Clostridial necrotizing enteritis
| Clostridial necrotizing enteritis | |
|---|---|
| Other names: Enteritis necroticans or Pigbel | |
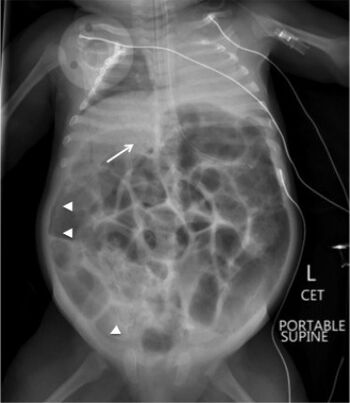 | |
| (Fatal) Clostridial necrotizing enterocolitis in infant | |
| Specialty | Infectious disease, Gastroenterology |
Clostridial necrotizing enteritis (CNE) is a severe and potentially fatal type of food poisoning caused by a β-toxin of Clostridium perfringens,[1] Type C. It occurs in some developing regions, particularly in New Guinea, where it is known as pig-bel.[2] The disease was also documented in Germany following World War II, where it was called Darmbrand (literally "bowel fire," or bowel necrosis). The toxin is normally inactivated by certain proteolytic enzymes and by normal cooking, but when these protections are impeded by diverse factors, and high protein is consumed, the disease can emerge.
Sporadic and extremely rare cases occur in diabetics. In New Guinea, where people generally have low-protein diets apart from tribal feasts, a number of factors—diet and endemic helminth infections among them—compound to result in pig-bel.[3]
Signs and symptoms
CNE is a necrotizing inflammation of the small bowel (especially the jejunum but also the ileum). Clinical results may vary from mild diarrhea to a life-threatening sequence of severe abdominal pain, vomiting (often bloody), bloody stool, ulceration of the small intestine with leakage (perforation) into the peritoneal cavity and possible death within a single day due to peritonitis. Many patients exhibit meteorism (swelling of the abdomen due to excess gas) and fever. Fluid can enter the peritoneum.
Sepsis can occur, with one case having 28,500 white blood cells per cubic milliliter.[4]
Preterm infants
The majority of preterm infants who develop NEC are generally healthy, feeding well, and growing prior to developing NEC.[5] The most frequent sign of NEC is a sudden change in feeding tolerance, which can be manifest by numerous clinical signs listed below. While gastric residuals are often seen in early NEC, there is no evidence that routine measurement of gastric residual volumes in asymptomatic infants is a useful guide to prevent or detect the onset of NEC, or help to advance feeds.[6][7][8][9] The timing of the onset of symptoms varies and appears to be inversely related to gestational age (GA). There appears to be a bimodal distribution (early versus late onset) based on GA.[10] For example, the median age at onset of NEC in infants with a GA of less than 26 weeks was 23 days (late), and for those with a GA of greater than 31 weeks, the median age at onset was 11 days (early).
Laboratory findings of infants presenting with NEC often include anemia, thrombocytopenia, evidence of disseminated intravascular coagulopathy (DIC), and in 20 percent of cases a positive blood culture.[11][12]
Causes
All the factors collectively causing CNE are generally only present in the hinterlands of New Guinea and parts of Africa, Latin America, and Asia. These factors include protein deprivation (causing inadequate synthesis of the enzyme trypsin protease, to which the toxin is very sensitive), poor food hygiene, episodic meat feasting, staple diets containing trypsin inhibitors (sweet potatoes), and infection by Ascaris parasites, which secrete a trypsin inhibitor. In New Guinea (origin of the term "pig-bel"), the disease is usually spread through contaminated meat (especially pork) and perhaps by peanuts. CNE was also diagnosed in post-World War II Germany, where it was known as Darmbrand or "bowel fire," and reached epidemic proportions. The causative agents of these CNE cases have since been described as Type C isolates of C. perfringens, which possessed genes for β-toxins and enterotoxins.[13]
In developed countries, CNE can also occur in people with diabetes, including children.[14] This form of CNE is extremely rare: to demonstrate its scope, only three such cases have been reported in the United States up to 2002.[15]
Diagnosis
An abdominal x-ray shows multiple dilated loops of small bowel and gas. The abdomen can be tender, distended, and soft. A differential diagnosis can be an intussusception.
Treatment
Treatment involves suppressing the toxin-producing organisms with antibiotics such as penicillin G or metronidazole. About half of seriously ill patients require surgery for perforation, persistent intestinal obstruction, or failure to respond to the antibiotics. An investigational toxoid vaccine has been used successfully in some developing countries but is not available outside of research.
