Pinworm infection
| Pinworm infection | |
|---|---|
| Other names: Threadworm infection, enterobiasis, oxyuriasis[1] | |
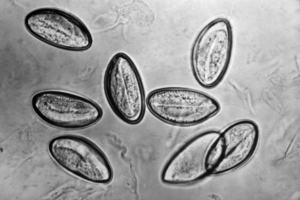 | |
| Pinworm eggs (Enterobius vermicularis) | |
| Specialty | Infectious disease |
| Symptoms | Itchy anal area[1] |
| Usual onset | 4 to 8 weeks from exposure[2] |
| Causes | Pinworms (Enterobius vermicularis)[3] |
| Risk factors | Attending school[1] |
| Diagnostic method | Seeing the worms or eggs[1] |
| Prevention | Handwashing, daily bathing in the morning, daily changing of underwear[1] |
| Medication | Mebendazole, pyrantel pamoate, or albendazole[4] |
| Prognosis | Non serious[5] |
| Frequency | Common[1][5] |
Pinworm infection, also known as enterobiasis and threadworm infection, is a human parasitic disease caused by the pinworm.[3] The most common symptom is itching in the anal area.[1] This can make sleeping difficult.[1] The period of time from swallowing eggs to the appearance of new eggs around the anus is 4 to 8 weeks.[2] Some people who are infected do not have symptoms.[1]
The disease is spread between people by pinworm eggs.[1] The eggs initially occur around the anus and can survive for up to three weeks in the environment.[1] They may be swallowed following contamination of the hands, food, or other articles.[1] Those at risk are those who go to school, live in a health care institution or prison, or take care of people who are infected.[1] Other animals do not spread the disease.[1] Diagnosis is by seeing the worms which are about one centimeter long or the eggs under a microscope.[1][6]
Treatment is typically with two doses of the medications mebendazole, pyrantel pamoate, or albendazole two weeks apart.[4] Everyone who lives with or takes care of an infected person should be treated at the same time.[1] Washing personal items in hot water after each dose of medication is recommended.[1] Good handwashing, daily bathing in the morning, and daily changing of underwear can help prevent reinfection.[1]
Pinworm infections commonly occur in all parts of the world.[1][5] They are the most common type of worm infection in the developed world.[1] School-aged children are the most commonly infected.[1] In the United States about 20% of people at one point in time develop pinworm.[3] Infection rates among high-risk groups may be as high as 50%.[2] It is not considered a serious disease.[5] Pinworms are believed to have affected humans throughout history.[7]
Signs and symptoms
One-third of individuals with pinworm infection are totally asymptomatic.[8] The main symptoms are itching in and around the anus and perineum.[8][9][10] The itching occurs mainly during the night,[9][11] and is caused by the female pinworms migrating to lay eggs around the anus.[12][10] Both the migrating females and the clumps of eggs are irritating, but the mechanisms causing the intense pruritus have not been explained.[11] The intensity of the itching varies, and it can be described as tickling, crawling sensations, or even acute pain.[13] The itching leads to continuously scratching the area around the anus, which can further result in tearing of the skin and complications such as secondary bacterial infections, including bacterial skin inflammation, and hair follicle inflammation.[9][10][13] General symptoms are trouble sleeping, and restlessness.[9] A considerable proportion of children suffer from loss of appetite, weight loss, irritability, emotional instability, and bed wetting.[9]
Pinworms cannot damage the skin,[14] and they do not normally migrate through tissues.[10] However, they may move onto the vulva and into the vagina, from there moving to the external orifice of the uterus, and onwards to the uterine cavity, fallopian tubes, ovaries, and peritoneal cavity.[14] This can cause inflammation of the vulva and vagina.[9][10] This causes vaginal discharge and itchiness of the vulva.[9] The pinworms can also enter the urethra, and presumably, they carry intestinal bacteria with them.[14] According to Gutierrez (2000), a statistically significant correlation between pinworm infection and urinary tract infections has been shown;[14] however, Burkhart & Burkhart (2005) maintain that the incidence of pinworms as a cause of urinary tract infections remains unknown.[8] One report indicated that 36% of young girls with a urinary tract infection also had pinworms.[8] Painful urination has been associated with pinworm infection.[8]
