Extramammary Paget's disease
| Extramammary Paget's disease | |
|---|---|
 | |
| Extensive Invasive Extramammary Paget Disease | |
| Specialty | Dermatology, Oncology |
| Symptoms | Rash, Itchiness, Eczematous lesions, Pain |
| Causes | Unknown |
| Diagnostic method | Excisional biopsy, histological pattern |
Extramammary Paget’s Disease (EMPD), is a rare and slow-growing malignancy which occurs within the epithelium[1] and accounts for 6.5% of all Paget’s disease.[2] The clinical presentation of this disease is similar to the characteristics of mammary Paget’s disease (MPD).[3] However, unlike MPD, which occurs in large lactiferous ducts and then extends into the epidermis,[3] EMPD originates in glandular regions rich in apocrine secretions outside the mammary glands.[4] EMPD incidence is increasing by 3.2% every year, affecting hormonally-targeted tissues such as the vulva and scrotum.[5] In women, 81.3% of EMPD cases are related to the vulva, while for men, 43.2% of the manifestations present at the scrotum.[5]
The disease can be classified as being either primary or secondary depending on the presence or absence of associated malignancies.[6] EMPD presents with typical symptoms such as scaly, erythematous, eczematous lesions accompanied by itchiness.[6] In addition to this, 10% of patients are often asymptomatic.[7] As a consequence, EMPD has high rates of misdiagnoses and delayed diagnoses.[8] There are a variety of treatment options available, but most are unsuccessful. If caught early and treated, prognosis is generally good.
Signs and symptoms
Patients with EMPD present with typical symptoms, similar to MPD,[3] such as severe itchiness (also called pruritus), rash, plaque formation, burning sensation, pain and tenderness.[7] These symptoms are often confused for dermatitis or eczema.[8] 10% of patients are asymptomatic resulting in delayed diagnosis.[7] In rare cases bleeding can also be seen.[9]
| Skin |
|
| Discharge |
|
| Sensation |
|
Disease of the vulva
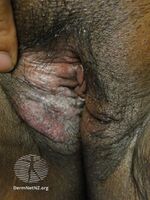
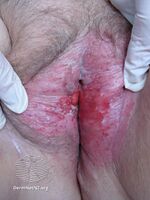
Vulvar Paget's disease affects both sexes and presents as erythematous (red), eczematous lesions.[10] It is itchy and sometimes pain can be associated with the affected area.[10] The lesion is clearly separated from normal skin in most cases, and sometimes scattered areas of white scale can be present, giving a "strawberries and cream" appearance.[11]
Involvement may be extensive including the perianal region, genitocrural, and inguinal folds. Clinical examination should determine the presence of periurethral and perianal lesions.[12] In these cases an involvement of the skin by a noncutaneous internal neoplasm may occur.[12]
-
Extramammary Paget disease of the skin of the vulva
-
Extramammary Paget disease of the skin of the vulva
-
Extramammary Paget disease of the skin of the vulva
Pathophysiology
EMPD occurs due to an invasion of the epidermis by Paget cells.[2] The cause of the disease is still under debate with recent research indicating that the disease may be associated with Toker cells.[13]
-
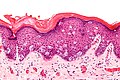
Micrograph of extramammary Paget's disease, H&E stain
-
H&E stained micrograph of Extramammary Paget's disease, showing Paget cells infiltrating the epidermis
Disease of the vulva
Originates from local organs such as the Bartholin gland, the urethra, or the rectum.[14] Predilection towards postmenopausal women.[14]
Metastatic disease
Metastasis of Paget cells from the epidermis to distant regions is a multistep process that involves:
- Invasion of local lymph nodes and venous system[4]
- Movement out from lymph nodes and venous system[4]
- Proliferation at new site[4]
Protein molecules HER2 and mTOR expressed in Paget cells are responsible for providing characteristics of proliferation and survival.[4]
Diagnosis
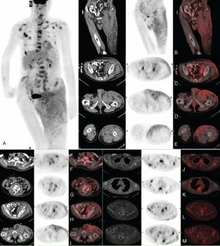
A Case Report |thumb|right|Due to the rarity of EMPD and lack of clinical knowledge, the disease is not very commonly diagnosed.[8] Patients are often misdiagnosed with eczema or dermatitis[8] and a delay of 2 years is expected from the onset of symptoms before a definitive diagnosis has been reached.[8]
It is important to include that the lesion is associated with another cancer. A biopsy will establish the diagnosis. Punch biopsies are not effective in differentially diagnosing for EMPD and as a result, excisional biopsies of the affected area are taken [XX]. A positive test result for EMPD shows increased numbers of large polygonal cells with a pale bluish cytoplasm, large nucleus and nucleolus, infiltrating the epidermal layer.[7] These neoplastic cells can be found singly scattered or can appear in groups called nests.[7]
Paget cells contain mucin and cytokeratins which can be used in the diagnosis of EMPD [8] MUC5A2 is found in EMPD of the vulvar and male genitalia regions whereas MUC2 is expressed in perianal EMPD. Loss of MUC5A2 can indicate an invasive spread.[15] Immunohistochemistry (IHC) can be used to determine whether EMPD is either primary or secondary.[15] Primary EMPD tests positive for CK7 but negative for CK20, whereas secondary is positive for both.[15] Lack of positivity for hormone receptors and HER2 protein is overexpressed meaning that the cells are dividing rapidly and can be indicate an aggressive and more recurrent disease.[citation needed]
