Glycogen storage disease type V
Glycogen storage disease type V (GSD5, GSD-V),[1] also known as McArdle's disease,[2] is a metabolic disorder, one of the metabolic myopathies, more specifically a muscle glycogen storage disease, caused by a deficiency of myophosphorylase.[3][4] Its incidence is reported as one in 100,000, roughly the same as glycogen storage disease type I.[2]
The disease was first reported in 1951 by Dr. Brian McArdle of Guy's Hospital, London.[5]
Signs and symptoms
Onset symptoms
The onset of this disease is usually noticed in childhood,[6][7][8] but often not diagnosed until the third or fourth decade of life, frequently due to misdiagnosis and dismissal of symptoms.[6][8] Signs and symptoms include exercise intolerance with muscle pain, premature muscle fatigue, painful cramps, inappropriate rapid heart rate response to exercise, heavy or rapid breathing, and may include myoglobin in the urine (often provoked by a bout of exercise).[2][9][10]
Heart rate during exercise is a key indicator as, unlike the symptoms of muscle fatigue and cramping, it is a medical sign (meaning that it is observable and measurable by a third party rather than felt subjectively by the patient). In regularly active individuals with McArdle disease, they may not feel the usual symptoms of muscle fatigue and cramping until they increase their speed to very brisk walking, jogging or cycling; however, they will still show an inappropriate rapid heart rate response to exercise, with a declining heart rate once second wind has been achieved.[11][12][13]
"In McArdle's, our heart rate tends to increase in what is called an 'inappropriate' response. That is, after the start of exercise it increases much more quickly than would be expected in someone unaffected by McArdle's."[10]
Myoglobinuria may be seen due to the breakdown of skeletal muscle known as rhabdomyolysis, a condition in which muscle cells breakdown, sending their contents into the bloodstream.[14] In a recent study of 269 GSD-V patients, 39.4% reported no previous episodes of myoglobinuria and 6.8% had normal CK even with fixed muscle weakness, so an absence of myoglobinuria and normal CK should not rule out the possibility of the disease.[15]
Younger people may display unusual symptoms, such as difficulty in chewing, swallowing or utilizing normal oral motor functions.[16] A number of comorbidities were found in GSD-V individuals at a higher rate than found in the general population, including (but not limited to): hypertension (17%), endocrine diseases (15.7%), muskuloskeletal/rheumatic disease (12.9%), hyperuricemia/gout (11.6%), gastrointestinal diseases (11.2%), neurological disease (10%), respiratory disease (9.5%), and coronary artery disease (8.3%).[15] They may have a pseudoathletic appearance of muscle hypertrophy, particularly of the legs, and may have lower bone mineral content and density in the legs.[17]
As skeletal muscle relies predominantly on glycogenolysis for the first few minutes as it transitions from rest to activity, as well as throughout high-intensity aerobic activity and all anaerobic activity, individuals with GSD-V experience during exercise: sinus tachycardia, tachypnea, muscle fatigue and pain, during the aforementioned activities and time frames.[9][18] They may exhibit a “second wind” phenomenon, which is characterized by the individual's better tolerance for aerobic exercise such as walking and cycling after approximately 10 minutes.[19] This is attributed to the combination of increased blood flow and the ability of the body to find alternative sources of energy, like fatty acids, proteins, and increased blood glucose uptake.[6][9] In the long term, patients may exhibit kidney failure due to the myoglobinuria, and with age, patients may exhibit progressively increasing weakness and substantial muscle loss.[citation needed]
AMP is primarily produced from the myokinase (adenylate kinase) reaction,[20] which runs when the ATP reservoir is low. The myokinase reaction is one of three reactions in the phosphagen system (ATP-PCr), with the myokinase reaction occurring after phosphocreatine (creatine phosphate) has been depleted. In McArdle disease individuals, their muscle cells produce far more AMP than non-affected individuals as the reduced glycolytic flux from impaired glycogenolysis results in a chronically low ATP reservoir during exercise.[20] The muscle cells need ATP (adenosine triphosphate) as it provides energy for muscle contraction by actively transporting calcium ions into the sarcoplasmic reticulum before muscle contraction, and it is used during muscle contraction for the release of myosin heads in the sliding filament model during the cross-bridge cycle.
