Byssinosis
| Byssinosis | |
|---|---|
| Other names: Brown lung disease, Monday fever | |
 | |
| Byssinosis is caused by exposure to cotton dust in inadequately ventilated working environments. Image of a textile mill where fibrous material, such as cotton, is processed from machinery. | |
Byssinosis[n 1] is an occupational lung disease.[2][3]
It is caused by inhalation of cotton or jute dust in inadequately ventilated working environments and can develop over time with repeated exposure.[4][5] Byssinosis commonly occurs in textile workers who are employed in yarn and fabric manufacture industries. It is now thought that the cotton dust directly causes the disease and some believe that the causative agents are endotoxins that come from the cell walls of gram-negative bacteria that grow on the cotton.[6] Although bacterial endotoxin is a likely cause, the absence of similar symptoms in workers in other industries exposed to endotoxins makes this uncertain.[7] Current smokers are also at risk for developing byssinosis or having complications relating to byssinosis.[6]
Of the 81 byssinosis-related fatalities reported in the United States between 1990 and 1999, 48% included an occupation in the yarn, thread, and fabric industry on their death certificate.[8] This disease often occurred in the times of the Industrial Revolution. Most commonly young girls working in mills or other textile factories would be affected by this disease. In the United States, from 1996 to 2005, North Carolina accounted for about 37% of all deaths caused by byssinosis, with 31, followed by South Carolina (8) and Georgia (7).[9]
There is a lack of information regarding the prevalence and impact of byssinosis in low and middle income countries (LMIC) despite the fact that of the 25 million tons of cotton produced worldwide, about two thirds of this production comes from LMICs like India, Pakistan, and China.[5] Many textile mills and fiber producing factories located in LMICs have high rates of chronic respiratory disease caused by byssinosis.[5]
The term "brown lung" is a misnomer, as the lungs of affected individuals are not brown.[10] Byssinosis is also referred to as cotton worker's lung, mill fever, brown lung disease, and Monday fever.[6]
Symptoms and signs

Symptoms of byssinosis can include:[6]
- Cough with sputum
- Dyspnea
- Breathing difficulties
- Chest tightness
- Wheezing
- Cough
Patients can develop these symptoms after a few hours of exposure at minimum.[6] For this reason, patients who develop and report these symptoms, and subsequently byssinosis, are one of the reasons why the term Monday Fever exists.[6] Byssinosis can become chronic in a patient if they are continually exposed to cotton, jute, or yarn dust over time.[6] Byssinosis can be misdiagnosed as COPD, or asthma however the difference in these lung diseases and byssinosis comes from the etiology.[6] Byssinosis can ultimately result in narrowing of the airways, lung scarring and death from infection or respiratory failure.[citation needed] Extended exposure to cotton or jute dust can lead to impaired lung function and further respiratory complications.[11] Patients may require oxygen to assist with breathing and may also have difficulty exercising.[11]
Diagnosis
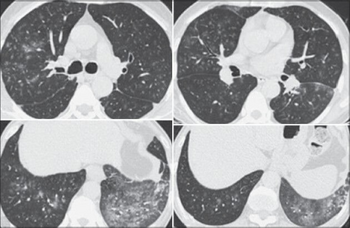
It can be difficult to accurately diagnose a patient with byssinosis due to symptoms that are similar to other respiratory diseases such as chronic obstructive pulmonary diseases (COPD), asthma, or bronchitis.[6] Byssinosis can be misdiagnosed as other pneumoconioses therefore a chest x-ray and/or lung function test is needed to accurately diagnose a patient who may have byssinosis.[6] The main distinction of byssinosis from other respiratory diseases comes from the initial exposure. Patients who have byssinosis have typically been exposed to cotton or just dust for an extended period of time and experience symptoms of chest tightness and coughing.[5]
Patient history should reveal exposure to cotton, flax, hemp, or jute dust. Measurable change in lung function before and after working shifts is key to diagnosis. Patients with byssinosis show a significant drop in FEV1 over the course of work shift. Chest radiographs show areas of opacity due to fibrosis of the pulmonary parenchyma.[citation needed]
Another form of diagnosis is observing patient symptoms throughout their work shift. Patients with byssinosis due to dust inhalation will experience adverse symptoms when they being their work shift on Monday which is where the term Monday Fever comes in.[6]
Treatment
There is currently no official form of diagnosing an individual with byssinosis.[6] Affected workers should be offered alternative employment. Employers in the manufacturing and textile industry should take preventative measures to ensure workers are not exposed to excessive dust and cotton during their work shifts as this is the main cause of byssinosis exposure. Continued exposure leads to development of persistent symptoms and progressive decline in FEV1.[6] Dust control measures can also help reduce the risk of textile workers developing byssinosis.[5]
Educational content aimed to raise awareness about byssinosis and other occupational lung diseases can be useful to inform workers and managers in textile industry as well as unions, and other health professionals.[6] Educational content should be based on signs and symptoms of byssinosis as well as other diagnostic measures.
