Benign prostatic hyperplasia
| Benign prostatic hyperplasia | |
|---|---|
| Other names: Benign enlargement of the prostate (BEP, BPE), adenofibromyomatous hyperplasia, benign prostatic hypertrophy,[1] benign prostatic obstruction[1] | |
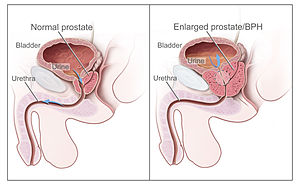 | |
| Diagram of a normal prostate (left) and benign prostatic hyperplasia (right) | |
| Specialty | Urology |
| Symptoms | Frequent urination, trouble starting to urinate, weak stream, inability to urinate, loss of bladder control[1] |
| Complications | Urinary tract infections, bladder stones, kidney failure[2] |
| Usual onset | Age over 40[1] |
| Causes | Unclear[1] |
| Risk factors | Family history, obesity, type 2 diabetes, not enough exercise, erectile dysfunction[1] |
| Diagnostic method | Based on symptoms and examination after ruling out other possible causes[2] |
| Differential diagnosis | Heart failure, diabetes, prostate cancer[2] |
| Treatment | Lifestyle changes, medications, a number of procedures, surgery[1][2] |
| Medication | Alpha blockers such as terazosin, 5α-reductase inhibitors such as finasteride[1] |
| Frequency | 105 million affected globally (2015)[3] |
Benign prostatic hyperplasia (BPH), also called prostate enlargement, is a noncancerous increase in size of the prostate gland.[1] Symptoms may include frequent urination, trouble starting to urinate, weak stream, inability to urinate, or loss of bladder control.[1] Complications can include urinary tract infections, bladder stones, and chronic kidney problems.[2]
The cause is unclear.[1] Risk factors include a family history, obesity, type 2 diabetes, not enough exercise, and erectile dysfunction.[1] Medications like pseudoephedrine, anticholinergics, and calcium channel blockers may worsen symptoms.[2] The underlying mechanism involves the prostate pressing on the urethra thereby making it difficult to pass urine out of the bladder.[1] Diagnosis is typically based on symptoms and examination after ruling out other possible causes.[2]
Treatment options including lifestyle changes, medications, a number of procedures, and surgery.[1][2] In those with mild symptoms weight loss, exercise, and decreasing caffeine intake is recommended.[2][4] In those with more significant symptoms, medications may include alpha blockers such as terazosin or 5α-reductase inhibitors such as finasteride.[1] A combination may be used.[5] Surgical removal of part of the prostate may be carried out in those who do not improve with other measures.[2] Alternative medicine, such as saw palmetto, does not appear to help.[2]
About 105 million men are affected globally.[3] BPH typically begins after the age of 40.[1] Half of males age 50 and over are affected.[2] After the age of 80 about 90% of males are affected.[1] Although prostate specific antigen levels may be elevated in males with BPH, the condition does not increase the risk of prostate cancer.[6]
Signs and symptoms

BPH is the most common cause of lower urinary tract symptoms (LUTS), which are divided into storage, voiding, and symptoms which occur after urination.[7] Storage symptoms include the need to urinate frequently, waking at night to urinate, urgency (compelling need to void that cannot be deferred), involuntary urination, including involuntary urination at night, or urge incontinence (urine leak following a strong sudden need to urinate).[8] Voiding symptoms include urinary hesitancy (a delay between trying to urinate and the flow actually beginning), intermittency (not continuous),[9] involuntary interruption of voiding, weak urinary stream, straining to void, a sensation of incomplete emptying, and uncontrollable leaking after the end of urination.[10][11][12] These symptoms may be accompanied by bladder pain or pain while urinating, called dysuria.[13]
Bladder outlet obstruction (BOO) can be caused by BPH.[14] Symptoms are abdominal pain, a continuous feeling of a full bladder, frequent urination, acute urinary retention (inability to urinate), pain during urination (dysuria), problems starting urination (urinary hesitancy), slow urine flow, starting and stopping (urinary intermittency), and nocturia.
BPH can be a progressive disease, especially if left untreated. Incomplete voiding results in residual urine or urinary stasis, which can lead to an increased risk of urinary tract infection.[15]
Causes
Hormones
Most experts consider androgens (testosterone and related hormones) to play a permissive role in the development of BPH. This means that androgens must be present for BPH to occur, but do not necessarily directly cause the condition. This is supported by evidence suggesting that castrated boys do not develop BPH when they age. In an unusual study of 26 eunuchs from the palace of the Qing dynasty still living in Beijing in 1960, the prostate could not be felt in 81% of the studied eunuchs.[16] The average time since castration was 54 years (range, 41–65 years). On the other hand, some studies suggest that administering exogenous testosterone is not associated with a significant increase in the risk of BPH symptoms, so the role of testosterone in prostate cancer and BPH is still unclear. Further randomized controlled trials with more participants are needed to quantify any risk of giving exogenous testosterone.[17]
Dihydrotestosterone (DHT), a metabolite of testosterone, is a critical mediator of prostatic growth. DHT is synthesized in the prostate from circulating testosterone by the action of the enzyme 5α-reductase, type 2. DHT can act in an autocrine fashion on the stromal cells or in paracrine fashion by diffusing into nearby epithelial cells. In both of these cell types, DHT binds to nuclear androgen receptors and signals the transcription of growth factors that are mitogenic to the epithelial and stromal cells. DHT is ten times more potent than testosterone because it dissociates from the androgen receptor more slowly. The importance of DHT in causing nodular hyperplasia is supported by clinical observations in which an inhibitor of 5α-reductase such as finasteride is given to men with this condition. Therapy with a 5α-reductase inhibitor markedly reduces the DHT content of the prostate and, in turn, reduces prostate volume and BPH symptoms.[18][19]
Testosterone promotes prostate cell proliferation,[20] but relatively low levels of serum testosterone are found in patients with BPH.[21][22] One small study has shown that medical castration lowers the serum and prostate hormone levels unevenly, having less effect on testosterone and dihydrotestosterone levels in the prostate.[23]
While there is some evidence that estrogen may play a role in the cause of BPH, this effect appears to be mediated mainly through local conversion of androgens to estrogen in the prostate tissue rather than a direct effect of estrogen itself.[24] In canine in vivo studies castration, which significantly reduced androgen levels but left estrogen levels unchanged, caused significant atrophy of the prostate.[25] Studies looking for a correlation between prostatic hyperplasia and serum estrogen levels in humans have generally shown none.[22][26]
In 2008, Gat et al. published evidence that BPH is caused by failure in the spermatic venous drainage system resulting in increased hydrostatic pressure and local testosterone levels elevated more than 100 fold above serum levels.[27] If confirmed, this mechanism explains why serum androgen levels do not seem to correlate with BPH and why giving exogenous testosterone would not make much difference.
