Deep vein thrombosis
| Deep vein thrombosis | |
|---|---|
| Other names: Deep venous thrombosis | |
 | |
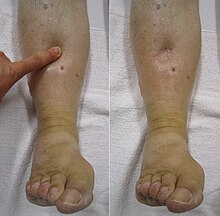
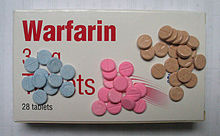
| DVT in the right leg with swelling and redness | |
| Specialty | Various |
| Symptoms | Pain, swelling, redness, enlarged veins in the affected limb[1] |
| Complications | Post-thrombotic syndrome, recurrent VTE[2] |
| Risk factors | Recent surgery, older age, active cancer, obesity, personal history or family history of VTE, injuries, trauma, lack of movement, hormonal birth control, pregnancy and the period following delivery, antiphospholipid syndrome, certain genetic factors[3][4] |
| Diagnostic method | Ultrasound[5] |
| Differential diagnosis | Ruptured Baker's cyst, cellulitis, hematoma, lymphedema, and chronic venous insufficiency |
| Prevention | Frequent walking, calf exercises, maintaining a healthy body weight, anticoagulants (blood thinners), intermittent pneumatic compression, graduated compression stockings, aspirin[6][7] |
| Treatment | Anticoagulation, catheter-directed thrombolysis |
| Medication | Direct oral anticoagulants, low-molecular-weight heparin, fondaparinux, unfractionated heparin, warfarin |
| Frequency | 1.0–1.8 out of 1,000 people per year with European ancestry[3] |
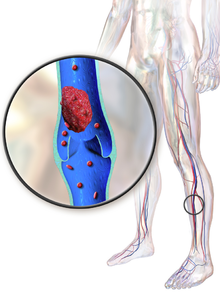
Deep vein thrombosis (DVT) is the formation of a blood clot in a deep vein, most commonly in the legs or pelvis.[8][lower-alpha 1] Symptoms can include pain, swelling, redness, and enlarged veins in the affected area, but some DVTs have no symptoms.[1] The most common life-threatening concern with DVT is the potential for a clot (or multiple clots) to detach, travel through the right side of the heart, and become stuck in arteries that supply blood to the lungs. This is called pulmonary embolism (PE). Both DVT and PE are considered as part of the same overall disease process, which is called venous thromboembolism (VTE). VTE can occur as an isolated DVT or as PE with or without DVT.[3] The most frequent long-term complication is post-thrombotic syndrome, which can cause pain, swelling, a sensation of heaviness, itching, and in severe cases, ulcers.[5] Also, recurrent VTE occurs in about 30% of those in the ten years following an initial VTE.[3]
The mechanism of clot formation typically involves some combination of decreased blood flow rate, increased tendency to clot, and injury to the blood vessel wall.[9] Risk factors include recent surgery, older age, active cancer, obesity, personal history and family history of VTE, trauma, injuries, lack of movement, hormonal birth control, pregnancy and the period following birth, and antiphospholipid syndrome. VTE has a strong genetic component, accounting for approximately 50 to 60% of the variability in VTE rates.[4] Genetic factors include non-O blood type, deficiencies of antithrombin, protein C, and protein S and the mutations of factor V Leiden and prothrombin G20210A. In total, dozens of genetic risk factors have been identified.[4][10]
People suspected of having a DVT can be assessed using a prediction rule such as the Wells score. A D-dimer test can also be used to assist with excluding the diagnosis or to signal a need for further testing.[5] Diagnosis is most commonly confirmed by ultrasound of the suspected veins.[5] An estimated 4–10% of DVTs affect the arms.[11] About 5–11% of people will develop VTE in their lifetime, with VTE becoming much more common with age.[12][13] When compared to those aged 40 and below, people aged 65 and above are at an approximate 15 times higher risk.[14] However, available data has been historically dominated by European and North American populations,[15] and Asian and Hispanic individuals have a lower VTE risk than whites or blacks.[4]
Using blood thinners (anticoagulation) is the standard treatment, and typical medications include rivaroxaban, apixaban, and warfarin. Beginning warfarin treatment requires an additional a non-oral anticoagulant, often injections of heparin.[16][17][18] Prevention of VTE for the general population includes avoiding obesity and maintaining an active lifestyle. Preventive efforts following low-risk surgery include early and frequent walking. Riskier surgeries generally prevent VTE with a blood thinner or aspirin combined with intermittent pneumatic compression.[7]
Signs and symptoms
Signs and symptoms of DVT, while highly variable, include pain or tenderness, swelling, warmth, dilation of surface veins, redness or discoloration, and cyanosis with fever.[5] However, some with DVT have no symptoms.[18] Signs and symptoms alone are not sufficiently sensitive or specific to make a diagnosis, but when considered in conjunction with pre-test probability, can help determine the likelihood of DVT.[18] In most suspected cases, DVT is ruled out after evaluation,[19] and symptoms are more often due to other causes, such as ruptured Baker's cyst, cellulitis, hematoma, lymphedema, and chronic venous insufficiency.[1] Other differential diagnoses include tumors, venous or arterial aneurysms, and connective tissue disorders.[20]
Causes
The three factors of Virchow's triad—venous stasis, hypercoagulability, and changes in the endothelial blood vessel lining—contribute to VTE and are used to explain its formation. Venous stasis is the most consequential of these three factors.[9] Other related causes include activation of immune system components, the state of microparticles in the blood, the concentration of oxygen, and possible platelet activation.[21] Various risk factors contribute to VTE, including genetic and environmental factors, though many with multiple risk factors never develop it.[22][12]
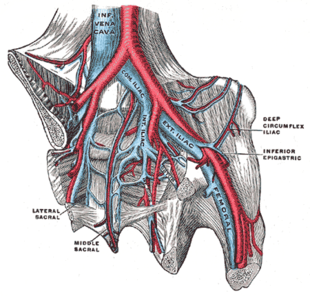
Acquired risk factors include the strong risk factor of older age,[5] which alters blood composition to favor clotting.[23] Previous VTE, particularly unprovoked VTE, is a strong risk factor.[24] Major surgery and trauma increase risk because of tissue factor from outside the vascular system entering the blood.[25] Minor injuries,[26] lower limb amputation,[27] hip fracture, and long bone fractures are also risks.[8] In orthopedic surgery, venous stasis can be temporarily provoked by a cessation of blood flow as part of the procedure.[21] Inactivity and immobilization contribute to venous stasis, as with orthopedic casts,[28] paralysis, sitting, long-haul travel, bed rest, hospitalization,[25] and in survivors of acute stroke.[29] Conditions that involve compromised blood flow in the veins are May–Thurner syndrome, where a vein of the pelvis is compressed, and venous thoracic outlet syndrome, which includes Paget–Schroetter syndrome, where compression occurs near the base of the neck.[30][31][32]
Cancer can grow in and around veins, causing venous stasis, and can also stimulate increased levels of tissue factor.[33] Cancers of the bone, ovary, brain, pancreas, and lymphomas are especially associated with increased VTE risk.[27] Chemotherapy treatment also increases risk.[34] Obesity increases the potential of blood to clot, as does pregnancy. In the postpartum, placental tearing releases substances that favor clotting. Oral contraceptives[lower-alpha 2] and hormonal replacement therapy increase the risk through a variety of mechanisms, including altered blood coagulation protein levels and reduced fibrinolysis.[21]

Genetic factors account for approximately 50 to 60% of the variability in VTE rates.[4] Family history of VTE is a risk factor for a first VTE.[36] Genetic factors that increase the risk of VTE include deficiencies of three proteins that normally prevent blood from clotting—protein C, protein S, and antithrombin. Deficiencies in antithrombin, protein C, and protein S[lower-alpha 3] are rare but strong, or moderately strong, risk factors.[25][21] These three deficiencies increase the risk of VTE by about 10 times.[37] Factor V Leiden, which makes factor V resistant to inactivation by activated protein C,[36] mildly increases VTE risk by about three times.[10][36] Having a non-O blood type roughly doubles VTE risk.[21] Non-O blood type is common globally, making it an important risk factor.[38] Individuals without O blood type have higher blood levels of von Willebrand factor and factor VIII than those with O blood type, increasing the likelihood of clotting.[38] Those homozygous for the common fibrinogen gamma gene variant rs2066865 have about a 1.6 times higher risk of VTE.[39] The genetic variant prothrombin G20210A, which increases prothrombin levels,[25] increases risk by about 2.5 times.[10] Additionally, approximately 5% of people have been identified with a background genetic risk comparable to the factor V Leiden and prothrombin G20210A mutations.[10]
Infection, including that of COVID-19, increases risk.[40][41] Inflammatory diseases[21][42] such as Behçet's syndrome,[43] and some autoimmune diseases,[44] such as primary antiphospholipid syndrome[45] and systemic lupus erythematosus (SLE),[46] increase risk. SLE itself is frequently associated with secondary antiphospholipid syndrome.[47] Other associated conditions include heparin-induced thrombocytopenia,[48] thrombotic storm,[49] catastrophic antiphospholipid syndrome,[50] paroxysmal nocturnal hemoglobinuria,[51] nephrotic syndrome,[12] HIV,[12] polycythemia vera,[28] intravenous drug use,[52] and smoking.[lower-alpha 4] Blood alterations including dysfibrinogenemia,[28] low free protein S,[12] activated protein C resistance,[12] hyperhomocysteinemia,[25] high fibrinogen levels,[25] high factor IX levels,[25] and high factor XI levels[25] are associated with increased risk.