History
In 1971, the Occupational Safety and Health Administration (OSHA) set a permissible exposure limit (PEL) of 1-mg/m3 (total dust) for cotton dust in work places.[12] Later in the 1978 OSHA developed the Cotton Dust Standard which aimed to prevent occupational respiratory disease, such as byssinosis, through medical monitoring of employees.[12] The PEL of cotton dust was set to 0.2 mg/m3 of airborne dust. This was considered the lowest level that could be measured by the vertical elutriator cotton dust sampler.[12]
OSHA regulators hoped that the Cotton Dust Standard Act would help decrease the impact of dust exposure of employees and reduce occupational respiratory diseases. However, a NISOH sponsored committee remained apprehensive about this standard as an earlier study conducted by NIOSH found that byssinosis diagnoses were brought on by cotton dust levels as low as 0.1 mg/m3 meaning that there is still a risk for the development of byssinosis for cotton dust exposure under the PEL.[12] Today, NIOSH has set a recommended exposure limit (REL) of cotton dust to less than 0.2 mg/m3 for up to a 10-hour workday.[13]
Notes and References
Notes
References
- ↑ βύσσινον, βύσσος. Liddell, Henry George; Scott, Robert; A Greek–English Lexicon at the Perseus Project.
- ↑ Byssinosis: MedlinePlus Medical Encyclopedia (NIH) Archived 2016-07-05 at the Wayback Machine
- ↑ Work-Related Lung Disease Surveillance System (eWoRLD): Work-Related Respiratory Diseases | CDC/NIOSH Archived 2022-01-21 at the Wayback Machine
- ↑ Hollander, AG (December 1953). "Byssinosis". Chest. American College of Chest Physicians. 24 (6): 674–678. doi:10.1378/chest.24.6.674. PMID 13107566.
{{cite journal}}: CS1 maint: url-status (link) - ↑ 5.0 5.1 5.2 5.3 5.4 Nafees, Asaad Ahmed; Matteis, Sara De; Burney, Peter; Cullinan, Paul (2022-01-24). "Contemporary Prevalence of Byssinosis in Low- and Middle-Income Countries: A Systematic Review". Asia-Pacific Journal of Public Health. 34 (5): 483–492. doi:10.1177/10105395211073051. hdl:10044/1/96110. ISSN 1010-5395. PMID 35073782. S2CID 246277619. Archived from the original on 2022-02-10. Retrieved 2022-07-22.
- ↑ 6.00 6.01 6.02 6.03 6.04 6.05 6.06 6.07 6.08 6.09 6.10 6.11 6.12 6.13 Patel, Pujan H.; Yarrarapu, Siva Naga S.; Anjum, Fatima (2022), "Byssinosis", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 30137833, archived from the original on 2022-08-04, retrieved 2022-02-10
- ↑ Newman, Lee S. (June 2008). "Byssinosis". Merck Manuals: online medical dictionary. Merck & Co. Archived from the original on 2010-09-08. Retrieved 2009-06-15.
- ↑ "Section 4. Byssinosis and Related Exposures". The Work-Related Lung Disease Surveillance Report, 2002. National Institute for Occupational Safety and Health. 2003. doi:10.26616/NIOSHPUB2003111. Archived from the original on 2019-06-15. Retrieved 2022-07-22.
- ↑ "Byssinosis: Number of deaths by state, U.S. residents age 15 and over, 1996-2005". National Institute for Occupational Safety and Health. March 2009. Archived from the original on 2013-02-20. Retrieved 2013-02-14.
- ↑ Barry S. Levy; David H. Wegman; Sherry L. Baron; Rosemary K. Sokas (2011). Occupational and environmental health recognizing and preventing disease and injury (6th ed.). New York: Oxford University Press. p. 416. ISBN 9780199750061.
- ↑ 11.0 11.1 Patel, Pujan H.; Yarrarapu, Siva Naga S.; Anjum, Fatima (2022), "Byssinosis", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 30137833, archived from the original on 2022-08-04, retrieved 2022-02-19
- ↑ 12.0 12.1 12.2 12.3 "Current intelligence bulletin 56 - washed cotton. A review and recommendations regarding batch kier washed cotton". 2020-10-06. doi:10.26616/NIOSHPUB95113. Archived from the original on 2022-07-07. Retrieved 2022-07-22.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ "PEL for cotton dust when exposure is from cotton fibers used in the manufacture of absorbent glass tubes. | Occupational Safety and Health Administration". www.osha.gov. Archived from the original on 2022-04-10. Retrieved 2022-04-10.
External links
| Classification | |
|---|---|
| External resources |
| Look up byssinosis in Wiktionary, the free dictionary. |
- Pages with script errors
- Articles containing Ancient Greek (to 1453)-language text
- Webarchive template wayback links
- CS1 maint: url-status
- CS1 errors: missing periodical
- All articles with unsourced statements
- Articles with unsourced statements from November 2020
- Articles with invalid date parameter in template
- Occupational diseases
- Lung diseases due to external agents
- Occupational safety and health