Diet
Studies indicate that dietary patterns may affect development of BPH, but further research is needed to clarify any important relationship.[28] Studies from China suggest that greater protein intake may be a factor in development of BPH. Men older than 60 in rural areas had very low rates of clinical BPH, while men living in cities and consuming more animal protein had a higher incidence.[29][30] On the other hand, a study in Japanese-American men in Hawaii found a strong negative association with alcohol intake, but a weak positive association with beef intake.[31] In a large prospective cohort study in the US (the Health Professionals Follow-up Study), investigators reported modest associations between BPH (men with strong symptoms of BPH or surgically confirmed BPH) and total energy and protein, but not fat intake.[32] There is also epidemiological evidence linking BPH with metabolic syndrome (concurrent obesity, impaired glucose metabolism and diabetes, high triglyceride levels, high levels of low-density cholesterol, and hypertension).[33]
Degeneration
Benign prostatic hyperplasia is an age-related disease. Misrepair-accumulation aging theory[34][35] suggests that development of benign prostatic hyperplasia is a consequence of fibrosis and weakening of the muscular tissue in the prostate.[36] The muscular tissue is important in the functionality of the prostate, and provides the force for excreting the fluid produced by prostatic glands. However, repeated contractions and dilations of myofibers will unavoidably cause injuries and broken myofibers. Myofibers have a low potential for regeneration; therefore, collagen fibers need to be used to replace the broken myofibers. Such misrepairs make the muscular tissue weak in functioning, and the fluid secreted by glands cannot be excreted completely. Then, the accumulation of fluid in glands increases the resistance of muscular tissue during the movements of contractions and dilations, and more and more myofibers will be broken and replaced by collagen fibers.
Pathophysiology
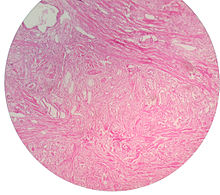
As men age, the enzymes aromatase and 5-alpha reductase increase in activity. These enzymes are responsible for converting androgen hormones into estrogen and dihydrotestosterone, respectively. This metabolism of androgen hormones leads to a decrease in testosterone but increased levels of DHT and estrogen.
Both the glandular epithelial cells and the stromal cells (including muscular fibers) undergo hyperplasia in BPH.[2] Most sources agree that of the two tissues, stromal hyperplasia predominates, but the exact ratio of the two is unclear.[37]:694
Anatomically the median and lateral lobes are usually enlarged, due to their highly glandular composition. The anterior lobe has little in the way of glandular tissue and is seldom enlarged. (Carcinoma of the prostate typically occurs in the posterior lobe – hence the ability to discern an irregular outline per rectal examination). The earliest microscopic signs of BPH usually begin between the age of 30 and 50 years old in the PUG, which is posterior to the proximal urethra.[37]:694 In BPH, the majority of growth occurs in the transition zone (TZ) of the prostate.[37]:694 In addition to these two classic areas, the peripheral zone (PZ) is also involved to a lesser extent.[37]:695 Prostatic cancer typically occurs in the PZ. However, BPH nodules, usually from the TZ are often biopsied anyway to rule out cancer in the TZ.[37]:695 BPH can be a progressive growth that in rare instances leads to exceptional enlargement.[38] In some males, the prostate enlargement exceeds 200 to 500 grams.[38] This condition has been defined as giant prostatic hyperplasia (GPH).[38]
Diagnosis
The clinical diagnosis of BPH is based on a history of LUTS (lower urinary tract symptoms), a digital rectal exam, and exclusion of other causes of similar signs and symptoms. The degree of LUTS does not necessarily correspond to the size of the prostate. An enlarged prostate gland on rectal examination that is symmetric and smooth supports a diagnosis of BPH.[2] However, if the prostate gland feels asymmetrical, firm, or nodular, this raises concern for prostate cancer.[2]
Urinalysis is typically performed when LUTS are present and BPH is suspected to evaluate for signs of a urinary tract infection, glucose in the urine (suggestive of diabetes), or protein in the urine (suggestive of kidney disease).[2] Bloodwork including kidney function tests and prostate specific antigen (PSA) are often ordered to evaluate for kidney damage and prostate cancer, respectively.[2] However, checking blood PSA levels for prostate cancer screening is controversial and not necessarily indicated in every evaluation for BPH.[2] Benign prostatic hyperplasia and prostate cancer are both capable of increasing blood PSA levels and PSA elevation is unable to differentiate these two conditions well.[2] If PSA levels are checked and are high, then further investigation is warranted. Measures including PSA density, free PSA, rectal examination, and transrectal ultrasonography may be helpful in determining whether a PSA increase is due to BPH or prostate cancer.[2] Ultrasound examination of the testes, prostate, and kidneys is often performed, again to rule out cancer and hydronephrosis.