Some risk factors influence the location of DVT within the body. In isolated distal DVT, the profile of risk factors appears distinct from proximal DVT. Transient factors, such as surgery and immobilization, appear to dominate, whereas thrombophilias[lower-alpha 5] and age do not seem to increase risk.[55] Common risk factors for having an upper extremity DVT include having an existing foreign body (such as a central venous catheter, a pacemaker, or a triple-lumen PICC line), cancer, and recent surgery.[11]
Classification
The disease term venous thromboembolism (VTE) includes the development of either DVT or pulmonary embolism (PE) or both simultaneously.[3] Provoked DVTs occur in association with acquired risk factors, such as surgery, oral contraceptives, trauma, immobility, obesity, or cancer; cases without acquired states are called unprovoked or idiopathic.[56] Acute DVT is characterized by pain and swelling[57] and is usually occlusive,[58] which means that it obstructs blood flow, whereas non-occlusive DVT is less symptomatic.[59] The label "chronic" has been applied to symptomatic DVT that persists longer than 10 to 14 days.[60] DVT that has no symptoms, but is found only by screening, is labeled asymptomatic or incidental.[61][62] An initial episode of DVT is called incident and any subsequent DVT is termed recurrent.[63][64] Bilateral DVT refers to clots in both legs while unilateral means that only a single leg is affected.[65]
DVT in the legs is proximal when above the knee and distal (or calf) when below the knee.[66][67] DVT below the popliteal vein, a proximal vein behind the knee, is classified as distal[58] and has limited clinical significance compared to proximal DVT.[68] Iliofemoral DVT has been described as involving either the iliac or common femoral vein;[69] elsewhere, it has been defined as involving at a minimum the common iliac vein, which is near the top of the pelvis.[18] Upper extremity DVT occurs in the arms or the base of the neck. A rare and massive DVT that causes significant obstruction is phlegmasia cerulea dolens, so named because of observed cases with a blue or purplish discoloration.[70][71][lower-alpha 6] It is a particularly severe form of acute, proximal, and occlusive DVT. It is life-threatening, limb-threatening, and carries a risk of venous gangrene.[72] It can occur in the arm but more commonly affects the leg.[59][73]
Pathophysiology

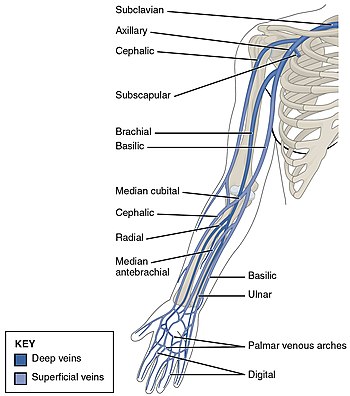
DVT often develops in the calf veins and "grows" in the direction of venous flow, towards the heart.[74] When DVT does not grow, it can be cleared naturally and dissolved into the blood (fibrinolysis).[75] Veins in the leg or pelvis are most commonly affected,[8] including the popliteal vein (behind the knee), femoral vein (of the thigh), and iliac veins of the pelvis. Extensive lower-extremity DVT can even reach into the inferior vena cava (in the abdomen).[76] Upper extremity DVT most commonly affects the subclavian, axillary, and jugular veins.[11]
The causes of arterial thrombosis, such as with heart attacks, are more clearly understood than those of venous thrombosis.[77] With arterial thrombosis, blood vessel wall damage is required, as it initiates coagulation,[77] but clotting in the veins mostly occurs without any such damage.[25] The beginning of venous thrombosis is thought to be caused by tissue factor, which leads to conversion of prothrombin to thrombin, followed by fibrin deposition.[34] Red blood cells and fibrin are the main components of venous thrombi,[25] and the fibrin appears to attach to the blood vessel wall lining (endothelium), a surface that normally acts to prevent clotting.[77] Platelets and white blood cells are also components. Platelets are not as prominent in venous clots as they are in arterial ones, but they can play a role.[21] Inflammation is associated with VTE,[lower-alpha 7] and white blood cells play a role in the formation and resolution of venous clots.[75]

Often, DVT begins in the valves of veins.[75] The blood flow pattern in the valves can cause low oxygen concentrations in the blood (hypoxemia) of a valve sinus. Hypoxemia, which is worsened by venous stasis, activates pathways—ones that include hypoxia-inducible factor-1 and early-growth-response protein 1. Hypoxemia also results in the production of reactive oxygen species, which can activate these pathways, as well as nuclear factor-κB, which regulates hypoxia-inducible factor-1 transcription.[34] Hypoxia-inducible factor-1 and early-growth-response protein 1 contribute to monocyte association with endothelial proteins, such as P-selectin, prompting monocytes to release tissue factor-filled microvesicles, which presumably begin clotting after binding to the endothelial surface.[34]
D-dimers are a fibrin degradation product, a natural byproduct of fibrinolysis that is typically found in the blood. An elevated level[lower-alpha 8] can result from plasmin dissolving a clot—or other conditions.[78] Hospitalized patients often have elevated levels for multiple reasons.[19] Anticoagulation, the standard treatment for DVT, prevents further clot growth and PE, but does not act directly on existing clots.[79]
Diagnosis
A clinical probability assessment using the Wells score (see dedicated column in the table below) to determine if a potential DVT is "likely" or "unlikely" is typically the first step of the diagnostic process. The score is used in suspected first lower extremity DVT (without any PE symptoms) in primary care and outpatient settings, including the emergency department.[1][5] The numerical result (possible score −2 to 9) is most commonly grouped into either "unlikely" or "likely" categories.[1][5] A Wells score of two or more means a DVT is considered "likely" (about a 28% chance), while those with a lower score are considered "unlikely" to have DVT (about a 6% chance).[19] In those unlikely to have DVT, a diagnosis is excluded by a negative D-dimer blood test.[1] In people with likely DVT, ultrasound is the standard imaging used to confirm or exclude a diagnosis.[5] Imaging is also needed for hospital inpatients with suspected DVT and those initially categorized as unlikely to have DVT but who have a positive D-dimer test.[1]
While the Wells score is the predominant and most studied clinical prediction rule for DVT,[19][80] it does have drawbacks. The Wells score requires a subjective assessment regarding the likelihood of an alternate diagnosis and performs less well in the elderly and those with a prior DVT. The Dutch Primary Care Rule has also been validated for use. It contains only objective criteria but requires obtaining a D-dimer value.[81] With this prediction rule, three points or less means a person is at low risk for DVT. A result of four or more points indicates an ultrasound is needed.[81] Instead of using a prediction rule, experienced physicians can make a pre-test DVT probability assessment using clinical assessment and gestalt, but prediction rules are more reliable.[1]
| Criteria | Wells score for DVT[lower-alpha 9] | Dutch Primary Care Rule |
|---|---|---|
| Active cancer (treatment within last 6 months or palliative) | +1 point | +1 point |
| Calf swelling ≥ 3 cm compared to asymptomatic calf (measured 10 cm below tibial tuberosity) | +1 point | +2 points |
| Swollen unilateral superficial veins (non-varicose, in symptomatic leg) | +1 point | +1 point |
| Unilateral pitting edema (in symptomatic leg) | +1 point | — |
| Previous documented DVT | +1 point | — |
| Swelling of entire leg | +1 point | — |
| Localized tenderness along the deep venous system | +1 point | — |
| Paralysis, paresis, or recent cast immobilization of lower extremities | +1 point | — |
| Recently bedridden ≥ 3 days, or major surgery requiring regional or general anesthetic in the past 12 weeks | +1 point | +1 point |
| Alternative diagnosis at least as likely | −2 points | — |
| Positive D-dimer (≥ 0.5 mcg/mL or 1.7 nmol/L) | — | +6 points |
| Absence of leg trauma | — | +1 point |
| Male sex | — | +1 point |
| Use of oral contraceptives | — | +1 point[5][81] |
Compression ultrasonography for suspected deep vein thrombosis is the standard diagnostic method, and it is highly sensitive for detecting an initial DVT.[13] A compression ultrasound is considered positive when the vein walls of normally compressible veins do not collapse under gentle pressure.[19] Clot visualization is sometimes possible, but is not required.[82] Three compression ultrasound scanning techniques can be used, with two of the three methods requiring a second ultrasound some days later to rule out the diagnosis.[13] Whole-leg ultrasound is the option that does not require a repeat ultrasound,[13] but proximal compression ultrasound is frequently used because distal DVT is only rarely clinically significant.[9] Ultrasound methods including duplex and color flow Doppler can be used to further characterize the clot[9] and Doppler ultrasound is especially helpful in the non-compressible iliac veins.[82]
CT scan venography, MRI venography, or a non-contrast MRI are also diagnostic possibilities.[83] The gold standard for judging imaging methods is contrast venography, which involves injecting a peripheral vein of the affected limb with a contrast agent and taking X-rays, to reveal whether the venous supply has been obstructed. Because of its cost, invasiveness, availability, and other limitations, this test is rarely performed.[19]
-
An ultrasound with a blood clot visible in the left common femoral vein. (The common femoral vein is distal to the external iliac vein.)
-
Doppler ultrasonography showing absence of flow and hyperechogenic content in a clotted femoral vein (labeled subsartorial[lower-alpha 10]) distal to the branching point of the deep femoral vein. When compared to this clot, clots that instead obstruct the common femoral vein cause more severe effects due to impacting a significantly larger portion of the leg.[85]
-
An abdominal CT scan demonstrating an iliofemoral DVT, with the clot in the right common iliac vein of the pelvis
Management
Treatment for DVT is warranted when the clots are either proximal, distal and symptomatic, or upper extremity and symptomatic.[2] Providing anticoagulation, or blood-thinning medicine, is the typical treatment after patients are checked to make sure they are not subject to bleeding.[2][lower-alpha 11] However, treatment varies depending upon the location of a DVT. For example, in cases of isolated distal DVT, ultrasound surveillance (a second ultrasound after 2 weeks to check for proximal clots), might be used instead of anticoagulation.[5][87] Although, those with isolated distal DVT at a high-risk of VTE recurrence are typically anticoagulated as if they had proximal DVT. Those at a low-risk for recurrence might receive a four to six week course of anticoagulation, lower doses, or no anticoagulation at all.[5] In contrast, those with proximal DVT should receive at least 3 months of anticoagulation.[5]
Some anticoagulants can be taken by mouth, and these oral medicines include warfarin (a vitamin K antagonist), rivaroxaban (a factor Xa inhibitor), apixaban (a factor Xa inhibitor), dabigatran (a direct thrombin inhibitor), and edoxaban (a factor Xa inhibitor).[2] Other anticoagulants cannot be taken by mouth. These parenteral (non-oral) medicines include low-molecular-weight heparin, fondaparinux, and unfractionated heparin. Some oral medicines are sufficient when taken alone, while others require the use of an additional parenteral blood thinner. Rivaroxaban and apixaban are the typical first-line medicines, and they are sufficient when taken orally.[18] Rivaroxaban is taken once daily, and apixaban is taken twice daily.[5] Warfarin, dabigatran, and edoxaban require the use of a parenteral anticoagulant to initiate oral anticoagulant therapy.[18][88] When warfarin is initiated for VTE treatment, a 5-day minimum of a parenteral anticoagulant[lower-alpha 12] together with warfarin is given, which is followed by warfarin only therapy.[16][17] Warfarin is taken to maintain an international normalized ratio (INR) of 2.0–3.0, with 2.5 as the target.[90] The benefit of taking warfarin declines as the duration of treatment extends,[91] and the risk of bleeding increases with age.[92] Periodic INR monitoring is not necessary when first-line direct oral anticoagulants are used. Overall, anticoagulation therapy is complex and many circumstances can affect how these therapies are managed.[93]
The duration of anticoagulation therapy (whether it will last 4 to 6 weeks,[5] 6 to 12 weeks, 3 to 6 months,[18] or indefinitely) is a key factor in clinical decision making.[94] When proximal DVT is provoked by surgery or trauma a 3-month course of anticoagulation is standard.[18] When a first VTE is proximal DVT that is either unprovoked or associated with transient non-surgical risk factor, low-dose anticoagulation beyond 3 to 6 months might be used.[18] In those with an annual risk of VTE in excess of 9%, as after an unprovoked episode, extended anticoagulation is a possibility.[95] Those who finish warfarin treatment after idiopathic VTE with an elevated D-dimer level show an increased risk of recurrent VTE (about 9% vs about 4% for normal results), and this result might be used in clinical decision making.[96] Thrombophilia test results rarely play a role in the length of treatment.[45]
Treatment for acute leg DVT can continue at home instead of one being hospitalized. This applies as long as individuals feel ready for it, and those with severe leg symptoms or comorbidities would not qualify. An appropriate home environment is expected: one that can provide a quick return to the hospital if necessary, support from family or friends, and phone access.[97] Walking is suggested for those without severe pain or edema.[98] Graduated compression stockings—which apply higher pressure at the ankles and a lower pressure around the knees[89] can be trialed for symptomatic management of acute DVT symptoms, but they are not recommended for reducing the risk of post-thrombotic syndrome,[88] as the potential benefit of using them for this goal "may be uncertain".[5] Nor are compression stockings likely to reduce VTE recurrence.[99] They are, however, recommended in those with isolated distal DVT.[5]
Investigations for cancer
An unprovoked VTE might signal the presence of an unknown cancer, as it is an underlying condition in up to 10% of unprovoked cases.[1] A thorough clinical assessment is needed and should include a physical examination, a review of medical history, and universal cancer screening done in people of that age.[18][100] A review of prior imaging is considered worthwhile, as is "reviewing baseline blood test results including full blood count, renal and hepatic function, PT and APTT."[100] It is not recommended practice to obtain tumor markers or a CT of the abdomen and pelvis in asymptomatic individuals.[1] NICE recommends that further investigations are unwarranted in those without relevant signs or symptoms.[100]
Interventions
Thrombolysis is the injection of an enzyme into the veins to dissolve blood clots, and while this treatment has been proven effective against the life-threatening emergency clots of stroke and heart attacks, randomized controlled trials[101][102][103] have not established a net benefit in those with acute proximal DVT.[5][104] Drawbacks of catheter-directed thrombolysis (the preferred method of administering the clot-busting enzyme[5]) include a risk of bleeding, complexity,[lower-alpha 13] and the cost of the procedure.[88] Thus, anticoagulation is the preferred treatment for DVT.[88] However, this preference does not apply to those with DVT so severe that there is "impending venous gangrene".[88] As of 2016, those thought to be the best candidates for catheter-directed thrombosis have iliofemoral DVT, symptoms for less than 14 days, good functional status (ability to perform one's activities of daily living), life expectancy of at least 1 year, and a low risk of bleeding.[105][needs update][88] Of note, however, is that a variety of contraindications to thrombolysis exist.[88] Catheter-directed thrombolysis against iliofemoral DVT has been associated with a reduction in the severity of post-thrombotic syndrome at an estimated cost-effectiveness ratio of about $138,000[lower-alpha 14] per gained QALY.[106][107] Phlegmasia cerulea dolens (bottom left image) might be treated with catheter-directed thrombolysis.[18] If found in the setting of acute compartment syndrome, an urgent fasciotomy is warranted.[108]
-
A case of phlegmasia cerulea dolens in the left leg
-
A venogram before catheter-directed thrombolysis against Paget–Schroetter syndrome, a rare and severe arm DVT shown here in a judo practitioner, with highly restricted blood flow shown in the vein
-
