Discrimination against people with HIV/AIDS
Discrimination against people with HIV/AIDS or serophobia is the prejudice, fear, rejection, and stigmatization of people with HIV/AIDS (PLHIV people living with HIV/AIDS). Marginalized, at-risk groups such as members of the LGBTQ+ community, intravenous drug users, and sex workers are most vulnerable to facing HIV/AIDS discrimination. The consequences of societal stigma against PLHIV are quite severe, as HIV/AIDS discrimination actively hinders access to HIV/AIDS screening and care around the world.[1] Moreover, these negative stigmas become used against members of the LGBTQ+ community in the form of stereotypes held by physicians.[2][failed verification]
HIV/AIDS discrimination takes many forms such as blood donation restrictions on at-risk populations, compulsory HIV testing without prior consent, violations of confidentiality within healthcare settings, and targeted violence against persons living with HIV. Although disability laws within many countries prohibit HIV/AIDS discrimination in housing, employment, and access to health/social services, HIV-positive individuals around the world still experience instances of stigma and abuse.[3] Overall, pervasive HIV/AIDS discrimination leads to low turn-out for HIV counseling and testing, identity crises, isolation, loneliness, low self-esteem, and a lack of interest in containing the disease.[4] Additionally, violent acts against HIV-infected individuals or people who are perceived to be infected with HIV can severely shut down the advancement of treatment in response to the progression of the disease.[5]
| Part of a series on |
| Discrimination |
|---|
 |
Stigma is often perpetuated by discrimination, callous actions, and bigotry. HIV/AIDS stigma is divided into the following three categories:
- Instrumental AIDS stigma—a reflection of the fear and apprehension that are likely to be associated with any deadly and transmissible illness.[6]
- Symbolic AIDS stigma—the use of HIV/AIDS to express attitudes toward the social groups or lifestyles perceived to be associated with the disease.[6]
- Courtesy AIDS stigma—stigmatization of people connected to the issue of HIV/AIDS or HIV-positive people.[4]
People living with HIV/AIDS may also experience internalized stigma. Internalized stigma is when a person applies negative ideas or stereotypes about HIV towards themselves. This can lead to feelings of shame or isolation. Internalized stigma can increase the fear that a HIV diagnosis will be disclosed, and subsequently, increase fear of discrimination or lack of acceptance due to the HIV positive status.[7] HIV-related stigma, and resulting discrimination, can negatively impact the mental health of people living with HIV.[7]
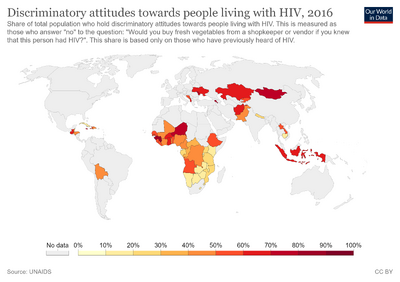
Stigma towards people living with HIV is widespread. In 35 percent of countries with available data, UNAIDS reports 50 percent of people admitted to having discriminatory attitudes towards people living with HIV.[8][9] The People Living with HIV Stigma Index (PLHIV Stigma Index) exists as a tool to collect evidence on the prevalence and impact of stigma and discrimination towards people living with HIV. The PLHIV Stigma Index was developed by GNP+, ICW, UNAIDS and IPPF in 2008, and is utilized in over 100 countries.[10] Individual country reports of the PLHIV Stigma Index are available from 2016 and beyond.[11]
People living with HIV face discrimination in many sectors, including healthcare, education, employment, and law enforcement.[9] Discrimination takes the form of denial of services, lack of accessible services for key populations, and insufficient funding and scale for services.[9] In conjunction with internalized stigma, HIV/AIDS stigma and discrimination make it more difficult for PLHIV to feel comfortable in obtaining the medical services they need.[12]
Misconceptions about HIV in the United States
Today, there continues to be significant misconceptions about HIV within the United States. Furthermore, misconceptions about the transmission of HIV promotes fear amongst many members of society, and this often translates into biased and discriminatory actions against PLHIV.[13]
A 2009 study conducted by the Kaiser Family Foundation found that many Americans still lack basic knowledge about HIV.[14] According to the survey, a third of Americans erroneously believe that HIV could be transmitted through sharing a drink or touching a toilet used by an HIV-positive individual.[14] Furthermore, the study reported that 42 percent of Americans would be uncomfortable with having an HIV-positive roommate, 23 percent would be uncomfortable with an HIV-positive coworker, 50 percent would be uncomfortable with an HIV-positive person preparing their food, and 35 percent would be uncomfortable with their child having an HIV-positive teacher.[14] Many of the respondents who were able to correctly answer questions about HIV transmission still reported similar biased views against HIV-positive individuals; in fact, 85 percent of these respondents reported that they would feel uncomfortable working with an HIV-positive coworker.[14]
Misconceptions about transmission of HIV
The only way that HIV can be transmitted from one individual to the next is by sharing of certain bodily fluids such as semen, blood, and vaginal discharge which the virus uses as a medium to enter the bloodstream of the recipient; HIV is not transmissible via fluids such as saliva, sweat, tears, or urine as it is not in high enough concentrations to spread in these matters.[15] In order for HIV to enter another person, either the semen, blood, or vaginal discharge must find an entry point by way of injection, unprotected sex, or during pregnancy as the mother can pass it along; one would only contract the virus when coming in direct contact with these fluids, for example, with an open cut on the skin that exposes blood.[15]
PLHIV do not always pass on the virus to someone else when engaging in sexual activities or sharing bodily fluids; PLHIV can have no transmission risk by taking medication which lowers the amount of HIV present in the bloodstream, rendering the individual as having an undetectable viral load.[16][17] PrEP (pre-exposure prophylaxis), on the other hand, is a drug that is used as a preventative measure against HIV for those who are at a higher risk of contracting the virus but does not cure someone who has HIV; furthermore, the medication should be taken regularly in order to have a higher protective chance against HIV and is not a one-time medication nor does it treat PLHIV.[18]