Validated questionnaires such as the American Urological Association Symptom Index (AUA-SI), the International Prostate Symptom Score (I-PSS), and more recently the UWIN score (urgency, weak stream, incomplete emptying, and nocturia) are useful aids to making the diagnosis of BPH and quantifying the severity of symptoms.[2][39][40]
Differential diagnosis
Medical conditions
The differential diagnosis for LUTS is broad and includes various medical conditions, neurologic disorders, and other diseases of the bladder, urethra, and prostate such as bladder cancer, urinary tract infection, urethral stricture, urethral calculi (stones), chronic prostatitis, and prostate cancer.[2] Neurogenic bladder can cause urinary retention and cause symptoms similar to those of BPH. This may occur as a result of uncoordinated contraction of the bladder muscle or impairment in the timing of bladder muscle contraction and urethral sphincter relaxation.[2] Notable causes of neurogenic bladder include disorders of the central nervous system such as Parkinson's disease, multiple sclerosis, and spinal cord injuries as well as disorders of the peripheral nervous system such as diabetes mellitus, vitamin B12 deficiency, and alcohol-induced nerve damage.[2] Individuals affected by heart failure often experience nighttime awakenings to urinate due to redistribution of fluid accumulated in swollen legs.[2]
Medications
Certain medications can increase urination difficulties by increasing bladder outlet resistance due to increased smooth muscle tone at the prostate or bladder neck and contribute to LUTS.[2] Alpha-adrenergic agonist medications, such as decongestants with pseudoephedrine can increase bladder outlet resistance.[2] In contrast, calcium channel blockers and anticholinergic medications can worsen urinary retention by promoting bladder muscle relaxation.[2] Diuretic medications such as loop diuretics (e.g., furosemide) or thiazides (e.g., chlorthalidone) can cause or worsen urinary frequency and nighttime awakenings to urinate.[2]
-
Micrograph showing nodular hyperplasia (left off center) of the prostate from a transurethral resection of the prostate (TURP). H&E stain.
-
Microscopic examination of different types of prostate tissues (stained with immunohistochemical techniques): A. Normal (non-neoplastic) prostatic tissue (NNT). B. Benign prostatic hyperplasia. C. High-grade prostatic intraepithelial neoplasia. D. Prostatic adenocarcinoma (PCA).
Management
When managing benign prostatic hyperplasia, the aim is to prevent complications related to the disease and improve or relieve symptoms.[41] Approaches used include lifestyle modifications, medications, and surgery.
Lifestyle
Lifestyle alterations to address the symptoms of BPH include physical activity,[42] decreasing fluid intake before bedtime, moderating the consumption of alcohol and caffeine-containing products and following a timed voiding schedule. Patients can also attempt to avoid products and medications with anticholinergic properties that may exacerbate urinary retention symptoms of BPH, including antihistamines, decongestants, opioids, and tricyclic antidepressants; however, changes in medications should be done with input from a medical professional.[43]
Voiding position
Voiding position when urinating may influence urodynamic parameters (urinary flow rate, voiding time, and post-void residual volume).[44] A meta-analysis found no differences between the standing and sitting positions for healthy males, but that, for elderly males with lower urinary tract symptoms, voiding in the sitting position:[45]
- decreased the post void residual volume
- increased the maximum urinary flow, comparable with pharmacological intervention
- decreased the voiding time
This urodynamic profile is associated with a lower risk of urologic complications, such as cystitis and bladder stones.
Medications
The two main medication classes for BPH management are alpha blockers and 5α-reductase inhibitors.[46] While alpha blockers are generally used initially, a combination has greater benefits.[5]
Alpha blockers
Selective α1-blockers are the most common choice for initial therapy.[47][48][49] They include alfuzosin,[50][51] doxazosin,[52] silodosin, tamsulosin, terazosin, and naftopidil.[41] They have a small to moderate benefit at improving symptoms.[53][41][54] Selective alpha-1 blockers are similar in effectiveness but have slightly different side effect profiles.[53][41][54] Alpha blockers relax smooth muscle in the prostate and the bladder neck, thus decreasing the blockage of urine flow. Common side effects of alpha blockers include orthostatic hypotension (a head rush or dizzy spell when standing up or stretching), ejaculation changes, erectile dysfunction,[55] headaches, nasal congestion, and weakness. Naftopidil and tamsulosin may have similar levels of unwanted sexual side effects and silodosin may have more unwanted side effects.[41]
Tamsulosin and silodosin are selective α1 receptor blockers that preferentially bind to the α1A receptor in the prostate instead of the α1B receptor in the blood vessels. Less-selective α1 receptor blockers such as terazosin and doxazosin may lower blood pressure. The older, less selective α1-adrenergic blocker prazosin is not a first line choice for either high blood pressure or prostatic hyperplasia; it is a choice for patients who present with both problems at the same time. The older, broadly non-selective alpha blocker medications such as phenoxybenzamine are not recommended for control of BPH.[56] Non-selective alpha blockers such as terazosin and doxazosin may also require slow dose adjustments as they can lower blood pressure and cause syncope (fainting) if the response to the medication is too strong.
5α-Reductase inhibitors
The 5α-reductase inhibitors finasteride and dutasteride may also be used in men with BPH.[57] These medications inhibit the 5α-reductase enzyme, which, in turn, inhibits production of DHT, a hormone responsible for enlarging the prostate. Effects may take longer to appear than alpha blockers, but they persist for many years.[58] When used together with alpha blockers, no benefit was reported in short-term trials, but in a longer-term study (3–4 years) there was a greater reduction in BPH progression to acute urinary retention and surgery than with either agent alone, especially in people with more severe symptoms and larger prostates.[59][60][61] Other trials have confirmed reductions in symptoms, within 6 months in one trial, an effect that was maintained after withdrawal of the alpha blocker.[60][62] Side effects include decreased libido and ejaculatory or erectile dysfunction.[63][64] The 5α-reductase inhibitors are contraindicated in pregnant women because of their teratogenicity due to interference with fetal testosterone metabolism, and as a precaution, pregnant women should not handle crushed or broken tablets.[65]
Phosphodiesterase-5 inhibitors
A meta‐analysis found that tadalafil 5 mg once‐daily is an effective treatment for lower urinary tract symptoms and that such treatment had a low rate of adverse effects. Other phosphodiesterase-5 inhibitors are also effective, but may require multiple doses daily to maintain adequate urine flow.[66][67] suggesting a possible common cause with erectile dysfunction. Tadalafil was considered then rejected by NICE in the UK for the treatment of symptoms associated with BPH.[68] In 2011, the U.S. Food and Drug Administration approved tadalafil to treat the signs and symptoms of benign prostatic hyperplasia, and for the treatment of BPH and erectile dysfunction (ED), when the conditions occur simultaneously.[69]
Others
Antimuscarinics such as tolterodine may also be used, especially in combination with alpha blockers.[70] They act by decreasing acetylcholine effects on the smooth muscle of the bladder, thus helping control symptoms of an overactive bladder.[71]
Phosphodiesterase-5 inhibitors such as sildenafil citrate show some symptomatic relief,[67] suggesting a possible common cause with erectile dysfunction. Tadalafil was considered then rejected by NICE in the UK for the treatment of symptoms associated with BPH.[68] In 2011, the U.S. Food and Drug Administration approved tadalafil to treat the signs and symptoms of benign prostatic hyperplasia, and for the treatment of BPH and erectile dysfunction (ED), when the conditions occur simultaneously.[69]
Self-catheterization
Intermittent urinary catheterization is used to relieve the bladder in people with urinary retention. Self-catheterization is an option in BPH when it is difficult or impossible to completely empty the bladder.[72] Urinary tract infection is the most common complication of intermittent catheterization.[73] Several techniques and types of catheter are available, including sterile (single-use) and clean (multiple use) catheters, but, based on current information, none is superior to others in reducing the incidence of urinary tract infection.[74]
Surgery

If medical treatment is not effective, surgery may be performed. Surgical techniques used include the following:
- Transurethral resection of the prostate (TURP): the gold standard.[75] TURP is thought to be the most effective approach for improving urinary symptoms and urinary flow, however, this surgical procedure may be associated with complications in up to 20% of men.[75] Surgery carries some risk of complications, such as retrograde ejaculation (most commonly), erectile dysfunction, urinary incontinence, urethral strictures.[76]
- Open prostatectomy: not usually performed nowadays, even if results are very good.
