Fournier gangrene
| Fournier gangrene | |
|---|---|
| Other names: Fournier's gangrene | |
 | |
| An area of skin death of the scrotum | |
| Specialty | Infectious disease, urology |
| Symptoms | Initially none specific, scrotum or labia pain and swelling, fever, redness[1] |
| Complications | Sepsis[2] |
| Usual onset | Rapid[1] |
| Causes | Infection, often by multiple types of bacteria[3] |
| Risk factors | Diabetes, alcoholism, immunocompromised, long term urinary catheters[3][2] |
| Diagnostic method | Based on symptoms, may be supported by medical imaging[3] |
| Treatment | Antibiotics, surgical removal of infected tissue, supportive care[3] |
| Prognosis | Guarded[1] |
| Frequency | 1 per 62,500 males a year[2] |
| Deaths | High risk[3] |
Fournier gangrene (FG) is a type of necrotizing fasciitis affecting the perineum.[3][2] Initial symptoms are often non specific; though rapidly worsen.[1] This may include scrotum or labia pain and swelling, fever, and redness.[1] The infection spreads at about 2.5 cm per hour.[1] Complications may include sepsis.[2]
Risk factors include diabetes, alcoholism, being immunocompromised, an long term urinary catheters.[3][2] In diabetes sodium-glucose co-transporter-2 inhibitors (SGLT2 inhibitors) may be a particular risk.[1] Infection is by multiple types of bacteria in more than 80% of cases.[3] Often the infection spreads from the gastrointestinal tract, urinary tract, or skin.[4] Diagnosis is based on symptoms and may be supported by medical imaging.[3]
Treatment involves antibiotics, surgical removal of infected tissue, and supportive care.[3] Other options may include hyperbaric oxygen therapy and negative-pressure wound therapy.[1] The risk of death is high at 20 to 80%, though varies based on other health problems.[1][3] In those who survive reconstructive surgery is required.[1]
Fournier gangrene affects about one per 62,500 males per year.[2] Older people and males are more commonly affected with males affected 40 times more often than females.[2] It was first described by Baurienne in 1764 and is named after Jean Alfred Fournier, following five cases he presented in 1883.[4]
Signs and symptoms
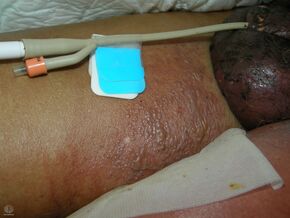
Initial symptoms include swelling or sudden pain in the scrotum, fever, pallor, and generalized weakness. It is characterized by pain that extends beyond the border of the redness.[4]
Most cases begin mildly, but can progress in hours. Subcutaneous air is one of the specific signs, but is not seen in over half of cases. More marked cases are characterized by a foul odor and necrotic infected tissue. Crepitus has been reported.[4]
It begins as a subcutaneous infection. However, necrotic patches soon appear in the overlying skin, which later develop into necrosis.[4]
Cause
Most cases involve infect with both aerobic and anaerobic bacteria such as Clostridium perfringens. It can also result from infections caused by group A streptococcus (GAS), as well as other pathogens such as Staphylococcus aureus and Vibrio vulnificus.[5]
Blood sugar levels are elevated in about half of people.[6] About a third were alcoholic, diabetic, and malnourished, while another ten percent had been immunosuppressed through chemotherapy, steroids, or malignancy.[7]
Fournier gangrene is a recognized side effect of SGLT2 inhibitors (canagliflozin, dapagliflozin, and empagliflozin),[8][9] which result in increased glucose in the urine.
Diagnosis
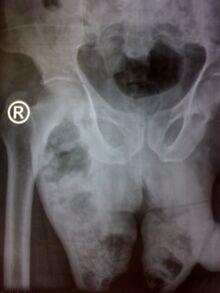
Fournier gangrene is usually diagnosed based on symptoms and examination.[3] Common findings include swelling of the scrotum, fast heart rate, bad smelling discharge, crepitus, and fever.[1]
Laboratory tests and medical imaging may support the diagnosis, determine severity, and predict outcomes.[4] X-rays and ultrasound may show the presence of gas below the surface of the skin.[4] A CT scan can be useful in determining the site of origin and extent of spread.[4]
Treatment
Fournier gangrene is an emergency requiring intravenous antibiotics and debridement (surgical removal of dead tissue).[4] In addition, hyperbaric oxygen therapy may be useful to inhibit the growth of anaerobic bacteria.[10]
Prognosis
Studies have found a mortality rate of 7.5–40%.[11] Rates are as high as 76% in those with sepsis.[3] Lack of access to sanitation, medical care, and psychosocial resources has been linked to increased mortality.[12]
Epidemiology
Fournier gangrene occurs in about 1.6 per 100,000 males, in the United States.[11] Males 50 to 79 years old had the highest rate at 3.3 per 100,000.[11] Of 1,680 cases, 39 were women.[11]
Society and culture
Historically notable cases include Herod the Great, his grandson Herod Agrippa, and possibly the Roman emperor Galerius.[citation needed] Puerto Rican abolitionist and pro-independence leader Segundo Ruiz Belvis died from Fournier gangrene in November 1867.
