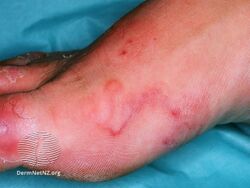
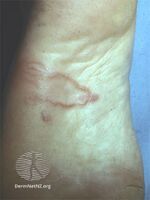
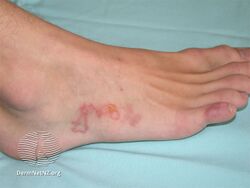
Cutaneous larva migrans
| Cutaneous larva migrans | |
|---|---|
| Other names: CLM | |
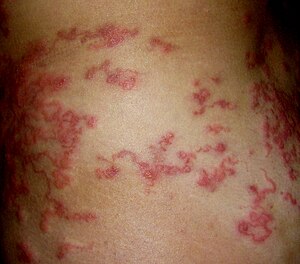 | |
| Typical "creeping eruption" associated with cutaneous larva migrans | |
Cutaneous larva migrans (abbreviated CLM) is a skin disease in humans, caused by the larvae of various nematode parasites of the hookworm family (Ancylostomatidae).[1] These parasites live in the intestines of dogs, cats, and wild animals and should not be confused with other members of the hookworm family for which humans are definitive hosts, namely Ancylostoma duodenale and Necator americanus.
Colloquially called creeping eruption[2][3] due to its presentation, the disease is also somewhat ambiguously known as "ground itch" or (in some parts of the Southern USA) "sandworms", as the larvae like to live in sandy soil. Another vernacular name is plumber's itch. The medical term CLM literally means "wandering larvae in the skin".
Symptoms and signs
The infection causes a red, intensely pruritic (itchy) eruption, and may look like twirling lesions.[4] The itching can become very painful and if scratched may allow a secondary bacterial infection to develop. Cutaneous larva migrans usually heals spontaneously over weeks to months and has been known to last as long as one year.[5] However, the severity of the symptoms usually causes those infected to seek medical treatment before spontaneous resolution occurs. Following proper treatment, migration of the larvae within the skin is halted and relief of the associated itching can occur in less than 48 hours (reported for thiabendazole).[2]
This is separate from the similar cutaneous larva currens which is caused by Strongyloides. Larva currens is also a cause of migratory pruritic eruptions but is marked by 1) migratory speed on the order of inches per hour 2) perianal involvement due to autoinfection from stool and 3) a wide band of urticaria.[6]
-
Cutaneous larva migrans
-
Cutaneous larva migrans
-
Cutaneous larva migrans
-
Cutaneous larva migrans
Cause
Hookworm eggs are shed in the infected dog (or other animal) feces to the ground and beach sand, where they then develop over a period of 1–2 weeks into the infectious larval form (filariform larvae).[7] The filariform larvae can burrow through intact skin that comes into contact with soil or sand that is contaminated with feces. Although they are able to infect the deeper tissues of animals (through to the lungs and then the intestinal tract), humans are incidental hosts and the larvae are only able to penetrate the epidermis of the skin[2] and thus create the typical wormlike burrows visible underneath the skin. These parasites apparently lack the collagenase enzymes required to penetrate through the basement membrane deeper into the dermal layers of the skin.[8]
Treatment
CLM can be treated in a number of different ways:
- Systemic (oral) agents include albendazole[2][3] (trade name Albenza)[9] and ivermectin[2] (trade name Stromectol).[10]
- Another agent which can be applied either topically or taken by mouth is thiabendazole[2][3] (trade name Mintezol),[11] an anti-helminthic.
- Topical freezing agents, such as ethylene chloride or liquid nitrogen,[2] applied locally can freeze and kill the larvae, but this method has a high failure rate because the larvae are usually located away from the site of the visible skin trails. Additionally, this is a painful method which can cause blistering and/or ulceration of the skin and it is therefore not recommended.[2]
- It is recommended to use Benadryl or some anti-itch cream (i.e. Cortizone or Calamine lotion). This will help relieve some of the itch.[citation needed]
- Wearing shoes in areas where these parasites are known to be endemic offers protection from infection.[2] In general, avoiding exposure of skin to contaminated soil or sand offers the best protection. In some areas dogs have been prohibited from beaches in an attempt to control human infection.[2]
See also
References
- ↑ Morris-Jones, Rachel (2019). "117. Insect bites and infestations". In Morris-Jones, Rachael (ed.). ABC of Dermatology (7th ed.). Hoboken: Wiley Blackwell. p. 145. ISBN 978-1-119-48899-6. Archived from the original on 2023-07-18. Retrieved 2023-07-15.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Caumes, E. (1 May 2000). "Treatment of Cutaneous Larva Migrans". Clinical Infectious Diseases. 30 (5): 811–814. doi:10.1086/313787. PMID 10816151.
- ↑ 3.0 3.1 3.2 Albanese, G; Caterina Venturi; Giuseppe Galbiati (2001). "Treatment of larva migrans cutanea (creeping eruption): a comparison between albendazole and traditional therapy". International Journal of Dermatology. 40 (1): 67–71. doi:10.1046/j.1365-4362.2001.01103.x. PMID 11277961.
- ↑ "About Cutaneous Larva Migrans". Heathline. Heathline. Archived from the original on 14 January 2020. Retrieved 13 January 2020.
- ↑ Chaudhry, AZ; Lonworth DL (1989). "Cutaneous manifestations of intestinal helminthic infections". Dermatol Clin. 7 (2): 275–90. doi:10.1016/S0733-8635(18)30599-0. PMID 2670373.
- ↑ ARTHUR, ROBERT P. (1 August 1958). "Larva Currens". AMA Archives of Dermatology. 78 (2): 186–90. doi:10.1001/archderm.1958.01560080044007. PMID 13558704.
- ↑ CDC. "Parasites". Archived from the original on 2 May 2021. Retrieved 25 April 2013.
- ↑ "Archive copy". Archived from the original on 2021-08-29. Retrieved 2021-05-17.
{{cite web}}: CS1 maint: archived copy as title (link) - ↑ Drugs.com. "Albenza". Drugs.com. Archived from the original on 14 October 2012. Retrieved 25 April 2013.
- ↑ Drugs.com. "Stromectol". Drugs.com. Archived from the original on 7 January 2012. Retrieved 25 April 2013.
- ↑ Drugs.com. "Mintezol". Drugs.com. Archived from the original on 13 October 2012. Retrieved 25 April 2013.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 maint: archived copy as title
- All articles with unsourced statements
- Articles with unsourced statements from January 2021
- Articles with invalid date parameter in template
- Parasitic infestations, stings, and bites of the skin
- Helminthiases
- Neglected tropical diseases
- Tropical diseases
- Zoonoses