- Transurethral incision of the prostate (TUIP): rarely performed; the technique is similar to TURP but less definitive.
- Photoselective (laser) vaporization of the prostate (PVP): common treatment.
- Prostatic urethral lift (marketed as UroLift), a minimally invasive device to open the urethra. May preserve sexual function. [77]
Endovascular
The latest alternative to surgical treatment is arterial embolization, an endovascular procedure performed in interventional radiology.[78] Through catheters, embolic agents are released in the main branches of the prostatic artery, in order to induce a decrease in the size of the prostate gland, thus reducing the urinary symptoms.[79]
Transurethral microwave thermotherapy
Transurethral microwave thermotherapy (TUMT) is an outpatient procedure that is less invasive compared to surgery and involves using microwaves (heat) to shrink prostate tissue that is enlarged.[75] TUMT may be effective at safely improving symptoms, however, TUMT does not appear to be as effective as a surgical approaches such as TURP.[75]
Alternative medicine
While herbal remedies are commonly used, a 2016 review found them to be no better than placebo.[80] Saw palmetto extract from Serenoa repens, while one of the most commonly used, is no better than placebo in both symptom relief and decreasing prostate size.[81][82][83] Other ineffective herbal medicines include beta-sitosterol[84] from Hypoxis rooperi (African star grass), pygeum (extracted from the bark of Prunus africana),[85] pumpkin seeds (Cucurbita pepo) and stinging nettle (Urtica dioica) root.[86] A systematic review of Chinese herbal medicines found that the quality of studies was insufficient to indicate any superiority over Western medicines.[87]
Epidemiology

Globally, benign prostatic hyperplasia affects about 210 million males as of 2010 (6% of the population).[89]
The prostate gets larger in most men as they get older. For a symptom-free man of 46 years, the risk of developing BPH over the next 30 years is 45%. Incidence rates increase from 3 cases per 1000 man-years at age 45–49 years, to 38 cases per 1000 man-years by the age of 75–79 years. While the prevalence rate is 2.7% for men aged 45–49, it increases to 24% by the age of 80 years.[90]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 "Prostate Enlargement (Benign Prostatic Hyperplasia)". NIDDK. September 2014. Archived from the original on 4 October 2017. Retrieved 19 October 2017.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 2.25 2.26 2.27 2.28 Kim, EH; Larson, JA; Andriole, GL (2016). "Management of Benign Prostatic Hyperplasia". Annual Review of Medicine (Review). 67: 137–51. doi:10.1146/annurev-med-063014-123902. PMID 26331999.
- ↑ 3.0 3.1 GBD 2015 Disease and Injury Incidence and Prevalence, Collaborators. (8 October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ↑ Silva, Valter; Grande, Antonio Jose; Peccin, Maria S (6 April 2019). "Physical activity for lower urinary tract symptoms secondary to benign prostatic obstruction". Cochrane Database of Systematic Reviews. 4: CD012044. doi:10.1002/14651858.CD012044.pub2. PMC 6450803. PMID 30953341.
- ↑ 5.0 5.1 Ton, Joey (30 May 2022). "#316 To Pee or Not to Pee: Combination agents for benign prostatic hypertrophy". CFPCLearn. Retrieved 14 June 2023.
- ↑ Chang, RT; Kirby, R; Challacombe, BJ (Apr 2012). "Is there a link between BPH and prostate cancer?". Practitioner. 256 (1750): 13–6, 2. PMID 22792684.
- ↑ Lower urinary tract symptoms in men: management, NICE (National Institute for Health and Care Excellence)
- ↑ "Urge incontinence". MedlinePlus. US National Library of Medicine. Archived from the original on 6 October 2015. Retrieved 26 October 2015.
- ↑ White, JM; O'Brien, DP; Walker, HK; Hall, WD; Hurst, JW (1990). "Incontinence and Stream Abnormalities". PMID 21250138.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Robinson, J (11 February 2008). "Post-micturition dribble in men: causes and treatment". Nursing Standard. 22 (30): 43–6. doi:10.7748/ns2008.04.22.30.43.c6440. PMID 18459613.
- ↑ Sarma, AV; Wei, JT (19 July 2012). "Clinical practice. Benign prostatic hyperplasia and lower urinary tract symptoms". The New England Journal of Medicine. 367 (3): 248–57. doi:10.1056/nejmcp1106637. PMID 22808960.
- ↑ "Urination – difficulty with flow". MedlinePlus. US National Library of Medicine. Archived from the original on 6 October 2015. Retrieved 26 October 2015.
- ↑ "Urination – painful". MedlinePlus. US National Library of Medicine. Archived from the original on 6 October 2015. Retrieved 26 October 2015.
- ↑ "Bladder outlet obstruction". MedlinePlus. US National Library of Medicine. Archived from the original on 6 October 2015. Retrieved 26 October 2015.