After treatment with catheter-directed thrombolysis, blood flow in the axillary and subclavian vein were significantly improved. Afterwards, a first rib resection provided thoracic outlet decompression to reduce the risk of recurrent DVT and the risk of sequelae from thoracic outlet compression.[109]

The placement of an inferior vena cava filter (IVC filter) is a potential treatment option when either the standard treatment for acute DVT, anticoagulation, is absolutely contraindicated (not possible), or if someone develops a PE despite being anticoagulated.[100] However, a 2020 NICE review found "little good evidence" for their use.[100] A 2018 study associated IVC filter placement with a 50% reduction in PE, a 70% increase in DVT, and an 18% increase in 30 day mortality when compared to no IVC placement.[1][110] As such, if someone develops a PE despite being anticoagulated, care should be given to optimize anticoagulation treatment and address other related concerns before considering the placement of a IVC filter.[100]
A mechanical thrombectomy device can remove venous clots, although the ACCP considers it an option only when the following conditions apply: "iliofemoral DVT, symptoms for < 7 days (criterion used in the single randomized trial), good functional status, life expectancy of ≥ 1 year, and both resources and expertise are available."[89] Anticoagulation alone is suggested over thrombectomy.[111]
Prevention
For the prevention of blood clots in the general population, incorporating leg exercises and walking when sitting for hours at a time, having an active lifestyle, and maintaining a healthy body weight are recommended.[6] Walking and leg exercises reduce venous stasis because leg muscle contractions compress the veins and pump blood up towards the heart.[112] Excess body weight is modifiable unlike most risk factors, and interventions or lifestyle modifications that help someone who is overweight or obese lose weight reduce DVT risk.[36] Statins have been investigated for primary prevention, and the JUPITER trial, which used rosuvastatin, has provided some tentative evidence of effectiveness.[10][113] Out of all the statins that have been studied, rosuvastatin appears to be the only one with the potential to reduce VTE risk.[114] However, the number needed to treat to prevent one initial VTE is about 2000, limiting its applicability.[115]
After VTE
Anticoagulation, which increases the risk of bleeding, is sometimes used indefinitely (lifelong treatment) in those with a high-risk for recurrence. The risk of major bleeding with long-term anticoagulation is about 3% per year,[37] and the point where annual VTE risk is thought to warrant long-term anticoagulation is estimated to be between 3 and 9%.[95] Usually, only when individuals exceed a 9% annual VTE risk is long-term anticoagulation a common consideration.[95] For example, antithrombin deficiency, a strong or moderately strong risk factor, carries an annual risk of VTE of only 0.8–1.5%;[37] as such, asymptomatic individuals with thrombophilia do not warrant long-term anticoagulation.[116] If someone decides to stop anticoagulation after an unprovoked VTE instead of being on lifelong anticoagulation, aspirin can be used to reduce the risk of recurrence,[117] but it is less effective at preventing VTE than anticoagulation.[citation needed][quantify] Statins have also been investigated for their potential to reduce recurrent VTE rates, with some studies suggesting effectiveness.[118]
Hospital (non-surgical) patients

Acutely ill hospitalized patients are suggested to receive a parenteral anticoagulant, although the potential net benefit is uncertain.[26] Critically ill hospitalized patients are recommended to either receive unfractionated heparin or low-molecular weight heparin instead of foregoing these medicines.[26]
After surgery

Major orthopedic surgery—total hip replacement, total knee replacement, or hip fracture surgery—has a high risk of causing VTE.[119] If prophylaxis is not used after these surgeries, symptomatic VTE has about a 4% chance of developing within 35 days.[120] Following major orthopedic surgery, a blood thinner or aspirin is typically paired with intermittent pneumatic compression, which is the preferred mechanical prophylaxis over graduated compression stockings.[7]
Options for VTE prevention in people following non-orthopedic surgery include early walking, mechanical prophylaxis, and blood thinners (low-molecular-weight heparin and low-dose-unfractionated heparin) depending upon the risk of VTE, risk of major bleeding, and person's preferences.[121] After low-risk surgeries, early and frequent walking is the best preventive measure.[7]
Pregnancy
The risk of VTE is increased in pregnancy by about five times[37][122] because of a more hypercoagulable state, a likely adaptation against fatal postpartum hemorrhage.[123] Additionally, pregnant women with genetic risk factors are subject to a roughly three to 30 times increased risk for VTE.[124] Preventive treatments for pregnancy-related VTE in hypercoagulable women were suggested by the ACCP in 2012. Homozygous carriers of factor V Leiden or prothrombin G20210A with a family history of VTE were suggested for antepartum LMWH and either LMWH or a vitamin K antagonist (VKA) for the six weeks following childbirth. Those with another thrombophilia and a family history but no previous VTE were suggested for watchful waiting during pregnancy and LMWH or—for those without protein C or S deficiency—a VKA. Homozygous carriers of factor V Leiden or prothrombin G20210A with no personal or family history of VTE were suggested for watchful waiting during pregnancy and LMWH or a VKA for six weeks after childbirth. Those with another thrombophilia but no family or personal history of VTE were suggested for watchful waiting only.[125] Warfarin, a common VKA, can cause harm to the fetus and is not used for VTE prevention during pregnancy.[124][126]
Travelers

Suggestions for at-risk long-haul travelers[lower-alpha 15] include calf exercises, frequent walking, and aisle seating in airplanes to ease walking.[127][128] Graduated compression stockings have sharply reduced the levels of asymptomatic DVT in airline passengers, but the effect on symptomatic DVT, PE, or mortality is unknown, as none of the individuals studied developed these outcomes.[129] However, graduated compression stockings are not suggested for long-haul travelers (>4 hours) without risk factors for VTE. Likewise, neither aspirin nor anticoagulants are suggested in the general population undertaking long-haul travel.[26] Those with significant VTE risk factors[lower-alpha 16] undertaking long-haul travel are suggested to use either graduated compression stockings or LMWH for VTE prevention. If neither of these two methods are feasible, then aspirin is suggested.[26]
Prognosis
As DVT is most frequently a disease of older age that occurs in the context of nursing homes, hospitals, and active cancer,[3] DVT is associated with a 30-day mortality rate of about 6%.[1] PE is the cause of most of these deaths.[1] Proximal DVT is frequently associated with PE, unlike distal DVT, which is rarely if ever associated with PE.[19] Around 56% of those with proximal DVT also have PE, although a chest CT is not needed simply because of the presence of a DVT.[1] If proximal DVT is left untreated, in the following 3 months approximately half of people will experience symptomatic PE.[8]
Another frequent complication of proximal DVT, and the most frequent chronic complication, is post-thrombotic syndrome, where individuals have chronic venous symptoms.[5] Symptoms can include pain, itching, swelling, paresthesia, a sensation of heaviness, and in severe cases, leg ulcers.[5] After proximal DVT, an estimated 20–50% of people develop the syndrome, with 5–10% experiencing severe symptoms.[130] Post-thrombotic syndrome can also be a complication of distal DVT, though to a lesser extent than with proximal DVT.[131]
Recurrence of DVT is another potential consequence. In the 10 years following an initial VTE, about 30% of people will have a recurrence.[132][3] VTE recurrence in those with prior DVT is more likely to recur as DVT than PE.[133] Cancer[5] and unprovoked DVT are strong risk factors for recurrence.[24] After initial proximal unprovoked DVT with and without PE, 16–17% of people will have recurrent VTE in the 2 years after they complete their course of anticoagulants. VTE recurrence is less common in distal DVT than proximal DVT.[134] In upper extremity DVT, annual VTE recurrence is about 2–4%.[92] After surgery, a provoked proximal DVT or PE has an annual recurrence rate of only 0.7%.[24]
Epidemiology
About 1.5 out of 1000 adults a year have a first VTE in high-income countries,[135][136] and about 5–11% of people will develop VTE in their lifetime.[12][13] VTE becomes much more common with age.[12] VTE rarely occurs in children, but when it does, it predominantly affects hospitalized children.[137] Children in North America and the Netherlands have VTE rates that range from 0.07 to 0.49 out of 10,000 children annually.[137] Meanwhile, almost 1% of those aged 85 and above experience VTE each year.[3] About 60% of all VTEs occur in those 70 years of age or older,[8] and those aged 65 and above are subject to about a 15 times higher risk than those aged 40 and below.[14] Incidence is about 18% higher in males than in females.[4] VTE occurs in association with hospitalization or nursing home residence about 60% of the time, active cancer about 20% of the time, and a central venous catheter or transvenous pacemaker about 9% of the time.[3]
During pregnancy and after childbirth, acute VTE occurs about 1.2 of 1000 deliveries. Despite it being relatively rare, it is a leading cause of maternal morbidity and mortality.[138] After surgery with preventive treatment, VTE develops in about 10 of 1000 people after total or partial knee replacement, and in about 5 of 1000 after total or partial hip replacement.[139] About 400,000 Americans develop an initial VTE each year, with 100,000 deaths or more attributable to PE.[136] In England, an estimated 25,000 a year die from hospital-related VTE.[140] Asian and Hispanic individuals have a lower VTE risk than whites or blacks.[4]
In North American and European populations, around 4–8% of people have a thrombophilia,[37] most commonly factor V leiden and prothrombin G20210A. For populations in China, Japan, and Thailand, deficiences in protein S, protein C, and antithrombin predominate.[141] Non-O blood type is present in around 50% of the general population and varies with ethnicity, and it is present in about 70% of those with VTE.[38][142] Altogether, global data is incomplete,[143] and as of 2011, available data was dominated by North American and European populations.[15]
DVT occurs in the upper extremities in about 4–10% of cases,[11] with an incidence of 0.4–1.0 people out of 10,000 a year.[5] A minority of upper extremity DVTs are due to Paget–Schroetter syndrome, also called effort thrombosis, which occurs in 1–2 people out of 100,000 a year, usually in athletic males around 30 years of age or in those who do significant amounts of overhead manual labor.[31][109]
Society and culture

Being on blood thinners because of DVT can be life-changing for patients because it may prevent them from continuing lifestyle activities such as contact or winter sports to prevent bleeding episodes after potential injuries.[145] Head injuries prompting brain bleeds are of particular concern. This has caused NASCAR driver Brian Vickers to forego participation in races. Professional basketball players including NBA players Chris Bosh and hall of famer Hakeem Olajuwon have dealt with recurrent blood clots,[146] and Bosh's career was significantly hampered by DVT and PE.[147]
Tennis star Serena Williams was hospitalized in 2011 for PE thought to have originated from a DVT.[148] Years later, in 2017, due to her knowledge of DVT and PE, Serena accurately advocated for herself to have a PE diagnosed and treated. During this encounter with VTE, she was hospitalized after a C-section surgery and was off of blood thinners. After feeling the sudden onset of a PE symptom, shortness of breath, she told her nurse and requested a CT scan and an IV heparin drip, all while gasping for air. She started to receive an ultrasound to look for DVT in the legs, prompting her to express dissatisfaction to the medical staff that they were not looking for clots where she had symptoms (her lungs), and they were not yet treating her presumed PE. After being diagnosed with PE and not DVT, and after receiving heparin by IV, the coughing from the PE caused her C-section surgical site to open and the heparin contributed to bleeding at the site. Serena later received an IVC filter while in the hospital.[144]
Other notable people have been affected by DVT. Former US President Richard Nixon had recurrent DVT,[149] and so has former Secretary of State Hillary Clinton. She was first diagnosed while First Lady in 1998 and again in 2009.[150] Dick Cheney was diagnosed with an episode while Vice President,[151] and TV show host Regis Philbin had a DVT after hip-replacement surgery.[152] DVT has also contributed to the deaths of famous people. For example, DVT and PE played a role in rapper Heavy D's death at age 44.[153] NBC journalist David Bloom died at age 39 while covering the Iraq War from a PE that was thought to have progressed from a missed DVT.[154] And actor Jimmy Stewart had a DVT that progressed to a PE and triggered a fatal heart attack when he was 89.[152][155]
Field of medicine
Patients with a history of DVT might be managed by primary care, general internal medicine, hematology, cardiology, vascular surgery, or vascular medicine.[156] Patients suspected of having an acute DVT are often referred to the emergency department for evaluation.[157] Interventional radiology is the specialty that typically places and retrieves IVC filters,[158] and vascular surgery might do catheter directed thrombosis for some severe DVTs.[109]
History

The earliest case of DVT was described by Sushruta in his book Sushruta Samhita around 600–900 BC.[159] The next case was not described until 1271, in the leg of a 20-year-old male.[159][160] At some point, the increased incidence of DVT in women after childbirth was noticed, and in the late 1700s, a public health recommendation was issued to encourage women to breastfeed as a means to prevent this phenomenon; the DVT was called "milk leg", as it was thought to result from milk building up in the leg.[161]
In 1856, German physician and pathologist Rudolf Virchow published what is referred to as Virchow's triad, the three major causes of thrombosis.[12][161] The triad provides the theoretical framework for the current explanation of venous thrombosis,[12] although it was focused on the effect of a foreign body in the venous system and the conditions required for clot propagation.[162]
Methods to observe DVT by ultrasound were established in the 1960s.[83] Diagnoses were commonly performed by impedance plethysmography in the 1970s and 1980s, but ultrasound, particularly after utility of probe compression was demonstrated in 1986, became the preferred diagnostic method.[159][163] Yet, in the mid 1990s, contrast venography and impedance plethysmography were still described as common.[164]
Multiple pharmacological therapies for DVT were introduced in the 20th century: oral anticoagulants in the 1940s, subcutaneous injections of LDUH in 1962 and subcutaneous injections of LMWH in 1982.[165] For around 50 years, a months-long warfarin (Coumadin) regimen was the mainstay of pharmacological treatment.[166][167] To avoid the blood monitoring required with warfarin and the injections required by heparin and heparin-like medicines, a new generation of oral anticoagulant pills that do not require blood monitoring has sought to replace these traditional anticoagulants.[167] In the late 2000s to early 2010s, direct oral anticoagulants—including rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa)—came to the market, making this field of medicine fast changing.[24] The New York Times described a "furious battle" among the three makers of these drugs "for the prescription pads of doctors".[166]
Economics
Initial DVT costs for an average hospitalized patient in the U.S. are around $7,700–$10,800.[168] VTE follow-up costs at three months, six months, and a year are about $5,000, $10,000, and $33,000 respectively; in Europe, the three and six-month figures are about €1,800 and €3,200.[169] Post-thrombotic syndrome is a significant contributor to DVT follow-up costs.[168] Annual DVT costs in the U.S. are an estimated $5 billion[170] or in excess of $8 billion,[171][172] and the average annual cost per treated individual is thought to be about $20,000.[171] As an example, if 300,000 symptomatic DVT patients were treated at costs averaging $20,000 annually, that would cost $6 billion a year.
