Gastroschisis
| Gastroschisis | |
|---|---|
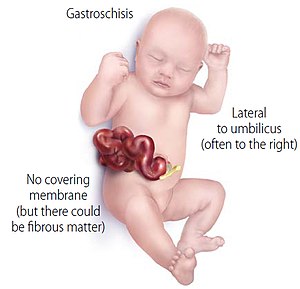 | |
| Drawing of a child with gastroschisis | |
| Pronunciation |
|
| Specialty | General surgery, medical genetics |
| Symptoms | Intestines extend outside of the body through a hole next to the belly button[2] |
| Complications | Feeding problems, prematurity, intrauterine growth retardation[1][3] |
| Usual onset | During early development[1] |
| Causes | Unknown[1] |
| Risk factors | Mother who smokes, drinks alcohol, or is younger than 20[3][1] |
| Diagnostic method | Ultrasound during pregnancy, based on symptom at birth[1] |
| Differential diagnosis | Omphalocele, prune belly syndrome[3][4] |
| Treatment | Early surgery[1] |
| Frequency | 4 per 10,000 births[3] |
Gastroschisis is a birth defect in which the baby's intestines extend outside of the abdomen through a hole next to the belly button.[2] The size of the hole is variable, and other organs including the stomach and liver may also occur outside the baby's body.[1] Complications may include feeding problems, prematurity, intestinal atresia, and intrauterine growth retardation.[1][3]
The cause is typically unknown.[3][1] Rates are higher in babies born to mothers who smoke, drink alcohol, or are younger than 20 years old.[3][1] Ultrasounds during pregnancy may make the diagnosis.[1] Otherwise diagnosis occurs at birth.[1] It differs from omphalocele in that there is no covering membrane over the intestines.[3]
Treatment involves surgery.[1] This typically occurs shortly after birth.[1] In those with large defects the exposed organs may be covered with a special material and slowly moved back into the abdomen.[1] The condition affects about 4 per 10,000 newborns.[3] Rates of the condition appear to be increasing.[1]
Signs and symptoms
There are no signs during pregnancy. About sixty percent of infants with gastroschisis are born prematurely.[5] At birth, the baby will have a relatively small (<4 cm) hole in the abdominal wall, usually just to the right of the belly button.[6] Some of the intestines are usually outside the body, passing through this opening. In rare circumstances, the liver and stomach may also come through the abdominal wall.[7] After birth these organs are directly exposed to air.[5]
Causes
The cause of gastroschisis is not known. There may be genetic causes in some cases, and there may be environmental factors to which the mother is exposed during pregnancy.[8]
Risk factors include the mother being young, and use of alcohol or tobacco.[8]
Pathophysiology
During the fourth week of human embryonic development, the lateral body wall folds of the embryo meet at the midline and fuse together to form the anterior body wall.[9] However, in gastroschisis and other anterior body wall defects, this fails to occur by either one or both of the lateral body wall folds not moving properly to meet with the other and fusing together.[10] This incomplete fusion results in a defect that allows abdominal organs to protrude through the abdominal wall, and the intestines typically herniate through the rectus abdominis muscle, lying to the right of the umbilicus. The forces responsible for the movement of the lateral body wall folds are poorly understood, and a better understanding of these forces would help to explain why gastroschisis occurs mostly to the right of the umbilicus, while other ventral body wall defects occur in the midline.[9]
At least six hypotheses have been proposed for the pathophysiology:
- Failure of mesoderm to form in the body wall[11]
- Rupture of the amnion around the umbilical ring with subsequent herniation of bowel[12]
- Abnormal involution of the right umbilical vein leading to weakening of the body wall and gut herniation[13]
- Disruption of the right vitelline (yolk sac) artery with subsequent body wall damage and gut herniation[14]
- Abnormal folding of the body wall results in a ventral body wall defect through which the gut herniates[10]
- Failure to incorporate the yolk sac and related vitelline structures into the yolk sac[15]
The first hypothesis does not explain why the mesoderm defect would occur in such a specific small area. The second hypothesis does not explain the low percentage of associated abnormality compared with omphalocele. The third hypothesis was criticized due to no vascular supplement of anterior abdominal wall by umbilical vein. The fourth hypothesis was commonly accepted, but it was later shown that the right vitelline artery (right omphalomesenteric artery) did not supply the anterior abdominal wall in this area.[16] More evidence is needed to support the fifth hypothesis.[10]
