Frontal lobe epilepsy
| Frontal lobe epilepsy | |
|---|---|
| Other names: Frontal lobe seizures | |
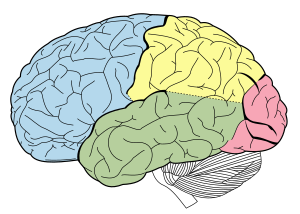 | |
| Lobes of the human brain with the frontal lobe shown in blue | |
| Specialty | Neurology |
| Symptoms | Seizures with significant movement but without loss of consciousness[1] |
| Causes | Genetics, malformed areas of brain, brain tumors, injury[2] |
| Diagnostic method | Based on symptoms, supported by medical imaging[2] |
| Differential diagnosis | Psychogenic non-epileptic seizures (PNES);[3] sleep disorders; absence seizures;[1] paroxysmal kinesigenic choreoathetosis[2] |
| Treatment | Anti-epileptic medications, ketogenic diet, vagal nerve stimulation, surgery[2][3] |
| Frequency | 1 in 5,000 to 20,000[2][4] |
Frontal lobe epilepsy (FLE) is a type of epilepsy often characterized by seizures with significant movement but without loss of consciousness.[1] Movements may include pelvic thrusting or peddling of both legs.[1] Other symptoms may include making sounds, unusual behavior, loss of bladder control, and eyes turned to one side.[1] People may feel the seizures coming on.[1] Following the seizure there may be a period were the person is unable to move part of their body; while, a period of confusion is often lacking.[2]
Causes may include genetics, malformed areas of brain, brain tumors, and injury.[2] They often only occur while the person is sleeping.[5][6] They arise from the frontal lobe of the brain.[2] Diagnosis may be based on symptoms.[2] In around 66% of cases MRI finds abnormalities, while an EEG often adds little.[2] Positron emission tomography (PET) or single photon emission CT (SPECT) may also help localize the area affected.[3] Other conditions that may appear similar include psychogenic non-epileptic seizures (PNES), and sleep disorders.[1][3]
Initial treatment may involve anti-epileptic medications, a ketogenic diet, or vagal nerve stimulation.[2][3] While medications often do not stop seizures, they may prevent generalized seizures from occurring.[2] If this is not effective, surgery to remove the effected part of the frontal lobe may be carried out.[3] Surgery is fully successful in about 30% of people at 5 years.[3]
Epilepsy is relatively common, affecting 0.5-1% of the population,[4] with frontal lobe epilepsy accounts for about 1-2% of this number (1 in 5,000 to 20,000).[2] It is the second most common type of focal epilepsy after temporal lobe epilepsy.[5] Males and females are affected with similar frequency.[2] The first clear description of a frontal lobe seizure dates from 1827 by J. F. Bravais.[6]
Signs and symptoms
Symptoms of frontal lobe seizures may include[7]
- Head and eye movements to one side
- Complete or partial unresponsiveness or difficulty speaking
- Explosive screams, including profanities, or laughter
- Abnormal body posturing, especially fencing position
- Repetitive movements, such as rocking, bicycle pedaling or pelvic thrusting
Epileptic symptoms are frequently the product of the spread of overactivation occurring within one central foci that travels to lateral brain regions thereby causing an array of symptoms. Due to the massive amount of diversity in both the cognitive and motor functions that occur within the frontal lobes, there is an immense variety in the types of symptoms that can arise from epileptic seizures based on the side and topography of the focal origin. In general these symptoms can range anywhere from asymmetric and abnormal body positioning to repetitive vocal outbursts and repetitive jerking movements.[7] The symptoms typically come in short bursts that last less than a minute and often occur while a patient is sleeping.[8] In most cases, a patient will experience a physical or emotional Aura of tingling, numbness or tension prior to a seizure occurring.[9] Fear is associated with temporal and frontal lobe epilepsies, but in FLE the fear is predominantly expressed on the person's face whereas in TLE the fear is subjective and internal, not perceptible to the observer.[2]
Tonic posture and clonic movements are common symptoms among most of the areas of the frontal lobe, therefore the type of seizures associated with frontal lobe epilepsy are commonly called tonic-clonic seizures. Dystonic motor movements are common to both TLE and FLE, but are usually the first symptom in FLE episodes where they are quite brief and do not affect consciousness. The seizures are complex partial, simple partial, secondarily generalized or a combination of the three. These partial seizures are often misdiagnosed as psychogenic seizures.[2]
Types
A wide range of more specific symptoms arise depending on the parts of the frontal cortex are affected.[10]
- Supplementary motor area (SMA)
- The onset and relief of the seizure are quite abrupt.
- The tonic posturing in this area is unilateral or asymmetric between the left and right hemispheres. A somatosensory aura frequently precedes many large motor and vocal symptoms and most often the afflicted person is responsive.
- Motor symptoms: Facial grimacing and complex automatisms like kicking and pelvic thrusting
- Vocal symptoms: Laughing, yelling, or speech arrest.[9]
- Primary motor cortex
- The primary motor cortex has jacksonian seizures that spread to adjacent areas of the lobe which often trigger a second round of seizures originating in another cortical area. The seizures are much simpler than those that originate in the SMA and are usually clonic or myoclonic movements with speech arrest. Some dystonic or contralateral adversive posturing may also be present.[10][9]
- Medial frontal, cingulate gyrus, orbitofrontal, or frontopolar regions
- Motor symptoms of seizures in this area are accompanied by emotional feelings and viscerosensory symptoms. Motor and vocal agitation are similar to that of the SMA with short repetitive thrashing, pedaling, thrusting, laughing, screaming and/or crying.