People cannot contract AIDS, rather they are infected with HIV which progresses into AIDS over time when left unchecked; if someone has HIV, it does not guarantee that they will develop AIDS. By frequently taking medication such as antiretroviral therapy (ART), the abundance of HIV in the bloodstream is reduced and prevents it from developing into AIDS.[19]
Misconceptions about at-risk populations
Tim McCaskell Archived 2022-05-12 at the Wayback Machine explains that AIDS wasn't seen as a health crisis until public health officials realized that marginalized people could infect other, non-marginalized people. This was the first time that he realized that medicine and health were viewed as political topics. Suddenly, access to proper health care became a political problem. AIDS Action Now explored the fact that medical professionals were treating people in the hospital as lesser humans. He also found out that there was no money for research or education. Doctors were ignoring their roles as fiduciaries for medically fragile people while the public believed that the doctor-patient relationship meant remaining as neutral as possible.[20]
Many people incorrectly believe that HIV is exclusive to gay men who have sex, but, although the risks are higher for gay and bisexual males, anyone is susceptible to contracting the virus regardless of their sexual orientation, race, age, and so forth.[21] Some forms of violence such as childhood trauma, rape, and sexual assault can lead people to engage in unsafe sexual practices which would increase their chances of contracting HIV.[22] In some cases, young girls and women who experience these traumatic events become sex workers or engage in prostitution which further increases these risks as well as contributes to the development of AIDS with lack of treatment.[22]
These discriminatory views of HIV-positive patients also persist within the medical field. A 2006 study of health professionals in Los Angeles County found that 56 percent of nursing facilities, 47 percent of obstetricians, and 26 percent of plastic surgeons had unlawfully refused to treat an HIV-positive patient, citing concerns of HIV transmission.[23] Overall, this societal stigma and discrimination has exacerbated distrust towards healthcare workers within the HIV-positive population.[23] The health care community therefore has an ethical duty to dispel stereotypes and misconceptions about HIV.[24]
Discriminatory practices in health-care settings
Discriminatory practices within the medical field have been found to greatly impact the health outcomes of HIV-positive individuals.[25] In both low-income and high-income nations, there have been several reported cases of medical providers administering low-quality care or denying care altogether to patients with HIV.[25] In a 2013 study conducted in Thailand, 40.9 percent of health workers reported worrying about touching the clothing and personal belongings of patients with HIV, despite possessing the knowledge that HIV does not spread through such items.[25] In a 2008 study of 90 countries, one in four persons living with HIV reported experiencing some form of discrimination in health-care settings.[25] Furthermore, one in five individuals with HIV reported having been denied medical care.[25] Even more concerning is the impact HIV-related discrimination has had on HIV-positive women. According to the 2008 study, one in three women living with HIV have reported instances of discrimination related to their sexual and reproductive health within a health-care setting.[25]
Another common form of discrimination within healthcare settings is the disclosure of a patient's HIV status without the patient's explicit permission.[25] Within many countries, an HIV-positive status can result in social exclusion, loss of social support, and decreased chances of getting married.[26] Therefore, concerns about potential breaches of confidentiality by health workers pose significant barriers to care for HIV-positive individuals. In a comprehensive study of 31 countries, one in five persons living with HIV reported instances of a health provider disclosing their HIV-positive status without consent.[25]
These discriminatory practices within the medical field have resulted in the delayed initiation of HIV treatment among HIV-positive individuals.[26] In New York City, men who have sex with men, transgender women, and persons of color living with HIV have all reported that stigma among medical providers was a major deterrent from entering or staying in HIV care.[25] A 2011 community-based study found that the most widely reported barrier to care amongst HIV-positive individuals is fear of stigma within healthcare settings.[26] HIV-positive individuals who have experienced significant HIV-related stigma are 2.4 times less likely to present for HIV care.[25] Currently, as many as 20–40 percent of Americans who are HIV-positive do not begin a care regimen within the first six months of diagnosis.[27] Overall, this perpetuation of HIV stigma has been detrimental to the health outcomes of HIV-positive individuals, as patients who begin treatment late in the progression of HIV have a 1.94 times greater risk of mortality in comparison to those who start treatment at the onset of diagnosis, suggesting that HIV treatment delays stemming from fears of discrimination may have fatal consequences.[28]
Blood donation restrictions on at-risk populations
Between 1970 and 1980, more than 20,000 HIV infections were attributed to contaminated blood transfusions.[29] The lack of sensitive blood screening methods for HIV detection prompted the enactment of lifetime bans on blood donations from men who have sex with men (MSM), sex workers, and intravenous drug users, as these population groups were viewed to be at high risk of contracting HIV.[29] At the time, this policy was viewed by health professionals as an emergency measure to prevent the contamination of the general blood supply. Multilateral institutions such as the World Health Organization actively promoted the enactment of lifetime bans in efforts to mitigate transfusion-related HIV infections.[29] This ban was adopted by the United States, as well as several European countries in the 1980s.[29]
