Isolated levocardia
| Levocardia | |
|---|---|
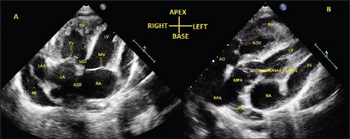 | |
| a) Transthoracic echo in apical 4-chamber view shows inverted atria b) D-transposition of great arteries | |
| Specialty | Cardiology |
Isolated levocardia (also known as situs inversus with levocardia) is a rare type of organs' situs inversus in which the heart is still in normal position but other abdominal viscera are transposed.[1][2] Isolated levocardia may occur with heart defects and patients without having operations have low life expectancy: only about 5% to 13% of patients survive more than 5 years.[3] Therefore, even though the risk of cardiac surgeries is high, once patients are diagnosed, operations are suggested to be held as soon as possible. Isolated levocardia is congenital. So far, there is not sufficient evidence to prove that chromosome abnormalities will result in isolated levocardia, and the cause of isolated levocardia is still unknown.
Symptoms and signs
Isolated levocardia patients have low exercise tolerance. They easily feel exhausted and can not finish a long distance of walk or run. In more severe cases, patients are even not able to walk 1 mile without fatigue.
Complications
There are extensive cases reporting that children and adults with isolated levocardia have complex cardiac defects,[4] and neonate or infant with isolated levocardia may be complicated by bowel obstruction and cardiac anomalies.[5] It is estimated that up to 95% of cases of isolated levocardia have associated cardiac deformities like right ventricular outflow tract (RVOT) obstruction, septal defects, inversion of cardiac chambers and transposition of cardiac chambers.[6]
Diagnosis
Systematic examination is need to be diagnosed. To determine the position of organs and major blood vessels of isolated levocardia patients, Ultrasonography, CT, and MRI are used alone and in combination:[7]
- The advantage of ultrasonography is noninvasive, and its good temporal and spatial resolution helps to evaluate cardiac valve motion in variable imaging planes. However, imaging may be interfered because of overlying bony structures, air in the lungs or bowel, wounds, or chest wall fibrosis.
- CT scanning presents a larger visual filed. Images will in high spatial resolution and the anatomic structures can be displayed in three dimensions. Thus, CT scanning is able to better demonstrate anatomic relationships and avert additional invasive studies. If the scanning times is faster in the near future, structures will be in even greater definition.
- Since magnetic resonance imaging (MRI) can provide with clear tissue contrast between vasculature and other surrounding structures, MRI technology is considered to have some benefits over ultrasound and CT scans. However, more studies are needed to confirm the diagnostic value of this technique.[8]
Through data comparison, the average value of cardiovascular malformation in levocardia patients is 4.8±1.8, and for isolated levocardia, the average value is 3.0±1.7.[9]
Through the analysis of isolated levocardia cases, some common features of isolated levocardia patients are:
- Pulmonary blood flow is inadequate
- Right ventricle is enlarged
- Pulmonary venous return to the right side of the heart
- The aorta is right-sided
Treatment
Examination
Isolated levocardia is congenital, and so far, there is no efficient way to prevent it. However, in the prenatal period, a prenatal evaluation is suggested. It is recommended to include determination of the situs, identification of heart anomalies, and detection of the major vessels and abdominal viscera in the prenatal evaluation. In the postnatal period, a detection of IVC interruption Archived 2019-11-17 at the Wayback Machine may be helpful and a prophylactic lifelong antibiotic should be prescribed for the neonate to treat the increase of incidence of overwhelming sepsis in congenital asplenia. Besides, parents should be counseled appropriately.
With accurate, thorough sonographic examination and if there is no congenital heart malformations and chromosomal aberrations, the risk of morbidity and mortality will decrease.
Operation
Main surgeries procedure includes: Blalock-Taussig, total cavopulmonary connection (Fontan procedure), Rastelli procedure. Blalock-Taussig is a traditional procedure, and Fontan procedure is widely operated recently. The goal of most isolated levocardia surgeries is to rebuild parts of the heart and "redirect" the way blood flows in order to augment pulmonary blood flow.
Cardiac surgeries have high risk. Despite the advances in the operative management, morbidity and mortality remain high. Most death after receiving operations may attribute to a combination of cardiac failure and renal insufficiency. The surgical strategy chosen – hybrid versus traditional procedures, choices regarding the most appropriate pulmonary blood flow – will affect management throughout a patient’s life. However, further studies are still required to identify determinants of the optimal surgical strategy in individual patients.[10]
Epidemiology
In general population, the incidence of isolated levocardia is 1: 22,000; in all patients with congenital heart disease, the incidence is from 0.4% to 1.2%.