- This is some of what can cause the misdiagnosis of a psychological disorder.[10][8]
- Dorsolateral cortex
- This area does not seem to have many motor symptoms beyond tonic posturing or clonic movements. Contralateral or less commonly ipsilateral head turn and eye deviation are commonly associated with this area as well.[10]
- Operculum
- Many of the symptoms associated with this area involve the head and digestive tract: swallowing, salivation, mastication and possibly gustatory hallucinations. Preceding the seizure the person is fearful and often has an epigastric aura. There is not much physical movement except clonic facial movements. Speech is often arrested.[10]
Causes

The origins of frontal lobe seizures can be different deviations.[11] One of the major reasons for FLE is abnormal cognitive development or sometimes congenital abnormal brain development.[11] Other reasons are:
- Tumors[11]
- Head Trauma
- Genetic
Apart from the above-mentioned reason, there are a few unknown factors that can trigger the seizures:[12]
- Sleep deprivation
- Waking up
- Stress
- Hormonal changes, such as during menstruation
- Alcohol
- Certain medications
- Illegal substances [12]
Tumors
Tumors account for about one-third of all frontal lobe epilepsy cases.[10] Low-grade tumors such as gangliogliomas, low-grade gliomas, and epidermoid tumors are most common, but many high-grade tumors were most likely once involved with seizures.[10] Other lesions on the frontal lobe such as hamartomas and nodular heterotopias can cause frontal lobe symptoms as well.[10] Birth defects such as vascular malformation are known to cause seizures, especially arteriovenous malformations, and cavernous angiomas.[10]
Head trauma
Head trauma frequently causes damage to the frontal lobe and can cause seizures directly or indirectly through gliosis.[10] Seizures originating directly from head trauma usually occur within a few months, but occasionally they can take years to manifest.[10] On occasion, encephalitis can cause frontal lobe seizures but it is most often associated with an affected temporal lobe.[10]
Genetics
The main genetic cause of frontal lobe epilepsy is an autosomal dominant disease called Autosomal Dominant Nocturnal Frontal Lobe Epilepsy, which involves mutations in 2 nicotinic acetylcholine receptor genes.[10] A genetic mutation on chromosome 22 has also been associated with another genetic form of the disorder.[10]
Mechanism
Due to the difference in brain processing and function as well as various surface anatomy landmarks, the frontal lobes have traditionally been divided into two major areas known as the precentral cortex and prefrontal cortex.
Precentral cortex
The precentral cortex is an area of the frontal cortex that is located directly anterior to the central sulcus and includes both the primary motor cortex and the supplementary motor area.[9] Inputs that project to both of these areas arise from a variety of locations in the brain that integrate sensory stimuli including the primary motor cortex, the thalamus and corticospinal projections.[9] These two areas along with several other main functional areas control both the preparation of motor movement as well as the execution of movements. These main functional areas are crucial to the development of the motor related symptoms associated with frontal lobe epilepsy focally when seizures are located within these defined areas.[13] The major functional areas include:
- Primary motor cortex
- Contains large neurons that project axons down to the spinal cord where they synapse onto alpha motor neurons. These neurons are involved in the planning of motor movements and the refining of motor movements based on sensory inputs that are received from the cerebellum.[14]
- Supplementary motor area
- Frontal eye field
- The frontal eye field is a posterior part of the middle frontal gyrus and is involved in the control of saccadic, contralateral and conjugate eye movement. This area receives its main inputs from both the occipital cortex and dorsal thalamus.[9]
- Broca's area
- Controls the motor movements of both the tongue and larynx that enables speech formation. This area receives direct inputs from the primary motor area as well as Wernicke's area located in the temporal lobe.[15]
Prefrontal cortex
The prefrontal cortex, the most anterior region of the brain, comprises several key areas that are particularly important for higher mental functions that control various aspects of human personality including anticipation and planning, initiative/judgement, memory and the control of decision making.[16] Damage or lesions to this region of the brain can result in major changes in personality. A classic example is Phineas Gage, who exhibited a change in behavior after one or both frontal lobes were destroyed by a large iron bar accidentally driven through his head (though Gage, despite conventional presentations of his case, did not exhibit the aggression, antisocial behavior, or loss of impulse control sometimes reported in patients with similar injuries).