The blood donation ban on MSM and transgender women, in particular, has provoked substantial criticism. Members of the LGBTQ+ community view these laws as discriminatory and homophobic.[30] A significant criticism of the blood donation restrictions is that healthcare workers treat the LGBTQ+ community as a homogenous population that engages in similar sexual practices and behaviors.[30] However, like any other population, MSM vary greatly in the number of sexual partners they have and in their engagement in high-risk sexual behaviors.[30] Overall, the donation ban on MSM and transgender women has further exacerbated growing distrust of the medical system within the LGBTQ+ community, especially given the history of homophobia within the medical profession.[29] As a result of these policies, LGBTQ+ individuals have felt substantial pressure to conceal their sexual orientation from medical providers and healthcare personnel.[29]
Blood banks today utilize advanced serological testing technologies with close to 100% sensitivity and specificity.[29] Currently, the risk of HIV-contaminated blood infection is 1 per 8-to-12 million donations, thus demonstrating the effectiveness of modern HIV screening technologies.[29] Despite these significant laboratory advances, the lifetime blood donation ban on MSM remains in several Western countries.[29] Today, medical organizations such as the American Red Cross and World Health Organization are highly critical of these lifetime bans on men who have sex with men, as the epidemiology of HIV has changed drastically in the last 40 years.[31] In 2015, a mere 27% of novel HIV infections originated from the MSM population.[29] In response to this epidemiological data, public health experts, medical personnel, and blood-banking organizations have called upon country governments to reform these outdated MSM blood donation policies.[31]
Mounting public pressure has prompted countries such as the United States and United Kingdom to reform their MSM blood donation restrictions.[31] In 2015, the United States substituted its lifetime ban for a 12-month deferral since last MSM sexual contact, although indefinite lifetime bans remain in place for sex workers and IV drug users.[32] Despite these small steps in the right direction, the American Red Cross has recommended that the Food and Drug Administration (FDA) further revise its policy by adopting a 3-month deferral period for MSM, as this is the current standard in countries such as Canada and the United Kingdom.[33] Overall, it is estimated that completely lifting the MSM blood donation ban could increase the total blood supply in the United States by 2-4%, which could help save millions of lives.[34] Given the blood supply shortage during the COVID-19 pandemic, blood donation restrictions have recently become the subject of further criticism.[35]
On April 2, 2020, the Food and Drug Administration provided updated guidance regarding blood donation in response to the blood shortage caused by the COVID-19 pandemic. This change came following pressure from Democratic Senators and LGBTQ+ rights organizations such as the Human Rights Campaign and GLAAD to reduce the twelve-month deferral period for MSM and women who have sex with men who have sex with men.[36] The updated guidance released by the FDA reduced the deferral period to three months, but did not meet activists' demands to base blood donation eligibility on individualized situations rather than "inaccurate stereotypes."[36][37] On June 8, 2020, the American Red Cross implemented these changes made by the FDA and reaffirmed in their announcement of these changes their belief that sexual orientation should not affect blood donation eligibility.[38] These changes catalyzed increased advocacy to end the ban against blood donations from MSM and transgender women entirely. The National LGBT Bar Association launched a "End the Gay Blood Ban" Campaign which called on the FDA to replace the current policy that singles-out MSM and transgender women with an individualized risk-based assessment, a policy currently used in countries such as Italy and Argentina. This policy would assess a potential donor's personal risk factors rather than their sexual orientation.[39] On April 16, 2020, GLAAD issued an open-letter to the FDA from over 500 infectious disease and HIV specialists, public health professionals, clinicians, healthcare administrators, trainees and researchers calling for a reevaluation of the updated guidance and the elimination of the blood ban in its entirety.[40]
Violence against persons living with HIV
Discrimination that is violent or threatening violence stops a lot of individuals from getting tested for HIV, which does not aid in curing the virus. Violence is an important factor against the treatment of people with AIDS. When PLHIV, particularly women, develop an intimate relationship, they tend not to be able to disclose to their partners of the presence of HIV in their system for fear of violence against them; this fear prevents them from receiving financial support to seek out testing, treatment, and general support from medical professionals & family members.[5] A study done on PLHIV in South Africa shows that out of a study population of 500, 16.1% of participants reported being physically assaulted, with 57.7% of those resulting from one's intimate partners such as husbands and wives. The available data show high rates of participants socially isolating themselves from both friends and family, in addition to avoiding the seeking of treatment at hospitals or clinics due to increasing internalized fears.[41]
Psychological impact of HIV discrimination
Persons living with HIV have developed self-depreciating mindsets and coping skills to deal with the social repercussions of an HIV-positive diagnosis. A common concern of PLHIV is the belief that they will automatically develop AIDS and not be able to live a long, productive life as others around them. While there is no cure for HIV/AIDS, ART and other medication prevent the virus from worsening and spreading which allows for PLHIV to live longer and still establish a life or family with people.[42] Albeit, not every PLHIV is knowledgeable about these resources which can lead them to adopt a depressive state of mind by associating their condition with early death.[43] In some cases, ART can reduce feelings of anxiety in individuals while induce other symptoms that worsen the mental health of some PLHIV and should be taken as directed by a physician; likewise, taking ART with other prescriptions might exacerbate these mental health conditions.[43]