The relationship between pinworm infestation and appendicitis has been researched, but there is a lack of clear consensus on the matter: While Gutierres (2005) maintains that there exists a consensus that pinworms do not produce the inflammatory reaction,[15] Cook (1994) states that it is controversial whether pinworms are causatively related to acute appendicitis,[13] and Burkhart & Burkhart (2004) state that pinworm infection causes symptoms of appendicitis to surface.[8]
Cause

The cause of a pinworm infection is the worm Enterobius vermicularis. The entire lifecycle — from egg to adult — takes place in the human gastrointestinal tract of a single human host.[12][16] This process is two to eight weeks.[17][9]
Spread
Pinworm infection spreads through human-to-human transmission, by swallowing infectious pinworm eggs.[17][18] The eggs are hardy and can remain infectious in a moist environment for up to three weeks,[11][17] though in a warm dry environment they usually last only 1–2 days.[19] They do not tolerate heat well, but can survive in low temperatures: at −8 degrees Celsius (18 °F), two-thirds of the eggs are still viable after 18 hours.[11]
After the eggs have been initially deposited near the anus, they are readily transmitted to other surfaces through contamination.[18] The surface of the eggs is sticky when laid,[12][11] and the eggs are readily transmitted from their initial deposit near the anus to fingernails, hands, night-clothing and bed linen.[9] From here, eggs are further transmitted to food, water, furniture, toys, bathroom fixtures and other objects.[12][17][18] Household pets often carry the eggs in their fur, while not actually being infected.[20] Dust containing eggs can become airborne and widely dispersed when dislodged from surfaces, for instance when shaking out bed clothes and linen.[11][17][20] Consequently, the eggs can enter the mouth and nose through inhalation, and be swallowed later.[9][11][17][18] Although pinworms do not strictly multiply inside the body of their human host,[9] some of the pinworm larvae may hatch on the anal mucosa, and migrate up the bowel and back into the gastrointestinal tract of the original host.[9][17] This process is called retroinfection.[11][17] According to Burkhart (2005), when this retroinfection occurs, it leads to a heavy parasitic load and ensures that the pinworm infestation continues.[17] This statement is contradictory to a statement by Caldwell, who contends that retroinfection is rare and not clinically significant.[11] Despite the limited, 13-week lifespan of individual pinworms,[12] autoinfection (infection from the original host to itself), either through the anus-to-mouth route or through retroinfection, causes the pinworms to inhabit the same host indefinitely.[17]
Life cycle

The life cycle begins with eggs being ingested.[12] The eggs hatch in the duodenum (first part of the small intestine).[18] The emerging pinworm larvae grow rapidly to a size of 140 to 150 micrometers,[9] and migrate through the small intestine towards the colon.[12] During this migration they moult twice and become adults.[12][17] Females survive for 5 to 13 weeks, and males about 7 weeks.[12] The male and female pinworms mate in the ileum (last part of the small intestine),[12] whereafter the male pinworms usually die,[18] and are passed out with stool.[11] The gravid female pinworms settle in the ileum, caecum (beginning of the large intestine), appendix and ascending colon,[12] where they attach themselves to the mucosa[17] and ingest colonic contents.[10] Almost the entire body of a gravid female becomes filled with eggs.[18] The estimations of the number of eggs in a gravid female pinworm ranges from about 11,000[12] to 16,000.[17] The egg-laying process begins approximately five weeks after initial ingestion of pinworm eggs by the human host.[12] The gravid female pinworms migrate through the colon towards the rectum at a rate of 12 to 14 centimeters per hour.[12] They emerge from the anus, and while moving on the skin near the anus, the female pinworms deposit eggs either through (1) contracting and expelling the eggs, (2) dying and then disintegrating, or (3) bodily rupture due to the host scratching the worm.[18] After depositing the eggs, the female becomes opaque and dies.[11] The reason the female emerges from the anus is to obtain the oxygen necessary for the maturation of the eggs.[11]