- ↑ Carlos, J; Almeida, Flavio (July 2008). "Residual Urinary Volume and Urinary Tract Infection- when are they linked?". The Journal of Urology. 180 (1): 182–185. doi:10.1016/j.juro.2008.03.044. PMID 18499191.
- ↑ Wu, CP; Gu, FL (1991). "The prostate in eunuchs". Prog Clin Biol Res. 370: 249–55. PMID 1924456.
- ↑ "Testosterone and Aging: Clinical Research Directions". NCBI Bookshelf. Archived from the original on 5 November 2017. Retrieved 2 February 2015.
- ↑ "Proscar (finisteride) Prescribing Information" (PDF). FDA – Drug Documents. Merck and Company. Archived (PDF) from the original on 3 March 2016. Retrieved 2 March 2015.
- ↑ Bartsch, G; Rittmaster, RS; Klocker, H (2002). "Dihydrotestosterone and the concept of 5alpha-reductase inhibition in human benign prostatic hyperplasia". World J Urol. 19 (6): 413–25. doi:10.1007/s00345-002-0248-5. PMID 12022710.
- ↑ Feldman, Brian J.; Feldman, David (2001). "The development of androgen-independent prostate cancer". Nature Reviews Cancer. 1 (1): 34–45. doi:10.1038/35094009. PMID 11900250.
- ↑ Lagiou, Pagona; Mantzoros, Christos S.; Tzonou, Anastasia; Signorello, Lisa B.; Lipworth, Loren; Trichopoubs, Dimitrios (1997). "Serum Steroids in Relation to Benign Prostatic Hyperplasia". Oncology. 54 (6): 497–501. doi:10.1159/000227609. PMID 9394847.
- ↑ 22.0 22.1 Roberts, Rosebud O.; Jacobson, Debra J.; Rhodes, Thomas; Klee, George G.; Leiber, Michael M.; Jacobsen, Steven J. (2004). "Serum sex hormones and measures of benign prostatic hyperplasia". The Prostate. 61 (2): 124–31. doi:10.1002/pros.20080. PMID 15305335.
- ↑ Page, S. T.; Lin, D. W.; Mostaghel, E. A.; Hess, D. L.; True, L. D.; Amory, J. K.; Nelson, P. S.; Matsumoto, A. M.; Bremner, W. J. (2006). "Persistent Intraprostatic Androgen Concentrations after Medical Castration in Healthy Men". Journal of Clinical Endocrinology & Metabolism. 91 (10): 3850–6. doi:10.1210/jc.2006-0968. PMID 16882745.
- ↑ Ho, C. K M; Nanda, J.; Chapman, K. E; Habib, F. K (2008). "Oestrogen and benign prostatic hyperplasia: effects on stromal cell proliferation and local formation from androgen". Journal of Endocrinology. 197 (3): 483–91. doi:10.1677/JOE-07-0470. PMID 18492814.
- ↑ Niu, YJ; Ma, TX; Zhang, J; Xu, Y; Han, RF; Sun, G (2003). "Androgen and prostatic stroma". Asian Journal of Andrology. 5 (1): 19–26. PMID 12646998.
- ↑ Ansari, Mohammad Abduljalil; Begum, Dilruba; Islam, Fakhrul (2008). "Serum sex steroids, gonadotrophins and sex hormone-binding globulin in prostatic hyperplasia". Annals of Saudi Medicine. 28 (3): 174–8. doi:10.4103/0256-4947.51727. PMC 6074428. PMID 18500180.
- ↑ Gat, Y; Gornish, M; Heiblum, M; Joshua, S (2008). "Reversal of benign prostate hyperplasia by selective occlusion of impaired venous drainage in the male reproductive system: novel mechanism, new treatment". Andrologia. 40 (5): 273–281. doi:10.1111/j.1439-0272.2008.00883.x. PMID 18811916.
- ↑ Heber, D (2002). "Prostate enlargement: the canary in the coal mine?". Am J Clin Nutr. 75 (4): 605–6. doi:10.1093/ajcn/75.4.605. PMID 11916745.
- ↑ Zhang, SX; Yu, B; Guo, SL; Wang, YW; Yin, CK (February 2003). "[Comparison of incidence of BPH and related factors between urban and rural inhabitants in district of Wannan]". Zhonghua Nan Ke Xue = National Journal of Andrology. 9 (1): 45–7. PMID 12680332.
- ↑ Gu, F (March 1997). "Changes in the prevalence of benign prostatic hyperplasia in China". Chinese Medical Journal. 110 (3): 163–6. PMID 9594331.
- ↑ Chyou, PH (1993). "A prospective study of alcohol, diet, and other lifestyle factors in relation to obstructive uropathy". Prostate. 22 (3): 253–64. doi:10.1002/pros.2990220308. PMID 7683816.
- ↑ Suzuki, S (2002). "Intakes of energy and macronutrients and the risk of benign prostatic hyperplasia". Am J Clin Nutr. 75 (4): 689–97. doi:10.1093/ajcn/75.4.689. PMID 11916755.
- ↑ Gacci, M (2015). "Metabolic syndrome and benign prostatic enlargement: a systematic review and meta-analysis". BJU International. 115 (1): 24–31. doi:10.1111/bju.12728. PMID 24602293.
- ↑ Wang, Jicun; Michelitsch, Thomas; Wunderlin, Arne; Mahadeva, Ravi (2009). "Aging as a consequence of Misrepair –a novel theory of aging". 0904 (575). arXiv:0904.0575. Bibcode:2009arXiv0904.0575W.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Wang-Michelitsch, Jicun; Michelitsch, Thomas (2015). "Aging as a process of accumulation of Misrepairs". 1503 (7163). arXiv:1503.07163. Bibcode:2015arXiv150307163W.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Wang-Michelitsch, Jicun; Michelitsch, Thomas (2015). "Tissue fibrosis: a principal evidence for the central role of Misrepairs in aging". 1505 (1376). arXiv:1503.01376. Bibcode:2015arXiv150301376C.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 37.0 37.1 37.2 37.3 37.4 Wasserman, Neil F. (1 September 2006). "Benign Prostatic Hyperplasia: A Review and Ultrasound Classification". Radiologic Clinics of North America. 44 (5): 689–710. doi:10.1016/j.rcl.2006.07.005. PMID 17030221.