There are two main regions of the prefrontal cortex that each control various aspects of behavior and personality:
- Dorsolateral prefrontal cortex
- This area is associated with the impairment of the cognitive abilities that control and regulate behavior and long-term memory formation (especially relating to procedural sequence memory) when either brain damage or a lesion is present.[16]
- Orbitofrontal cortex
- The orbitofrontal cortex has similar functions as the dorsolateral prefrontal cortex but is thought to be mainly responsible for the ability to make choices and determine right from wrong.[17][citation needed]
Diagnosis
The diagnosis of FLE is difficult due to the overlapping and similar symptoms to psychiatric disorders.[11] The diagnosis of FLE has been done by clinicians, and their reviews of the medical history, and physical and neurological examinations. The following neurological tests can be helpful for diagnosing FLE[11]
- Electroencephalography (EEG)
- MRI
- Video EEG
Electroencephalography
Electroencephalography (EEG) helps in finding out the exact area of the brain where seizures occur.[11] In the case of FLE, the EEG is almost normal.[11] MEG and electroencephalography (EEG) in the temporal domain provides a better and wider view of information exchange across networks in patients with impaired and unimpaired FLE.[18]
Neuroimaging
Advancements in technology, has given rise to newer, more efficient methods of diagnosis, most prominent being in the domain of neuroimaging.[18] The high spatial resolution from fMRI has implications on certain brain regions contributing to memory.[18] The usage of task fMRI for examination of memory or other higher cognitive networks may also be used to predict ictal onset zone(s) in patients with FLE, giving the advantage of refinement of patient-specific analyses.[18] The use of multi-modal approaches in association with neuroimaging techniques like fMRI and MEG or EEG will be informative in characterizing atypical functional brain networks in FLE.[18] But, difficulty remains in the evaluation of potential compensatory mechanisms between patients with FLE with normal and impaired memory, without properly characterizing transfer of information during memory tasks.[18]
Genetics
Diagnosis of ADNFLE, however, is not only based on neuroimaging, and ictal and interictal EEGs, but also on family history and genetic counseling.[19] Certain molecular and genomics testing that can include multi-gene panel of CHRNA4, CHRNB2, CHRNA2, KCNT1, DEPDC5, CRH, serial single gene testing of pathogenic variants, and can also be comprehensive genomic testing.[20] There has to be continuous neuroimaging and EEGs, for reevaluation at regular intervals, to keep a check on disease progression.[20]
Video EEG
As the FLE occurred during sleep video EEG is one of the useful tools for diagnosis of FLE.[11] The monitoring can be done in the sleep lab in the hospital overnight.[11] Both brain activity, as well as behavioral movement, can be captured by using video EEG.[11]
PET scan
Positron emission tomography (PET) helps to locate epileptogenic loci.[9] If the MRI were normal the PET scan could locate some abnormalities.[9]
Differential diagnosis
Episodes that include complex hyperactivity of the proximal portions of the limbs that lead to increased overall motor activity are called hypermotor seizures. When associated with bizarre movements and vocalizations these seizures are often misdiagnosed as pseudoseizures or other episodic movement disorders such as psychogenic movement disorders, familial paroxysmal dystonic choreoathetosis, paroxysmal kinesogenic choreoathetosis, or episodic ataxia type 1.[2] Hypermotor seizure in children are often confused with pavor nocturnus (night terrors). Paroxysmal nocturnal dystonia or hypnogenic paroxysmal dystonia are other names given to describe FLE symptoms but are simply just FLE.[2]
Autosomal dominant nocturnal frontal lobe epilepsy (ADNFLE) is the best understood form of frontal lobe epilepsy but is often misdiagnosed as sleep apnea. Both disorders are characterized by awakening during the night which leads to daytime sleepiness. Some symptoms of sleep apnea overlap with those of ADNFLE, such as sudden awakening accompanied by a feeling of choking and on occasion motor activity which makes diagnosis difficult based on symptoms alone. Video surveillance as well as EEG is occasionally needed to differentiate between the two disorders. It has been reported that sleep apnea might be associated with epilepsy which would account for some of the misdiagnoses.[2]
Treatments
There are several different ways to treat frontal lobe epileptic seizures, however, the most common form of treatment is through the use of anticonvulsant medications that help to prevent seizures from occurring. In some cases, however, when medications are ineffective, a neurologist may choose to operate on the patient in order to remove the focal area of the brain in which the seizures are occurring. Other treatments that can be administered to aid in reducing the occurrence of seizures include the implementation of a specific, regimented diet and/or the implantation of a vagus nerve stimulator, or deep brain stimulation (DBS).
Medications
Anticonvulsants like oxcarbazepine or other drugs are the most successful medication in reducing and preventing frontal lobe seizures.[11] Oxcarbazepine helps in the reduction of seizure frequencies.[11] There are a wide range of anticonvulsants that have both different modes of action and different abilities in preventing certain types of seizures. Some of the anticonvulsants that are prescribed to patients today include: oxcarbazepine, carbamazepine, phenytoin, gabapentin, levetiracetam, lamotrigine, topiramate, tiagabine, zonisamide and pregabalin.[10] KCNT1 pathogenic variant associated ADNFLE can be managed by treatment with quinidine,[21] and ADNFLE associated with CHRNA4 shows better responsiveness to zonisamide.[22]
Lorazepam, diazepam, and midazolam are front line treatment for severe convulsions, belonging to the benzodiazepine class of medications.