Clinical cases
- A ten-year-old boy received a Blalock-Taussig operation in 1947. He was diagnosed to have isolated levocardia, a pulmonic stenosis with a ventricular septal defect and an overriding aorta. After the operation, he gradually suffered from cardiac failure and died from it.[11]
- In 1948, a 15 months old white female was considered to have isolated levocardia, tetralogy of Fallot with an auricular septal defect, a left aortic arch and a left superior vena cava. Her condition was temporary improved but she still died 6 months after the operation from gradually developed cardiac failure and anuria with uremia and convulsions.
- A Blalock-Taussig operation performed by Dr. Alfred Blalock in 1947 helped to significantly improve the condition of the patient. Before the operation, the patient was diagnosed to have isolated levocardia, pulmonary stenosis, overriding aorta with a right aortic arch and anomalous return of the pulmonary and systemic circulations. After the operation, his heart enlarged but he did not develop cardiac failure and he was even able to walk a long distance without drastic discomfort.
- A boy's exercise tolerance remarkably improved after receiving a Blalock-Taussig operation in 1947. The size of his heart did not change a lot after the operation and there was no evidence of cardiac failure.
- In 1948, a patient who had diagnosed to have situs inversus of the abdominal viscera with levocardia and tetralogy of Fallot gain weight after receiving the Blalock-Taussig operation and was able to easily finish a 1.5 miles walk.[12]
References
- ↑ MITTAL, REKHA; PATHAK, KAMAL; MANOHARAN, S (April 1994). "ISOLATED LEVOCARDIA WITH SITUS INVERSUS (A Case Report)". Medical Journal Armed Forces India. 50 (2): 151–154. doi:10.1016/S0377-1237(17)31023-7. PMC 5529679. PMID 28769192.
- ↑ Harris, Thomas R.; Rainey, Robert L. (1965-10-01). "Ideal isolated levocardia". American Heart Journal. 70 (4): 440–448. doi:10.1016/0002-8703(65)90354-6. PMID 5834189.
- ↑ Vijayakumar, V.; Brandt, T. (1991). "Prolonged survival with isolated levocardia and situs inversus". Cleveland Clinic Journal of Medicine. 58 (3): 243–247. doi:10.3949/ccjm.58.3.243. ISSN 0891-1150. PMID 1893555.
- ↑ Gindes, L.; Hegesh, J.; Barkai, G.; Jacobson, J. M.; Achiron, R. (2007). "Isolated Levocardia: Prenatal Diagnosis, Clinical Importance, and Literature Review". Journal of Ultrasound in Medicine. 26 (3): 361–5. doi:10.7863/jum.2007.26.3.361. PMID 17324986.
- ↑ Gindes, Liat; Hegesh, Julian; Barkai, Gad; Jacobson, Jeffrey M.; Achiron, Reuven (2007). "Isolated Levocardia". Journal of Ultrasound in Medicine. 26 (3): 361–365. doi:10.7863/jum.2007.26.3.361. ISSN 1550-9613. PMID 17324986.
- ↑ Winer-Muram, Helen T. (1995). "Adult Presentation of Heterotaxic Syndromes and Related Complexes". Journal of Thoracic Imaging. 10 (1): 43–57. doi:10.1097/00005382-199501010-00004. ISSN 0883-5993. PMID 7891396.
- ↑ "Isolated levocardia | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program". rarediseases.info.nih.gov. Archived from the original on 2019-10-17. Retrieved 2019-10-17.
- ↑ Vijayakumar, Vaniand, and Thomas Brandt (1991). "Prolonged survival with isolated levocardia and situs inversus". Cleveland Clinic Journal of Medicine. 58 (3): 243–247. doi:10.3949/ccjm.58.3.243. PMID 1893555.
- ↑ Hu, Jiaxin (2001). "The Diagnosis and Surgical Management of Levoversion and Isolated Levocardia". Academic Journal of Sun Yat-sen University of Medical Sciences.
- ↑ "Hypoplastic Left Heart Syndrome Surgery: The Fontan Procedure (for Parents) - KidsHealth". kidshealth.org. Archived from the original on 2021-06-16. Retrieved 2019-11-10.
- ↑ Young, Maurice D.; Griswold, Herbert E. (1951). "Situs Inversus of the Abdominal Viscera with Levocardia: Report of Eight Cases Submitted to the Blalock-Taussig Operation". Circulation. 3 (2): 202–214. doi:10.1161/01.CIR.3.2.202. ISSN 0009-7322. PMID 14812648.
- ↑ Young, Maurice D.; Griswold, Herbert E. (1951). "Situs Inversus of the Abdominal Viscera with Levocardia: Report of Eight Cases Submitted to the Blalock-Taussig Operation". Circulation. 3 (2): 202–214. doi:10.1161/01.CIR.3.2.202. ISSN 0009-7322. PMID 14812648.