- ↑ 38.0 38.1 38.2 Üçer, Oktay (1 December 2011). "Giant prostatic hyperplasia: Case report and literature review". Dicle Medical Journal / Dicle tıp Dergisi. 38 (4): 489–491. doi:10.5798/diclemedj.0921.2011.04.0072.
- ↑ Parsons, JK (December 2010). "Benign Prostatic Hyperplasia and Male Lower Urinary Tract Symptoms: Epidemiology and Risk Factors". Current Bladder Dysfunction Reports. 5 (4): 212–218. doi:10.1007/s11884-010-0067-2. PMC 3061630. PMID 21475707.
- ↑ Eid, K; Krughoff, K; Stoimenova, D; Smith, D; Phillips, J; O'Donnell, C; Barqawi, A (January 2014). "Validation of the Urgency, Weak stream, Incomplete emptying, and Nocturia (UWIN) score compared with the American Urological Association Symptoms Score in assessing lower urinary tract symptoms in the clinical setting". Urology. 83 (1): 181–5. doi:10.1016/j.urology.2013.08.039. PMID 24139351.
- ↑ 41.0 41.1 41.2 41.3 41.4 Hwang, Eu Chang; Gandhi, Shreyas; Jung, Jae Hung; Imamura, Mari; Kim, Myung Ha; Pang, Ran; Dahm, Philipp (2018). "Naftopidil for the treatment of lower urinary tract symptoms compatible with benign prostatic hyperplasia". The Cochrane Database of Systematic Reviews. 10: CD007360. doi:10.1002/14651858.CD007360.pub3. ISSN 1469-493X. PMC 6516835. PMID 30306544.
- ↑ Silva, Valter (2019). "Physical activity for lower urinary tract symptoms secondary to benign prostatic obstruction". Cochrane Database of Systematic Reviews. 4 (4): CD012044. doi:10.1002/14651858.CD012044.pub2. PMC 6450803. PMID 30953341.
- ↑ "Benign prostatic hyperplasia". University of Maryland Medical Center. Archived from the original on 25 April 2017. Retrieved 9 October 2013.
- ↑ Y. de Jong; R.M. ten Brinck; J.H.F.M. Pinckaers; A.A.B. Lycklama à Nijeholt. "Influence of voiding posture on urodynamic parameters in men: a literature review" (PDF). Nederlands Tijdschrift voor urologie. Archived (PDF) from the original on 14 July 2014. Retrieved 2 July 2014.
- ↑ de Jong, Y; Pinckaers, JH; Ten Brinck, RM; Lycklama À Nijeholt, AA; Dekkers, OM (2014). "Urinating Standing versus Sitting: Position Is of Influence in Men with Prostate Enlargement. A Systematic Review and Meta-Analysis". PLOS ONE. 9 (7): e101320. Bibcode:2014PLoSO...9j1320D. doi:10.1371/journal.pone.0101320. PMC 4106761. PMID 25051345.
- ↑ Silva, J; Silva, CM; Cruz, F (January 2014). "Current medical treatment of lower urinary tract symptoms/BPH: do we have a standard?". Current Opinion in Urology. 24 (1): 21–8. doi:10.1097/mou.0000000000000007. PMID 24231531.
- ↑ Roehrborn, Claus G.; Nuckolls, James G.; Wei, John T.; Steers, William; BPH Registry and Patient Survey Steering Committee (2007). "The Benign Prostatic Hyperplasia Registry and Patient Survey: study design, methods and patient baseline characteristics". BJU International. 100 (4): 813–9. doi:10.1111/j.1464-410X.2007.07061.x. hdl:2027.42/73286. PMID 17822462.
- ↑ Black, L; Naslund, MJ; Gilbert Jr, TD; Davis, EA; Ollendorf, DA (2006). "An examination of treatment patterns and costs of care among patients with benign prostatic hyperplasia". The American Journal of Managed Care. 12 (4 Suppl): S99–S110. PMID 16551208.
{{cite journal}}: CS1 maint: url-status (link) - ↑ Hutchison, A; Farmer, R; Verhamme, K; Berges, R; Navarrete, R (2007). "The Efficacy of Drugs for the Treatment of LUTS/BPH, A Study in 6 European Countries". European Urology. 51 (1): 207–15 discussion 215–6. doi:10.1016/j.eururo.2006.06.012. PMID 16846678.
- ↑ MacDonald, Roderick; Wilt, Timothy J. (2005). "Alfuzosin for treatment of lower urinary tract symptoms compatible with benign prostatic hyperplasia: A systematic review of efficacy and adverse effects". Urology. 66 (4): 780–8. doi:10.1016/j.urology.2005.05.001. PMID 16230138.
- ↑ Roehrborn, Claus G (2001). "Efficacy and safety of once-daily alfuzosin in the treatment of lower urinary tract symptoms and clinical benign prostatic hyperplasia: a randomized, placebo-controlled trial". Urology. 58 (6): 953–9. doi:10.1016/S0090-4295(01)01448-0. PMID 11744466.
- ↑ MacDonald, Roderick; Wilt, Timothy J.; Howe, R. William (2004). "Doxazosin for treating lower urinary tract symptoms compatible with benign prostatic obstruction: a systematic review of efficacy and adverse effects". BJU International. 94 (9): 1263–70. doi:10.1111/j.1464-410X.2004.05154.x. PMID 15610102.
- ↑ 53.0 53.1 Wilt, TJ; Mac Donald, R; Rutks, I (2003). "Tamsulosin for benign prostatic hyperplasia". The Cochrane Database of Systematic Reviews (1): CD002081. doi:10.1002/14651858.CD002081. PMID 12535426.
- ↑ 54.0 54.1 Djavan, Bob; Marberger, Michael (1999). "A Meta-Analysis on the Efficacy and Tolerability of α1-Adrenoceptor Antagonists in Patients with Lower Urinary Tract Symptoms Suggestive of Benign Prostatic Obstruction". European Urology. 36 (1): 1–13. doi:10.1159/000019919. PMID 10364649.
- ↑ Santillo, VM; Lowe FC (2006). "Treatment of benign prostatic hyperplasia in patients with cardiovascular disease". Drugs & Aging. 23 (10): 795–805. doi:10.2165/00002512-200623100-00003. PMID 17067183.