Surgery
When both the amount and severity of seizures becomes uncontrollable and seizures remain resistant to the various anticonvulsants, a patient most likely will be considered for epilepsy surgery. But, while performing it, there is the need for identifying or pinpointing the exact location of the seizure in the brain. This, in recent times have been aided by some of the modern techniques such as, SISCOM i.e., subtraction ictal SPECT co registered to MRI, SPECT i.e. single-photon emission computerized tomography, brain mapping performed before the surgery and functional MRI (fMRI), especially for the language area mapping.[23]
Surgeries include, a frontal lobectomy.[24] This procedure involves the removal of focal regions of the frontal lobes that have been identified as being problematic for the patient. It has been found that around 30% to 50% of patients that undergo a frontal lobectomy will forever be free from seizures that cause a loss of consciousness or cause abnormal movements.[25]
If on the other hand, the seizures occur in an area that is too vital to remove (such as areas that control motor, sensory or language functions), then the surgeon will perform a procedure known as a multiple subpial transection. This procedure involves making a series of cuts that surround the focal region where the seizures have originated.[26] By making cuts surrounding the focal region, the surgeon is able to isolate that specific section of the brain and prevent electrical impulses from being able to travel horizontally to other areas of the brain.
The last surgical procedure that can be done to help prevent the reoccurrence of seizures in the frontal lobes is to implant a stimulator on the vagus nerve. This device is a self-activating device that is inserted directly under the skin and can be controlled directly by the patient.[27] When a patient is feeling the onset of an aura, he/she can activate the stimulator which in turn will provide stimulation to the left vagus nerve (the left vagus nerve is used because the right nerve plays a role in cardiac function). Although little is understood about the exact mechanism for vagal nerve stimulation, it has been proven to be a successful treatment that can often terminate seizures before they begin.
Another novel procedure that can be used, utilizes a mechanism similar to that of a cardiac pacemaker. The electrode is implanted into the patient's brain, while a neuro-stimulator machine is placed beneath the skin of the chest. The stimulator sends indication to the electrode in the brain to prevent any signal that potentially triggers or can trigger a seizure. This procedure is named as the deep brain stimulation (DBS).[28]
Diet
The use of a regimented diet is an approach that has been found to help control seizures in children with severe, medically intractable frontal lobe epilepsy. Although the use of dieting to prevent seizures from occurring is a lost treatment that has been replaced by the use of new types of anticonvulsants, it is still recommended to patients to this day. A ketogenic diet is a high-fat, low-carbohydrate based diet that patients are typically asked to follow in conjunction with their anticonvulsant medications.[29] This diet was designed in order to mimic many of the effects that starvation has on the metabolic functioning of the body. By limiting the amount of carbohydrates and increasing the amount of exogenous fats available to the metabolism, the body will create an excess of water-soluble compounds known as ketone bodies.[29] Although the mechanism of action is still unknown, it is believed that these excessive amounts of ketone bodies become the brain's main source of energy and in turn are able to suppress the frequency of seizure occurrence.
Epidemiology
Epilepsy is a relatively common disorder, affecting between 0.5-1% of the population,[30] and frontal lobe epilepsy accounts for about 1-2% of all epilepsies.[2] The most common subdivision of epilepsy is symptomatic partial epilepsy, which causes simple partial seizures, and can be further divided into temporal and frontal lobe epilepsy. Although the exact number of cases of frontal lobe epilepsy is not currently known, it is known that FLE is the less common type of partial epilepsy, accounting for 20-30% of operative procedures involving intractable epilepsy.[31] The disorder also has no gender or age bias, affecting males and females of all ages. In a recent study, the mean subject age with frontal lobe epilepsy was 28.5 years old, and the average age of epilepsy onset for left frontal epilepsy was 9.3 years old whereas for right frontal epilepsy it was 11.1 years old.[10]
Society and culture
Epilepsy has a substantial impact on the quality of life of the individuals that are afflicted with it. Physicians and researchers are coming to understand that the impact on the quality of life of the patient is as important as the effects of the seizures.[32] Quality of life questionnaires and other assessment tools have been created to help quantify quality of life for individual patients. They consider such factors as physical health (including numbers and severity of seizures, medication side effects etc.), mental health, social relationships, lifestyle, role activities and life fulfillment.[33] A Center for Disease Control study reported that seizure sufferers were more likely to have lower education levels, higher unemployment, higher levels of pain, hypersomnia/insomnia, increased psychological distress and social isolation/connection issues.[34] Some of the issues which impact quality of life for people with epilepsy are: ability to drive and travel, the ability to date, marry and have children, the ability to have a job and independence, the ability to have an education and learn, and the ability to have good health and mental functioning.[35] Future research is needed to find ways of not only controlling frontal lobe seizures, but of also addressing the specific quality-of-life issues that plague those with frontal lobe epilepsy.
- Driving and transportation restrictions
- Driving and travel restrictions are one of the greatest limitations that epileptic patients experience. Laws restricting driving privileges vary greatly in the United States as well as across the world. In the United States, 28 states require a patient to be seizure free for fixed periods of time ranging from 3–12 months.[36] However, research done by Johns Hopkins University showed that there was no difference in seizure-related fatal crash rates in states with 3-month restrictions versus states with 6-12 month seizure-free restrictions. In 23 states, the restrictions and seizure free periods vary depending on the type of epilepsy and the individual case and in 13 states physicians were responsible for determining whether their patients should be allowed to drive.[36] In 6 of those 13 states physicians could be held legally liable for their decisions regarding their epileptic patients’ driving capabilities.[36] In many states, patients can also be legally liable for accidents, injury, damage and death caused by seizure related accidents.