Along with the myokinase reaction, AMP is also produced by the purine nucleotide cycle, which also runs when the ATP reservoir in muscle cells is low, and is a part of protein metabolism. In the purine nucleotide cycle, three nucleotides: AMP (adenosine monophosphate), IMP (inosine monophosphate), and S-AMP (adenylosuccinate) are converted in a circular fashion; the byproducts are fumarate (which goes on to produce ATP via oxidative phosphorylation), ammonia (from the conversion of AMP into IMP), and uric acid (from excess AMP). GSD-V patients may experience myogenic hyperuricemia (exercise-induced accelerated breakdown of purine nucleotides in skeletal muscle).[21][22]
To avoid health complications, GSD-V patients need to get their ATP primarily from free fatty acids (lipid metabolism) rather than protein metabolism. Over-reliance on protein metabolism can be best avoided by not depleting their ATP reservoir, such as by not pushing through the pain and by not going too fast, too soon.[10][13]
"Be wary of pushing on when you feel pain start. This pain is a result of damaging muscles, and repeated damage will cause problems in the long term. But also this is counterproductive–it will stop you from getting into second wind. By pressing on despite the pain, you start your protein metabolism which then effectively blocks your glucose and fat metabolism. If you ever get into this situation, you need to stop completely for 30 minutes or more and then start the whole process again."[13]
Patients may present at emergency rooms with a transient
contracture of the muscles and often severe pain (e.g. "clawed hand"). These require urgent assessment for rhabdomyolysis as in about 30% of cases this leads to acute kidney injury, which left untreated can be life-threatening. In a small number of cases compartment syndrome has developed, requiring prompt surgical referral.[23][24][25]
Genetics

McArdle disease (GSD-V) is inherited in an autosomal recessive manner. If both parents are carriers (not having the disease, but each parent having one copy of the mutated allele), then each child of the couple will have a 25% chance of being affected (having McArdle disease), a 50% chance of being a carrier, and a 25% chance of being unaffected (neither a carrier nor diseased).[16]
Two autosomal recessive forms of this disease occur, childhood-onset and adult-onset. The gene for myophosphorylase, PYGM (the muscle-type of the glycogen phosphorylase gene), is located on chromosome 11q13. According to the most recent publications, 95 different mutations have been reported. The forms of the mutations may vary between ethnic groups. For example, the R50X (Arg50Stop) mutation (previously referred to as R49X) is most common in North America and western Europe, and the Y84X mutation is most common among central Europeans.[citation needed]
The exact method of protein disruption has been elucidated in certain mutations. For example, R138W is known to disrupt to pyridoxal phosphate binding site.[26] In 2006, another mutation (c.13_14delCT) was discovered which may contribute to increased symptoms in addition to the common Arg50Stop mutation.[27]
Myophosphorylase
Structure
The myophosphorylase structure consists of 842 amino acids. Its molecular weight of the unprocessed precursor is 97 kDa. The three-dimensional structure has been determined for this protein. The interactions of several amino acids in myophosphorylase's structure are known. Ser-14 is modified by phosphorylase kinase during activation of the enzyme. Lys-680 is involved in binding the pyridoxal phosphate, which is the active form of vitamin B6, a cofactor required by myophosphorylase. By similarity, other sites have been estimated: Tyr-76 binds AMP, Cys-109 and Cys-143 are involved in subunit association, and Tyr-156 may be involved in allosteric control.[citation needed]
Function
Myophosphorylase is the form of the glycogen phosphorylase found in muscle that catalyses the following reaction:[28][29][30]
((1→4)-alpha-D-glucosyl) (n) + phosphate = ((1→4)-alpha-D-glucosyl) (n-1) + alpha-D-glucose 1-phosphate
Failure of this enzyme ultimately impairs the operation of ATPases. This is due to the lack of normal pH fall during exercise, which impairs the creatine kinase equilibrium and exaggerates the rise of ADP.[citation needed]
Pathophysiology
Myophosphorylase is involved in the breakdown of glycogen to glucose for use in muscle. The enzyme removes 1,4 glycosyl residues from outer branches of glycogen and adds inorganic phosphate to form glucose-1-phosphate. Ordinarily, the removal of 1,4 glycosyl residues by myophosphorylase leads to the formation of glucose-1-phosphate during glycogen breakdown and the polar, phosphorylated glucose cannot leave the cell membrane and so is marked for intracellular catabolism. In McArdle's Disease, deficiency of myophosphorylase leads to accumulation of intramuscular glycogen and a lack of glucose-1-phosphate for cellular fuel.
