Chronic bacterial prostatitis
| Chronic bacterial prostatitis | |
|---|---|
 | |
| Specialty | Urology |
| Symptoms | Pain with urination, trouble with the stream, frequent urination[1] |
| Complications | Sexual dysfunction[1] |
| Duration | >3 months[1] |
| Causes | Often Escherichia coli[1] |
| Risk factors | Urinary catheterization, diabetes, prostate biopsy, uncircumcised, transurethral resection of the prostate (TURP)[1][2] |
| Diagnostic method | Based on symptoms, examination, and urine testing[1] |
| Differential diagnosis | Benign prostatic hyperplasia (BPH), chronic pelvic pain syndrome (CPPS), interstitial cystitis, prostate cancer, pelvic floor dysfunction, prostatic abscess, bladder cancer[1][2] |
| Treatment | Antibiotics, alpha blockers[1] |
| Frequency | <1% of males at some point[2] |
Chronic bacterial prostatitis (CBP) is a bacterial infection of the prostate gland that results in symptoms for greater than 3 months.[1] Typical symptoms include pain with urination, trouble with the stream, and frequent urination.[1] Other symptoms may include pain in the lower abdomen or perineum, sexual dysfunction, or fever.[1] Symptoms are generally milder than acute bacterial prostatitis.[3]
Chronic bacterial prostatitis develops in about 10% of people after acute bacterial prostatitis.[1] Risk factors include urinary catheterization, diabetes, prostate biopsy, being uncircumcised, and transurethral resection of the prostate (TURP).[1][2] Most cases are due to the bacteria Escherichia coli.[1] Diagnosis is based on symptoms, examination, and urine testing.[1] Positive cultures are required for the diagnosis.[4] Other forms of prostatitis include acute bacterial prostatitis and chronic pelvic pain syndrome (CPPS).[5]
Treatment is generally with antibiotics by mouth for 4 to 12 weeks.[1] The antibiotics used should be based on the urine culture results with commonly used agents including levofloxacin or azithromycin.[3][2] Alpha blockers, such as tamsulosin, and pain medications may also be used.[2] Re-occurrence of disease is common.[1] Chronic bacterial prostatitis occurs in less than 1% of males at some point in time.[2] It most commonly occurs in those under the age of 50.[1]
Signs and symptoms
Chronic bacterial prostatitis is a relatively rare condition that usually presents with an intermittent UTI-type picture. It is defined as recurrent urinary tract infections in men originating from a chronic infection in the prostate. Symptoms may be completely absent until there is also bladder infection, and the most troublesome problem is usually recurrent cystitis.[6] It is said that recurrent and relapsing UTIs (i.e., UTIs due to the same pathogen) are a hallmark of chronic bacterial prostatitis.[7][8][9]
Chronic bacterial prostatitis is the cause of less than 5% of prostate-related non-BPH lower urinary tract symptoms (LUTS).[citation needed]
Diagnosis
In chronic bacterial prostatitis, there are bacteria in the prostate, but there may be no symptoms or milder symptoms than occur with acute prostatitis.[10] The prostate infection is diagnosed by culturing urine as well as prostate fluid (expressed prostatic secretions or EPS) which are obtained by the doctor performing a rectal exam and putting pressure on the prostate. If no fluid is recovered after this prostatic massage, a post massage urine should also contain any prostatic bacteria.[citation needed]
Prostate specific antigen levels may be elevated, although there is no malignancy. Semen analysis is a useful diagnostic tool.[11] Semen cultures are also performed. Antibiotic sensitivity testing is also done to select the appropriate antibiotic. Other useful markers of infection are seminal elastase and seminal cytokines.
-
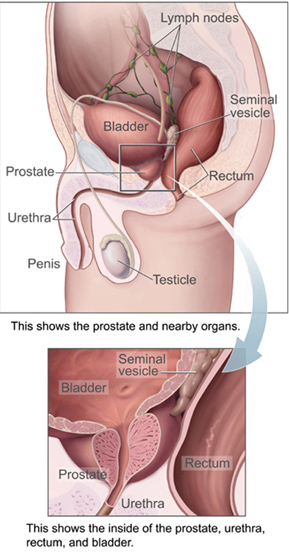
Prostate, urethra, and seminal vesicles.
-
The arteries of the pelvis.
-
Male pelvic organs seen from right side.