- One of the major arguments in favor of restricting the licensing of epileptic drivers is the concern for public safety. However, the Johns Hopkins study showed that in a particular 2 year timeframe only 0.2% of fatal crashes occurred as a result of seizures.[37] Alcohol related crash fatalities caused 156 times more driver deaths than seizure related crashes and young drivers between the ages of 16 and 24 were 123 times more likely to die in a fatal crash caused by their inexperience than an epileptic driver was to die in a crash that resulted from a seizure.[38]
- Frontal lobe epileptic seizures unlike other epileptic seizures create symptoms that are as dangerous as loss of consciousness and much more difficult to discern from other problems such as substance use disorders, psychiatric disorders and disobedience.[39] Jerking movements/lack of motor control, pedaling, pelvic thrusting, lapses in cognitive functioning and other hallmark symptoms of frontal lobe epileptic seizures all create dangerous behavior behind the wheel.[36] Studies have not been done to date to determine the differential risk posed by drivers with frontal lobe epilepsy relative to the general epileptic population.
- Hormones and pregnancy issues
- Hormonal changes and pregnancy can shift seizure activity and the use of antiepileptic drugs can alter the efficacy of hormones as well as cause congenital malformations in fetuses.[40] Seizure control in pregnant women is very important to the welfare of both the developing fetus and the mother. Hormonal shifts at puberty, with birth control and at menopause can also cause changes in the frequency and severity of seizures and must be closely monitored. Increased seizure activity is reported by 50% of women during the course of the pregnancy due to changing levels of hormones, fluids, salts and absorption and elimination of medications.[40]
- Employment
- A report by the Epilepsy Foundation noted that the unemployment rate amongst people with epilepsy is 25% and in patients whose seizures are poorly controlled the rate jumps to 50%.[41] Even though people with epilepsy are protected under The Americans with Disabilities Act, employment discrimination and high rates of unemployment due to employer attitudes still exist.[41] A study in the UK showed that 16% of employers surveyed felt there were no jobs in their company suitable for people with epilepsy and that 21% felt that employing an epileptic would be a “major issue”. Fifty percent of the employers said they had a high concern regarding employing people with epilepsy with most citing safety concerns/workplace accidents as their major issue.[42] Patients with frontal lobe epilepsy may be particularly prone to being discriminated against in employment and subject to higher rates of termination due to the unusual motor symptoms, speech, vocal outbursts and cognitive/judgment symptoms displayed during frontal lobe seizures.[42] Frontal lobe seizures also tend to come on suddenly and progress rapidly making it difficult for an employer to control the exposure of the seizure to others.
- Education, learning and cognitive function
- Patients with frontal lobe epilepsy will likely also experience issues with learning and education. Many factors contribute to these issues including the impact of anticonvulsant medications. Anticonvulsant medications cause patients to feel “foggy” and sluggish. Drugs such as Topiramate cause problems such as mental blunting, word retrieval difficulties and irritability. Phenobarbital, Primidone and Vigabatrin can cause depression and suicidal tendencies.[43] Stress and lack of sleep during exam periods can trigger seizures and many school sports teams restrict or ban people with epilepsy from sports for safety and liability reasons. Frontal lobe epilepsy sufferers also exhibit dysfunctional cognitive skills and memory issues which can make learning challenging. Research has shown that frontal lobe epilepsy has a greater negative impact than other forms of epilepsy on cognitive functioning. People with frontal lobe epilepsy show decreased cognitive capabilities in the following areas: humor appreciation, recognition of emotional expressions, response selection/initiation and inhibition, hyperactivity, conscientiousness, obsession, addictive behavior, motor coordination and planning, attention span, performance speed, continuous performance without intrusion and interference errors, copying and recall, concept formation, anticipatory behavior, memory span, working memory, executive planning, visuo-spatial organization, mental flexibility, conceptual shift, problem solving, programming of complex motor sequences, impulse control, judgment and forecasting of consequences.[16][44][45][46]
- Physical health and risk of other conditions
- Patients with epilepsy face a greater risk of accidents, injury and other medical conditions than the general population.[43] A European study showed that people with epilepsy were at greater risk for accidental injuries related to seizures such as concussions, abrasions and wounds and reported more hospitalizations and medical action than the general population.[47] Other studies have shown that people with epilepsy are at a greater risk of seizure related drowning, suffocation, broken bones and burns and more likely to die in a fatal automobile crash.[48]
- Epilepsy Ontario reports that people with epilepsy are also more likely to have other conditions than the general population such as: 30% of autistic children have epilepsy, 33% of cerebral palsy patients have epilepsy, 15-20% of fragile X syndrome patients have epilepsy, 50% of children with learning disabilities will have some form of epilepsy, 3-10% of patients with Lennox-Gastaut syndrome will have epilepsy, 80% of children with Rett syndrome will have epilepsy and 80% of patients with Tuberous Sclerosis will have epilepsy.[49]
- The frontal lobe has a significant function in attention regulation. Therefore, patients with frontal lobe epilepsy are often found to be co-morbid for another disease called attention-deficit hyperactivity disorder (ADHD), which has a higher prevalence in children. This adds to the various cognitive and behavioral challenges, that they already face.[50]
- Mental and emotional health
- Epileptic patients are more prone to suffer psychological and social dysfunction than individuals that do not have epilepsy. They report higher levels of anxiety and stress due to social isolation, discrimination, the unpredictability of their seizures and people's reactions to them as well as fear of injury, death and brain damage from their seizures. Anticonvulsants can also result in lower functioning, depression, sluggishness and suicidal thoughts. Approximately 20% of people with epilepsy are depressed and the rate of suicide amongst people with epilepsy is 5 times the rate in the general population.[51]
- People with frontal lobe epilepsy experience more significant social effects because the manifested symptoms are more unusual. Symptoms such as screaming, bicycling limbs, pelvic thrusting, inhibition control and other outbursts can be particularly embarrassing and isolating for the patient.[51]
- The ultimate result from all these, is a significant impact on overall personality development.