Myophosphorylase exists in the active form when phosphorylated. The enzyme phosphorylase kinase plays a role in phosphorylating glycogen phosphorylase to activate it and another enzyme, protein phosphatase-1, inactivates glycogen phosphorylase through dephosphorylation.
Diagnosis
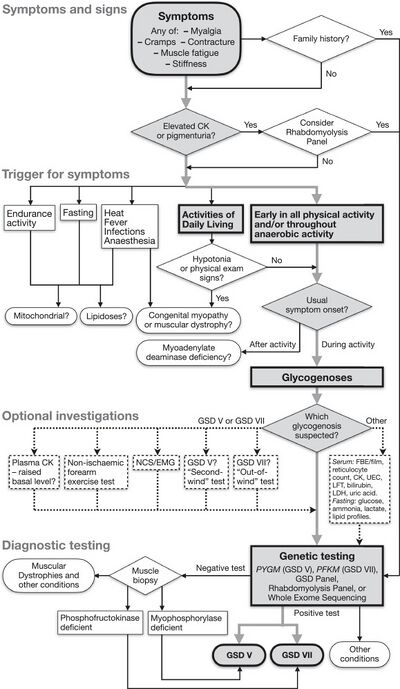
There are some laboratory tests that may aid in diagnosis of GSD-V. A muscle biopsy will note the absence of myophosphorylase in muscle fibers. In some cases, acid-Schiff stained glycogen can be seen with microscopy.[citation needed]
Genetic sequencing of the PYGM gene (which codes for the muscle isoform of glycogen phosphorylase[31][32]) may be done to determine the presence of gene mutations, determining if McArdle's is present. This type of testing is considerably less invasive than a muscle biopsy.[16]
The physician can also perform an ischemic forearm exercise test as described above. Some findings suggest a nonischemic test could be performed with similar results.[33] The nonischemic version of this test would involve not cutting off the blood flow to the exercising arm. Findings consistent with McArdle's disease would include a failure of lactate to rise in venous blood and exaggerated ammonia levels. These findings would indicate a severe muscle glycolytic block.
Serum lactate may fail to rise in part because of increased uptake via the monocarboxylate transporter (MCT1), which is upregulated in skeletal muscle in McArdle disease. Lactate may be used as a fuel source once converted to pyruvate. Ammonia levels may rise given ammonia is a by-product of the adenylate kinase pathway, an alternative pathway for ATP production. In this pathway, two ADP molecules combine to make ATP; AMP is deaminated in this process, producing inosine monophosphate (IMP) and ammonia (NH3).[34]
Physicians may also check resting levels of creatine kinase, which are moderately increased in 90% of patients.[9] In some, the level is increased by multitudes - a person without GSD-V will have a CK between 60 and 400IU/L, while a person with the syndrome may have a level of 5,000 IU/L at rest, and may increase to 35,000 IU/L or more with muscle exertion. This can help distinguish McArdle's syndrome from carnitine palmitoyltransferase II deficiency (CPT-II), a lipid-based metabolic disorder which prevents fatty acids from being transported into mitochondria for use as an energy source. Also, serum electrolytes and endocrine studies (such as thyroid function, parathyroid function and growth hormone levels) will also be completed. Urine studies are required only if rhabdomyolysis is suspected. Urine volume, urine sediment and myoglobin levels would be ascertained. If rhabdomyolysis is suspected, serum myoglobin, creatine kinase, lactate dehydrogenase, electrolytes and renal function will be checked.[citation needed]
Physicians may also conduct an exercise stress test to test for an inappropriate rapid heart rate (sinus tachycardia) in response to exercise. Due to the rare nature of the disease, the inappropriate rapid heart rate in response to exercise may be misdiagnosed as inappropriate sinus tachycardia (which is a diagnosis of exclusion). The 12 Minute Walk Test (12MWT) can be used to determine "second wind," which requires a treadmill (no incline), heart rate monitor, stop watch, pain scale, and that the patient has rested for 30 minutes prior to the test to ensure that "second wind" has stopped (that is, that increased ATP production primarily from free fatty acids has returned to resting levels).[11][35]
