoin Mean (%CV), N=74". U. S. Food and Drug Administration (FDA). Archived from the original on 1 February 2014. Retrieved 20 January 2014.
- ↑ "FDA information, side effects, and uses / Accutane (isotretinoin) : Drug Interactions". U. S. Food and Drug Administration (FDA). Archived from the original on 1 February 2014. Retrieved 20 January 2014.
- ↑ Gina Kolata for the New York Times. April 22, 1988 Anti-Acne Drug Faulted in Birth Archived 2020-09-28 at the Wayback Machine
- ↑ CDC. January 21, 2000 Accutane®-Exposed Pregnancies -- California, 1999 Archived 2020-09-25 at the Wayback Machine MMWR Weekly 49(02);28-31
- ↑ Shari Roan (7 November 2009). "New study may deal final blow to acne drug Accutane". LA Times. Archived from the original on 3 December 2020. Retrieved 19 September 2020.
- ↑ "Roche Discontinues and Plans to Delist Accutane in the U.S." (Press release). Genentech. 2009-06-29. Archived from the original on 2009-11-08. Retrieved 2010-11-12.
- ↑ Feeley J (2011-03-11). "Roche Accutane Acne Drug Caused 'Tragedy' for Actor, Brian Dennehy Says". Bloomberg. Archived from the original on 2015-01-10. Retrieved 2020-09-19.
- ↑ Silverman E (2011-11-04). "It's Curtains On Actor's Accutane Lawsuit". Pharmalot. UBM Canon.
{{cite web}}: CS1 maint: url-status (link) - ↑ Voreacos D (May 30, 2007). "Roche Found Liable in First Of 400 Suits Over Accutane". The Washington Post. Bloomberg News. Archived from the original on November 6, 2012. Retrieved April 30, 2012.
- ↑ Halverstam CP, Zeichner J, Lebwohl M (2006). "Lack of significant skeletal changes after long-term, low-dose retinoid therapy: case report and review of the literature". Journal of Cutaneous Medicine and Surgery. 10 (6): 291–9. doi:10.2310/7750.2006.00065. PMID 17241599. S2CID 36785828.
External links
| Identifiers: |
|
|---|
- Drugs.com Isotretinoin Information Archived 2020-10-11 at the Wayback Machine
- DermNet treatments/isotretinoin
- Pages using duplicate arguments in template calls
- Webarchive template wayback links
- Wikipedia articles needing page number citations from May 2012
- Articles with invalid date parameter in template
- Wikipedia articles needing page number citations from October 2010
- All articles lacking reliable references
- Articles lacking reliable references from August 2013
- CS1 maint: unrecognized language
- CS1 uses Ελληνικά-language script (el)
- Articles lacking reliable references from April 2012
- CS1 maint: url-status
- Drugs with non-standard legal status
- Chemical articles with unknown parameter in Infobox drug
- Chemical articles without CAS registry number
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Chemical pages without DrugBank identifier
- Articles without KEGG source
- Articles without UNII source
- Drugs missing an ATC code
- Drugboxes which contain changes to watched fields
- Wikipedia articles needing clarification from January 2019
- Wikipedia articles needing clarification from May 2019
- All articles with unsourced statements
- Articles with unsourced statements from December 2015
- Retinoids
- Anti-acne preparations
- Cyclohexenes
- Hoffmann-La Roche brands
- Polyenes
- Enones
- RTT