Diagnosis
Diagnosis depends on finding the eggs or the adult pinworms.[18] Individual eggs are not visible to the naked eye, but they can be seen using a low-power microscope.[20] On the other hand, the light-yellowish thread-like adult pinworms are clearly visually detectable, usually during the night when they move near the anus, or on toilet paper.[8][13][20] Transparent adhesive tape (e.g. Scotch Tape) applied on the anal area will pick up deposited eggs, and diagnosis can be made by examining the tape with a microscope.[15][20] This test is most successful if done every morning for several days, because the females do not lay eggs every day, and the number of eggs vary.[20]
Pinworms do not lay eggs in the feces,[20] but sometimes eggs are deposited in the intestine.[18] As such, routine examination of fecal material gives a positive diagnosis in only 5 to 15% of infected subjects,[13] and is therefore of little practical diagnostic use.[9] In a heavy infection, female pinworms may adhere to stools that pass out through the anus, and they may thus be detected on the surface on the stool.[13][18] Adult pinworms are occasionally seen during colonoscopy.[13] On a microscopic level, pinworms have an identifying feature of alae (i.e., protruding ridges) running the length of the worm.[21]
-
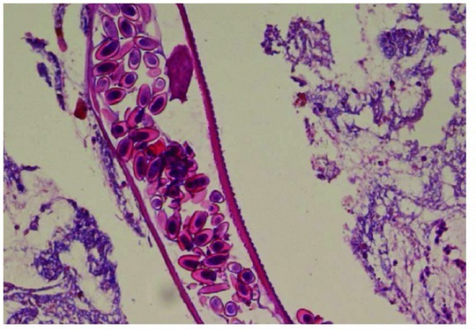
Longitudinal section through the larval stage of female pinworm (with numerous eggs)
-
High magnification micrograph of a pinworm in cross section in the appendix. H&E stain.
Prevention
Pinworm infection cannot be totally prevented under most circumstances.[22] This is due to the prevalence of the parasite and the ease of transmission through soiled night clothes, airborne eggs, contaminated furniture, toys and other objects.[18] Infection may occur in the highest strata of society, where hygiene and nutritional status are typically high.[23] The stigma associated with pinworm infection is hence considered a possible over-emphasis.[23] Counselling is sometimes needed for upset parents who have discovered their children are infected, as they may not realize how prevalent the infection is.[18]
Preventive action revolves around personal hygiene and the cleanliness of the living quarters.[23] The rate of reinfection can be reduced through hygienic measures, and this is recommended especially in recurring cases.[20][23]
The main measures are keeping fingernails short, and washing and scrubbing hands and fingers carefully, especially after defecation and before meals.[23][24] Under ideal conditions, bed covers, sleeping garments, and hand towels should be changed daily.[23] Simple laundering of clothes and linen disinfects them.[23] Children should wear gloves while asleep, and the bedroom floor should be kept clean.[23] Food should be covered to limit contamination with dust-borne parasite eggs.[23] Household detergents have little effect on the viability of pinworm eggs, and cleaning the bathroom with a damp cloth moistened with an antibacterial agent or bleach will merely spread the still-viable eggs.[23] Similarly, shaking clothes and bed linen will detach and spread the eggs.[23]
Treatment
Medication is the primary treatment for pinworm infection.[23] They are so effective that many medical scientists regard hygienic measures as impractical.[20] However, reinfection is frequent regardless of the medication used.[8] Total elimination of the parasite in a household may require repeated doses of medication for up to a year or more.[9] Because the drugs kill the adult pinworms, but not the eggs, the first retreatment is recommended in two weeks.[20] Also, if one household member spreads the eggs to another, it will be a matter of two or three weeks before those eggs become adult worms and thus amenable to treatment.[24] Asymptomatic infections, often in small children, can serve as reservoirs of infection, and therefore the entire household should be treated regardless of whether or not symptoms are present.[9][23]