Research directions
A 2019 study published in Nature Genetics reported more than doubling the known genetic loci associated with VTE.[10] In their updated 2018 clinical practice guidelines, the American Society of Hematology identified 29 separate research priorities, most of which related to patients who are acutely or critically ill.[26] Inhibition of Factor XI, P-selectin, E-selectin, and a reduction in formation of neutrophil extracellular traps are potential therapies that might treat VTE without increasing bleeding risk.[173]
See also
- Disseminated intravascular coagulation
- Superficial vein thrombosis
- Thrombotic microangiopathy
- HELLP syndrome
- Deaths from thrombosis
Notes
- ↑ Thrombosis associated with the head (cerebral venous sinus thrombosis) and the abdominal organs (viscera)—such as portal vein thrombosis, renal vein thrombosis, and Budd–Chiari syndrome—are separate diseases excluded from the scope of this definition.
- ↑ Third-generation combined oral contraceptives (COCs) have an approximate two to three times higher risk than second-generation COCs.[27] Progestogen-only pill use is not associated with increased VTE risk.[35]
- ↑ Type I[12]
- ↑ "It is important to note that smoking is not an independent risk factor, although it increases the risk for cancers and other comorbidities and works synergistically with other independent risk factors."[53]
- ↑ The term 'thrombophilia' as used here applies to the five inherited abnormalities of antithrombin, protein C, protein S, factor V, and prothrombin, as is done elsewhere.[37][54]
- ↑ Cerulea is from Latin, and denotes a bluish color, as does the related English word cerulean.
- ↑ VTE might cause the observed inflammation.[21]
- ↑ An elevated level is greater than 250 ng/mL D-dimer units (DDU) or greater than 0.5 μg/mL fibrinogen equivalent units (FEU). A normal level is below these values.[78]
- ↑ The Wells score as displayed here is the more recent modified score, which added a criteron for a previous documented DVT and increased the time range after a surgery to 12 weeks from 4 weeks.[9]
- ↑ (Subsartorial is a proposed name for a section of the femoral vein.)[84]
- ↑ Evidence for anticoagulation comes from studies other than definitive randomized controlled trials that demonstrate efficacy and safety for anticoagulation vs. placebo or using NSAIDs.[86]
- ↑ The international normalized ratio should be ≥ 2.0 for 24 hours minimum,[17] but if the ratio is > 3.0, then the parenteral anticoagulant is not needed for five days.[89]
- ↑ "Up to 83% of patients treated by any catheter-based therapy, need adjunctive angioplasty, and stenting".[5]
- ↑ Estimated in United States dollars, estimate published in 2019
- ↑ Specified as those with "previous VTE, recent surgery or trauma, active malignancy, pregnancy, estrogen use, advanced age, limited mobility, severe obesity, or known thrombophilic disorder"
- ↑ For example "recent surgery, history of VTE, postpartum women, active malignancy, or ≥2 risk factors, including combinations of the above with hormone replacement therapy, obesity, or pregnancy"[26]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Kruger PC, Eikelboom JW, Douketis JD, Hankey GJ (June 2019). "Deep vein thrombosis: update on diagnosis and management". The Medical Journal of Australia. 210 (11): 516–524. doi:10.5694/mja2.50201. PMID 31155730.
- ↑ 2.0 2.1 2.2 2.3 Bartholomew JR (December 2017). "Update on the management of venous thromboembolism". Cleveland Clinic Journal of Medicine. 84 (12 Suppl 3): 39–46. doi:10.3949/ccjm.84.s3.04. PMID 29257737.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Heit JA, Spencer FA, White RH (January 2016). "The epidemiology of venous thromboembolism". Journal of Thrombosis and Thrombolysis. 41 (1): 3–14. doi:10.1007/s11239-015-1311-6. PMC 4715842. PMID 26780736.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Crous-Bou M, Harrington LB, Kabrhel C (November 2016). "Environmental and Genetic Risk Factors Associated with Venous Thromboembolism". Seminars in Thrombosis and Hemostasis. 42 (8): 808–820. doi:10.1055/s-0036-1592333. PMC 5146955. PMID 27764878.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 5.15 5.16 5.17 5.18 5.19 5.20 5.21 5.22 5.23 Mazzolai L, Aboyans V, Ageno W, Agnelli G, Alatri A, Bauersachs R, et al. (December 2018). "Diagnosis and management of acute deep vein thrombosis: a joint consensus document from the European Society of Cardiology working groups of aorta and peripheral vascular diseases and pulmonary circulation and right ventricular function". European Heart Journal. 39 (47): 4208–4218. doi:10.1093/eurheartj/ehx003. PMID 28329262.
- ↑ 6.0 6.1 "What is Venous Thromboembolism?". Centers for Disease Control and Prevention. 14 March 2019. Archived from the original on 7 May 2019. Retrieved 6 January 2020.
- ↑ 7.0 7.1 7.2 7.3 Anderson DR, Morgano GP, Bennett C, Dentali F, Francis CW, Garcia DA, et al. (December 2019). "American Society of Hematology 2019 guidelines for management of venous thromboembolism: prevention of venous thromboembolism in surgical hospitalized patients". Blood Advances. 3 (23): 3898–3944. doi:10.1182/bloodadvances.2019000975. PMC 6963238. PMID 31794602.
- ↑ 8.0 8.1 8.2 8.3 8.4 Phillippe HM (December 2017). "Overview of venous thromboembolism". The American Journal of Managed Care. 23 (20 Suppl): S376–S382. PMID 29297660. Archived from the original on 30 January 2020. Retrieved 2 August 2020.
- ↑ 9.0 9.1 9.2 9.3 9.4 Stone J, Hangge P, Albadawi H, Wallace A, Shamoun F, Knuttien MG, et al. (December 2017). "Deep vein thrombosis: pathogenesis, diagnosis, and medical management". Cardiovascular Diagnosis and Therapy. 7 (Suppl 3): S276–S284. doi:10.21037/cdt.2017.09.01. PMC 5778510. PMID 29399531.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 Klarin D, Busenkell E, Judy R, Lynch J, Levin M, Haessler J, et al. (November 2019). "Genome-wide association analysis of venous thromboembolism identifies new risk loci and genetic overlap with arterial vascular disease" (PDF). Nature Genetics. 51 (11): 1574–1579. doi:10.1038/s41588-019-0519-3. PMC 6858581. PMID 31676865. Archived (PDF) from the original on 28 January 2020. Retrieved 2 August 2020.
- ↑ 11.0 11.1 11.2 11.3 11.4 Heil J, Miesbach W, Vogl T, Bechstein WO, Reinisch A (April 2017). "Deep Vein Thrombosis of the Upper Extremity". Deutsches Ärzteblatt International. 114 (14): 244–249. doi:10.3238/arztebl.2017.0244. PMC 5415909. PMID 28446351.
- ↑ 12.00 12.01 12.02 12.03 12.04 12.05 12.06 12.07 12.08 12.09 12.10 Lijfering WM, Rosendaal FR, Cannegieter SC (June 2010). "Risk factors for venous thrombosis - current understanding from an epidemiological point of view". British Journal of Haematology. 149 (6): 824–33. doi:10.1111/j.1365-2141.2010.08206.x. PMID 20456358.
- ↑ 13.0 13.1 13.2 13.3 13.4 Wells PS, Ihaddadene R, Reilly A, Forgie MA (January 2018). "Diagnosis of Venous Thromboembolism: 20 Years of Progress". Annals of Internal Medicine. 168 (2): 131–140. doi:10.7326/M17-0291. PMID 29310137.
- ↑ 14.0 14.1 Faller N, Limacher A, Méan M, Righini M, Aschwanden M, Beer JH, et al. (February 2017). "Predictors and Causes of Long-Term Mortality in Elderly Patients with Acute Venous Thromboembolism: A Prospective Cohort Study". The American Journal of Medicine. 130 (2): 198–206. doi:10.1016/j.amjmed.2016.09.008. PMID 27742261.
- ↑ 15.0 15.1 Zakai NA, McClure LA (October 2011). "Racial differences in venous thromboembolism". Journal of Thrombosis and Haemostasis. 9 (10): 1877–82. doi:10.1111/j.1538-7836.2011.04443.x. PMID 21797965.
- ↑ 16.0 16.1 Keeling D, Alikhan R (June 2013). "Management of venous thromboembolism – controversies and the future". British Journal of Haematology. 161 (6): 755–63. doi:10.1111/bjh.12306. PMID 23531017.
- ↑ 17.0 17.1 17.2 Guyatt et al. 2012, p. 20S: 2.4.