Negative social consequences such as stigmatization and discrimination have severe psychological implications on PLHIV: when a person chooses to disclose their status, it can lead to restricted options for marriage and even employment. This tends to worsen the mental health of these individuals and often results in a fear of disclosure.[44]
Research done in South Africa has found that the high levels of stigma experienced by HIV-positive individuals has a severe psychological impact. Internalized stigma and discrimination run rampant throughout the PLHIV community, as many PLHIV in South Africa blamed themselves for their current situation.[45] Psychological support for PLHIV in certain countries around the world is scarce.[46]
A study examining the impact of stigma on PLHIV concluded that experiencing higher levels of HIV discrimination is correlated with a depressive state and even receiving psychiatric care the previous year. Depressive symptoms have also been correlated with elevated rates of suicidal ideation, anxiety and disease progression.[47] Another recent study that predominantly focused on HIV-positive African American men concluded that stigma has a profound impact on reducing the quality of life of these individuals.[48]
Studies have also shown that individuals living in non-metropolitan areas of the United States also experience large amounts of emotional distress. 60% of participants enrolled in a randomized clinical trial reported moderate or severe levels of depressive symptomatology on the Beck Depression Inventory. This is due to these participants receiving much less social support, and also due to great levels of HIV-related stigma and rejection within families.[47] Furthermore, relative to their urban counterparts, PLHIV in non-metropolitan areas experience more loneliness, a lack of sufficient healthcare and social services, and higher levels of discrimination which contribute to much greater levels of emotional distress.[47]
HIV/AIDS health disparities in marginalized groups
The U.S. HIV epidemic has drastically evolved over the course of the last 30 years and has been rampantly widespread in socially marginalized and underrepresented communities. Statistics show that most HIV infections occur in sexual minorities and communities of color. For example, in 2009, African Americans accounted for 44% of all new HIV infections while making up only 14% of the U.S. population.[49] Similarly, 78% of HIV infections in Georgia occur among African Americans, while African Americans comprise only 30% of the overall population.[49] Hall et al. (2008) found distinct incidence rates of HIV infection among African Americans (83/100,000 population) and Latinos (29/100,000), specifically when compared to whites (11/100,000).[49]
The single group that is consistently at the greatest risk for HIV infection happens to form the intersection of sexual orientation and racial background; MSM (men who have sex with men) are the most HIV affected Americans, and African American MSM are at an HIV risk that is six times greater than that of white MSM.[49] Aside from race and sexual orientation, socioeconomic status, education and employment are all equally important factors that studies link to HIV infection. The CDC reports that HIV rates are highest among groups who are at or below the poverty level; they also found that individuals who are unemployed and/or have less than a high school education are more prone to HIV infection.[49]
In order to help HIV infected persons receive care, the first vital step revolves around HIV testing and early diagnosis. Delayed testing is highly detrimental and leads to an increased risk of HIV transmission. Currently, there are many issues associated with HIV diagnosis and lack of available testing for minorities. A study of 16 US cities found that African Americans are more likely to be tested much later for HIV infection, which places this group at a stark disadvantage for gaining access to proper treatment.[50] This is problematic because HIV is only half of the story: a prolonged HIV infection can quickly become an AIDS diagnosis, and this can be prevented with early and frequent testing. Approximately 35%-45% of those diagnosed with HIV are believed to also have AIDS at the time of testing.[50] About half of the people diagnosed with HIV do not receive care in any given year, which poses a risk that they are endangering others while they are not given treatment.[50] Various studies suggest that groups with lower socioeconomic status and lower education level are associated with poorer medication adherence.[51] These individuals have also been found to be more likely to die after initiating treatment.[52]
Access to Pre-Exposure Prophylaxis among marginalized groups
Marginalized groups also face barriers to accessing HIV/AIDS preventative care such as Pre-Exposure Prophylaxis (PrEP). Studies have shown that concerns about paying for PrEP and talking to healthcare providers about sexual behaviors have contributed to low PrEP use among young sexual minority men.[53] Other structural barriers to PrEP use include limited knowledge of its availability, stigma surrounding HIV, and distrust of the medical establishment among minority groups due to years of discrimination within the medical field against marginalized groups.[54] A poll conducted on the gay dating-app Grindr found a high prevalence of poor access to health insurance and lack of education about PrEP among respondents.[55] Studies have found that cost concerns, mental health, substance use issues, concerns about hormone interaction, uncomfortable side effects, difficulty taking pills, stigma, exclusion of transgender women in advertising, and lack of research on transgender women and PrEP are all barriers to PrEP use among transgender women. Structural barriers to PrEP use among transgender women include employment, transportation, and housing insecurity/homelessness.[56][57] A study of Black MSM in London found that instances of racism in spaces dedicated to gay men led to an avoidance of these spaces among the study participants, leading Black MSM to miss out on PrEP awareness that was disseminated via gay channels.[58]
HIV/AIDS Disparities amongst the Incarcerated Population