Differential diagnoses
Dynamic symptoms of exercise intolerance (e.g. muscle fatigue and cramping) with or without fixed proximal muscle weakness:
- Another glycogen storage disease that affects muscle (muscle GSD);
- Metabolic myopathy other than glycogen storage disease;
- Endocrine myopathy that affects carbohydrate metabolism secondary to the primary disease;
- Inadequate blood flow (ischemia), particularly of the calves
- Poor diet or malabsorption disease resulting in malnutrition of micronutrients essential for muscle glycogen metabolism.
Fixed symptom of muscle weakness, predominantly of the proximal muscles:
Treatment
Supervised exercise programs have been shown in small studies to improve exercise capacity by several measures: lowering heart rate, lowering serum creatine kinase (CK), increasing the exercise intensity threshold before symptoms of muscle fatigue and cramping are experienced, and the skeletal muscles becoming aerobically conditioned.[36][37][6]
Oral sucrose treatment (for example a sports drink with 75 grams of sucrose in 660 ml.) taken 30 minutes prior to exercise has been shown to help improve exercise tolerance, including a lower heart rate and lower perceived level of exertion compared with placebo.[38] This is because the ingestion of a high-carbohydrate meal or drink causes transient hyperglycaemia, with the exercising muscle cells utilizing the high glucose in the blood for the glycolytic pathway. However, the ingestion of a high-carbohydrate meal or drink is problematic as a frequent form of treatment since it will increase the release of insulin, which inhibits the release of fatty acids[39] and subsequently will delay the ability to get into second wind.[10] The frequent ingestion of sucrose (e.g. sugary drinks), in order to avoid premature muscle fatigue and cramping, is also problematic in that it can lead to obesity as insulin will also stimulate triglyceride synthesis (develop body fat), and obesity-related ill health (e.g. type II diabetes and heart disease).[10]
A low dosage treatment with creatine showed a significant improvement of muscle problems compared to placebo in a small clinical study.[40]
A ketogenic diet has demonstrated beneficial for McArdle disease (GSD-V) as ketones readily convert to acetyl CoA for oxidative phosphorylation, whereas free fatty acids take a few minutes to convert into acetyl CoA.[41][42] Ketones are a part of fat metabolism,[39] the ketones can act as the main fuel before fatty acid catabolism takes over (second wind), during which the ketones would act as a supplementary fuel along side the fatty acids to produce adenosine triphosphate (ATP) by oxidative phosphorylation.
History
The deficiency was the first metabolic myopathy to be recognized, when the physician Brian McArdle described the first case in a 30-year-old man who always experienced pain and weakness after exercise. McArdle noticed this patient's cramps were electrically silent and his venous lactate levels failed to increase upon ischemic exercise. (The ischemic exercise consists of the patient squeezing a hand dynamometer at maximal strength for a specific period of time, usually a minute, with a blood pressure cuff, which is placed on the upper arm and set at 250 mmHg, blocking blood flow to the exercising arm.)