- ↑ Aua Practice Guidelines, Committee (2003). "AUA Guideline on Management of Benign Prostatic Hyperplasia (2003). Chapter 1: Diagnosis and Treatment Recommendations". The Journal of Urology. 170 (2 Pt 1): 530–47. doi:10.1097/01.ju.0000078083.38675.79. PMID 12853821.
- ↑ Blankstein, U; Van Asseldonk, B; Elterman, DS (February 2016). "BPH update: medical versus interventional management" (PDF). The Canadian Journal of Urology. 23 (Supplement 1): 10–15. PMID 26924590. Archived (PDF) from the original on 7 August 2016.
- ↑ Roehrborn, C; Bruskewitz, R; Nickel, J; McConnell, J; Saltzman, B; Gittelman, M; Malek, G; Gottesman, J; et al. (2004). "Sustained Decrease in Incidence of Acute Urinary Retention and Surgery With Finasteride for 6 Years in Men With Benign Prostatic Hyperplasia". The Journal of Urology. 171 (3): 1194–8. doi:10.1097/01.ju.0000112918.74410.94. PMID 14767299.
- ↑ Roehrborn, CG; Barkin, J; Tubaro, A; Emberton, M; Wilson, TH; Brotherton, BJ; Castro, R (April 2014). "Influence of baseline variables on changes in International Prostate Symptom Score after combined therapy with dutasteride plus tamsulosin or either monotherapy in patients with benign prostatic hyperplasia and lower urinary tract symptoms: 4-year results of the CombAT study". BJU International. 113 (4): 623–35. doi:10.1111/bju.12500. PMID 24127818.
- ↑ 60.0 60.1 Greco, KA; McVary, KT (December 2008). "The role of combination medical therapy in benign prostatic hyperplasia". International Journal of Impotence Research. 20 Suppl 3: S33–43. doi:10.1038/ijir.2008.51. PMID 19002123.
- ↑ Kaplan, S; McConnell, J; Roehrborn, C; Meehan, A; Lee, M; Noble, W; Kusek, J; Nybergjr, L; Medical Therapy of Prostatic Symptoms (MTOPS) Research Group (2006). "Combination Therapy With Doxazosin and Finasteride for Benign Prostatic Hyperplasia in Patients With Lower Urinary Tract Symptoms and a Baseline Total Prostate Volume of 25 Ml or Greater". The Journal of Urology. 175 (1): 217–20, discussion 220–1. doi:10.1016/S0022-5347(05)00041-8. PMID 16406915.
- ↑ Barkin, J; Guimarães, M; Jacobi, G; Pushkar, D; Taylor, S; van Vierssen Trip, OB (October 2003). "Alpha-blocker therapy can be withdrawn in the majority of men following initial combination therapy with the dual 5alpha-reductase inhibitor dutasteride". European Urology. 44 (4): 461–6. doi:10.1016/s0302-2838(03)00367-1. PMID 14499682.
- ↑ Gormley, Glenn J.; Stoner, Elizabeth; Bruskewitz, Reginald C.; Imperato-Mcginley, Julianne; Walsh, Patrick C.; McConnell, John D.; Andriole, Gerald L.; Geller, Jack; et al. (1992). "The Effect of Finasteride in Men with Benign Prostatic Hyperplasia". New England Journal of Medicine. 327 (17): 1185–91. doi:10.1056/NEJM199210223271701. PMID 1383816.
- ↑ Gacci, M; Ficarra, V; Sebastianelli, A; Corona, G; Serni, S; Shariat, SF; Maggi, M; Zattoni, F; Carini, M; Novara, G (June 2014). "Impact of medical treatments for male lower urinary tract symptoms due to benign prostatic hyperplasia on ejaculatory function: a systematic review and meta-analysis". The Journal of Sexual Medicine. 11 (6): 1554–66. doi:10.1111/jsm.12525. PMID 24708055.
- ↑ Deters, Levi. "Benign Prostatic Hypertrophy Treatment & Management". Medscape. Archived from the original on 30 October 2015. Retrieved 14 November 2015.
- ↑ Wang Y, Bao Y, Liu J, Duan L, Cui Y (January 2018). "Tadalafil 5 mg Once Daily Improves Lower Urinary Tract Symptoms and Erectile Dysfunction: A Systematic Review and Meta-analysis". Low Urin Tract Symptoms. 10 (1): 84–92. doi:10.1111/luts.12144. PMID 29341503.
- ↑ 67.0 67.1 Pattanaik, Smita; Mavuduru, Ravimohan S.; Panda, Arabind; Mathew, Joseph L.; Agarwal, Mayank M.; Hwang, Eu Chang; Lyon, Jennifer A.; Singh, Shrawan K.; Mandal, Arup K. (2018-11-16). "Phosphodiesterase inhibitors for lower urinary tract symptoms consistent with benign prostatic hyperplasia". The Cochrane Database of Systematic Reviews. 11: CD010060. doi:10.1002/14651858.CD010060.pub2. ISSN 1469-493X. PMC 6517182. PMID 30480763.
- ↑ 68.0 68.1 "Hyperplasia (benign prostatic) – tadalafil (terminated appraisal) (TA273)". National Institute for Health and Clinical Excellence (NICE). Archived from the original on 24 February 2013. Retrieved 27 January 2013.
- ↑ 69.0 69.1 "FDA approves Cialis to treat benign prostatic hyperplasia". U.S. Food and Drug Administration (FDA). Archived from the original on 11 May 2013. Retrieved 7 May 2013.
- ↑ Kaplan, S. A.; Roehrborn, C. G.; Rovner, E. S.; Carlsson, M.; Bavendam, T.; Guan, Z. (2006). "Tolterodine and Tamsulosin for Treatment of Men With Lower Urinary Tract Symptoms and Overactive Bladder: A Randomized Controlled Trial". JAMA: The Journal of the American Medical Association. 296 (19): 2319–28. doi:10.1001/jama.296.19.2319. PMID 17105794.
- ↑ Abrams, P; Andersson, KE (November 2007). "Muscarinic receptor antagonists for overactive bladder". BJU International. 100 (5): 987–1006. doi:10.1111/j.1464-410x.2007.07205.x. PMID 17922784.