Treatment
Antibiotic therapy has to overcome the blood/prostate barrier that prevents many antibiotics from reaching levels that are higher than minimum inhibitory concentration.[12] Treatment requires prolonged courses (4–8 weeks) of antibiotics that penetrate the prostate well.[13] The fluoroquinolones, tetracyclines and macrolides have the best penetration. There have been contradictory findings regarding the penetrability of nitrofurantoin, quinolones (ciprofloxacin, levofloxacin), sulfas (trimethoprim-sulfamethoxazole), doxycycline and macrolides (erythromycin, clarithromycin). This is particularly true for gram-positive infections. Other antibiotics with the potential for improved activity, including linezolid, moxifloxacin, tigecycline, daptomycin, clindamycin, and vancomycin, have been used limitedly with reported success.[14]
Levofloxacin was found to reach prostatic fluid concentrations 5.5 times higher than ciprofloxacin, indicating a greater ability to penetrate the prostate.[15] Moxifloxacin shows even greater prostatic penetration than levofloxacin and may be the only fluoroquinolone able to obtain prostatic concentrations 10-fold above the minimum inhibitory concentration against Enterococcus faecalis.[16] However, limited experience with moxifloxacin for chronic prostatitis exists.[16][14]
Success rates with antibiotics by mouth can reach 70% to 90% at 6 months, although trials comparing them with placebo or no treatment do not exist.[17]
Persistent infections may be helped in 80% by the use of alpha blockers (tamsulosin, alfuzosin), or long term low dose antibiotic therapy.[18] Recurrent infections may be caused by inefficient urination (benign prostatic hypertrophy, neurogenic bladder), prostatic stones or a structural abnormality that acts as a reservoir for infection.
In theory, the ability of some strains of bacteria to form biofilms might be one of the factors that facilitate development of chronic bacterial prostatitis.[19]
There is tentative evidence to support pelvic floor physiotherapy.[2]
Prostatectomy has been used to treat chronic bacterial prostatitis but inadequate data —including no randomized controlled trials— exists to allow clinical decisions.[20] Moreover, prostatectomy can result in erectile dysfunction and urinary incontinence as complications.[20]
Prognosis
Over time, the relapse rate is high, exceeding 50%. However, combination therapies offer a better prognosis than antibiotics alone.
A 2014 found that recurrence occurred within 2 months in 28% of the group using antibiotics alone (prulifloxacin 600 mg), but in only 8% of the group taking prulifloxacin in combination with Serenoa repens extract, Lactobacillus Sporogens and Arbutin.[21]
Large prostatic stones was shown to be related with the presence of bacteria,[22] a higher urinary symptoms and pain score, a higher IL-1β and IL-8 concentration in seminal plasma, a greater prostatic inflammation and a lower response to antibiotic treatment.[23]
Epidemiology
Chronic bacterial prostatitis is rare.[24]
Research
Bacteriophages hold promise as another potential treatment for chronic bacterial prostatatis.[25]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 Su, ZT; Zenilman, JM; Sfanos, KS; Herati, AS (3 June 2020). "Management of Chronic Bacterial Prostatitis". Current urology reports. 21 (7): 29. doi:10.1007/s11934-020-00978-z. PMID 32488742.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Holt, JD; Garrett, WA; McCurry, TK; Teichman, JM (15 February 2016). "Common Questions About Chronic Prostatitis". American family physician. 93 (4): 290–6. PMID 26926816.
- ↑ 3.0 3.1 Davis, NG; Silberman, M (January 2023). "Bacterial Acute Prostatitis". PMID 29083799.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Bowen, DK; Dielubanza, E; Schaeffer, AJ (27 August 2015). "Chronic bacterial prostatitis and chronic pelvic pain syndrome". BMJ clinical evidence. 2015. PMID 26313612.
- ↑ Holt JD, Garrett WA, McCurry TK, Teichman JM (February 2016). "Common Questions About Chronic Prostatitis". American Family Physician. 93 (4): 290–6. PMID 26926816.
- ↑ Habermacher GM, Chason JT, Schaeffer AJ (2006). "Prostatitis/chronic pelvic pain syndrome". Annual Review of Medicine. 57 (1): 195–206. doi:10.1146/annurev.med.57.011205.135654. PMID 16409145.
- ↑ Najar MS, Saldanha CL, Banday KA (October 2009). "Approach to urinary tract infections". Indian J Nephrol. 19 (4): 129–39. doi:10.4103/0971-4065.59333. PMC 2875701. PMID 20535247.
- ↑ Lipsky BA, Byren I, Hoey CT (June 2010). "Treatment of bacterial prostatitis". Clin Infect Dis. 50 (12): 1641–52. doi:10.1086/652861. PMID 20459324.
- ↑ Wright ET, Chmiel JS, Grayhack JT, Schaeffer AJ (December 1994). "Prostatic fluid inflammation in prostatitis". J Urol. 152 (6 Pt 2): 2300–3. doi:10.1016/s0022-5347(17)31662-2. PMID 7966728.
- ↑ "Prostatitis - Symptoms". NHS Choices. 2017-10-19. Archived from the original on 2017-10-17. Retrieved 2022-08-19.
- ↑ Magri V, Wagenlehner FM, Montanari E, Marras E, Orlandi V, Restelli A, et al. (July 2009). "Semen analysis in chronic bacterial prostatitis: diagnostic and therapeutic implications". Asian Journal of Andrology. 11 (4): 461–77. doi:10.1038/aja.2009.5. PMC 3735310. PMID 19377490.
- ↑ Fulmer BR, Turner TT (May 2000). "A blood-prostate barrier restricts cell and molecular movement across the rat ventral prostate epithelium". The Journal of Urology. 163 (5): 1591–4. doi:10.1016/S0022-5347(05)67685-9. PMID 10751894. Archived from the original on 2019-12-10. Retrieved 2022-08-19.