- ↑ 18.00 18.01 18.02 18.03 18.04 18.05 18.06 18.07 18.08 18.09 18.10 Tran HA, Gibbs H, Merriman E, Curnow JL, Young L, Bennett A, et al. (March 2019). "New guidelines from the Thrombosis and Haemostasis Society of Australia and New Zealand for the diagnosis and management of venous thromboembolism". The Medical Journal of Australia. 210 (5): 227–235. doi:10.5694/mja2.50004. PMID 30739331.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 19.6 Bates SM, Jaeschke R, Stevens SM, Goodacre S, Wells PS, Stevenson MD, et al. (February 2012). "Diagnosis of DVT: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e351S–e418S. doi:10.1378/chest.11-2299. PMC 3278048. PMID 22315267.
- ↑ Arumilli BR, Lenin Babu V, Paul AS (January 2008). "Painful swollen leg—think beyond deep vein thrombosis or Baker's cyst". World Journal of Surgical Oncology. 6: 6. doi:10.1186/1477-7819-6-6. PMC 2244628. PMID 18205917.
- ↑ 21.0 21.1 21.2 21.3 21.4 21.5 21.6 21.7 Reitsma PH, Versteeg HH, Middeldorp S (March 2012). "Mechanistic view of risk factors for venous thromboembolism". Arteriosclerosis, Thrombosis, and Vascular Biology. 32 (3): 563–8. doi:10.1161/ATVBAHA.111.242818. PMID 22345594.
- ↑ Kujovich JL (January 2011). "Factor V Leiden thrombophilia". Genetics in Medicine. 13 (1): 1–16. doi:10.1097/GIM.0b013e3181faa0f2. PMID 21116184.
- ↑ Tzoran I, Hoffman R, Monreal M (October 2018). "Hemostasis and Thrombosis in the Oldest Old". Seminars in Thrombosis and Hemostasis. 44 (7): 624–631. doi:10.1055/s-0038-1657779. PMID 29920621.
- ↑ 24.0 24.1 24.2 24.3 Keeling D, Alikhan R (June 2013). "Management of venous thromboembolism--controversies and the future". British Journal of Haematology. 161 (6): 755–63. doi:10.1111/bjh.12306. PMID 23531017.
- ↑ 25.0 25.1 25.2 25.3 25.4 25.5 25.6 25.7 25.8 25.9 Martinelli I, Bucciarelli P, Mannucci PM (February 2010). "Thrombotic risk factors: basic pathophysiology". Critical Care Medicine. 38 (2 Suppl): S3-9. doi:10.1097/CCM.0b013e3181c9cbd9. PMID 20083911.
- ↑ 26.0 26.1 26.2 26.3 26.4 26.5 26.6 Schünemann HJ, Cushman M, Burnett AE, Kahn SR, Beyer-Westendorf J, Spencer FA, et al. (November 2018). "American Society of Hematology 2018 guidelines for management of venous thromboembolism: prophylaxis for hospitalized and nonhospitalized medical patients". Blood Advances. 2 (22): 3198–3225. doi:10.1182/bloodadvances.2018022954. PMC 6258910. PMID 30482763.
- ↑ 27.0 27.1 27.2 Wong P, Baglin T (2012). "Epidemiology, risk factors and sequelae of venous thromboembolism". Phlebology. 27 (Suppl 2): 2–11. doi:10.1258/phleb.2012.012S31. PMID 22457300.
- ↑ 28.0 28.1 28.2 Rosendaal FR, Reitsma PH (July 2009). "Genetics of venous thrombosis". Journal of Thrombosis and Haemostasis. 7 (Suppl 1): 301–4. doi:10.1111/j.1538-7836.2009.03394.x. PMID 19630821.
- ↑ Winstein CJ, Stein J, Arena R, Bates B, Cherney LR, Cramer SC, et al. (June 2016). "Guidelines for Adult Stroke Rehabilitation and Recovery: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association". Stroke. 47 (6): e98–e169. doi:10.1161/STR.0000000000000098. PMID 27145936.
- ↑ Béliard S, Feuvrier D, Ducroux E, Salomon du Mont L (2018). "May Thurner syndrome revealed by left calf venous claudication during running, a case report". BMC Sports Science, Medicine & Rehabilitation. 10: 3. doi:10.1186/s13102-018-0092-6. PMC 5796503. PMID 29435334.
- ↑ 31.0 31.1 Hangge P, Rotellini-Coltvet L, Deipolyi AR, Albadawi H, Oklu R (December 2017). "Paget-Schroetter syndrome: treatment of venous thrombosis and outcomes". Cardiovascular Diagnosis and Therapy. 7 (Suppl 3): S285–S290. doi:10.21037/cdt.2017.08.15. PMC 5778512. PMID 29399532.
- ↑ Jabri H, Mukherjee S, Sanghavi D, Chalise S (2014). "Bilateral Upper Extremity DVT in a 43-Year-Old Man: Is It Thoracic Outlet Syndrome?!". Case Reports in Medicine. 2014: 758010. doi:10.1155/2014/758010. PMC 4129160. PMID 25140182.
- ↑ Falanga A, Russo L, Milesi V, Vignoli A (October 2017). "Mechanisms and risk factors of thrombosis in cancer". Critical Reviews in Oncology/Hematology. 118: 79–83. doi:10.1016/j.critrevonc.2017.08.003. PMID 28917273.
- ↑ 34.0 34.1 34.2 34.3 Bovill EG, van der Vliet A (2011). "Venous valvular stasis-associated hypoxia and thrombosis: what is the link?". Annual Review of Physiology. 73: 527–45. doi:10.1146/annurev-physiol-012110-142305. PMID 21034220.
- ↑ Mantha S, Karp R, Raghavan V, Terrin N, Bauer KA, Zwicker JI (August 2012). "Assessing the risk of venous thromboembolic events in women taking progestin-only contraception: a meta-analysis". BMJ. 345: e4944. doi:10.1136/bmj.e4944. PMC 3413580. PMID 22872710.
- ↑ 36.0 36.1 36.2 36.3 Shaheen K, Alraies MC, Alraiyes AH, Christie R (April 2012). "Factor V Leiden: how great is the risk of venous thromboembolism?". Cleveland Clinic Journal of Medicine. 79 (4): 265–72. doi:10.3949/ccjm.79a.11072. PMID 22473726. Archived from the original on 28 August 2021. Retrieved 2 August 2020.
- ↑ 37.0 37.1 37.2 37.3 37.4 37.5 Varga EA, Kujovich JL (January 2012). "Management of inherited thrombophilia: guide for genetics professionals". Clinical Genetics. 81 (1): 7–17. doi:10.1111/j.1399-0004.2011.01746.x. PMID 21707594.
- ↑ 38.0 38.1 38.2 Dentali F, Sironi AP, Ageno W, Turato S, Bonfanti C, Frattini F, et al. (July 2012). "Non-O blood type is the commonest genetic risk factor for VTE: results from a meta-analysis of the literature". Seminars in Thrombosis and Hemostasis. 38 (5): 535–48. doi:10.1055/s-0032-1315758. PMID 22740183.
- ↑ Paulsen B, Skille H, Smith EN, Hveem K, Gabrielsen ME, Brækkan SK, et al. (October 2019). "Fibrinogen gamma gene rs2066865 and risk of cancer-related venous thromboembolism". Haematologica. 105 (7): 1963–1968. doi:10.3324/haematol.2019.224279. PMC 7327659. PMID 31582554.
- ↑ Beristain-Covarrubias N, Perez-Toledo M, Thomas MR, Henderson IR, Watson SP, Cunningham AF (2019). "Understanding Infection-Induced Thrombosis: Lessons Learned From Animal Models". Frontiers in Immunology. 10: 2569. doi:10.3389/fimmu.2019.02569. PMC 6848062. PMID 31749809.
- ↑ Zhai Z, Li C, Chen Y, Gerotziafas G, Zhang Z, Wan J, et al. (April 2020). "Prevention and Treatment of Venous Thromboembolism Associated with Coronavirus Disease 2019 Infection: A Consensus Statement before Guidelines" (PDF). Thrombosis and Haemostasis. 120 (6): 937–948. doi:10.1055/s-0040-1710019. PMC 7295267. PMID 32316065. Archived (PDF) from the original on 10 July 2020. Retrieved 2 August 2020.
- ↑ Tichelaar YI, Kluin-Nelemans HJ, Meijer K (May 2012). "Infections and inflammatory diseases as risk factors for venous thrombosis. A systematic review". Thrombosis and Haemostasis. 107 (5): 827–37. doi:10.1160/TH11-09-0611. PMID 22437808.
- ↑ Becatti M, Emmi G, Bettiol A, Silvestri E, Di Scala G, Taddei N, Prisco D, Fiorillo C (March 2019). "Behçet's syndrome as a tool to dissect the mechanisms of thrombo-inflammation: clinical and pathogenetic aspects". Clinical and Experimental Immunology. 195 (3): 322–333. doi:10.1111/cei.13243. PMC 6378375. PMID 30472725.
- ↑ Zöller B, Li X, Sundquist J, Sundquist K (January 2012). "Risk of pulmonary embolism in patients with autoimmune disorders: a nationwide follow-up study from Sweden". Lancet. 379 (9812): 244–9. doi:10.1016/S0140-6736(11)61306-8. PMID 22119579.
- ↑ 45.0 45.1 Baglin T (April 2012). "Inherited and acquired risk factors for venous thromboembolism". Seminars in Respiratory and Critical Care Medicine. 33 (2): 127–37. doi:10.1055/s-0032-1311791. PMID 22648484.
- ↑ Knight CL, Nelson-Piercy C (2017). "Management of systemic lupus erythematosus during pregnancy: challenges and solutions". Open Access Rheumatology: Research and Reviews. 9: 37–53. doi:10.2147/OARRR.S87828. PMC 5354538. PMID 28331377.
- ↑ Svenungsson E, Antovic A (January 2020). "The antiphospholipid syndrome – often overlooked cause of vascular occlusions?". Journal of Internal Medicine. 287 (4): 349–372. doi:10.1111/joim.13022. PMID 31957081.
- ↑ Greinacher A, Selleng K, Warkentin TE (November 2017). "Autoimmune heparin-induced thrombocytopenia". Journal of Thrombosis and Haemostasis. 15 (11): 2099–2114. doi:10.1111/jth.13813. PMID 28846826.
- ↑ Rana MA, Mady AF, Lashari AA, Eltreafi R, Fischer-Orr N, Naser K (2018). "Lethal End of Spectrum of Clots-Thrombotic Storm". Case Reports in Critical Care. 2018: 7273420. doi:10.1155/2018/7273420. PMC 5994281. PMID 29977623.
- ↑ Abdul Haium AA, Sheppard M, Rubens M, Daubeney P (July 2013). "Catastrophic antiphospholipid syndrome in childhood: presentation with an inferior caval vein mass". BMJ Case Reports. 2013: bcr2013010043. doi:10.1136/bcr-2013-010043. PMC 3736204. PMID 23861282.
- ↑ Lazo-Langner A, Kovacs MJ, Hedley B, Al-Ani F, Keeney M, Louzada ML, et al. (June 2015). "Screening of patients with idiopathic venous thromboembolism for paroxysmal nocturnal hemoglobinuria clones". Thrombosis Research. 135 (6): 1107–9. doi:10.1016/j.thromres.2015.04.006. PMID 25890452.
- ↑ Kyrle PA, Eichinger S (2005). "Deep vein thrombosis". Lancet. 365 (9465): 1163–74. doi:10.1016/S0140-6736(05)71880-8. PMID 15794972.
- ↑ McLendon K, Attia M (2019). "Deep Venous Thrombosis (DVT) Risk Factors". StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. PMID 29262230. Archived from the original on 12 November 2020. Retrieved 2 August 2020.
- ↑ Middeldorp S (2011). "Is thrombophilia testing useful?". Hematology. American Society of Hematology. Education Program. 2011 (1): 150–5. doi:10.1182/asheducation-2011.1.150. PMID 22160027.
- ↑ Palareti G, Schellong S (January 2012). "Isolated distal deep vein thrombosis: what we know and what we are doing". Journal of Thrombosis and Haemostasis. 10 (1): 11–9. doi:10.1111/j.1538-7836.2011.04564.x. PMID 22082302.
- ↑ Iorio A, Kearon C, Filippucci E, Marcucci M, Macura A, Pengo V, et al. (October 2010). "Risk of recurrence after a first episode of symptomatic venous thromboembolism provoked by a transient risk factor: a systematic review". Archives of Internal Medicine. 170 (19): 1710–6. doi:10.1001/archinternmed.2010.367. PMID 20975016.