As of the end of 2018, the black imprisonment rate was about twice that of Hispanics and more than five times the imprisonment rate amongst whites in the United States.[59] Moreover, black males are more likely to be imprisoned with 2,272 inmates per 100,000 black men, in comparison to 1,018 inmates per 100,000 Hispanic men and 392 inmates per 100,000 white men.[59] Incarcerated individuals have a much higher risk of having HIV than non-incarcerated individuals. The estimated global HIV prevalence for prisoners is 3%, whereas the estimated global HIV prevalence for adults in general is 0.7%.[60][61] Additionally, women in prison have a higher HIV prevalence than men.[60] Incarcerated individuals also have a high risk of transmission as well due to high-risk activity (i.e. unsafe and unsterile tattooing, needle sharing, and unprotected sexual activity). Needle sharing is much more prevalent in prisons because possession of needles in prison is oftentimes a criminal offense, causing clean needles to be scarce.[62] Only about 30% of countries worldwide offer condoms for incarcerated individuals, but for the countries that do offer condoms, coverage and access is not reported.[63] Moreover, these individuals have a harder time accessing critical HIV resources such as ART.[64] Even if ART is offered, those with HIV may still lack the ability to get specialized care and specific ART regimens.[65]
Effects of COVID-19 pandemic on people with HIV/AIDS
Inequities resulting from discrimination and stigma towards PLHIV can impact susceptibility to other public health threats. Discrimination in the housing, medical, and employment sectors towards PLHIV has helped to drive the COVID-19 public health threat in marginalized populations.[66] Many of the groups most vulnerable to HIV infection, such as communities of color or individuals living in poverty, are also at increased risk of contracting COVID-19. PLHIV also appear to be more likely to live in the areas hit hardest by COVID-19. The Kaiser Family Foundation found that 15 of the 20 counties with the highest HIV prevalence in the United States were also ranked in the top 20 counties with the highest COVID-19 morbidity and mortality rates.[67]
The effects of COVID-19 on people with HIV is still being studied. It is thought individuals of older age or with serious underlying medical conditions may be at greater risk for severe illness from COVID-19. This includes people with HIV who have comorbidities, a low CD4 cell count, or are not currently on effective HIV treatment.[68] The Coronavirus Under Research Exclusion (CURE HIV-COVID) database collects information on outcome of COVID-19 in people living with HIV.[69] According to the WHO, 23.1% of PLHIV hospitalized for COVID-19 died from the disease, making HIV a risk-factor for severe illness or death due to the virus.[70] The CDC, WHO, and other health organizations have recommended that PLHIV are given priority for COVID-19 vaccination, and the CDC has recommended additional vaccine doses for PLHIV with advanced disease or who are not taking medication to treat their HIV.[70][71] Some states have explicitly prioritized vaccination for people living with HIV, while others used the broader criteria of individual who are in an "immunocompromised state", which can include PLHIV. [67]
At various points in the pandemic, hospitals were overwhelmed by the number of COVID-19 patients, some of whom required intensive treatments like invasive ventilation and extracorporeal membrane oxygenation (ECMO).[72][73] As a result, there were serious concerns about the need to institute care rationing systems which would provide criteria for the prioritization of patients to receive medical attention and treatment. As there was little coordination between hospitals or guidance from local and state governments, many immunocompromised individuals, including PLHIV, were uncertain of the implications of these policies on their access to care. In March 2020, the Office for Civil Rights in the Department of Health and Human Services filed a complaint against Washington and Alabama for their care rationing policies, citing them as discriminatory against individuals with disabilities.[74]
See also
References
- ↑ Mahajan AP, Sayles JN, Patel VA, Remien RH, Sawires SR, Ortiz DJ, et al. (August 2008). "Stigma in the HIV/AIDS epidemic: a review of the literature and recommendations for the way forward". AIDS. 22 Suppl 2 (Suppl 2): S67-79. doi:10.1097/01.aids.0000327438.13291.62. PMC 2835402. PMID 18641472.
- ↑ Morris M, Cooper RL, Ramesh A, Tabatabai M, Arcury TA, Shinn M, et al. (August 2019). "Training to reduce LGBTQ-related bias among medical, nursing, and dental students and providers: a systematic review". BMC Medical Education. 19 (1): 325. doi:10.1186/s12909-019-1727-3. PMC 6716913. PMID 31470837.
- ↑ "Civil Rights". HIV.gov. 2017-11-10. Archived from the original on 2018-10-29. Retrieved 2018-04-10.
- ↑ Parker R, Aggleton P (July 2003). "HIV and AIDS-related stigma and discrimination: a conceptual framework and implications for action". Social Science & Medicine. 57 (1): 13–24. doi:10.1016/S0277-9536(02)00304-0. PMID 12753813.
- ↑ 5.0 5.1 "Violence Against Women and HIV/AIDS: Critical Intersections. Intimate Partner Violence and HIV/AIDS" (PDF). World Health Organization. 2004. Archived (PDF) from the original on 2021-11-04. Retrieved 2022-07-02.
- ↑ 6.0 6.1 Herek GM (1999). "AIDS and stigma in the United States. [Special issue]". American Behavioral Scientist. 42 (7).
- ↑ 7.0 7.1 "Facts about HIV Stigma | HIV Basics | HIV/AIDS | CDC". www.cdc.gov. 2020-10-22. Archived from the original on 2021-03-26. Retrieved 2021-04-08.
- ↑ "HIV Stigma and Discrimination". Avert. 2015-07-20. Archived from the original on 2018-10-22. Retrieved 2021-04-08.
- ↑ 9.0 9.1 9.2 https://www.unaids.org/sites/default/files/media_asset/WAD2015_report_en_part01.pdf Archived 2022-04-23 at the Wayback Machine[bare URL PDF]
- ↑ "What is the People Living with HIV Stigma Index?". People Living with HIV Stigma Index. Archived from the original on 2021-04-17. Retrieved 2021-04-08.
- ↑ "Country Reports". People Living with HIV Stigma Index. Archived from the original on 2021-04-26. Retrieved 2021-04-26.
- ↑ Mirza, Shabab Ahmed; Rooney, Caitlin (2018-01-18). "Discrimination Prevents LGBTQ People From Accessing Health Care". Center for American Progress. Archived from the original on 2021-04-01. Retrieved 2021-04-08.