- ↑ "Prostate enlargement (benign prostatic hyperplasia)". Harvard Health Content. Harvard Health Publications. Archived from the original on 3 April 2015. Retrieved 2 February 2015.
- ↑ Wyndaele, JJ (2002). "Complications of intermittent catheterization: their prevention and treatment". Spinal Cord. 40 (10): 536–41. doi:10.1038/sj.sc.3101348. PMID 12235537.
- ↑ Prieto, J; Murphy, CL; Moore, KN; Fader, M (10 Sep 2014). "Intermittent catheterisation for long-term bladder management". Cochrane Database Syst Rev. 9 (9): CD006008. doi:10.1002/14651858.CD006008.pub3. PMID 25208303.
- ↑ 75.0 75.1 75.2 75.3 Hoffman, Richard M.; Monga, Manoj; Elliott, Sean P.; Macdonald, Roderick; Langsjoen, Jens; Tacklind, James; Wilt, Timothy J. (2012-09-12). "Microwave thermotherapy for benign prostatic hyperplasia". The Cochrane Database of Systematic Reviews (9): CD004135. doi:10.1002/14651858.CD004135.pub3. ISSN 1469-493X. PMID 22972068.
- ↑ "Transurethral resection of the prostate (TURP) - Risks". nhs.uk. 2017-10-24. Archived from the original on 18 February 2020. Retrieved 2020-03-08.
- ↑ Helo, Sevann; Welliver, Charles; McVary, Keviv (2020). "Minimally Invasive and Endoscopic Management of Benign Prostatic Hyperplasia". Campbell-Walsh-Wein urology. Partin, Alan W.,, Dmochowski, Roger R.,, Kavoussi, Louis R.,, Peters, Craig (Craig Andrew) (Twelfth ed.). Philadelphia, PA: Elsevier. pp. 3403–3488. ISBN 0-323-54642-0. OCLC 1130700336. Archived from the original on 20 July 2020. Retrieved 19 July 2020.
- ↑ Kuang M, Vu A, Athreya S (2017). "A systematic review of prostatic artery embolization in the treatment of symptomatic benign prostatic hyperplasia". Cardiovasc Intervent Radiol. 40 (5): 655–663. doi:10.1007/s00270-016-1539-3. PMID 28032133.
- ↑ Pisco J, Bilhim T, Pinheiro LC, Fernandes L, Pereira J, Costa NV, Duarte M, Oliveira AG (2016). "Prostate embolization as an alternative to open surgery in patients with large prostate and moderate to severe lower urinary tract symptoms". J Vasc Interv Radiol. 27 (5): 700–8. doi:10.1016/j.jvir.2016.01.138. PMID 27019980.
- ↑ Keehn; Taylor; Lowe (2016). "Phytotherapy for benign prostatic hyperplasia". Curr. Urol. Rep. 17 (7): 53. doi:10.1007/s11934-016-0609-z. PMID 27180172.
- ↑ Bent, Stephen; Kane, Christopher; Shinohara, Katsuto; Neuhaus, John; Hudes, Esther S.; Goldberg, Harley; Avins, Andrew L. (2006). "Saw Palmetto for Benign Prostatic Hyperplasia" (PDF). New England Journal of Medicine. 354 (6): 557–66. doi:10.1056/NEJMoa053085. PMID 16467543. Archived (PDF) from the original on 8 December 2019. Retrieved 27 August 2019.
- ↑ Dedhia, R; McVary, K (2008). "Phytotherapy for Lower Urinary Tract Symptoms Secondary to Benign Prostatic Hyperplasia". The Journal of Urology. 179 (6): 2119–25. doi:10.1016/j.juro.2008.01.094. PMID 18423748.
- ↑ Tacklind, J; Macdonald, R; Rutks, I; Stanke, JU; Wilt, TJ (December 2012). "Serenoa repens for benign prostatic hyperplasia". Cochrane Database of Systematic Reviews. 12: CD001423. doi:10.1002/14651858.CD001423.pub3. PMC 3090655. PMID 23235581.
- ↑ Wilt, Timothy; Ishani, Areef; MacDonald, Roderick; Stark, Gerold; Mulrow, Cynthia D; Lau, Joseph; Wilt, Timothy (1999). Wilt, Timothy J (ed.). "Beta-sitosterols for benign prostatic hyperplasia". Cochrane Database of Systematic Reviews (2): CD001043. doi:10.1002/14651858.CD001043. PMID 10796740.
- ↑ Wilt, Timothy; Ishani, Areef; Wilt, Timothy; Rutks, I; Stark, G (1998). Wilt, Timothy J (ed.). "Pygeum africanum for benign prostatic hyperplasia". Cochrane Database of Systematic Reviews (1): CD001044. doi:10.1002/14651858.CD001044. PMC 7032619. PMID 11869585.
- ↑ Wilt, Timothy J; Ishani, Areef; Rutks, Indulis; MacDonald, Roderick (2007). "Phytotherapy for benign prostatic hyperplasia". Public Health Nutrition. 3 (4A): 459–72. doi:10.1017/S1368980000000549. PMID 11276294.
- ↑ Ma, CH; Lin, WL; Lui, SL; Cai, XY; Wong, VT; Ziea, E; Zhang, ZJ (July 2013). "Efficacy and safety of Chinese herbal medicine for benign prostatic hyperplasia: systematic review of randomized controlled trials". Asian Journal of Andrology. 15 (4): 471–82. doi:10.1038/aja.2012.173. PMC 3739225. PMID 23728585.
- ↑ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 11 November 2009. Retrieved 11 November 2009.
- ↑ Vos, Theo; et al. (1 December 2012). "Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010". The Lancet. 380 (9859): 2163–2196. doi:10.1016/S0140-6736(12)61729-2. PMC 6350784. PMID 23245607.
- ↑ Verhamme, K; Dieleman, JP; Bleumink, GS; Van Der Lei, J; Sturkenboom, MC; Artibani, W; Begaud, B; Berges, R; et al. (2002). "Incidence and Prevalence of Lower Urinary Tract Symptoms Suggestive of Benign Prostatic Hyperplasia in Primary Care—The Triumph Project". European Urology. 42 (4): 323–8. doi:10.1016/S0302-2838(02)00354-8. PMID 12361895.
External links
| Classification | |
|---|---|
| External resources |