- ↑ Conklin P, Soares GM, Dubel GJ, Ahn SH, Murphy TP (December 2009). "Acute deep vein thrombosis (DVT): evolving treatment strategies and endovascular therapy" (PDF). Medicine and Health, Rhode Island. 92 (12): 394–7. PMID 20066826. Archived (PDF) from the original on 6 February 2013.
- ↑ 58.0 58.1 Scarvelis D, Wells PS (October 2006). "Diagnosis and treatment of deep-vein thrombosis". CMAJ. 175 (9): 1087–92. doi:10.1503/cmaj.060366. PMC 1609160. PMID 17060659.
Scarvelis D, Wells PS (November 2007). "Correction: Diagnosis and treatment of deep-vein thrombosis". CMAJ. 177 (11): 1392. doi:10.1503/cmaj.071550. - ↑ 59.0 59.1 Owings JT (2005). "Management of venous thromboembolism". ACS Surgery. American College of Surgeons. Archived from the original on 27 January 2012. Retrieved 16 January 2012.
- ↑ Rao AS, Konig G, Leers SA, Cho J, Rhee RY, Makaroun MS, et al. (November 2009). "Pharmacomechanical thrombectomy for iliofemoral deep vein thrombosis: an alternative in patients with contraindications to thrombolysis". Journal of Vascular Surgery. 50 (5): 1092–8. doi:10.1016/j.jvs.2009.06.050. PMID 19782528.
- ↑ Lloyd NS, Douketis JD, Moinuddin I, Lim W, Crowther MA (March 2008). "Anticoagulant prophylaxis to prevent asymptomatic deep vein thrombosis in hospitalized medical patients: a systematic review and meta-analysis". Journal of Thrombosis and Haemostasis. 6 (3): 405–14. doi:10.1111/j.1538-7836.2007.02847.x. PMID 18031292.
- ↑ Font C, Farrús B, Vidal L, Caralt TM, Visa L, Mellado B, et al. (September 2011). "Incidental versus symptomatic venous thrombosis in cancer: a prospective observational study of 340 consecutive patients". Annals of Oncology. 22 (9): 2101–6. doi:10.1093/annonc/mdq720. PMID 21325446. Archived from the original on 15 April 2013. Retrieved 2 August 2020.
- ↑ Heit JA, Mohr DN, Silverstein MD, Petterson TM, O'Fallon WM, Melton LJ (March 2000). "Predictors of recurrence after deep vein thrombosis and pulmonary embolism: a population-based cohort study". Archives of Internal Medicine. 160 (6): 761–8. doi:10.1001/archinte.160.6.761. PMID 10737275.
- ↑ Spencer FA, Emery C, Lessard D, Anderson F, Emani S, Aragam J, et al. (July 2006). "The Worcester Venous Thromboembolism study: a population-based study of the clinical epidemiology of venous thromboembolism". Journal of General Internal Medicine. 21 (7): 722–7. doi:10.1111/j.1525-1497.2006.00458.x. PMC 1924694. PMID 16808773.
- ↑ Casella IB, Bosch MA, Sabbag CR (2009). "Incidence and risk factors for bilateral deep venous thrombosis of the lower limbs". Angiology. 60 (1): 99–103. doi:10.1177/0003319708316897. PMID 18504268.
- ↑ Johnson SA, Stevens SM, Woller SC, Lake E, Donadini M, Cheng J, et al. (February 2010). "Risk of deep vein thrombosis following a single negative whole-leg compression ultrasound: a systematic review and meta-analysis". JAMA. 303 (5): 438–45. doi:10.1001/jama.2010.43. PMID 20124539.
- ↑ Welch 2010, p. 2.
- ↑ Galanaud JP, Bosson JL, Quéré I (September 2011). "Risk factors and early outcomes of patients with symptomatic distal vs. proximal deep-vein thrombosis". Current Opinion in Pulmonary Medicine. 17 (5): 387–91. doi:10.1097/MCP.0b013e328349a9e3. PMID 21832920.
- ↑ Comerota AJ, Kearon C, Gu CS, Julian JA, Goldhaber SZ, Kahn SR, et al. (February 2019). "Endovascular Thrombus Removal for Acute Iliofemoral Deep Vein Thrombosis". Circulation. 139 (9): 1162–1173. doi:10.1161/CIRCULATIONAHA.118.037425. PMC 6389417. PMID 30586751.
- ↑ Chinsakchai K, Ten Duis K, Moll FL, de Borst GJ (January 2011). "Trends in management of phlegmasia cerulea dolens". Vascular and Endovascular Surgery. 45 (1): 5–14. doi:10.1177/1538574410388309. PMID 21193462.
- ↑ Turner DPB (November 1952). "A case of phlegmasia cerulea dolens". British Medical Journal. 2 (4795): 1183–5. doi:10.1136/bmj.2.4795.1183. PMC 2021962. PMID 12997687.
- ↑ Aggarwal DG, Bhojraj SS, Behrainwalla AA, Jani CK, Mehta SS (January 2018). "Phlegmasia Cerulea Dolens Following Heparin-Induced Thrombocytopenia". Indian Journal of Critical Care Medicine. 22 (1): 51–52. doi:10.4103/ijccm.IJCCM_183_16. PMC 5793026. PMID 29422736.
- ↑ Mazer BA, Hughes PG (November 2018). "Pacemaker-associated Phlegmasia Cerulea Dolens Treated with Catheter-directed Thrombolysis". Clinical Practice and Cases in Emergency Medicine. 2 (4): 316–319. doi:10.5811/cpcem.2018.8.39444. PMC 6230348. PMID 30443615.
- ↑ Chan WS, Spencer FA, Ginsberg JS (April 2010). "Anatomic distribution of deep vein thrombosis in pregnancy". CMAJ. 182 (7): 657–60. doi:10.1503/cmaj.091692. PMC 2855912. PMID 20351121.
- ↑ 75.0 75.1 75.2 Saha P, Humphries J, Modarai B, Mattock K, Waltham M, Evans CE, et al. (March 2011). "Leukocytes and the natural history of deep vein thrombosis: current concepts and future directions". Arteriosclerosis, Thrombosis, and Vascular Biology. 31 (3): 506–12. doi:10.1161/ATVBAHA.110.213405. PMC 3079895. PMID 21325673.
- ↑ Kim ES, Bartholomew JR. "Venous thromboembolism". Disease Management Project. Cleveland Clinic. Archived from the original on 23 February 2011. Retrieved 15 February 2011.
- ↑ 77.0 77.1 77.2 López JA, Chen J (2009). "Pathophysiology of venous thrombosis". Thrombosis Research. 123 (Suppl 4): S30-4. doi:10.1016/S0049-3848(09)70140-9. PMID 19303501.
- ↑ 78.0 78.1 "DDI/9290 clinical: D-dimer, plasma". Mayo Medical Laboratories. Archived from the original on 8 October 2012. Retrieved 27 August 2012.
- ↑ Vedantham S, Goldhaber SZ, Kahn SR, Julian J, Magnuson E, Jaff MR, et al. (April 2013). "Rationale and design of the ATTRACT Study: a multicenter randomized trial to evaluate pharmacomechanical catheter-directed thrombolysis for the prevention of postthrombotic syndrome in patients with proximal deep vein thrombosis". American Heart Journal. 165 (4): 523–530.e3. doi:10.1016/j.ahj.2013.01.024. PMC 3612268. PMID 23537968.
- ↑ Geersing GJ, Zuithoff NP, Kearon C, Anderson DR, Ten Cate-Hoek AJ, Elf JL, et al. (March 2014). "Exclusion of deep vein thrombosis using the Wells rule in clinically important subgroups: individual patient data meta-analysis". BMJ. 348: g1340. doi:10.1136/bmj.g1340. PMC 3948465. PMID 24615063.
- ↑ 81.0 81.1 81.2 Pyzocha N (December 2019). "Diagnosing DVT in nonpregnant adults in the primary care setting". American Family Physician. 100 (12): 778–780. PMID 31845779.
- ↑ 82.0 82.1 Le Gal G, Righini M (June 2015). "Controversies in the diagnosis of venous thromboembolism". Journal of Thrombosis and Haemostasis. 13 Suppl 1: S259–65. doi:10.1111/jth.12937. PMID 26149033.
- ↑ 83.0 83.1 Rahaghi FN, Minhas JK, Heresi GA (September 2018). "Diagnosis of Deep Venous Thrombosis and Pulmonary Embolism: New Imaging Tools and Modalities". Clinics in Chest Medicine. 39 (3): 493–504. doi:10.1016/j.ccm.2018.04.003. PMC 6317734. PMID 30122174.
- ↑ Häggström, M (January 2019). "Subsartorial Vessels as Replacement Names for Superficial Femoral Vessels" (PDF). International Journal of Anatomy, Radiology and Surgery. 8 (1): AV01–AV02. doi:10.7860/IJARS/2019/40329:2458. Archived (PDF) from the original on 27 September 2020. Retrieved 2 August 2020.
- ↑ Jaff MR, McMurtry MS, Archer SL, Cushman M, Goldenberg N, Goldhaber SZ, Jenkins JS, Kline JA, Michaels AD, Thistlethwaite P, Vedantham S, White RJ, Zierler BK (April 2011). "Management of massive and submassive pulmonary embolism, iliofemoral deep vein thrombosis, and chronic thromboembolic pulmonary hypertension: a scientific statement from the American Heart Association". Circulation. 123 (16): 1788–830. doi:10.1161/CIR.0b013e318214914f. PMID 21422387.
- ↑ Cundiff DK, Manyemba J, Pezzullo JC (January 2006). Cundiff DK (ed.). "Anticoagulants versus non-steroidal anti-inflammatories or placebo for treatment of venous thromboembolism". The Cochrane Database of Systematic Reviews (1): CD003746. doi:10.1002/14651858.CD003746.pub2. PMID 16437461.
- ↑ Fleck D, Albadawi H, Wallace A, Knuttinen G, Naidu S, Oklu R (December 2017). "Below-knee deep vein thrombosis (DVT): diagnostic and treatment patterns". Cardiovascular Diagnosis and Therapy. 7 (Suppl 3): S134–S139. doi:10.21037/cdt.2017.11.03. PMC 5778527. PMID 29399516.
- ↑ 88.0 88.1 88.2 88.3 88.4 88.5 88.6 Kearon C, Akl EA, Ornelas J, Blaivas A, Jimenez D, Bounameaux H, et al. (February 2016). "Antithrombotic therapy for VTE disease: CHEST guideline and expert panel report". Chest. 149 (2): 315–352. doi:10.1016/j.chest.2015.11.026. PMID 26867832.
- ↑ 89.0 89.1 89.2 Kearon C, Akl EA, Comerota AJ, Prandoni P, Bounameaux H, Goldhaber SZ, et al. (February 2012). "Antithrombotic therapy for VTE disease: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e419S–e496S. doi:10.1378/chest.11-2301. PMC 3278049. PMID 22315268.
- ↑ Guyatt et al. 2012, p. 22S: 3.2.
- ↑ Middeldorp S, Prins MH, Hutten BA (August 2014). "Duration of treatment with vitamin K antagonists in symptomatic venous thromboembolism". The Cochrane Database of Systematic Reviews (8): CD001367. doi:10.1002/14651858.CD001367.pub3. PMC 7074008. PMID 25092359.
- ↑ 92.0 92.1 de Jong PG, Coppens M, Middeldorp S (August 2012). "Duration of anticoagulant therapy for venous thromboembolism: balancing benefits and harms on the long term". British Journal of Haematology. 158 (4): 433–41. doi:10.1111/j.1365-2141.2012.09196.x. PMID 22734929.
- ↑ Witt DM, Nieuwlaat R, Clark NP, Ansell J, Holbrook A, Skov J, et al. (November 2018). "American Society of Hematology 2018 guidelines for management of venous thromboembolism: optimal management of anticoagulation therapy". Blood Advances. 2 (22): 3257–3291. doi:10.1182/bloodadvances.2018024893. PMC 6258922. PMID 30482765.