Notably, this is the same phenomenon that occurs when muscle is poisoned in vitro by iodoacetate, which inhibits the breakdown of glycogen into glucose and prevents the formation of lactate; as well as produces an electronically silent muscle contracture. Knowing what occurs to muscle poisoned by iodoacetate, helped McArdle speculate that a glycogenolytic block might be occurring when he first described the disease.[43] McArdle accurately concluded that the patient had a disorder of glycogen breakdown that specifically affected skeletal muscle. The associated enzyme deficiency was discovered in 1959 by W. F. H. M. Mommaerts et al.[44]
See also
- Glycogen storage disease
- Hitting the wall (muscle fatigue due to glycogen depletion)
- Inborn errors of carbohydrate metabolism
- Purine nucleotide cycle§Glycogenoses (GSDs)
- Second wind (increased ATP production primarily by fatty acids after glycogen depletion)
References
- ↑ Bissonnette B, Luginbuehl I, Engelhardt T (2019). "Glycogen Storage Disease Type V (GSD V)". Syndromes: Rapid Recognition and Perioperative Implications (2nd ed.). New York, NY: McGraw-Hill Education. Archived from the original on 2023-10-29. Retrieved 2021-12-12.
- ↑ 2.0 2.1 2.2 Nagaraju K, Lundberg IE (2013). "Inflammatory Diseases of Muscle and Other Myopathies". In Firestein GS, Budd RC, Gabriel SE, McInnes IB, O'Dell JR (eds.). Kelley's Textbook of Rheumatology. pp. 1404–1430.e5. doi:10.1016/b978-1-4377-1738-9.00085-2. ISBN 978-1-4377-1738-9.
- ↑ Rubio JC, Garcia-Consuegra I, Nogales-Gadea G, Blazquez A, Cabello A, Lucia A, et al. (February 2007). "A proposed molecular diagnostic flowchart for myophosphorylase deficiency (McArdle disease) in blood samples from Spanish patients". Human Mutation. 28 (2): 203–204. doi:10.1002/humu.9474. PMID 17221871.
- ↑ Valberg SJ (2008). "Skeletal Muscle Function". In Kaneko JJ, Harvey JW, Bruss MO (eds.). Clinical Biochemistry of Domestic Animals. pp. 459–484. doi:10.1016/b978-0-12-370491-7.00015-5. ISBN 978-0-12-370491-7.
- ↑ Brian McArdle at Who Named It?
- ↑ 6.0 6.1 6.2 6.3 Reason SL, Voermans N, Lucia A, Vissing J, Quinlivan R, Bhai S, Wakelin A (July 2023). "Development of Continuum of Care for McArdle disease: A practical tool for clinicians and patients". Neuromuscular Disorders. 33 (7): 575–579. doi:10.1016/j.nmd.2023.05.006. PMID 37354872. S2CID 259141690.
- ↑ Wolfe GI, Baker NS, Haller RG, Burns DK, Barohn RJ (April 2000). "McArdle's disease presenting with asymmetric, late-onset arm weakness". Muscle & Nerve. 23 (4): 641–645. doi:10.1002/(SICI)1097-4598(200004)23:4<641::AID-MUS25>3.0.CO;2-M. PMID 10716777. S2CID 22423841.
- ↑ 8.0 8.1 Scalco, Renata Siciliani; Morrow, Jasper M.; Booth, Suzanne; Chatfield, Sherryl; Godfrey, Richard; Quinlivan, Ros (September 2017). "Misdiagnosis is an important factor for diagnostic delay in McArdle disease". Neuromuscular disorders: NMD. 27 (9): 852–855. doi:10.1016/j.nmd.2017.04.013. ISSN 1873-2364. PMID 28629675. Archived from the original on 2023-07-30. Retrieved 2023-10-23.
- ↑ 9.0 9.1 9.2 9.3 9.4 Lucia, Alejandro; Martinuzzi, Andrea; Nogales-Gadea, Gisela; Quinlivan, Ros; Reason, Stacey; Bali, Deeksha; Godfrey, Richard; Haller, Ronald; Kishnani, Priya; Laforêt, Pascal; Løkken, Nicoline; Musumeci, Olimpia; Santalla, Alfredo; Tarnopolsky, Mark; Toscano, Antonio; Vissing, John; Voermans, Nicol; Wakelin, Andrew (December 2021). "Clinical practice guidelines for glycogen storage disease V & VII (McArdle disease and Tarui disease) from an international study group". Neuromuscular Disorders. 31 (12): 1296–1310. doi:10.1016/j.nmd.2021.10.006. Retrieved 26 October 2023.