Research
Over the past decade or so, researchers have been attempting to discover less invasive, safer and more efficient technologies that enable surgeons to remove epileptogenic focal zones without causing any damage to neighboring cortical areas. One such technology that has emerged and has great promise, is the use of gamma knife radiosurgery to either excise a brain tumor or repair a vascular malformation.[52]
In Gamma Knife radiosurgery, intersecting gamma radiation beams are applied directly to the tumor site or vascular malformation site that had been established using neuroimaging.[52] Although each beam itself is not strong enough to damage brain tissue, when the beams intersect they are strong enough to destroy the specific brain tissue that is to be excised. This process is extremely efficient and entirely non-invasive and is therefore much safer than actual neurosurgery itself.
Recently researchers and surgeons alike have begun to use Gamma Knife radiosurgery to treat cases of epilepsy by removing tumors responsible for causing the seizures.[53][54] The early success rates in being able to alleviate seizures seem to be similar to those of temporal resective surgery however Gamma Knife radiosurgery has less associated risk factors.[54] Current research on this topic is aimed at improving the technique in order to increase success rates as well as developing non-invasive forms of physiologic monitoring in order to determine the epileptogenic focus conclusively.[54]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 "Frontal lobe seizure". www.epilepsydiagnosis.org. Archived from the original on 13 December 2022. Retrieved 10 September 2023.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 Panayiotopoulos C (2005). "Symptomatic and Probably Symptomatic Focal Epilepsies: Topographical Symptomatology and Classification". The Epilepsies. Blandon Medical Publishing. Bladon Medical. Archived from the original on 2022-03-27. Retrieved 2022-03-25.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Beleza, P; Pinho, J (May 2011). "Frontal lobe epilepsy". Journal of clinical neuroscience : official journal of the Neurosurgical Society of Australasia. 18 (5): 593–600. doi:10.1016/j.jocn.2010.08.018. PMID 21349720.
- ↑ 4.0 4.1 Fiest, KM; Sauro, KM; Wiebe, S; Patten, SB; Kwon, CS; Dykeman, J; Pringsheim, T; Lorenzetti, DL; Jetté, N (17 January 2017). "Prevalence and incidence of epilepsy: A systematic review and meta-analysis of international studies". Neurology. 88 (3): 296–303. doi:10.1212/WNL.0000000000003509. PMID 27986877.
- ↑ 5.0 5.1 McGonigal, Aileen (10 January 2022). "Frontal lobe seizures: overview and update". Journal of Neurology. doi:10.1007/s00415-021-10949-0. ISSN 1432-1459. PMID 35006387. Archived from the original on 25 March 2022. Retrieved 25 March 2022.
- ↑ 6.0 6.1 Baulac, Michel (December 2018). "History of frontal lobe seizures". Revue Neurologique. 174 (10): 742. doi:10.1016/j.neurol.2018.09.010.
- ↑ 7.0 7.1 "Frontal lobe seizures: Symptoms". Diseases and Conditions. Mayoclinic.com. 2008-10-11. Archived from the original on 2008-09-13. Retrieved 2009-10-17.
- ↑ 8.0 8.1 Kramer U, Riviello JJ, Carmant L, Black PM, Madsen J, Holmes GL (February 1997). "Clinical characteristics of complex partial seizures: a temporal versus a frontal lobe onset". Seizure. 6 (1): 57–61. doi:10.1016/S1059-1311(97)80054-4. PMID 9061825. S2CID 18313275.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 Kellinghaus, Christoph; Luders, Hans (December 2004). "Frontal Lobe Epilepsy". Epileptic Disorders. john-libbey-eurotext.com. 6 (4): 223–239. PMID 15634619. Archived from the original on 2018-04-05. Retrieved 2009-11-29.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 10.13 10.14 10.15 Haut S (7 May 2009). "Frontal Lobe Epilepsy". eMedicine Neurology. Archived from the original on 9 March 2021. Retrieved 5 May 2009.
- ↑ 11.00 11.01 11.02 11.03 11.04 11.05 11.06 11.07 11.08 11.09 11.10 11.11 "Frontal Lobe Seizure: What Is It, Symptoms, Causes & Treatment". Cleveland Clinic. Archived from the original on 2022-07-22. Retrieved 2022-09-30.
- ↑ 12.0 12.1 "All About Frontal Lobe Epilepsy (FLE)". Healthline. 17 December 2021. Archived from the original on 27 April 2022. Retrieved 30 September 2022.