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 Lewis, GD; Majeed, M; Olang, CA; Patel, A; Gorantla, VR; Davis, N; Gluschitz, S (October 2021). "Fournier's Gangrene Diagnosis and Treatment: A Systematic Review". Cureus. 13 (10): e18948. doi:10.7759/cureus.18948. PMID 34815897.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Hamdy, Freddie C.; Eardley, Ian (2017). Oxford Textbook of Urological Surgery. Oxford University Press. p. 76. ISBN 9780191022524. Archived from the original on 2021-08-28. Retrieved 2021-06-15.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 El-Qushayri, AE; Khalaf, KM; Dahy, A; Mahmoud, AR; Benmelouka, AY; Ghozy, S; Mahmoud, MU; Bin-Jumah, M; Alkahtani, S; Abdel-Daim, MM (March 2020). "Fournier's gangrene mortality: A 17-year systematic review and meta-analysis". International journal of infectious diseases : IJID : official publication of the International Society for Infectious Diseases. 92: 218–225. doi:10.1016/j.ijid.2019.12.030. PMID 31962181.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 Mallikarjuna, MN; Vijayakumar, A; et al. (2012). "Fournier's gangrene: Current practices". ISRN Surgery. 2012: 942437. doi:10.5402/2012/942437. PMC 3518952. PMID 23251819.
- ↑ Thwaini, A; Khan, A; et al. (2006). "Fournier's gangrene and its emergency management". Postgrad Med J. 82 (970): 516–9. doi:10.1136/pgmj.2005.042069. PMC 2585703. PMID 16891442.
- ↑ Yanar, H; Taviloglu, K; et al. (2006). "Fournier's gangrene: Risk factors and strategies for management". World J Surg. 30 (9): 1750–4. doi:10.1007/s00268-005-0777-3. PMID 16927060. S2CID 32207714.
- ↑ Tahmaz, L; Erdemir, F; et al. (2006). "Fournier's gangrene: Report of thirty-three cases and a review of the literature". Int J Urol. 13 (7): 960–7. doi:10.1111/j.1442-2042.2006.01448.x. PMID 16882063. S2CID 10161279.
- ↑ "FDA warns about rare occurrences of a serious infection of the genital area with SGLT2 inhibitors for diabetes". www.fda.gov. Center for Drug Evaluation and Research. 7 September 2018. p. Drug Safety and Availability. Archived from the original on 7 February 2019. Retrieved 16 April 2019.
- ↑ Bersoff-Matcha SJ, Chamberlain C, Cao C, Kortepeter C, Chong WH (June 4, 2019). "Fournier Gangrene Associated With Sodium–Glucose Cotransporter-2 Inhibitors: A Review of Spontaneous Postmarketing Cases". Ann Intern Med. 170 (11): 764–769. doi:10.7326/M19-0085. PMID 31060053.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Zamboni, WA; Riseman, JA; Kucan, JO (1990). "Management of Fournier's gangrene and the role of hyperbaric oxygen". J. Hyperbaric Med. 5 (3): 177–86. Archived from the original on 2011-02-03. Retrieved 2008-05-16.
- ↑ 11.0 11.1 11.2 11.3 Sorensen, MD; Krieger, JN; et al. (2009). "Fournier's gangrene: Population based epidemiology and outcomes". The Journal of Urology. 181 (5): 2120–6. doi:10.1016/j.juro.2009.01.034. PMC 3042351. PMID 19286224.
- ↑ Kessler, CS; Bauml, J (November 2009). "Non-Traumatic Urologic Emergencies in Men: A Clinical Review". West J Emerg Med. 10 (4): 281–7. PMC 2791735. PMID 20046251.
External links
| Classification | |
|---|---|
| External resources |