- ↑ 10.0 10.1 10.2 10.3 10.4 Wakelin A (2017). Living With McArdle Disease (PDF). IAMGSD. p. 15. Archived (PDF) from the original on 2023-03-05. Retrieved 2023-10-23.
- ↑ 11.0 11.1 Salazar-Martínez E, Santalla A, Valenzuela PL, Nogales-Gadea G, Pinós T, Morán M, et al. (2021). "The Second Wind in McArdle Patients: Fitness Matters". Frontiers in Physiology. 12: 744632. doi:10.3389/fphys.2021.744632. PMC 8555491. PMID 34721068.
- ↑ Perez, M.; Martin, M. A.; Rubio, J. C.; Maté-Muñoz, J. L.; Gómez-Gallego, F.; Foster, C.; Andreu, A. L.; Arenas, J.; Lucia, A.; Fleck, S. J. (August 2006). "Exercise capacity in a 78 year old patient with McArdle's disease: it is never too late to start exercising". British Journal of Sports Medicine. 40 (8): 725–726, discussion 726. doi:10.1136/bjsm.2006.026666. ISSN 1473-0480. PMC 2579473. PMID 16864568. Archived from the original on 2023-05-15. Retrieved 2023-10-23.
- ↑ 13.0 13.1 13.2 Wakelin A (2013). 101 Tips For A Good Life With McArdle Disease (PDF). AGSD-UK Ltd. Archived (PDF) from the original on 2023-02-08. Retrieved 2023-10-23.
- ↑ Stanley M, Chippa V, Aeddula NR, Quintanilla Rodriguez BS, Adigunet R (10 August 2022). "Rhabdomyolysis". StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. PMID 28846335. Archived from the original on 28 October 2022. Retrieved 23 October 2023.
- ↑ 15.0 15.1 Scalco RS, Lucia A, Santalla A, Martinuzzi A, Vavla M, Reni G, et al. (November 2020). "Data from the European registry for patients with McArdle disease and other muscle glycogenoses (EUROMAC)". Orphanet Journal of Rare Diseases. 15 (1): 330. doi:10.1186/s13023-020-01562-x. PMC 7687836. PMID 33234167.
- ↑ 16.0 16.1 16.2 Martín MA, Lucia A, Arenas J, Andreu AL (1993). "Glycogen Storage Disease Type V". GeneReviews®. University of Washington, Seattle. PMID 20301518. Archived from the original on 2023-02-04. Retrieved 2023-10-23.
- ↑ Rodríguez-Gómez I, Santalla A, Díez-Bermejo J, Munguía-Izquierdo D, Alegre LM, Nogales-Gadea G, et al. (November 2018). "Non-osteogenic muscle hypertrophy in children with McArdle disease". Journal of Inherited Metabolic Disease. 41 (6): 1037–1042. doi:10.1007/s10545-018-0170-7. hdl:10578/19657. PMID 29594644. S2CID 4394513.
- ↑ Scalco RS, Chatfield S, Godfrey R, Pattni J, Ellerton C, Beggs A, et al. (July 2014). "From exercise intolerance to functional improvement: the second wind phenomenon in the identification of McArdle disease". Arquivos de Neuro-Psiquiatria. 72 (7): 538–541. doi:10.1590/0004-282x20140062. PMID 25054987.
- ↑ Pearson CM, Rimer DG, Mommaerts WF (April 1961). "A metabolic myopathy due to absence of muscle phosphorylase". The American Journal of Medicine. 30 (4): 502–517. doi:10.1016/0002-9343(61)90075-4. PMID 13733779.
- ↑ 20.0 20.1 Brull A, de Luna N, Blanco-Grau A, Lucia A, Martin MA, Arenas J, et al. (June 2015). "Phenotype consequences of myophosphorylase dysfunction: insights from the McArdle mouse model". The Journal of Physiology. 593 (12): 2693–2706. doi:10.1113/JP270085. PMC 4500353. PMID 25873271.