- ↑ Waite KR, Paasche-Orlow M, Rintamaki LS, Davis TC, Wolf MS (September 2008). "Literacy, social stigma, and HIV medication adherence". Journal of General Internal Medicine. 23 (9): 1367–72. doi:10.1007/s11606-008-0662-5. PMC 2518013. PMID 18563494.
- ↑ 14.0 14.1 14.2 14.3 "2009 Survey of Americans on HIV/AIDS: Summary of Findings on the Domestic Epidemic". The Henry J. Kaiser Family Foundation. 2009-04-02. Archived from the original on 2020-07-29. Retrieved 2020-04-27.
- ↑ 15.0 15.1 "HIV Transmission | HIV Basics | HIV/AIDS | CDC". www.cdc.gov. 2019-09-25. Archived from the original on 2016-12-29. Retrieved 2020-06-30.
- ↑ "Undetectable Viral Load and HIV Transmission Risk". Healthline. 12 September 2018. Archived from the original on 2020-06-25. Retrieved 2020-06-23.
- ↑ "HIV Treatment as Prevention | HIV Risk and Prevention | HIV/AIDS | CDC". www.cdc.gov. 2020-04-06. Archived from the original on 2022-07-16. Retrieved 2020-06-30.
- ↑ "PrEP | HIV Basics | HIV/AIDS | CDC". www.cdc.gov. 2020-06-04. Archived from the original on 2019-10-31. Retrieved 2020-06-23.
- ↑ "Symptoms of HIV". HIV.gov. 2020-06-05. Archived from the original on 2020-06-21. Retrieved 2020-06-23.
- ↑ "Toronto Interviews". 14 October 2016. Archived from the original on 12 May 2022. Retrieved 2 July 2022.
- ↑ "Who Is at Risk for HIV?". HIV.gov. 2017-05-15. Archived from the original on 2020-06-29. Retrieved 2020-06-30.
- ↑ 22.0 22.1 "WHO | Violence against women and HIV". WHO. Archived from the original on 2020-07-29. Retrieved 2020-06-26.
- ↑ 23.0 23.1 Sears B, Ho D (2006-12-01). "HIV Discrimination in Health Care Services in Los Angeles County: The Results of Three Testing Studies". UCLA: The Williams Institute: Other Recent Work. Archived from the original on 2022-04-17. Retrieved 2022-07-02.
- ↑ Anderson BJ (December 2009). "HIV Stigma and Discrimination Persist, Even in Health Care". The Virtual Mentor. 11 (12): 998–1001. doi:10.1001/virtualmentor.2009.11.12.oped1-0912. PMID 23207098.
- ↑ 25.0 25.1 25.2 25.3 25.4 25.5 25.6 25.7 25.8 25.9 "UNAIDS warns that HIV-related stigma and discrimination is preventing people from accessing HIV services". www.unaids.org. Archived from the original on 2020-05-14. Retrieved 2020-05-13.
- ↑ 26.0 26.1 26.2 Pollini RA, Blanco E, Crump C, Zúñiga ML (October 2011). "A community-based study of barriers to HIV care initiation". AIDS Patient Care and STDs. 601-09. 25 (10): 601–9. doi:10.1089/apc.2010.0390. PMC 3183651. PMID 21955175.
- ↑ Mugavero MJ (December 2008). "Improving engagement in HIV care: what can we do?". Topics in HIV Medicine. 16 (5): 156–61. PMID 19106431.
- ↑ "Guidelines for the use of antiretroviral agents in HIV-1-infected adults and adolescents". Department of Health and Human Services. Panel on Antiretroviral Guidelines for Adults and Adolescents. October 14, 2011.
- ↑ 29.0 29.1 29.2 29.3 29.4 29.5 29.6 29.7 29.8 29.9 Karamitros G, Kitsos N, Karamitrou I (2017-06-08). "The ban on blood donation on men who have sex with men: time to rethink and reassess an outdated policy". The Pan African Medical Journal. 27: 99. doi:10.11604/pamj.2017.27.99.12891. PMC 5554671. PMID 28819520.
- ↑ 30.0 30.1 30.2 "Ban the Ban: An argument against the 12 month blood donation deferral for men who have sex with men". GLAAD. 2018-11-28. Archived from the original on 2020-03-31. Retrieved 2020-04-06.
- ↑ 31.0 31.1 31.2 Miyashita A (September 2014). "Effects of Lifting Blood Donation Bans on Men Who Have Sex with Men" (PDF). Archived (PDF) from the original on 2021-11-04. Retrieved 2022-07-02.
- ↑ Center for Biologics Evaluation and Research (2019-04-11). "Revised Recommendations for Reducing the Risk of Human Immunodeficiency Virus Transmission by Blood and Blood Products - Questions and Answers". FDA. Archived from the original on 2022-06-21. Retrieved 2022-07-02.
- ↑ "American Red Cross Statement on FDA MSM Deferral Policy". www.redcross.org. Archived from the original on 2020-04-04. Retrieved 2020-04-06.
- ↑ Miyashita A (2014). "Effects of Lifting Blood Donation Bans on Men who Have Sex with Men" (PDF). The Williams Institute. Archived (PDF) from the original on 2022-06-17. Retrieved 2022-07-02.
- ↑ "PAHO warns of potential blood shortages during the COVID-19 pandemic - PAHO/WHO | Pan American Health Organization". www.paho.org (in español). Archived from the original on 2020-04-21. Retrieved 2020-04-27.
- ↑ 36.0 36.1 "Senators, activists urge FDA to revise blood donation policy for gay, bisexual men amid coronavirus pandemic". ABC News. Archived from the original on 2021-03-30. Retrieved 2021-04-07.