- ↑ Kearon C, Kahn SR (January 2020). "Long-term treatment of venous thromboembolism". Blood. 135 (5): 317–325. doi:10.1182/blood.2019002364. PMID 31917402.
- ↑ 95.0 95.1 95.2 Keeling D, Baglin T, Tait C, Watson H, Perry D, Baglin C, et al. (August 2011). "Guidelines on oral anticoagulation with warfarin – fourth edition". British Journal of Haematology. 154 (3): 311–24. doi:10.1111/j.1365-2141.2011.08753.x. PMID 21671894.
- ↑ Douketis J, Tosetto A, Marcucci M, Baglin T, Cushman M, Eichinger S, et al. (October 2010). "Patient-level meta-analysis: effect of measurement timing, threshold, and patient age on ability of D-dimer testing to assess recurrence risk after unprovoked venous thromboembolism". Annals of Internal Medicine. 153 (8): 523–31. doi:10.7326/0003-4819-153-8-201010190-00009. PMID 20956709.
- ↑ Guyatt et al. 2012, p. 21S: 2.7.
- ↑ Guyatt et al. 2012, p. 21S: 2.14.
- ↑ Berntsen CF, Kristiansen A, Akl EA, Sandset PM, Jacobsen EM, Guyatt G, et al. (April 2016). "Compression Stockings for Preventing the Postthrombotic Syndrome in Patients with Deep Vein Thrombosis". The American Journal of Medicine. 129 (4): 447.e1–447.e20. doi:10.1016/j.amjmed.2015.11.031. PMID 26747198.
- ↑ 100.0 100.1 100.2 100.3 100.4 100.5 National Institute for Health and Care Excellence. "NICE Guideline 148: Venous thromboembolic diseases: diagnosis, management and thrombophilia testing Archived 10 September 2020 at the Wayback Machine" London, 26 March 2020.
- ↑ Enden T, Haig Y, Kløw NE, Slagsvold CE, Sandvik L, Ghanima W, et al. (January 2012). "Long-term outcome after additional catheter-directed thrombolysis versus standard treatment for acute iliofemoral deep vein thrombosis (the CaVenT study): a randomised controlled trial". Lancet. 379 (9810): 31–8. doi:10.1016/S0140-6736(11)61753-4. PMID 22172244.
- ↑ Haig Y, Enden T, Grøtta O, Kløw NE, Slagsvold CE, Ghanima W, et al. (February 2016). "Post-thrombotic syndrome after catheter-directed thrombolysis for deep vein thrombosis (CaVenT): 5-year follow-up results of an open-label, randomised controlled trial". The Lancet Haematology. 3 (2): e64–71. doi:10.1016/S2352-3026(15)00248-3. PMID 26853645.
- ↑ Vedantham S, Goldhaber SZ, Julian JA, Kahn SR, Jaff MR, Cohen DJ, et al. (December 2017). "Pharmacomechanical Catheter-Directed Thrombolysis for Deep-Vein Thrombosis". The New England Journal of Medicine. 377 (23): 2240–2252. doi:10.1056/NEJMoa1615066. PMC 5763501. PMID 29211671.
- ↑ Bhandari, Tamara (6 December 2017). "Clot-busting drugs not recommended for most patients with blood clots". Washington University School of Medicine. Archived from the original on 30 January 2020. Retrieved 21 January 2020.
- ↑ National Institute for Health and Clinical Excellence. Clinical guideline 144: Venous thromboembolic diseases: the management of venous thromboembolic diseases and the role of thrombophilia testing. London, 2012.
- ↑ Comerota AJ, Kearon C, Gu CS, Julian JA, Goldhaber SZ, Kahn SR, et al. (February 2019). "Endovascular Thrombus Removal for Acute Iliofemoral Deep Vein Thrombosis". Circulation. 139 (9): 1162–1173. doi:10.1161/CIRCULATIONAHA.118.037425. PMC 6389417. PMID 30586751.
- ↑ Magnuson EA, Chinnakondepalli K, Vilain K, Kearon C, Julian JA, Kahn SR, et al. (October 2019). "Cost-Effectiveness of Pharmacomechanical Catheter-Directed Thrombolysis Versus Standard Anticoagulation in Patients With Proximal Deep Vein Thrombosis: Results From the ATTRACT Trial". Circulation. Cardiovascular Quality and Outcomes. 12 (10): e005659. doi:10.1161/CIRCOUTCOMES.119.005659. PMID 31592728.
- ↑ Abdul W, Hickey B, Wilson C (April 2016). "Lower extremity compartment syndrome in the setting of iliofemoral deep vein thrombosis, phlegmasia cerulea dolens and factor VII deficiency". BMJ Case Reports. 2016: bcr2016215078. doi:10.1136/bcr-2016-215078. PMC 4854131. PMID 27113791.
- ↑ 109.0 109.1 109.2 Ijaopo R, Oguntolu V, DCosta D, Garnham A, Hobbs S (March 2016). "A case of Paget-Schroetter syndrome (PSS) in a young judo tutor: a case report". Journal of Medical Case Reports. 10: 63. doi:10.1186/s13256-016-0848-0. PMC 4797165. PMID 26987584.
- ↑ Turner TE, Saeed MJ, Novak E, Brown DL (July 2018). "Association of Inferior Vena Cava Filter Placement for Venous Thromboembolic Disease and a Contraindication to Anticoagulation With 30-Day Mortality". JAMA Network Open. 1 (3): e180452. doi:10.1001/jamanetworkopen.2018.0452. PMC 6324296. PMID 30646021.
- ↑ Guyatt et al. 2012, p. 21S: 2.11.
- ↑ Hecht 2010, p. 47.
- ↑ Li L, Zhang P, Tian JH, Yang K (December 2014). "Statins for primary prevention of venous thromboembolism". The Cochrane Database of Systematic Reviews (12): CD008203. doi:10.1002/14651858.CD008203.pub3. PMID 25518837.
- ↑ Kunutsor SK, Seidu S, Khunti K (February 2017). "Statins and primary prevention of venous thromboembolism: a systematic review and meta-analysis" (PDF). The Lancet Haematology. 4 (2): e83–e93. doi:10.1016/S2352-3026(16)30184-3. PMID 28089655. Archived (PDF) from the original on 21 April 2020. Retrieved 2 August 2020.
- ↑ Biere-Rafi S, Hutten BA, Squizzato A, Ageno W, Souverein PC, de Boer A, et al. (June 2013). "Statin treatment and the risk of recurrent pulmonary embolism". European Heart Journal. 34 (24): 1800–6. doi:10.1093/eurheartj/eht046. PMID 23396492.
- ↑ Guyatt et al. 2012, p. 11S: 7.1.
- ↑ Wigle P, Hein B, Bernheisel CR (October 2019). "Anticoagulation: Updated Guidelines for Outpatient Management". American Family Physician. 100 (7): 426–434. PMID 31573167.
- ↑ Wallace A, Albadawi H, Hoang P, Fleck A, Naidu S, Knuttinen G, et al. (December 2017). "Statins as a preventative therapy for venous thromboembolism". Cardiovascular Diagnosis and Therapy. 7 (Suppl 3): S207–S218. doi:10.21037/cdt.2017.09.12. PMC 5778529. PMID 29399524.
- ↑ Sobieraj DM, Lee S, Coleman CI, Tongbram V, Chen W, Colby J, et al. (May 2012). "Prolonged versus standard-duration venous thromboprophylaxis in major orthopedic surgery: a systematic review". Annals of Internal Medicine. 156 (10): 720–7. doi:10.7326/0003-4819-156-10-201205150-00423. PMID 22412039.
- ↑ Falck-Ytter Y, Francis CW, Johanson NA, Curley C, Dahl OE, Schulman S, et al. (February 2012). "Prevention of VTE in orthopedic surgery patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e278S–e325S. doi:10.1378/chest.11-2404. PMC 3278063. PMID 22315265.
- ↑ Gould MK, Garcia DA, Wren SM, Karanicolas PJ, Arcelus JI, Heit JA, et al. (February 2012). "Prevention of VTE in nonorthopedic surgical patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e227S–e277S. doi:10.1378/chest.11-2297. PMC 3278061. PMID 22315263.
- ↑ Marik PE, Plante LA (November 2008). "Venous thromboembolic disease and pregnancy". The New England Journal of Medicine. 359 (19): 2025–33. doi:10.1056/NEJMra0707993. PMID 18987370.
- ↑ Jackson E, Curtis KM, Gaffield ME (March 2011). "Risk of venous thromboembolism during the postpartum period: a systematic review". Obstetrics and Gynecology. 117 (3): 691–703. doi:10.1097/AOG.0b013e31820ce2db. PMID 21343773.
- ↑ 124.0 124.1 Bates SM, Greer IA, Middeldorp S, Veenstra DL, Prabulos AM, Vandvik PO (February 2012). "VTE, thrombophilia, antithrombotic therapy, and pregnancy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e691S–e736S. doi:10.1378/chest.11-2300. PMC 3278054. PMID 22315276.
- ↑ Guyatt et al. 2012, pp. 39S–40S: 3.0.
- ↑ Guyatt et al. 2012, p. 38S: 3.0.1.
- ↑ Guyatt et al. 2012, p. 11S: 6.1.1.
- ↑ "New DVT guidelines: No evidence to support "economy-class syndrome"". American College of Chest Physicians. 7 February 2012. Archived from the original on 3 June 2016. Retrieved 10 February 2012.
oral contraceptives, sitting in a window seat, advanced age, and pregnancy increase DVT risk in long-distance travelers
- ↑ Clarke MJ, Broderick C, Hopewell S, Juszczak E, Eisinga A (September 2016). "Compression stockings for preventing deep vein thrombosis in airline passengers". The Cochrane Database of Systematic Reviews. 9: CD004002. doi:10.1002/14651858.CD004002.pub3. PMC 6457834. PMID 27624857.
- ↑ Galanaud JP, Monreal M, Kahn SR (April 2018). "Epidemiology of the post-thrombotic syndrome". Thrombosis Research. 164: 100–109. doi:10.1016/j.thromres.2017.07.026. PMID 28844444.
- ↑ Galanaud JP, Righini M, Le Collen L, Douillard A, Robert-Ebadi H, Pontal D, et al. (January 2020). "Long-term risk of postthrombotic syndrome after symptomatic distal deep vein thrombosis: The CACTUS-PTS study". Journal of Thrombosis and Haemostasis. 18 (4): 857–864. doi:10.1111/jth.14728. PMID 31899848.
- ↑ Beckman MG, Hooper WC, Critchley SE, Ortel TL (April 2010). "Venous thromboembolism: a public health concern". American Journal of Preventive Medicine. 38 (4 Suppl): S495–501. doi:10.1016/j.amepre.2009.12.017. PMID 20331949.
- ↑ Konstantinides SV, Torbicki A, Agnelli G, Danchin N, Fitzmaurice D, Galiè N, et al. (November 2014). "2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism". European Heart Journal. 35 (43): 3033–69, 3069a–3069k. doi:10.1093/eurheartj/ehu283. PMID 25173341. Archived from the original on 19 November 2016. Retrieved 2 August 2020.
- ↑ Khan F, Rahman A, Carrier M, Kearon C, Weitz JI, Schulman S, et al. (July 2019). "Long term risk of symptomatic recurrent venous thromboembolism after discontinuation of anticoagulant treatment for first unprovoked venous thromboembolism event: systematic review and meta-analysis". BMJ. 366: l4363. doi:10.1136/bmj.l4363. PMC 6651066. PMID 31340984.
- ↑ Johannesen CD, Flachs EM, Ebbehøj NE, Marott JL, Jensen GB, Nordestgaard BG, et al. (January 2020). "Sedentary work and risk of venous thromboembolism". Scandinavian Journal of Work, Environment & Health. 46 (1): 69–76. doi:10.5271/sjweh.3841. PMID 31385593.
- ↑ 136.0 136.1 Grosse SD, Nelson RE, Nyarko KA, Richardson LC, Raskob GE (January 2016). "The economic burden of incident venous thromboembolism in the United States: A review of estimated attributable healthcare costs". Thrombosis Research. 137: 3–10. doi:10.1016/j.thromres.2015.11.033. PMC 4706477. PMID 26654719.