- ↑ Mineo I, Kono N, Hara N, Shimizu T, Yamada Y, Kawachi M, et al. (July 1987). "Myogenic hyperuricemia. A common pathophysiologic feature of glycogenosis types III, V, and VII". The New England Journal of Medicine. 317 (2): 75–80. doi:10.1056/NEJM198707093170203. PMID 3473284.
- ↑ Mineo I, Tarui S (1995). "Myogenic hyperuricemia: what can we learn from metabolic myopathies?". Muscle & Nerve. Supplement. 3: S75–S81. doi:10.1002/mus.880181416. PMID 7603532. S2CID 41588282.
- ↑ Ph.D, Kathryn Elizabeth Birch (2011-07-01). The McArdle Disease Handbook: A guide to the scientific and medical research into McArdle Disease, explained in plain English. AGSD-UK. ISBN 978-0-9569658-1-3. Archived from the original on 2020-09-22. Retrieved 2023-10-23.
- ↑ Triplet, Jacob J.; Goss, David A.; Taylor, Benjamin (September 2017). "Spontaneous Compartment Syndrome in a Patient with McArdle Disease: A Case Report and Review of the Literature". JBJS Case Connector. 7 (3): e49–e49. doi:10.2106/JBJS.CC.16.00196. ISSN 2160-3251. Archived from the original on 2023-10-29. Retrieved 2023-10-23.
- ↑ Mull, Aaron B.; Wagner, Janelle I.; Mycktayn, Terence M.; Kells, Amy F. (December 2015). "Recurrent Compartment Syndrome Leading to the Diagnosis of McArdle Disease: Case Report". The Journal of Hand Surgery. 40 (12): 2377–2379. doi:10.1016/j.jhsa.2015.09.015. ISSN 0363-5023. Archived from the original on 2023-10-29. Retrieved 2023-10-23.
- ↑ Martín MA, Rubio JC, Wevers RA, Van Engelen BG, Steenbergen GC, Van Diggelen OP, et al. (January 2004). "Molecular analysis of myophosphorylase deficiency in Dutch patients with McArdle's disease". Annals of Human Genetics. 68 (Pt 1): 17–22. doi:10.1046/j.1529-8817.2003.00067.x. PMID 14748827. S2CID 41149417.
- ↑ Rubio JC, Lucia A, Fernández-Cadenas I, Cabello A, Blázquez A, Gámez J, et al. (December 2006). "Novel mutation in the PYGM gene resulting in McArdle disease". Archives of Neurology. 63 (12): 1782–1784. doi:10.1001/archneur.63.12.1782. PMID 17172620.
- ↑ "PYGM - Glycogen phosphorylase, muscle form - Homo sapiens (Human) - PYGM gene & protein". www.uniprot.org. Archived from the original on 2021-04-14. Retrieved 2018-08-31.
 This article incorporates text available under the CC BY 4.0 license.
This article incorporates text available under the CC BY 4.0 license.
- ↑ "UniProt: the universal protein knowledgebase". Nucleic Acids Research. 45 (D1): D158–D169. January 2017. doi:10.1093/nar/gkw1099. PMC 5210571. PMID 27899622.
- ↑ "Reaction participants of glycogen phosphorylase". www.rhea-db.org. Archived from the original on 2021-01-25. Retrieved 2020-12-26.
- ↑ NCBI Gene ID 5837: PYGM phosphorylase, glycogen, muscle, archived from the original on 7 April 2021, retrieved 22 May 2013
- ↑ "PYGM", NLM Genetics Home Reference, archived from the original on 21 September 2020, retrieved 22 May 2013
- ↑ Kazemi-Esfarjani P, Skomorowska E, Jensen TD, Haller RG, Vissing J (August 2002). "A nonischemic forearm exercise test for McArdle disease". Annals of Neurology. 52 (2): 153–159. doi:10.1002/ana.10263. PMID 12210784. S2CID 43237025.