Diagnosis

In the developed world, around 90% of cases are identified during normal ultrasound screens, usually in the second trimester.[17]
Distinguished from other ventral body wall defects such as omphalocele, there is no overlying sac or peritoneum, and the defect is usually much smaller in gastroschisis.[10]
Treatment

Gastroschisis requires surgical treatment to return the exposed intestines to the abdominal cavity and close the hole in the abdomen. Sometimes this is done immediately but more often the exposed organs are covered with sterile drapings, and only later is the surgery done. Affected newborns frequently require more than one surgery, as only about 10% of cases can be closed in a single surgery.[5]: 1141–1142
Given the urgent need for surgery after birth, it is recommended that delivery occur at a facility equipped for caring for these high-risk neonates, as transfers to other facilities may increase risk of adverse outcomes.[7] There is no evidence that cesarean deliveries lead to better outcomes for babies with gastroschisis, so cesarean delivery is only considered if there are other indications.[19]
The main cause for lengthy recovery periods is the time taken for the infant's bowel function to return to normal. After surgery infants are fed through IV fluids and gradually introduced to normal feeding.[5]
Prognosis
If left untreated, gastroschisis is fatal to the infant; however, in adequate settings the survival rate for treated infants is 90%.[20][21]
Most risks of gastroschisis are related to decreased bowel function. Sometimes blood flow to the exposed organs is impaired or there is less than the normal amount of intestine. This may put infants at risk for other dangerous conditions such as necrotizing enterocolitis. Also, because their intestines are exposed, infants with gastroschisis are at increased risk for infection, and must be closely monitored.[5]
After surgery a child with gastroschisis will have some degree of intestinal malrotation. About 1% of children will experience a midgut volvulus after surgery.[22]
Epidemiology
As of 2015 the worldwide incidence was about 2 to 5 per 10 000 live births, and this number seemed to be increasing.[17]
As of 2017 the CDC estimates that about 1,871 babies are born each year in the United States with gastroschisis.[8]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 "Facts about Gastroschisis". National Center on Birth Defects and Developmental Disabilities Home | NCBDDD | CDC. 27 June 2017. Archived from the original on 18 July 2017. Retrieved 14 July 2017.
- ↑ 2.0 2.1 "Gastroschisis". Genetic and Rare Diseases Information Center (GARD). 2017. Archived from the original on 5 July 2017. Retrieved 14 July 2017.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Reference, Genetics Home (August 2016). "Abdominal wall defect". Genetics Home Reference. Archived from the original on 10 July 2017. Retrieved 14 July 2017.
- ↑ "Gastroschisis". NORD (National Organization for Rare Disorders). 2007. Archived from the original on 21 February 2017. Retrieved 14 July 2017.
- ↑ 5.0 5.1 5.2 5.3 5.4 Conn's current therapy 2017. Bope, Edward T., Kellerman, Rick D. Philadelphia: Elsevier. 2017. ISBN 9780323443203. OCLC 961064076.
{{cite book}}: CS1 maint: others (link) - ↑ Sadler, Thomas W. (August 2010). "The embryologic origin of ventral body wall defects". Seminars in Pediatric Surgery. 19 (3): 209–214. doi:10.1053/j.sempedsurg.2010.03.006. ISSN 1532-9453. PMID 20610194.
- ↑ 7.0 7.1 W., Bianchi, Diana (2000). Fetology: diagnosis & management of the fetal patient. Bianchi, Diana W., Crombleholme, Timothy M., D'Alton, Mary E. New York: McGraw-Hill, Medical Pub. Division. ISBN 0838525709. OCLC 44524363.
- ↑ 8.0 8.1 8.2 "Facts about Gastroschisis". CDC. June 27, 2017. Archived from the original on July 18, 2017.
- ↑ 9.0 9.1 Sadler, T. W.; Feldkamp, Marcia L. (2008-08-15). "The embryology of body wall closure: relevance to gastroschisis and other ventral body wall defects". American Journal of Medical Genetics Part C: Seminars in Medical Genetics. 148C (3): 180–185. doi:10.1002/ajmg.c.30176. ISSN 1552-4876. PMID 18655098.