The benzimidazole compounds albendazole and mebendazole are the most effective.[23] They work by inhibiting the microtubule function in the pinworm adults, causing glycogen depletion,[23] thereby effectively starving the parasite.[24] A single 100 milligram dose of mebendazole with one repetition after a week, is considered the safest, and is usually effective with cure rate of 96%.[8][23] Mebendazole has no serious side effects, although abdominal pain and diarrhea have been reported.[23] Pyrantel pamoate (also called pyrantel embonate, brand names e.g., Reese's Pinworm Medicine, Pin-X, Combantrin, Anthel, Helmintox, and Helmex) kills adult pinworms through neuromuscular blockade,[24] and is considered as effective as the benzimidazole compounds and is used as a second-line medication.[9] Other medications are piperazine, which causes flaccid paralysis in the adult pinworms, and pyrvinium pamoate (also called pyrvinium embonate), which works by inhibiting oxygen uptake of the adult pinworms.[24] Pinworms located in the genitourinary system (in this case, female genital area) may require other drug treatments.[8]
Epidemiology
Pinworm infection occurs worldwide,[10] and is the most common helminth (i.e., parasitic worm) infection in the United States and Western Europe.[17] In the United States, a study by the Center of Disease Control reported an overall incidence rate of 11.4% among people of all ages.[17] Pinworms are particularly common in children, with prevalence rates in this age group having been reported as high as 61% in India, 50% in England, 39% in Thailand, 37% in Sweden, and 29% in Denmark.[17] Finger sucking has been shown to increase both incidence and relapse rates,[17] and nail biting has been similarly associated.[13] Because it spreads from host to host through contamination, enterobiasis is common among people living in close contact, and tends to occur in all people within a household.[10] The prevalence of pinworms is not associated with gender,[10] nor with any particular social class, race, or culture.[17] Pinworms are an exception to the tenet that intestinal parasites are uncommon in affluent communities.[17]
History
The earliest known instance of pinworms is evidenced by pinworm eggs found in coprolite, carbon dated to 7837 BC at western Utah.[12] Pinworm infection is not classified as a neglected tropical disease unlike many other parasitic worm infections.[25]
Garlic has been used as a treatment in the ancient cultures of China, India, Egypt, and Greece.[26] Hippocrates (459–370 BC) mentioned garlic as a remedy against intestinal parasites.[27] German botanist Lonicerus (1564) recommended garlic against parasitic worms.[28] Applying raw garlic on skin may cause a chemical burn.[29][30]
Notes
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 "Pinworm Infection FAQs". CDC. 10 January 2013. Archived from the original on 15 October 2016. Retrieved 16 October 2016.
- ↑ 2.0 2.1 2.2 "Epidemiology & Risk Factors". CDC. 10 January 2013. Archived from the original on 18 October 2016. Retrieved 16 October 2016.
- ↑ 3.0 3.1 3.2 Stermer, E; Sukhotnic, I; Shaoul, R (May 2009). "Pruritus ani: an approach to an itching condition". Journal of Pediatric Gastroenterology and Nutrition. 48 (5): 513–6. doi:10.1097/mpg.0b013e31818080c0. PMID 19412003.
- ↑ 4.0 4.1 "Treatment". CDC. 23 September 2016. Archived from the original on 18 October 2016. Retrieved 16 October 2016.
- ↑ 5.0 5.1 5.2 5.3 Griffiths, Christopher; Barker, Jonathan; Bleiker, Tanya; Chalmers, Robert; Creamer, Daniel (2016). Rook's Textbook of Dermatology, 4 Volume Set (9 ed.). John Wiley & Sons. p. 33.13. ISBN 9781118441176. Archived from the original on 5 November 2017.
- ↑ "Biology". CDC. 10 January 2013. Archived from the original on 18 October 2016. Retrieved 16 October 2016.
- ↑ Bynum, W. F.; Porter, Roy (2013). Companion Encyclopedia of the History of Medicine. Routledge. p. 358. ISBN 9781136110368. Archived from the original on 5 November 2017.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 8.8 8.9 Burkhart & burkhart 2005, p. 838
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 9.11 9.12 9.13 9.14 9.15 9.16 Cook et al. 2009, p. 1516
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 10.7 10.8 Gutiérrez 2005, p. 355.