Antibiotic therapy — For all infants with suspected or established NEC, initiating broad-spectrum antibiotics after obtaining appropriate specimens for culture is a suggested treatment. The empiric antibiotic regimen should provide broad-spectrum coverage, including coverage for common causes of late-onset neonatal sepsis. The choice is also guided by the local susceptibility patterns (ie, the local antibiogram in a particular neonatal intensive care unit [NICU]).
Acceptable empiric regimens include, but are not limited to, the following:[16]
•Ampicillin plus gentamicin (or amikacin) plus metronidazole
•Ampicillin plus gentamicin (or amikacin) plus clindamycin
•Ampicillin plus an expanded-spectrum cephalosporin (eg, cefotaxime [where available], ceftazidime, or cefepime) plus metronidazole
•Monotherapy with piperacillin-tazobactam
•Monotherapy with meropenem
Vancomycin should be included in the regimen (ie, replacing ampicillin or added to monotherapy) in centers where there is a high prevalence of methicillin-resistant Staphylococcus aureus (MRSA) or ampicillin-resistant enterococcal infections. Centers with significant gentamicin resistance patterns should consider amikacin in place of gentamicin.
The use of oral aminoglycosides is not recommended because it can result in the development of resistant bacterial strains, and has not been shown to be more beneficial than standard care.[17][18]
Other clostridial toxemias
- Leukemia patients, cancer chemotherapy recipients and others suffering from suppressed white blood cells (neutropenia) can be afflicted by a similar syndrome, neutropenic enterocolitis, in which the cecum is targeted by Clostridium septicum in much the same way.
- In neonatal intensive-care units, the syndrome of neonatal necrotizing enterocolitis may be caused in a similar way by C. perfringens, C. butyricum, and C. difficile, but this has not been proved.
See also
- Protein poisoning refers to a different diet-induced phenomenon.
References
- ↑ "Clostridial Necrotizing Enteritis: Anaerobic Bacteria: Merck Manual Professional". Archived from the original on 2010-08-21. Retrieved 2008-12-19.
- ↑ Cooke RA. Pig Bel. Perspect Pediatr Pathol. 1979;5:137-52. PMID 575409.
- ↑ "Pigbel, Clostridial Enteritis Necrotans, Much Nastier than C diff Diarrhoea - Resus". Resus. 2014-09-04. Archived from the original on 2018-03-30. Retrieved 2018-03-30.
- ↑ "The Beast in the Belly | DiscoverMagazine.com". Discover Magazine. Archived from the original on 2015-12-25. Retrieved 2018-04-12.
- ↑ Kliegman, R. M.; Walker, W. A.; Yolken, R. H. (December 1993). "Necrotizing enterocolitis: research agenda for a disease of unknown etiology and pathogenesis". Pediatric Research. 34 (6): 701–708. doi:10.1203/00006450-199312000-00001. ISSN 0031-3998. PMID 8108179. S2CID 22717529. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Neu, Josef; Walker, W. Allan (2011-01-20). "Necrotizing enterocolitis". The New England Journal of Medicine. 364 (3): 255–264. doi:10.1056/NEJMra1005408. ISSN 1533-4406. PMC 3628622. PMID 21247316.
- ↑ Cobb, Bridget Arnold; Carlo, Waldemar A.; Ambalavanan, Namasivayam (January 2004). "Gastric residuals and their relationship to necrotizing enterocolitis in very low birth weight infants". Pediatrics. 113 (1 Pt 1): 50–53. doi:10.1542/peds.113.1.50. ISSN 1098-4275. PMID 14702446. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Li, Yue-Feng; Lin, Hung-Chih; Torrazza, Roberto Murgas; Parker, Leslie; Talaga, Elizabeth; Neu, Josef (October 2014). "Gastric residual evaluation in preterm neonates: a useful monitoring technique or a hindrance?". Pediatrics and Neonatology. 55 (5): 335–340. doi:10.1016/j.pedneo.2014.02.008. ISSN 2212-1692. PMID 25129325. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Parker, Leslie A.; Weaver, Michael; Murgas Torrazza, Roberto J.; Shuster, Jonathon; Li, Nan; Krueger, Charlene; Neu, Josef (2019-06-01). "Effect of Gastric Residual Evaluation on Enteral Intake in Extremely Preterm Infants: A Randomized Clinical Trial". JAMA Pediatrics. 173 (6): 534–543. doi:10.1001/jamapediatrics.2019.0800. ISSN 2168-6211. PMC 6547072. PMID 31034045.