Classification
Primary EMPD is of cutaneous origins and is found within the epidermis or the underlying apocrine glands.[1] Although it is limited to the epithelium, it has potential to spread and progress into an invasive tumour, metastasising to the local lymph nodes and distant organs.[6] This form of EMPD is not associated with an adenocarcinoma.[1]
The secondary form results due to an underlying adenocarcinoma spreading to the epidermis.[15] Similar to the primary form, if secondary EMPD invades the dermis, the neoplastic cells can metastasise to the lymph nodes and in some cases, the dermis.[4]
According to the Wilkinson and Brown subclassification system, there are 3 subtypes for each classification.[16]
| Primary (cutaneous) | Secondary (non-cutaneous) |
|---|---|
| Intraepithelial cutaneous Paget disease of the usual type | Anorectal |
| Intraepithelial cutaneous Paget disease with invasion | Urothelial |
| Intraepithelial cutaneous Paget disease as a manifestation of underlying
adenocarcinoma of skin appendage |
Other |
Treatment
Many chemotherapy treatments have been used, however the results are not desirable as prognosis remains to be poor.[16] Surgery remains to be the preferred treatment of choice. Wide local excision with a 3cm margin and intra-operative frozen sections are suggested, due to high risk of local extension despite normal appearing tissue. However, in cases where the Paget cells have invaded into the dermis, and metastasised complete removal of is unsuccessful, meaning that recurrence is common.[15] Lymphadenoectomy is often performed for infiltrative cases.[16] In lieu of surgery, radiotherapy is also an option and is especially preferred for elderly patients or for inoperable cases where the tumour size if too large.[6] This form of treatment is also considered as possible adjuvant therapy following excision to combat the high recurrence rate.[2] However, there are side effects of radiotherapy, including but not limited to: vulvitis, post-radiation atrophy of mucus membranes, vaginal stenosis and sexual dysfunction.[2]
Laser therapy and photodynamic therapies were also used in the past, but it was discovered the carbon dioxide laser did not penetrate deep enough and both treatment modalities resulted in high rate recurrence rates.[2]
Topical chemotherapy treatments are effective, with imiquimod showing promising results.[2] However, overall survival begins to decline 10 months following treatment with chemotherapy.[4] Patients suffering from metastatic EMPD only survive for a median of 1.5 years, and have a 7% 5-year survival rate.[4]
Prognosis
Prognosis is generally good, but factors such as depth of invasion and duration of disease need to be considered.[16] In primary EMPD, if invasion of the underlying tissue is non-existent or even minimal, treatment options are more likely to be effective, however, if there are signs that the disease has metastasised, the prognosis is usually poor.[3]
Epidemiology
EMPD is most prevalent in Caucasian women and Asian men over the age of 60.[9] The invasive form occurs in 5-25% of all EMPD patients and 17-30% of the cases involve an underlying adenocarcinoma.[16] 10-20% of EMPD is of the secondary form.[16] Approximately 10% of patients develop invasive adenocarcinoma that may progress to metastatic disease.[17]
The disease affects regions that are rich in apocrine secretions.[4] 65% EMPD occurs at the vulva,[15] followed by 15% at perianal areas and 14% at the male genitalia.[2] In terms of the vulva, the labia majora is the site that is most often involved, followed by labia minora, clitoris and perineum.[16] EMPD originating at the vulva can spread to the upper vaginal mucosa and cervix.[16] Other areas where EMPD can be found, although very rarely, include: the axillae, eyelids, external auditory canal, umbilical region, trunk and extremities.[2]
History
The first case of Paget’s disease was described by James Paget in 1874.[3] Radcliffe Crocker, in 1889, then described EMPD following an observation of a patient with urinary carcinoma affecting the penis and scrotum,[18] showing symptoms that were almost identical to MPD as described by Paget.[6] Later in 1893, Darier and Coulillaud described the perianal location of EMPD.[6]
References
- ↑ 1.0 1.1 1.2 Isrow D, Oregel KZ, Cortes J, Gomez H, Milikowski C, Feun L, Silva O (2014-07-06). "Advanced Extramammary Paget's Disease of the Groin, Penis, and Scrotum". Clinical Medicine Insights: Oncology. 8: 87–90. doi:10.4137/CMO.S13107. PMC 4116380. PMID 25089091.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Wagner G, Sachse MM (June 2011). "Extramammary Paget disease - clinical appearance, pathogenesis, management". Journal der Deutschen Dermatologischen Gesellschaft. 9 (6): 448–54. doi:10.1111/j.1610-0387.2010.07581.x. PMID 21205169.