- ↑ Luppino G, Rizzolatti G (October 2000). "The Organization of the Frontal Motor Cortex". News in Physiological Sciences. 15 (5): 219–224. doi:10.1152/physiologyonline.2000.15.5.219. PMID 11390914. Archived from the original on 2013-01-13.
- ↑ 14.0 14.1 "The Motor Cortex". The Brain from Top to Bottom. thebrain.mcgill.ca. Archived from the original on 2015-12-07. Retrieved 2009-12-06.
- ↑ Lesser RP, Lueders H, Dinner DS, Hahn J, Cohen L (March 1984). "The location of speech and writing functions in the frontal language area. Results of extraoperative cortical stimulation". Brain. 107 (1): 275–91. doi:10.1093/brain/107.1.275. PMID 6697159.
- ↑ 16.0 16.1 16.2 Helmstaedter C (October 2001). "Behavioral Aspects of Frontal Lobe Epilepsy". Epilepsy & Behavior. 2 (5): 384–395. doi:10.1006/ebeh.2001.0259. PMID 12609276. S2CID 22256219.
- ↑ Damasio AR, Tranel D, Damasio H (December 1990). "Individuals with sociopathic behavior caused by frontal damage fail to respond autonomically to social stimuli". Behavioural Brain Research. 41 (2): 81–94. doi:10.1016/0166-4328(90)90144-4. PMID 2288668. S2CID 1365170.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 Nair, S; Szaflarski, JP (February 2020). "Neuroimaging of memory in frontal lobe epilepsy". Epilepsy & Behavior. 103 (Pt A): 106857. doi:10.1016/j.yebeh.2019.106857. PMID 31937510. S2CID 210153584.
- ↑ Kurahashi, H; Hirose, S; Adam, MP; Mirzaa, GM; Pagon, RA; Wallace, SE; Bean, LJH; Gripp, KW; Amemiya, A (1993). "Autosomal Dominant Nocturnal Frontal Lobe Epilepsy". PMID 20301348.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 20.0 20.1 Kurahashi, H; Hirose, S; Adam, MP; Mirzaa, GM; Pagon, RA; Wallace, SE; Bean, LJH; Gripp, KW; Amemiya, A (1993). "Autosomal Dominant Nocturnal Frontal Lobe Epilepsy". PMID 20301348.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Milligan, Carol J.; Li, Melody; Gazina, Elena V.; Heron, Sarah E.; Nair, Umesh; Trager, Chantel; Reid, Christopher A.; Venkat, Anu; Younkin, Donald P.; Dlugos, Dennis J.; Petrovski, Slavé; Goldstein, David B.; Dibbens, Leanne M.; Scheffer, Ingrid E.; Berkovic, Samuel F.; Petrou, Steven (April 2014). "KCNT1 gain of function in 2 epilepsy phenotypes is reversed by quinidine: KCNT1 and Human Epilepsy". Annals of Neurology. 75 (4): 581–590. doi:10.1002/ana.24128. PMC 4158617. PMID 24591078.
- ↑ Provini, F. (1 June 1999). "Nocturnal frontal lobe epilepsy: A clinical and polygraphic overview of 100 consecutive cases". Brain. 122 (6): 1017–1031. doi:10.1093/brain/122.6.1017. PMID 10356056.
- ↑ ePainAssist Team (17 January 2017). "Frontal Lobe Seizures or Epilepsy|Causes|Symptoms|Treatment|Recovery|Prevention". ePainAssist. Archived from the original on 29 January 2022. Retrieved 10 February 2022.
- ↑ Schachter SC, Shafer PO (2008-03-28). "Treatment". epilepsy.com. Archived from the original on 2009-10-28. Retrieved 2009-10-24.
- ↑ Weiner HL (2004-03-08). "Treatment". epilepsy.com. Archived from the original on 2009-10-28. Retrieved 2009-10-24.
- ↑ "Epilepsy: Multiple Subpial Transection (MST)". Medicinenet.com. Archived from the original on 2009-11-28. Retrieved 2009-10-23.
- ↑ "Vagus nerve stimulation". MayoClinic.com. 2008-07-31. Archived from the original on January 13, 2010. Retrieved 2009-10-24.
- ↑ "Frontal lobe seizures - Diagnosis and treatment - Mayo Clinic". www.mayoclinic.org. Archived from the original on 2022-02-02. Retrieved 2022-03-25.
- ↑ 29.0 29.1 "Ketogenic Diet". Epilepsy Action. Archived from the original on 2009-12-16. Retrieved 2009-10-24.
- ↑ Glass J (2009-09-16). "Understanding Epilepsy and Seizures". WebMD. Archived from the original on 2022-03-23. Retrieved 2022-03-25.
- ↑ Waterman K, Wada J (1991). "Frontal lobe epilepsy". In Gram L, Dam M (eds.). Comprehensive epileptology. New York: Raven Press. pp. 197–213. ISBN 978-0-88167-646-4.
- ↑ "Living With Epilepsy". Epilepsy foundation.org. Archived from the original on 2011-08-05. Retrieved 2009-12-01.
- ↑ "Wellness and Quality of Life Kit". epilepsyontario.org. Archived from the original on 2009-12-01. Retrieved 2009-12-01.