- ↑ Yee, Wendy H.; Soraisham, Amuchou Singh; Shah, Vibhuti S.; Aziz, Khalid; Yoon, Woojin; Lee, Shoo K.; Canadian Neonatal Network (February 2012). "Incidence and timing of presentation of necrotizing enterocolitis in preterm infants". Pediatrics. 129 (2): e298–304. doi:10.1542/peds.2011-2022. ISSN 1098-4275. PMID 22271701. S2CID 26079047. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Kliegman, R. M.; Fanaroff, A. A. (1984-04-26). "Necrotizing enterocolitis". The New England Journal of Medicine. 310 (17): 1093–1103. doi:10.1056/NEJM198404263101707. ISSN 0028-4793. PMID 6369134. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Hällström, Minna; Koivisto, Anna-Maija; Janas, Martii; Tammela, Outi (April 2006). "Laboratory parameters predictive of developing necrotizing enterocolitis in infants born before 33 weeks of gestation". Journal of Pediatric Surgery. 41 (4): 792–798. doi:10.1016/j.jpedsurg.2005.12.034. ISSN 1531-5037. PMID 16567195. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Ma M, Li J, McClane BA. Genotypic and phenotypic characterization of Clostridium perfringens isolates from Darmbrand cases in post-World War II Germany. Infect Immun. 2012 Dec;80(12):4354-63. doi: 10.1128/IAI.00818-12. Epub 2012 Oct 1. PMID 23027533; PMCID: PMC3497428.
- ↑ Petrillo, T. M. et al. Enteritis necroticans (pigbel) in a diabetic child. N. Engl. J. Med. 342, 1250–1253. https://doi.org/10.1056/nejm200004273421704 (2000).
- ↑ Gui L, Subramony C, Fratkin J, Hughson MD. Fatal enteritis necroticans (pigbel) in a diabetic adult. Mod Pathol. 2002 Jan;15(1):66-70. doi: 10.1038/modpathol.3880491. PMID 11796843.
- ↑ Smith, Michael J.; Boutzoukas, Angelique; Autmizguine, Julie; Hudak, Mark L.; Zinkhan, Erin; Bloom, Barry T.; Heresi, Gloria; Lavery, Adrian P.; Courtney, Sherry E.; Sokol, Gregory M.; Cotten, C. Michael (2021-06-01). "Antibiotic Safety and Effectiveness in Premature Infants With Complicated Intraabdominal Infections". The Pediatric Infectious Disease Journal. 40 (6): 550–555. doi:10.1097/INF.0000000000003034. ISSN 1532-0987. PMID 33902072. S2CID 233408814. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Hansen, T. N.; Ritter, D. A.; Speer, M. E.; Kenny, J. D.; Rudolph, A. J. (November 1980). "A randomized, controlled study of oral gentamicin in the treatment of neonatal necrotizing enterocolitis". The Journal of Pediatrics. 97 (5): 836–839. doi:10.1016/s0022-3476(80)80283-6. ISSN 0022-3476. PMID 7000998. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- ↑ Egan, E. A.; Mantilla, G.; Nelson, R. M.; Eitzman, D. V. (September 1976). "A prospective controlled trial of oral kanamycin in the prevention of neonatal necrotizing enterocolitis". The Journal of Pediatrics. 89 (3): 467–470. doi:10.1016/s0022-3476(76)80553-7. ISSN 0022-3476. PMID 784926. Archived from the original on 2022-06-22. Retrieved 2023-01-19.
- Cooke RA (1979). "Pig Bel". Perspect Pediatr Pathol. 5: 137–52. PMID 575409.
- Murrell TG, Roth L, Egerton J, Samels J, Walker PD (January 1966). "Pig-bel: enteritis necroticans. A study in diagnosis and management". Lancet. 1 (7431): 217–22. doi:10.1016/s0140-6736(66)90048-1. PMID 4159182.
- Murrell TG, Egerton JR, Rampling A, Samels J, Walker PD (September 1966). "The ecology and epidemiology of the pig-bel syndrome in man in New Guinea". J Hyg (Lond). 64 (3): 375–96. doi:10.1017/S0022172400040663. PMC 2134745. PMID 4288244.
- Nuland, Sherwin B., “The Beast in the Belly”, Discover, Vol. 16 No. 02 (February 1995).
External links
| Classification |
|---|