- ↑ Office of the Commissioner (2020-07-17). "Coronavirus (COVID-19) Update: FDA Provides Updated Guidance to Address the Urgent Need for Blood During the Pandemic". FDA. Archived from the original on 2020-08-07. Retrieved 2021-04-07.
- ↑ "Red Cross to Implement FDA Eligibility Changes". www.redcross.org. Archived from the original on 2021-04-23. Retrieved 2021-04-07.
- ↑ "End the Blood Ban". The National LGBT Bar Association. 2020-07-20. Archived from the original on 2021-04-10. Retrieved 2021-04-07.
- ↑ "Open letter to FDA from medical professionals". GLAAD. 2020-04-16. Archived from the original on 2021-04-12. Retrieved 2021-04-07.
- ↑ Dos Santos MM, Kruger P, Mellors SE, Wolvaardt G, van der Ryst E (January 2014). "An exploratory survey measuring stigma and discrimination experienced by people living with HIV/AIDS in South Africa: the People Living with HIV Stigma Index". BMC Public Health. 14 (1): 80. doi:10.1186/1471-2458-14-80. PMC 3909177. PMID 24461042.
- ↑ "HIV/AIDS". www.who.int. Archived from the original on 2022-05-01. Retrieved 2020-06-23.
- ↑ 43.0 43.1 "Mental Health". HIV.gov. 2020-03-19. Archived from the original on 2020-06-21. Retrieved 2020-06-23.
- ↑ "The Psychological Impact of HIV – AIDS 2020". Archived from the original on 2020-06-27. Retrieved 2020-06-26.
- ↑ Visser MJ, Makin JD, Vandormael A, Sikkema KJ, Forsyth BW (February 2009). "HIV/AIDS stigma in a South African community". AIDS Care. 21 (2): 197–206. doi:10.1080/09540120801932157. PMC 4238924. PMID 19229689.
- ↑ "Funding for HIV and AIDS". Avert. 2015-07-20. Archived from the original on 2022-02-14. Retrieved 2022-02-14.
- ↑ 47.0 47.1 47.2 Heckman TG, Anderson ES, Sikkema KJ, Kochman A, Kalichman SC, Anderson T (January 2004). "Emotional distress in nonmetropolitan persons living with HIV disease enrolled in a telephone-delivered, coping improvement group intervention". Health Psychology. 23 (1): 94–100. doi:10.1037/0278-6133.23.1.94. PMID 14756608.
- ↑ Buseh AG, Kelber ST, Stevens PE, Park CG (2008). "Relationship of symptoms, perceived health, and stigma with quality of life among urban HIV-infected African American men". Public Health Nursing. 25 (5): 409–19. doi:10.1111/j.1525-1446.2008.00725.x. PMID 18816358.
- ↑ 49.0 49.1 49.2 49.3 49.4 Pellowski JA, Kalichman SC, Matthews KA, Adler N (2013). "A pandemic of the poor: social disadvantage and the U.S. HIV epidemic". The American Psychologist. 68 (4): 197–209. doi:10.1037/a0032694. PMC 3700367. PMID 23688088.
- ↑ 50.0 50.1 50.2 Gardner EM, McLees MP, Steiner JF, Del Rio C, Burman WJ (March 2011). "The spectrum of engagement in HIV care and its relevance to test-and-treat strategies for prevention of HIV infection". Clinical Infectious Diseases. 52 (6): 793–800. doi:10.1093/cid/ciq243. PMC 3106261. PMID 21367734.
- ↑ Kleeberger CA, Phair JP, Strathdee SA, Detels R, Kingsley L, Jacobson LP (January 2001). "Determinants of heterogeneous adherence to HIV-antiretroviral therapies in the Multicenter AIDS Cohort Study". Journal of Acquired Immune Deficiency Syndromes. 26 (1): 82–92. doi:10.1097/00126334-200101010-00012. PMID 11176272.
- ↑ Cunningham, William E; Hays, Ron D; Duan, Naihua; Andersen, Ronald; Nakazono, Terry T; Bozzette, Samuel A; Shapiro, Martin F (2005). "The Effect of Socioeconomic Status on the Survival of People Receiving Care for HIV Infection in the United States". Journal of Health Care for the Poor and Underserved. 16 (4): 655–676. doi:10.1353/hpu.2005.0093. ISSN 1548-6869. Archived from the original on 2022-01-19. Retrieved 2022-07-02.
- ↑ Jaiswal J, Griffin M, Singer SN, Greene RE, Acosta IL, Kaudeyr SK, et al. (2018). "Structural Barriers to Pre-exposure Prophylaxis Use Among Young Sexual Minority Men: The P18 Cohort Study". Current HIV Research. 16 (3): 237–249. doi:10.2174/1570162x16666180730144455. PMC 8893045. PMID 30062970. S2CID 51876690.
- ↑ Mayer KH, Agwu A, Malebranche D (May 2020). "Barriers to the Wider Use of Pre-exposure Prophylaxis in the United States: A Narrative Review". Advances in Therapy. 37 (5): 1778–1811. doi:10.1007/s12325-020-01295-0. PMC 7467490. PMID 32232664.
- ↑ "Three Potential Barriers to HIV PrEP". Pharmacy Times. Archived from the original on 2021-04-23. Retrieved 2021-04-07.
