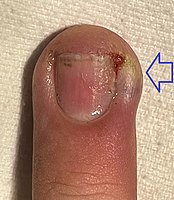
Paronychia
| Paronychia | |
|---|---|
| Other names: Perionychia[1] | |
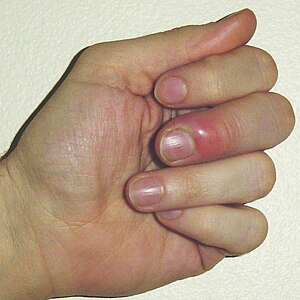 | |
| Acute paronychia of the middle finger | |
| Specialty | Dermatology, emergency medicine |
| Symptoms | Acute: Pain, redness, swelling, pus[2][3] Chronic Mild tenderness, redness, nail changes[2][3] |
| Complications | Abscess[3] |
| Types | Acute, chronic[3] |
| Causes | Infectious (bacterial, viral, fungal), frequent hand washing, nail biting, certain medications[3] |
| Diagnostic method | Based on examination[3] |
| Differential diagnosis | Cellulitis, felon, herpetic whitlow, onychomycosis, nail psoriasis[3] |
| Treatment | Acute: Warm compresses, antibiotics, incision and drainage[2][1] Chronic: Avoiding the underlying cause, antifungal and corticosteroid cream[2][1] |
| Frequency | Common[4] |
Paronychia is inflammation of the skin around the nail.[5] It may present suddenly with pain, redness, swelling, and pus; or gradually with mild tenderness, redness, and nail changes.[2][3] The index and middle fingers are most commonly affected, though other fingers or toes may be involved.[2][1] Complications may include an abscess.[3]
It may occur due to an infection (bacterial, viral, or fungal), as a result of irritation such as frequent hand washing or nail biting, or as a result of certain medications.[3] When due to the bacteria Staph. aureus onset is generally sudden, while when due to Candida albicans it is generally gradual.[2] Minor trauma may also result in an increased risk of infection.[6] Diagnosis is generally based on examination.[3]
Acute paronychia is generally treated by warm compresses, antibiotics, or incision and drainage.[1][2] Chronic paronychia is generally treated by avoiding the underlying cause together with an antifungal and corticosteroid cream such as clotrimazole and betamethasone.[2] It is a common infection of the hand.[4] Women are affected three times as often as men.[3]
Signs and symptoms
In acute paronychia there is generally a sudden onset of pain, redness, swelling, and pus within the nail fold.[2][3] Chronic paronychia generally presents gradually with mild tenderness, redness, and nail changes.[2][3] The index and middle fingers are most commonly affected.[2]
-
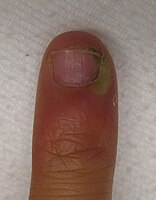
An infection of the cuticle secondary to a splinter
-
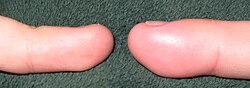
The finger on the right exhibits swelling due to acute paronychia.
-
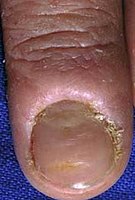
Chronic paronychia
-
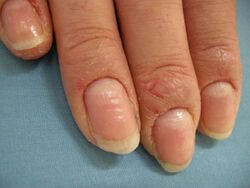
Chronic paronychia
-
Acute paronychia
Causes
Acute paronychia is usually caused by bacteria. Paronychia is often treated with antibiotics, either topical or oral or both. Chronic paronychia is most often caused by a yeast infection of the soft tissues around the nail but can also be traced to a bacterial infection. If the infection is continuous, the cause is often fungal and needs antifungal cream or paint to be treated.[7]
Risk factors include repeatedly washing hands and trauma to the cuticle such as may occur from repeated nail biting.[2] In the context of bartending, it is known as bar rot.[8]
Prosector's paronychia is a primary inoculation of tuberculosis of the skin and nails, named after its association with prosectors, who prepare specimens for dissection. Paronychia around the entire nail is sometimes referred to as runaround paronychia.[citation needed]
Painful paronychia in association with a scaly, erythematous, keratotic rash (papules and plaques) of the ears, nose, fingers, and toes may be indicative of acrokeratosis paraneoplastica, which is associated with squamous cell carcinoma of the larynx.[9]
Paronychia can occur with diabetes, drug-induced immunosuppression,[10] or systemic diseases such as pemphigus.[11]
Pathophysiology
Paronychia is an inflammation of the skin around the nail, which can occur suddenly (acute), when it is usually due to the bacteria Staph. aureus, or gradually (chronic) when it is commonly caused by Candida albicans.[2]
Diagnosis
Types
Paronychia may be divided as follows:[12]
- Acute paronychia is an infection of the folds of tissue surrounding the nail of a finger or, less commonly, a toe, lasting less than six weeks.[4] The infection generally starts in the paronychium at the side of the nail, with local redness, swelling, and pain.[13]: 660 Acute paronychia is usually caused by direct or indirect trauma to the cuticle or nail fold, and may be from relatively minor events, such as dishwashing, an injury from a splinter or thorn, nail biting, biting or picking at a hangnail, finger sucking, an ingrown nail, or manicure procedures.[1]
- Chronic paronychia is an infection of the folds of tissue surrounding the nail of a finger or, less commonly, a toe, lasting more than six weeks.[4] It is a nail disease prevalent in individuals whose hands or feet are subject to moist local environments, and is often due to contact dermatitis.[13]: 660 In chronic paronychia, the cuticle separates from the nail plate, leaving the region between the proximal nail fold and the nail plate vulnerable to infection.[1]: 343 It can be the result of dish washing, finger sucking, aggressively trimming the cuticles, or frequent contact with chemicals (mild alkalis, acids, etc.).