- ↑ 137.0 137.1 Monagle P, Cuello CA, Augustine C, Bonduel M, Brandão LR, Capman T, et al. (November 2018). "American Society of Hematology 2018 Guidelines for management of venous thromboembolism: treatment of pediatric venous thromboembolism". Blood Advances. 2 (22): 3292–3316. doi:10.1182/bloodadvances.2018024786. PMC 6258911. PMID 30482766.
- ↑ Bates SM, Rajasekhar A, Middeldorp S, McLintock C, Rodger MA, James AH, et al. (November 2018). "American Society of Hematology 2018 guidelines for management of venous thromboembolism: venous thromboembolism in the context of pregnancy". Blood Advances. 2 (22): 3317–3359. doi:10.1182/bloodadvances.2018024802. PMC 6258928. PMID 30482767.
- ↑ Januel JM, Chen G, Ruffieux C, Quan H, Douketis JD, Crowther MA, et al. (January 2012). "Symptomatic in-hospital deep vein thrombosis and pulmonary embolism following hip and knee arthroplasty among patients receiving recommended prophylaxis: a systematic review". JAMA. 307 (3): 294–303. doi:10.1001/jama.2011.2029. PMID 22253396.
- ↑ Young A, Chapman O, Connor C, Poole C, Rose P, Kakkar AK (July 2012). "Thrombosis and cancer". Nature Reviews. Clinical Oncology. 9 (8): 437–49. doi:10.1038/nrclinonc.2012.106. PMID 22777060.
- ↑ Margaglione M, Grandone E (February 2011). "Population genetics of venous thromboembolism. A narrative review". Thrombosis and Haemostasis. 105 (2): 221–31. doi:10.1160/TH10-08-0510. PMID 20941456.
- ↑ "Blood types". American Red Cross. Archived from the original on 14 August 2012. Retrieved 15 August 2012.
- ↑ Hamasaki N (October 2012). "Unmasking Asian thrombophilia: is APC dysfunction the real culprit?". Journal of Thrombosis and Haemostasis. 10 (10): 2016–8. doi:10.1111/j.1538-7836.2012.04893.x. PMID 22905992.
- ↑ 144.0 144.1 Haskell, Rob (10 January 2018). "Serena Williams on Motherhood, Marriage, and Making Her Comeback". Vogue. Archived from the original on 22 January 2020. Retrieved 22 January 2020.
- ↑ Golemi I, Salazar Adum JP, Tafur A, Caprini J (August 2019). "Venous thromboembolism prophylaxis using the Caprini score". Disease-a-month : DM. 65 (8): 249–298. doi:10.1016/j.disamonth.2018.12.005. PMID 30638566.
- ↑ Perez AJ (17 February 2016). "Expert: Chris Bosh, like many, at risk of blood clot recurrence". USA Today. Archived from the original on 30 January 2020. Retrieved 22 January 2020.
- ↑ Martin, Jill (4 May 2016). "Chris Bosh officially out as Heat make playoff push". CNN. Archived from the original on 30 January 2020. Retrieved 22 January 2020.
- ↑ Moisse, Katie (2 March 2011). "Serena Williams Hospitalized After Pulmonary Embolism". ABC News. Archived from the original on 30 January 2020. Retrieved 22 January 2020.
- ↑ Pascarella L, Pappas TN (February 2013). "Phlebitis, pulmonary emboli and presidential politics: Richard M. Nixon's complicated deep vein thrombosis". The American Surgeon. 79 (2): 128–34. doi:10.1177/000313481307900222. PMID 23336651.
- ↑ Frankel, Todd C. (11 September 2016). "Hillary Clinton has not been quick to share health information". The Washington Post. Archived from the original on 31 January 2020. Retrieved 22 January 2020.
- ↑ "Cheney diagnosed with deep-vein thrombosis". The Guardian. 6 March 2007. Archived from the original on 30 January 2020. Retrieved 22 January 2020.
- ↑ 152.0 152.1 Rodriguez, Diana (12 October 2018). "11 Celebrities Who Battled Deep Vein Thrombosis Risk". Everyday Health. Archived from the original on 30 January 2020. Retrieved 22 January 2020.
- ↑ "Coroner: Rapper Heavy D died of blood clot in lung". CNN. 27 December 2011. Archived from the original on 30 January 2020. Retrieved 22 January 2020.
- ↑ "My husband should be living today". TODAY. 3 March 2005. Archived from the original on 23 May 2019. Retrieved 22 January 2020.
- ↑ Eliot, Mark (2006). Jimmy Stewart: A Biography. New York: Random House. p. 409. ISBN 9781400052226.
- ↑ Moll, Stephan (9 May 2012). "What Kind of Doctor Do I Need?". Clot Connect. Archived from the original on 28 January 2020. Retrieved 28 January 2020.
- ↑ Kitchen L, Lawrence M, Speicher M, Frumkin K (July 2016). "Emergency Department Management of Suspected Calf-Vein Deep Venous Thrombosis: A Diagnostic Algorithm". The Western Journal of Emergency Medicine. 17 (4): 384–90. doi:10.5811/westjem.2016.5.29951. PMC 4944794. PMID 27429688.
- ↑ "Inferior Vena Cava (IVC) Filter Placement". Johns Hopkins Medicine. 2020. Archived from the original on 28 January 2020. Retrieved 28 January 2020.
- ↑ 159.0 159.1 159.2 Goodman LR (October 2013). "In search of venous thromboembolism: the first 2913 years". AJR. American Journal of Roentgenology. 201 (4): W576-81. doi:10.2214/AJR.13.10604. PMID 24059395.
- ↑ Galanaud JP, Laroche JP, Righini M (March 2013). "The history and historical treatments of deep vein thrombosis". Journal of Thrombosis and Haemostasis. 11 (3): 402–11. doi:10.1111/jth.12127. PMID 23297815.
- ↑ 161.0 161.1 Rosendaal 2009, p. 3.
- ↑ Bagot CN, Arya R (October 2008). "Virchow and his triad: a question of attribution". British Journal of Haematology. 143 (2): 180–90. doi:10.1111/j.1365-2141.2008.07323.x. PMID 18783400.
- ↑ Dalen 2003, p. 3.
- ↑ Line BR, Peters TL, Keenan J (January 1997). "Diagnostic test comparisons in patients with deep venous thrombosis" (PDF). Journal of Nuclear Medicine. 38 (1): 89–92. PMID 8998158. Archived (PDF) from the original on 28 August 2021. Retrieved 2 August 2020.
- ↑ Dalen 2003, p. 2.
- ↑ 166.0 166.1 Ornstein, Charles; Jones, Ryann Grochowski (7 January 2015). "The Drugs That Companies Promote to Doctors Are Rarely Breakthroughs". The New York Times. Archived from the original on 22 September 2020.
- ↑ 167.0 167.1 Franchini M, Mannucci PM (September 2016). "Direct oral anticoagulants and venous thromboembolism". European Respiratory Review. 25 (141): 295–302. doi:10.1183/16000617.0025-2016. PMID 27581829.
- ↑ 168.0 168.1 Dobesh PP (August 2009). "Economic burden of venous thromboembolism in hospitalized patients". Pharmacotherapy. 29 (8): 943–53. doi:10.1592/phco.29.8.943. PMID 19637948.
- ↑ Ruppert A, Steinle T, Lees M (2011). "Economic burden of venous thromboembolism: a systematic review". Journal of Medical Economics. 14 (1): 65–74. doi:10.3111/13696998.2010.546465. PMID 21222564.
- ↑ Grosse SD (January 2012). "Incidence-based cost estimates require population-based incidence data. A critique of Mahan et al" (PDF). Thrombosis and Haemostasis. 107 (1): 192–3, author reply 194–5. doi:10.1160/TH11-09-0666. PMID 22159589. Archived (PDF) from the original on 8 August 2017.
- ↑ 171.0 171.1 Mahan CE, Holdsworth MT, Welch SM, Borrego M, Spyropoulos AC (September 2011). "Deep-vein thrombosis: a United States cost model for a preventable and costly adverse event". Thrombosis and Haemostasis. 106 (3): 405–15. doi:10.1160/TH11-02-0132. PMID 21833446.
- ↑ Mahan CE, Holdsworth MT, Welch SM, et al. (2012). "Long-term attack rates, as compared with incidence rates, may provide improved cost-estimates in venous thromboembolism. A reply to S. D. Grosse". Thromb Haemost. 107 (1): 194–5. doi:10.1160/TH11-11-0802.
- ↑ Metz AK, Diaz JA, Obi AT, Wakefield TW, Myers DD, Henke PK (2018). "Venous Thrombosis and Post-Thrombotic Syndrome: From Novel Biomarkers to Biology". Methodist DeBakey Cardiovascular Journal. 14 (3): 173–181. doi:10.14797/mdcj-14-3-173 (inactive 26 July 2020). PMC 6217569. PMID 30410646.
{{cite journal}}: CS1 maint: DOI inactive as of July 2020 (link)
- Cited literature
- Dalen, James E. (2003). Venous thromboembolism. CRC Press. ISBN 978-0-8247-5645-1. Archived from the original on 20 June 2013. Retrieved 2 August 2020.
- Guyatt GH, Akl EA, Crowther M, Gutterman DD, Schuünemann HJ (February 2012). "Executive summary: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): 7S–47S. doi:10.1378/chest.1412S3. PMC 3278060. PMID 22315257.
{{cite journal}}: Cite has empty unknown parameters:|1=and|2=(help) - Hecht ME (2010). A practical guide to hip surgery: From pre-op to recovery. Sunrise River Press. ISBN 978-1-934716-12-0. Archived from the original on 31 December 2013. Retrieved 2 August 2020.
- Rosendaal, Frits R. (2009). van Beek, Edwin J. R.; Büller, Harry R.; Oudkerk, Mathijs (eds.). Deep vein thrombosis and pulmonary embolism. John Wiley & Sons. ISBN 978-0-470-74499-4. Archived from the original on 20 June 2013. Retrieved 2 August 2020.
- Welch, Ellen (2010). Venous thromboembolism: A nurse's guide to prevention and management. John Wiley & Sons. ISBN 978-0-470-51189-3. Archived from the original on 25 November 2020. Retrieved 2 August 2020.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1: long volume value
- Webarchive template wayback links
- CS1 maint: DOI inactive as of July 2020
- Articles with hatnote templates targeting a nonexistent page
- Use dmy dates from January 2020
- Articles with invalid date parameter in template
- Good articles
- Pages using multiple image with auto scaled images
- Wikipedia articles in need of updating from May 2020
- All Wikipedia articles in need of updating
- All articles with unsourced statements
- Articles with unsourced statements from February 2020
- CS1 errors: empty unknown parameters
- Coagulopathies
- Diseases of veins, lymphatic vessels and lymph nodes
- Hematology
- RTT

![Doppler ultrasonography showing absence of flow and hyperechogenic content in a clotted femoral vein (labeled subsartorial[lower-alpha 10]) distal to the branching point of the deep femoral vein. When compared to this clot, clots that instead obstruct the common femoral vein cause more severe effects due to impacting a significantly larger portion of the leg.[85]](https://upload.wikimedia.org/wikipedia/commons/thumb/4/4f/Ultrasonography_of_deep_vein_thrombosis_of_the_femoral_vein_-annotated.jpg/250px-Ultrasonography_of_deep_vein_thrombosis_of_the_femoral_vein_-annotated.jpg)




![After treatment with catheter-directed thrombolysis, blood flow in the axillary and subclavian vein were significantly improved. Afterwards, a first rib resection provided thoracic outlet decompression to reduce the risk of recurrent DVT and the risk of sequelae from thoracic outlet compression.[109]](https://upload.wikimedia.org/wikipedia/commons/thumb/6/6e/A-case-of-Paget-Schroetter-syndrome-%28PSS%29-in-a-young-judo-tutor-a-case-report-13256_2016_848_Fig2_HTML.jpg/196px-A-case-of-Paget-Schroetter-syndrome-%28PSS%29-in-a-young-judo-tutor-a-case-report-13256_2016_848_Fig2_HTML.jpg)