- ↑ 10.0 10.1 10.2 10.3 Feldkamp, Marcia L.; Carey, John C.; Sadler, Thomas W. (2007). "Development of gastroschisis: Review of hypotheses, a novel hypothesis, and implications for research". American Journal of Medical Genetics Part A. 143A (7): 639–652. doi:10.1002/ajmg.a.31578. PMID 17230493.
- ↑ Duhamel, B. (1963). "Embryology of Exomphalos and Allied Malformations". Archives of Disease in Childhood. 38 (198): 142–7. doi:10.1136/adc.38.198.142. PMC 2019006. PMID 21032411.
- ↑ Shaw, Anthony (1975). "The myth of gastroschisis". Journal of Pediatric Surgery. 10 (2): 235–44. doi:10.1016/0022-3468(75)90285-7. PMID 123582.
- ↑ Devries, Pieter A. (1980). "The pathogenesis of gastroschisis and omphalocele". Journal of Pediatric Surgery. 15 (3): 245–51. doi:10.1016/S0022-3468(80)80130-8. PMID 6445962.
- ↑ Hoyme, H; Higginbottom, M; Jones, K (1981). "The vascular pathogenesis of gastroschisis: Intrauterine interruption of the omphalomesenteric artery". The Journal of Pediatrics. 98 (2): 228–31. doi:10.1016/S0022-3476(81)80640-3. PMID 6450826.
- ↑ Stevenson, RE; Rogers, RC; Chandler, JC; Gauderer, MWL; Hunter, AGW (2009). "Escape of the yolk sac: a hypothesis to explain the embryogenesis of gastroschisis". Clinical Genetics. 75 (4): 326–33. doi:10.1111/j.1399-0004.2008.01142.x. PMID 19419415.
- ↑ Curry, Cynthia; Boyd, Ellen; Stevenson, Roger E. (2006). "Ventral Wall of the Trunk". In Stevenson, Roger E.; Hall, Judith G. (eds.). Human Malformations and Related Anomalies. Oxford: Oxford University Press. pp. 1023–49. ISBN 978-0-19-516568-5.
{{cite book}}:|archive-url=requires|url=(help); Unknown parameter|chapterurl=ignored (help) - ↑ 17.0 17.1 D'Antonio, F; Virgone, C; Rizzo, G; Khalil, A; Baud, D; Cohen-Overbeek, TE; Kuleva, M; Salomon, LJ; Flacco, ME; Manzoli, L; Giuliani, S (July 2015). "Prenatal Risk Factors and Outcomes in Gastroschisis: A Meta-Analysis". Pediatrics. 136 (1): e159-69. doi:10.1542/peds.2015-0017. PMID 26122809. Archived from the original on 2017-11-05.
- ↑ Oyinloye, Adewale O.; Abubakar, Auwal M.; Wabada, Samuel; Oyebanji, Lateef O. (4 March 2020). "Challenges and Outcome of Management of Gastroschisis at a Tertiary Institution in North-Eastern Nigeria". Frontiers in Surgery. 7: 8. doi:10.3389/fsurg.2020.00008.
- ↑ Segel, S. Y.; Marder, S. J.; Parry, S.; Macones, G. A. (November 2001). "Fetal abdominal wall defects and mode of delivery: a systematic review". Obstetrics and Gynecology. 98 (5 Pt 1): 867–873. doi:10.1016/s0029-7844(01)01571-x. ISSN 0029-7844. PMID 11704185.
- ↑ Santiago-Munoz PC, McIntire DD, Barber RG, Megison SM, Twickler DM, Dashe JS (2007). "Outcomes of pregnancies with fetal gastroschisis". Obstet Gynecol. 110 (3): 663–8. doi:10.1097/01.AOG.0000277264.63736.7e. PMID 17766615.
- ↑ Baerg J, Kaban G, Tonita J, Pahwa P, Reid D (2003). "Gastroschisis: A sixteen-year review". J Pediatr Surg. 38 (5): 771–4. doi:10.1016/jpsu.2003.50164. PMID 12720191.
- ↑ Fawley, Jason A (2016). "The risk of midgut volvulus in patients with abdominal wall defects: A multi-institutional study". Journal of Pediatric Surgery. 52 (1): 26–29. doi:10.1016/j.jpedsurg.2016.10.014. PMID 27847120.
External links
| Classification | |
|---|---|
| External resources |