Idiopathic scrotal calcinosis
| Idiopathic scrotal calcinosis | |
|---|---|
| Other names: Idiopathic calcified nodules of the scrotum[1] | |
 | |
| Specialty | Dermatology |
| Symptoms | One or more small bumps in the skin of the scrotum, may be chalky discharge[2] |
| Usual onset | Young boys and young men[2] |
Idiopathic scrotal calcinosis is a skin condition characterized by one or more small bumps in the skin of the scrotum, sometimes with chalky discharge.[2]
These bumps are calcifications of the skin resulting from the deposition of calcium and phosphorus.[3]: 528 However, the levels of calcium and phosphate in the blood are normal.[4] Idiopathic scrotal calcinosis typically affects young males, with an onset between adolescence and early adulthood.[4] The scrotal calcinosis appears, without any symptoms, as yellowish nodules that range in size from 1 mm to several centimeters.[5]
Signs and symptoms
- Single or multiple hard, marble-like nodules of varying size affecting scrotal skin.
- Nodules vary in size from a few millimeters to a few centimeters.
- Usually start to appear in childhood or early adult life
- Over time, nodules increase in number and size
- Nodules may break down and discharge chalky material
- Rarely, lesions may be polypoid
- Usually asymptomatic
Cause
The cause is not well defined.[5][6] Originally considered idiopathic condition. Now accepted that majority of cases develop from dystrophic calcification of cyst contents.
Diagnosis
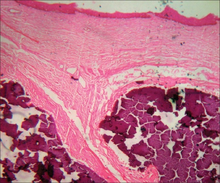
- Clinically Relevant Pathologic Features
- Lesions slowly progress throughout life
- They slowly increase in number and size
- Nodules are mobile and do not attach to underlying structures
Pathologic Interpretation Pearls
- Globular and granular purple deposits within dermis surrounded by giant cell granulomatous reaction
- Sometimes remnants of cystic lesion can be identified
- Very distinctive appearance with almost no histologic differential diagnosis.
Treatment
Treatment may involve surgery,[7] which is currently the only recommended intervention.[5] Surgery should include the removal of even small nodules, to prevent the recurrence of the scrotal calcinosis.[5]
Prognosis
- Benign condition
- Slow progression throughout life
- Lesions remain discrete and do not become confluent
Epidemiology
- Incidence: uncommon
- Age: children and young adults
History
Scrotal calcinosis was first described in 1883 by Lewinski.[5]
See also
References
- ↑ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ↑ 2.0 2.1 2.2 Johnstone, Ronald B. (2017). "14. Cutaneous deposits". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 280. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2022-09-27.
- ↑ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. ISBN 978-0-7216-2921-6.
- ↑ 4.0 4.1 Grenader, Tal; Shavit, Linda (Aug 18, 2011). "Scrotal Calcinosis". New England Journal of Medicine. 365 (7): 647. doi:10.1056/NEJMicm1013803. PMID 21848465.
- ↑ 5.0 5.1 5.2 5.3 5.4 Khallouk A, Yazami OE, Mellas S, Tazi MF, El Fassi J, Farih MH (2011). "Idiopathic scrotal calcinosis: a non-elucidated pathogenesis and its surgical treatment". Reviews in Urology. 13 (2): 95–7. PMC 3176555. PMID 21935341.
- ↑ Dubey S, Sharma R, Maheshwari V (2010). "Scrotal calcinosis: idiopathic or dystrophic?". Dermatol. Online J. 16 (2): 5. doi:10.5070/D34QV0S2PG. PMID 20178701. Archived from the original on 2013-05-02. Retrieved 2021-12-12.
- ↑ Karaca M, Taylan G, Akan M, Eker G, Gideroglu K, Gul AE (April 2010). "Idiopathic Scrotal Calcinosis: Surgical Treatment and Histopathologic Evaluation of Etiology". Urology. 76 (6): 1493–1495. doi:10.1016/j.urology.2010.02.001. PMID 20381842.