- ↑ 11.00 11.01 11.02 11.03 11.04 11.05 11.06 11.07 11.08 11.09 11.10 11.11 Caldwell 1982, p. 307.
- ↑ 12.00 12.01 12.02 12.03 12.04 12.05 12.06 12.07 12.08 12.09 12.10 12.11 12.12 12.13 12.14 Cook 1994, p. 1159
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 13.7 Cook 1994, p. 1160
- ↑ 14.0 14.1 14.2 14.3 Gutiérrez 2005, p. 356.
- ↑ 15.0 15.1 Gutiérrez 2005, p. 363.
- ↑ Gutiérrez 2005, p. 354.
- ↑ 17.00 17.01 17.02 17.03 17.04 17.05 17.06 17.07 17.08 17.09 17.10 17.11 17.12 17.13 17.14 17.15 17.16 17.17 17.18 Burkhart & burkhart 2005, p. 837
- ↑ 18.00 18.01 18.02 18.03 18.04 18.05 18.06 18.07 18.08 18.09 18.10 18.11 18.12 Garcia 1999, p. 246
- ↑ Cook, G C (1994). "Enterobius vermicularis infection". Gut. 35 (9): 1159–1162. doi:10.1136/gut.35.9.1159. ISSN 0017-5749. PMC 1375686. PMID 7959218.
{{cite journal}}: CS1 maint: url-status (link) - ↑ 20.0 20.1 20.2 20.3 20.4 20.5 20.6 20.7 20.8 20.9 Caldwell 1982, p. 308.
- ↑ dpdx 2009
- ↑ Garcia 1999, p. 247
- ↑ 23.00 23.01 23.02 23.03 23.04 23.05 23.06 23.07 23.08 23.09 23.10 23.11 23.12 23.13 23.14 23.15 23.16 Cook 1994, p. 1161
- ↑ 24.0 24.1 24.2 24.3 24.4 Caldwell 1982, p. 309.
- ↑ "Fact sheets: neglected tropical diseases". World Health Organization. WHO Media Centre. Archived from the original on 7 December 2014. Retrieved 6 December 2014.
- ↑ Petrovska BB, Cekovska S (2010). "Extracts from the history and medical properties of garlic". Pharmacognosy Reviews. 4 (7): 106–10. doi:10.4103/0973-7847.65321. PMC 3249897. PMID 22228949.
- ↑ Tucakov J. Beograd: Naucna knjiga; 1948. Farmakognozija; pp. 278–80.
- ↑ 3. Tucakov J. Beograd: Kultura; 1971. Lecenje biljem - fitoterapija; pp. 180–90.
- ↑ Borrelli, F; Capasso, R; Izzo, AA (November 2007). "Garlic (Allium sativum L.): adverse effects and drug interactions in humans". Molecular Nutrition & Food Research. 51 (11): 1386–97. doi:10.1002/mnfr.200700072. PMID 17918162.
- ↑ Friedman, T; Shalom, A; Westreich, M (October 2006). "Self-inflicted garlic burns: our experience and literature review". International Journal of Dermatology. 45 (10): 1161–3. doi:10.1111/j.1365-4632.2006.02860.x. PMID 17040429.
- References
- Hasegawa H, Ikeda Y, Fujisaki A, et al. (December 2005). "Morphology of chimpanzee pinworms, Enterobius (Enterobius) anthropopitheci (Gedoelst, 1916) (Nematoda: Oxyuridae), collected from chimpanzees, Pan troglodytes, on Rubondo Island, Tanzania". The Journal of Parasitology. 91 (6): 1314–7. doi:10.1645/GE-569R.1. PMID 16539010.
- "Pinworm". Encyclopædia Britannica. Archived from the original on 15 May 2015. Retrieved 8 April 2009.
- "Enterobiasis". Merriam-Webster's Medical Dictionary. Merriam-Webster. Archived from the original on 3 March 2016. Retrieved 8 April 2009.
- "Oxyuriasis". Merriam-Webster's Medical Dictionary. Merriam-Webster. Archived from the original on 24 February 2021. Retrieved 8 April 2009.