- ↑ 3.0 3.1 3.2 3.3 3.4 Lloyd J, Flanagan AM (October 2000). "Mammary and extramammary Paget's disease". Journal of Clinical Pathology. 53 (10): 742–9. doi:10.1136/jcp.53.10.742. PMC 1731095. PMID 11064666.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 Fukuda K, Funakoshi T (2018-02-16). "Metastatic Extramammary Paget's Disease: Pathogenesis and Novel Therapeutic Approach". Frontiers in Oncology. 8: 38. doi:10.3389/fonc.2018.00038. PMC 5820294. PMID 29503810.
- ↑ 5.0 5.1 Zhou S, Zhong W, Mai R, Zhang G (2017). "Mammary and Extramammary Paget's Disease Presented Different Expression Pattern of Steroid Hormone Receptors". BioMed Research International. 2017: 3768247. doi:10.1155/2017/3768247. PMC 5610822. PMID 29082243.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Lopes Filho LL, Lopes IM, Lopes LR, Enokihara MM, Michalany AO, Matsunaga N (April 2015). "Mammary and extramammary Paget's disease". Anais Brasileiros de Dermatologia. 90 (2): 225–31. doi:10.1590/abd1806-4841.20153189. PMC 4371672. PMID 25830993.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 Konda S, Chen W, Minus HR (March 2015). "What is your diagnosis? Extramammary Paget disease". Cutis. 95 (3): 132, 135–6, 142. PMID 25844784.
- ↑ 8.0 8.1 8.2 8.3 8.4 Hsu L, Shen Y, Chen C, Sung M, Chiang P (March 2013). "Extramammary Paget's disease with invasive adenocarcinoma of the penoscrotum: Case report and systematic review". Urological Science. 24 (1): 30–33. doi:10.1016/j.urols.2013.01.003. ISSN 1879-5226.
- ↑ 9.0 9.1 Kang Z, Zhang Q, Zhang Q, Li X, Hu T, Xu X, Wu Z, Zhang X, Wang H, Xu J, Xu F, Guan M (2015). "Clinical and pathological characteristics of extramammary Paget's disease: report of 246 Chinese male patients". International Journal of Clinical and Experimental Pathology. 8 (10): 13233–40. PMC 4680468. PMID 26722523.
- ↑ 10.0 10.1 Anton C, Luiz AV, Carvalho FM, Baracat EC, Carvalho JP (June 2011). "Clinical treatment of vulvar Paget's disease: a case report". Clinics. 66 (6): 1109–11. doi:10.1590/S1807-59322011000600033. PMC 3129957. PMID 21808885.
- ↑ Bolognia J, Jorizzo JL, Schaffer JV (2012). Dermatology. Bolognia, Jean., Jorizzo, Joseph L., Schaffer, Julie V. (3rd ed.). [Philadelphia]: Elsevier Saunders. ISBN 9780702051821. OCLC 802040381.
- ↑ 12.0 12.1 Preti M, Micheletti L, Massobrio M, Ansai S, Wilkinson EJ (April 2003). "Vulvar paget disease: one century after first reported". Journal of Lower Genital Tract Disease. 7 (2): 122–35. doi:10.1097/00128360-200304000-00009. hdl:2318/39322. PMID 17051057. S2CID 41852226.
- ↑ McDaniel, Brianna; Crane, Jonathan S. (2018), "Paget Disease, Extramammary", StatPearls, StatPearls Publishing, PMID 29630276, archived from the original on 2019-12-17, retrieved 2018-06-09
- ↑ 14.0 14.1 Fanning J, Lambert L, Hale TM, Morris PC, Schuerch C (1999). "Paget's disease of the vulva: prevalence of associated vulvar carcinoma, invasive Paget's disease, and recurrence after surgical excision". Am J Obstet Gynecol. 180 (1 Pt 1): 24–7. doi:10.1016/s0002-9378(99)70143-2. PMID 9914572.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 Lam C, Funaro D (October 2010). "Extramammary Paget's disease: Summary of current knowledge". Dermatologic Clinics. 28 (4): 807–26. doi:10.1016/j.det.2010.08.002. PMID 20883922.
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 16.6 16.7 16.8 Londero AP, Bertozzi S, Salvador S, Fruscalzo A, D'Aietti V, Grassi T, Driul L, Mariuzzi L, Marchesoni D (April 2013). "A review of extramammary paget's disease: Clinical presentation, diagnosis, management and prognosis". Journal of Medicine and Medical Sciences. 4 (4): 134–148.
- ↑ "International Classification of Diseases for Oncology". codes.iarc.fr. Archived from the original on 2019-01-21. Retrieved 2018-06-09.
- ↑ Marques-Costa JC, Cuzzi T, Carneiro S, Parish LC, Ramos-e-Silva M (May–Jun 2012). "Paget's disease of the breast". Skinmed. 10 (3): 160–5, quiz 165. PMID 22779098.
External links
- Definition at cancer.org
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- Articles with hatnote templates targeting a nonexistent page
- All articles with unsourced statements
- Articles with unsourced statements from May 2021
- Articles with invalid date parameter in template
- Male genital neoplasia
- Gynaecological cancer
- Epidermal nevi, neoplasms, and cysts
- Rare diseases