- ↑ Strine TW, Kobau R, Chapman DP, Thurman DJ, Price P, Balluz LS (July 2005). "Psychological distress, comorbidities, and health behaviors among U.S. adults with seizures: results from the 2002 National Health Interview Survey". Epilepsia. 46 (7): 1133–9. doi:10.1111/j.1528-1167.2005.01605.x. PMID 16026567.
- ↑ 36.0 36.1 36.2 36.3 Krauss GL, Ampaw L, Krumholz A (November 2001). "Individual state driving restrictions for people with epilepsy in the US". Neurology. 57 (10): 1780–5. doi:10.1212/wnl.57.10.1780. PMID 11723263. S2CID 23187968.
- ↑ Sheth SG, Krauss G, Krumholz A, Li G (September 2004). "Mortality in epilepsy: driving fatalities vs other causes of death in patients with epilepsy". Neurology. 63 (6): 1002–7. doi:10.1212/01.wnl.0000138590.00074.9a. PMID 15452290. S2CID 23183235.
- ↑ Richards KC (September 2004). "Patient page. The risk of fatal car crashes in people with epilepsy". Neurology. 63 (6): E12–3. doi:10.1212/01.WNL.0000142227.69091.D0. PMID 15452331.
- ↑ "Driving". Epilepsy.com. Retrieved 2009-12-01.
- ↑ 40.0 40.1 "Women and Epilepsy". Acta Neurologica Scandinavica. Retrieved 2009-12-01.[dead link]
- ↑ 41.0 41.1 "Epilepsy as a Disability". epilepsyfoundation.org. Archived from the original on 2012-12-13. Retrieved 2013-02-22.
- ↑ 42.0 42.1 Jacoby A, Gorry J, Baker GA (December 2005). "Employers' attitudes to employment of people with epilepsy: still the same old story?". Epilepsia. 46 (12): 1978–87. doi:10.1111/j.1528-1167.2005.00345.x. PMID 16393165.
- ↑ 43.0 43.1 Blum D (1999). "Total Impact of Epilepsy: Biological, Psychological, Social and Economic Aspects". Barrow Quarterly. Archived from the original on 2011-07-16. Retrieved 2009-12-01.
- ↑ Patrikelis P, Angelakis E, Gatzonis S (January 2009). "Neurocognitive and behavioral functioning in frontal lobe epilepsy: a review". Epilepsy & Behavior. 14 (1): 19–26. doi:10.1016/j.yebeh.2008.09.013. PMID 18926928. S2CID 12381094.
- ↑ Helmstaedter C, Kemper B, Elger CE (May 1996). "Neuropsychological aspects of frontal lobe epilepsy". Neuropsychologia. 34 (5): 399–406. doi:10.1016/0028-3932(95)00121-2. PMID 9148196. S2CID 46365124.
- ↑ Farrant A, Morris RG, Russell T, et al. (November 2005). "Social cognition in frontal lobe epilepsy". Epilepsy & Behavior. 7 (3): 506–16. doi:10.1016/j.yebeh.2005.07.018. PMID 16165399. S2CID 23417742.
- ↑ van den Broek M, Beghi E (June 2004). "Accidents in patients with epilepsy: types, circumstances, and complications: a European cohort study". Epilepsia. 45 (6): 667–72. doi:10.1111/j.0013-9580.2004.33903.x. PMID 15144432. S2CID 5927958.
- ↑ Mayes BN (February 2009). "Review: people with epilepsy have higher risk of death by drowning than the general population". Evidence-Based Medicine. 14 (1): 21. doi:10.1136/ebm.14.1.21. PMID 19181953.
- ↑ "Other Conditions". epilepsyontario.org. Retrieved 2009-12-01.[dead link]
- ↑ Williams, Amy E; Giust, Julianne M; Kronenberger, William G; Dunn, David W (9 February 2016). "Epilepsy and attention-deficit hyperactivity disorder: links, risks, and challenges". Neuropsychiatric Disease and Treatment: 287–296. doi:10.2147/NDT.S81549. PMC 4755462. PMID 26929624.
- ↑ 51.0 51.1 "Mental Health". epilepsyontario.org. Retrieved 2009-12-01.[dead link]
- ↑ 52.0 52.1 "Gamma-Knife Radiosurgery". mayoclinic.com. 2008-10-08. Archived from the original on 2008-11-20. Retrieved 2009-12-03.
- ↑ Vojtech Z, Vladyka V, Kalina M, et al. (September 2009). "The use of radiosurgery for the treatment of mesial temporal lobe epilepsy and long-term results". Epilepsia. 50 (9): 2061–71. doi:10.1111/j.1528-1167.2009.02071.x. PMID 19400872.
- ↑ 54.0 54.1 54.2 "Gamma Knife Radiosurgery for Epilepsy". University of Virginia School of Medicine. 2007-10-11. Archived from the original on 2008-10-10. Retrieved 2009-12-03.
External links
- Pages with script errors
- CS1 errors: missing periodical
- All articles with dead external links
- Articles with dead external links from May 2016
- Articles with invalid date parameter in template
- All articles with unsourced statements
- Articles with unsourced statements from March 2017
- Articles with hatnote templates targeting a nonexistent page
- Epilepsy types
- Seizure types
- Frontal lobe
- RTT
- RTTILAE