- Totkova A, Klobusicky M, Holkova R, Valent M (2003). "Enterobius gregorii—reality or fiction?" (PDF). Bratislavské Lekárske Listy. 104 (3): 130–133. PMID 12940699. Archived (PDF) from the original on 4 March 2017. Retrieved 3 March 2017.
- "Enterobius". NCBI taxonomy database. National Center for Biotechnology Information, U.S. National Library of Medicine. 2009. Archived from the original on 14 May 2018. Retrieved 8 April 2009.
- "Enterobiasis". DPDx. Division of Parasitic Diseases, Centers for Disease Control and Prevention. Archived from the original on 27 November 2013. Retrieved 8 April 2009.
- Nakano T, Okamoto M, Ikeda Y, Hasegawa H (December 2006). "Mitochondrial cytochrome c oxidase subunit 1 gene and nuclear rDNA regions of Enterobius vermicularis parasitic in captive chimpanzees with special reference to its relationship with pinworms in humans". Parasitology Research. 100 (1): 51–7. doi:10.1007/s00436-006-0238-4. PMID 16788831.
- Hugot JP (1983). "Enterobius gregorii (Oxyuridae, Nematoda), a new human parasite". Annales de Parasitologie Humaine et Comparée (in French). 58 (4): 403–4. doi:10.1051/parasite/1983584403. PMID 6416131.
{{cite journal}}: CS1 maint: unrecognized language (link) - Hasegawa H, Takao Y, Nakao M, Fukuma T, Tsuruta O, Ide K (February 1998). "Is Enterobius gregorii Hugot, 1983 (Nematoda: Oxyuridae) a distinct species?". Journal of Parasitology. 84 (1): 131–4. doi:10.2307/3284542. JSTOR 3284542. PMID 9488350.
- Gutiérrez, Yezid (2000). Diagnostic pathology of parasitic infections with clinical correlations (PDF) (Second ed.). Oxford University Press. pp. 354–366. ISBN 0-19-512143-0. Retrieved 21 August 2009.
- Cook, Gordon C; Zumla, Alimuddin I. (2009). Manson's tropical diseases (Twentysecond ed.). Saunders Elsevier. pp. 1515–1519. ISBN 978-1-4160-4470-3. Retrieved 18 November 2009.
- "B80: Enterobiasis". International Statistical Classification of Diseases and Related Health Problems (ICD) 10th Revision. World Health Organization. 2007. Archived from the original on 6 September 2009. Retrieved 5 December 2009.
- Cook GC (September 1994). "Enterobius vermicularis infection". Gut. 35 (9): 1159–62. doi:10.1136/gut.35.9.1159. PMC 1375686. PMID 7959218.
- Garcia, Lynne Shore (2009). Practical guide to diagnostic parasitology. American Society for Microbiology. pp. 246–247. ISBN 978-1-55581-154-9. Retrieved 5 December 2009.
- Burkhart CN, Burkhart CG (October 2005). "Assessment of frequency, transmission, and genitourinary complications of enterobiasis (pinworms)". International Journal of Dermatology. 44 (10): 837–40. doi:10.1111/j.1365-4632.2004.02332.x. PMID 16207185.
- Caldwell JP (February 1982). "Pinworms (Enterobius vermicularis)". Canadian Family Physician. 28: 306–9. PMC 2306321. PMID 21286054.
- Vanderkooi M (2000). Village Medical Manual (5th ed.).
External links
| Classification |
|---|
- Brown MD (March 2006). "Images in clinical medicine. Enterobius vermicularis". The New England Journal of Medicine. 354 (13): e12. doi:10.1056/NEJMicm040931. PMID 16571876.
- Pages with script errors
- CS1 maint: url-status
- Use dmy dates from December 2011
- Articles with invalid date parameter in template
- CS1 maint: unrecognized language
- Portal templates with all redlinked portals
- Colorectal surgery
- Parasites of equines
- Helminthiases
- Parasitic infestations, stings, and bites of the skin
- RTT
- Foodborne illnesses