- ↑ Charalabopoulos K, Karachalios G, Baltogiannis D, Charalabopoulos A, Giannakopoulos X, Sofikitis N (December 2003). "Penetration of antimicrobial agents into the prostate" (PDF). Chemotherapy. 49 (6): 269–79. doi:10.1159/000074526. PMID 14671426. S2CID 14731590. Archived (PDF) from the original on 2021-05-06. Retrieved 2022-08-19.
- ↑ 14.0 14.1 Perletti G, Trinchieri A, Stamatiou K, Magri V (February 2022). "Safety considerations with new antibacterial approaches for chronic bacterial prostatitis". Expert Opin Drug Saf. 21 (2): 171–182. doi:10.1080/14740338.2021.1956459. PMID 34260337.
- ↑ "Levofloxacin and Its Effective Use in the Review Management of Bacterial Prostatitis" (PDF). Archived from the original (PDF) on 2017-08-09. Retrieved 2016-02-08.
- ↑ 16.0 16.1 Xiong S, Liu X, Deng W, Zhou Z, Li Y, Tu Y, Chen L, Wang G, Fu B (2020). "Pharmacological Interventions for Bacterial Prostatitis". Front Pharmacol. 11: 504. doi:10.3389/fphar.2020.00504. PMC 7203426. PMID 32425775.
- ↑ Bowen DK, Dielubanza E, Schaeffer AJ (August 2015). "Chronic bacterial prostatitis and chronic pelvic pain syndrome". BMJ Clinical Evidence. 2015: 1802–1831. PMC 4551133. PMID 26313612.
- ↑ Shoskes DA, Hakim L, Ghoniem G, Jackson CL (April 2003). "Long-term results of multimodal therapy for chronic prostatitis/chronic pelvic pain syndrome". The Journal of Urology. 169 (4): 1406–10. doi:10.1097/01.ju.0000055549.95490.3c. PMID 12629373.
- ↑ Wagenlehner FM, Pilatz A, Bschleipfer T, Diemer T, Linn T, Meinhardt A, et al. (August 2013). "Bacterial prostatitis". World Journal of Urology. 31 (4): 711–6. doi:10.1007/s00345-013-1055-x. PMID 23519458. S2CID 1925596.
- ↑ 20.0 20.1 Schoeb DS, Schlager D, Boeker M, Wetterauer U, Schoenthaler M, Herrmann TR, Miernik A (November 2017). "Surgical therapy of prostatitis: a systematic review". World J Urol. 35 (11): 1659–1668. doi:10.1007/s00345-017-2054-0. PMID 28612108.
- ↑ Busetto GM, Giovannone R, Ferro M, Tricarico S, Del Giudice F, Matei DV, et al. (July 2014). "Chronic bacterial prostatitis: efficacy of short-lasting antibiotic therapy with prulifloxacin (Unidrox®) in association with saw palmetto extract, lactobacillus sporogens and arbutin (Lactorepens®)". BMC Urology. 14 (1): 53. doi:10.1186/1471-2490-14-53. PMC 4108969. PMID 25038794.
- ↑ Mazzoli, Sandra (August 2010). "Biofilms in chronic bacterial prostatitis (NIH-II) and in prostatic calcifications". FEMS Immunology and Medical Microbiology. 59 (3): 337–344. doi:10.1111/j.1574-695X.2010.00659.x. ISSN 1574-695X. PMID 20298500.
- ↑ Soric, Tomislav; Selimovic, Mirnes; Bakovic, Lada; Šimurina, Tatjana; Selthofer, Robert; Dumic, Jerka (2017). "Clinical and Biochemical Influence of Prostatic Stones". Urologia Internationalis. 98 (4): 449–455. doi:10.1159/000455161. ISSN 1423-0399. PMID 28052296. S2CID 4927272.
- ↑ Schneider H, Ludwig M, Hossain HM, Diemer T, Weidner W (October 2003). "The 2001 Giessen Cohort Study on patients with prostatitis syndrome--an evaluation of inflammatory status and search for microorganisms 10 years after a first analysis". Andrologia. 35 (5): 258–62. doi:10.1046/j.1439-0272.2003.00586.x. PMID 14535851. S2CID 21022117.
- ↑ Letkiewicz S, Międzybrodzki R, Kłak M, Jończyk E, Weber-Dąbrowska B, Górski A (November 2010). "The perspectives of the application of phage therapy in chronic bacterial prostatitis". FEMS Immunology and Medical Microbiology. 60 (2): 99–112. doi:10.1111/j.1574-695X.2010.00723.x. PMID 20698884.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 errors: missing periodical
- All articles with unsourced statements
- Articles with unsourced statements from April 2021
- Articles with invalid date parameter in template
- Articles with unsourced statements from September 2020
- Articles with Curlie links
- Bacterial diseases
- Sexually transmitted diseases and infections
- Inflammatory prostate disorders
- RTT