Alternatively, paronychia may be divided as follows:[13]
- Candidal paronychia is an inflammation of the nail fold produced by Candida albicans.[12]: 310
- Pyogenic paronychia is an inflammation of the folds of skin surrounding the nail caused by bacteria.[12]: 254 Generally acute paronychia is a pyogenic paronychia as it is usually caused by a bacterial infection.[4]
Differential
Other conditions that may present similarly include cellulitis, felon, herpetic whitlow, onychomycosis, and nail psoriasis.[3]
Treatment
Acute
When no pus is present, warm soaks are reasonable, even though there is a lack of evidence to support its use.[14] Over-the-counter antibiotics creams such as mupirocin or neomycin/polymyxin B/bacitracin may be sufficient for mild cases.[1] Antibiotics by mouth such as clindamycin or cephalexin are also often used, the first being more effective in areas where MRSA is common.[14] If there are signs of an abscess (the presence of pus) drainage is recommended.[14]
Chronic
Chronic paronychia is treated by avoiding whatever is causing it, a topical antifungal, and a topical steroid. In those who do not improve following these measures, oral antifungals and steroids may be used or the nail fold may be removed surgically.[1]
Word origin
The term is from Greek: παρωνυχία from para, "around", onyx, "nail" and the abstract noun suffix -ia.[15][16]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Rigopoulos D, Larios G, Gregoriou S, Alevizos A (February 2008). "Acute and chronic paronychia". Am Fam Physician. 77 (3): 339–46. PMID 18297959.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 James G. Marks; Jeffrey J. Miller (2013). "21. Nail disorders". Lookingbill and Marks' Principles of Dermatology E-Book (Fifth ed.). Elsevier Saunders. p. 256. ISBN 978-1-4557-2875-6. Archived from the original on 2021-08-29. Retrieved 2020-11-10.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 Dulski, A; Edwards, CW (January 2020). "Paronychia". PMID 31335027.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 4.0 4.1 4.2 4.3 4.4 Rockwell PG (March 2001). "Acute and chronic paronychia". Am Fam Physician. 63 (6): 1113–6. PMID 11277548.
- ↑ James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "14. Bacterial infections". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 256-257. ISBN 978-0-323-54753-6.
- ↑ Saavedra, Arturo; Roh, Ellen K.; Mikailov, Anar (2023). "32.Disorders of the nail apparatus". Fitzpatrick's Color Atlas and Synopsis of Clinical Dermatology (9th ed.). New York: McGraw Hill Professional. pp. 849–872. ISBN 978-1-264-27801-5. Archived from the original on 2023-12-31. Retrieved 2024-01-18.
- ↑ "Doctor's advice Q: Whitlow (paronychia)". bbc.co.uk. Archived from the original on 2007-12-19. Retrieved 2008-05-10.
- ↑ "Bar Rot". The Truth About Bartending. January 27, 2012. Archived from the original on 2013-03-22.
- ↑ Karen Allen, MD (2005-08-17). "eMedicine - Acrokeratosis Neoplastica". Archived from the original on 2008-12-05. Retrieved 2007-09-22.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Paronychia~clinical at eMedicine
- ↑ Serratos BD, Rashid RM (200). "Nail disease in pemphigus vulgaris". Dermatol. Online J. 15 (7): 2. PMID 19903430. Archived from the original on 2019-06-23. Retrieved 2017-08-01.
- ↑ 12.0 12.1 12.2 James, William D.; Berger, Timothy G. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. ISBN 978-0-7216-2921-6.
- ↑ 13.0 13.1 13.2 Freedberg, Irwin M., ed. (2003). Fitzpatrick's Dermatology in General Medicine (6th ed.). McGraw-Hill Publishing Company. ISBN 978-0071380768.
- ↑ 14.0 14.1 14.2 Ritting, AW; O'Malley, MP; Rodner, CM (May 2012). "Acute paronychia". The Journal of Hand Surgery. 37 (5): 1068–70, quiz page 1070. doi:10.1016/j.jhsa.2011.11.021. PMID 22305431.
- ↑ Harper, Douglas. "paronychia". Online Etymology Dictionary.
- ↑ παρωνυχία, παρά, ὄνυξ. Liddell, Henry George; Scott, Robert; A Greek–English Lexicon at the Perseus Project.
External links
| Classification | |
|---|---|
| External resources |
- "Paronychia Nail Infection". Dermatologic Disease Database. American Osteopathic College of Dermatology. Archived from the original on 2013-03-30. Retrieved 2006-07-12.
- Pages with script errors
- CS1 errors: missing periodical
- Articles containing Ancient Greek (to 1453)-language text
- Articles with hatnote templates targeting a nonexistent page
- All articles with unsourced statements
- Articles with unsourced statements from November 2020
- Articles with invalid date parameter in template
- Articles containing Greek-language text
- Occupational diseases
- Conditions of the skin appendages
- Nails (anatomy)
- Tuberculosis
- RTT