- ↑ Ogunbajo A, Storholm ED, Ober AJ, Bogart LM, Reback CJ, Flynn R, et al. (January 2021). "Multilevel Barriers to HIV PrEP Uptake and Adherence Among Black and Hispanic/Latinx Transgender Women in Southern California". AIDS and Behavior. 25 (7): 2301–2315. doi:10.1007/s10461-021-03159-2. ISSN 1090-7165. PMC 7845787. PMID 33515132.
- ↑ Rael CT, Martinez M, Giguere R, Bockting W, MacCrate C, Mellman W, et al. (November 2018). "Barriers and Facilitators to Oral PrEP Use Among Transgender Women in New York City". AIDS and Behavior. 22 (11): 3627–3636. doi:10.1007/s10461-018-2102-9. PMC 6160363. PMID 29589137.
- ↑ "Racism, marginalisation and PrEP stereotypes affect PrEP uptake for black MSM in London". aidsmap.com. Archived from the original on 2021-04-21. Retrieved 2021-04-07.
- ↑ 59.0 59.1 "Black imprisonment rate in the U.S. has fallen by a third since 2006". Pew Research Center. Archived from the original on 2021-04-25. Retrieved 2021-04-26.
- ↑ 60.0 60.1 "Transgender people". www.who.int. Archived from the original on 2020-10-20. Retrieved 2021-04-08.
- ↑ "The Global HIV/AIDS Epidemic". KFF. 2021-03-02. Archived from the original on 2021-04-11. Retrieved 2021-04-08.
- ↑ "Prisoners, HIV and AIDS". Avert. 2015-07-20. Archived from the original on 2021-04-12. Retrieved 2021-04-08.
- ↑ Moazen, Babak (January 2019). "Availability, coverage and barriers towards condom provision in prisons: a review of the evidence" (PDF). Frankfurt am Main/Germany: Institut für Suchtforschung (ISFF), Frankfurt University of Applied Sciences. Archived (PDF) from the original on 2021-11-04. Retrieved 2022-07-02.
- ↑ "Prisoners" (PDF). The Gap Report 2014. UNAIDS. Archived (PDF) from the original on 2022-03-08. Retrieved 2022-07-02.
- ↑ Rich, Josiah D; Beckwith, Curt G; Macmadu, Alexandria; Marshall, Brandon D L; Brinkley-Rubinstein, Lauren; Amon, Joseph J; Milloy, M-J; King, Maximilian R F; Sanchez, Jorge; Atwoli, Lukoye; Altice, Frederick L (10 September 2016). "Clinical care of incarcerated people with HIV, viral hepatitis, or tuberculosis". The Lancet. 388 (10049): 1103–1114. doi:10.1016/S0140-6736(16)30379-8. ISSN 0140-6736. PMC 5504684. PMID 27427452.
- ↑ Winwood, Jordan J.; Fitzgerald, Lisa; Gardiner, Bernard; Hannan, Kate; Howard, Chris; Mutch, Allyson (December 2021). "Exploring the Social Impacts of the COVID-19 Pandemic on People Living with HIV (PLHIV): A Scoping Review". AIDS and Behavior. 25 (12): 4125–4140. doi:10.1007/s10461-021-03300-1. ISSN 1090-7165. PMC 8137806. PMID 34019203. Archived from the original on 2022-07-16. Retrieved 2022-07-02.
- ↑ 67.0 67.1 "Key Questions: HIV and COVID-19". KFF. 2021-05-20. Archived from the original on 2022-03-11. Retrieved 2022-05-14.
- ↑ "COVID-19 and Your Health". Centers for Disease Control and Prevention. 2020-02-11. Archived from the original on 2021-03-02. Retrieved 2021-03-03.
- ↑ "HIV-COVID". HIV-COVID Database. Archived from the original on 2021-04-17. Retrieved 2021-04-08.
- ↑ 70.0 70.1 "Coronavirus disease (COVID-19): COVID-19 vaccines and people living with HIV". www.who.int. Archived from the original on 2022-04-25. Retrieved 2022-05-14.
- ↑ Dooling, Kathleen (2020). "The Advisory Committee on Immunization Practices' Interim Recommendation for Allocating Initial Supplies of COVID-19 Vaccine — United States, 2020". MMWR. Morbidity and Mortality Weekly Report. 69. doi:10.15585/mmwr.mm6949e1. ISSN 0149-2195. Archived from the original on 2022-07-01. Retrieved 2022-07-02.
- ↑ Fink, Sheri (2021-07-12). "The Rationing of a Last-Resort Covid Treatment". The New York Times. ISSN 0362-4331. Archived from the original on 2022-04-09. Retrieved 2022-05-14.
- ↑ Nagourney, Eric; Delkic, Melina; Rio, Giulia McDonnell Nieto del; Bogel-Burroughs, Nicholas (2020-10-26). "A surge in hospitalizations is straining some U.S. health care facilities". The New York Times. ISSN 0362-4331. Archived from the original on 2022-04-09. Retrieved 2022-05-14.
- ↑ Fink, Sheri (2020-03-28). "U.S. Civil Rights Office Rejects Rationing Medical Care Based on Disability, Age". The New York Times. ISSN 0362-4331. Archived from the original on 2022-05-06. Retrieved 2022-05-14.
- CS1: long volume value
- Webarchive template wayback links
- All articles with bare URLs for citations
- Articles with bare URLs for citations from March 2022
- Articles with invalid date parameter in template
- Articles with PDF format bare URLs for citations
- CS1 español-language sources (es)
- All articles with failed verification
- Articles with failed verification from November 2021
- Articles with broken excerpts
- Discrimination by type
- HIV/AIDS