- ↑ Kitaoka Y (February 2014). "McArdle Disease and Exercise Physiology". Biology. 3 (1): 157–166. doi:10.3390/biology3010157. PMC 4009758. PMID 24833339.
- ↑ "IAMGSD | Training support". iamgsd. Archived from the original on 2022-12-04. Retrieved 2022-12-04.
- ↑ Pérez M, Moran M, Cardona C, Maté-Muñoz JL, Rubio JC, Andreu AL, et al. (January 2007). "Can patients with McArdle's disease run?". British Journal of Sports Medicine. 41 (1): 53–54. doi:10.1136/bjsm.2006.030791. PMC 2465149. PMID 17000713.
- ↑ Haller RG, Wyrick P, Taivassalo T, Vissing J (June 2006). "Aerobic conditioning: an effective therapy in McArdle's disease". Annals of Neurology. 59 (6): 922–928. doi:10.1002/ana.20881. PMID 16718692. S2CID 31921729.
- ↑ Vissing J, Haller RG (December 2003). "The effect of oral sucrose on exercise tolerance in patients with McArdle's disease". The New England Journal of Medicine. 349 (26): 2503–2509. doi:10.1056/NEJMoa031836. PMID 14695410.
- ↑ 39.0 39.1 Coffee, Carole J. (1999). Quick Look Medicine: Metabolism. Hayes Barton Press. ISBN 1-59377-192-4.
- ↑ Vorgerd M, Grehl T, Jager M, Muller K, Freitag G, Patzold T, et al. (July 2000). "Creatine therapy in myophosphorylase deficiency (McArdle disease): a placebo-controlled crossover trial". Archives of Neurology. 57 (7): 956–963. doi:10.1001/archneur.57.7.956. PMID 10891977.
- ↑ Løkken N, Hansen KK, Storgaard JH, Ørngreen MC, Quinlivan R, Vissing J (July 2020). "Titrating a modified ketogenic diet for patients with McArdle disease: A pilot study". Journal of Inherited Metabolic Disease. 43 (4): 778–786. doi:10.1002/jimd.12223. PMID 32060930. S2CID 211121921.
- ↑ Løkken N, Voermans NC, Andersen LK, Karazi W, Reason SL, Zweers H, et al. (February 2023). "Patient-Reported Experiences with a Low-Carbohydrate Ketogenic Diet: An International Survey in Patients with McArdle Disease". Nutrients. 15 (4): 843. doi:10.3390/nu15040843. PMID 36839201.
- ↑ Layzer RB (February 1985). "McArdle's disease in the 1980s". The New England Journal of Medicine. 312 (6): 370–371. doi:10.1056/NEJM198502073120609. PMID 3855500.
- ↑ Mommaerts WF, Illingworth B, Pearson CM, Guillory RJ, Seraydarian K (June 1959). "A Functional Disorder of Muscle Associated with the Absence of Phosphorylase". Proceedings of the National Academy of Sciences of the United States of America. 45 (6): 791–797. Bibcode:1959PNAS...45..791M. doi:10.1073/pnas.45.6.791. PMC 222638. PMID 16590445.
External links
- Euromac, an EU-funded consortium of medical and research institutes across Europe which is building a patient registry and raising standards of care for people with McArdle Disease. Archived 2021-04-22 at the Wayback Machine
- International Association for Muscle Glycogen Storage Disease (IamGSD). Archived 2023-10-04 at the Wayback Machine
- Walking With McArdle's Archived 2022-12-07 at the Wayback Machine - IamGSD videos
- EUROMAC Introduction Archived 2022-12-07 at the Wayback Machine - Video about McArdle disease and the EUROMAC Registry of McArdle disease and other rare glycogenoses patients
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- Articles with imported freely licensed text
- All articles with unsourced statements
- Articles with unsourced statements from October 2021
- Articles with invalid date parameter in template
- Articles with unsourced statements from August 2022
- Articles with unsourced statements from December 2016
- Webarchive template wayback links
- Autosomal recessive disorders
- Inborn errors of carbohydrate metabolism
- Muscular disorders
