Balanitis circinata
| Balanitis circinata | |
|---|---|
| Other names: Circinate balanitis | |
 | |
| Balanitis circinata | |
| Specialty | Dermatology |
Balanitis circinata (also known as circinate balanitis) is a skin condition of reactive arthritis comprising a serpiginous ring-shaped dermatitis of the glans penis.[1] Circinate balanitis is one of the most common cutaneous manifestation of reactive arthritis. However, balanitis circinata can also occur independently. Topical corticosteroid therapy is the most commonly used treatment, and topical calcineurin inhibitors have also been used successfully.[2]
Signs and symptoms
At the beginning, people show pin-sized dots with white plaque on them which constantly grow into flat, red areas hardly surrounded by white plaque. Despite the visible symptoms, patients in nearly all cases do not suffer from burning or itching, nor does it smell strange.[3] Due to its analogy to a fungal skin infection, balanitis circinata is often misdiagnosed as mycosis – especially in cases where patients have no other symptoms of reactive arthritis.[citation needed]
Cause
Reactive arthritis is characterized by nongonococcal urethritis, conjunctivitis, and arthritis. Reactive arthritis belongs to the group of arthritides known as the spondyloarthritides. There are two main types of reactive arthritis: post-venereal and post-enteric. Chlamydia trachomatis is thought to be the most common cause of reactive arthritis, in general. Until recently, even the terminology for the condition itself was unclear as multiple eponyms and names have been associated with reactive arthritis. In recent years, a great deal has been learnt about the epidemiology, pathophysiology and treatment of reactive arthritis and chlamydia-induced reactive arthritis, specifically. Prospective epidemiologic data suggest that chlamydia-induced reactive arthritis is underdiagnosed. Other truths being actively revealed include data suggesting that the pathogen itself (i.e., chlamydia) might play an equally important role, or perhaps even more important, than the host with disease susceptibility; asymptomatic chlamydial infections might be a common cause of reactive arthritis and the two variants of reactive arthritis might respond differently to treatment in spite of the congruent clinical presentation. However, much about this syndrome remains shrouded in mystery. Recent data has been suggesting that Chlamydia-induced reactive arthritis might be a common condition that clinicians are simply failing to recognise. Therefore, an emphasis is placed on disease awareness since viable treatment options are emerging.[4]
Treatment
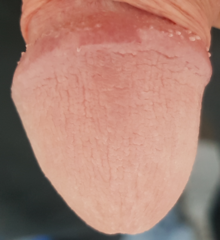
Balanitis circinata is one out of multiple manifestations of the reactive arthritis.[citation needed]
Right now, topical corticosteroid therapy is the most commonly used treatment, and topical calcineurin inhibitors have also been used successfully.[2] Newer tests on patients showed that a less harmful off-label topical treatment with the immunomodulator pimecrolimus or the immunosuppressant tacrolimus can prevent all visible symptoms of this disease.[citation needed] Since reactive arthritis cannot be healed as such, affected people are forced to a continuous topical treatment – otherwise they will again note first symptoms after three to four days without it.[citation needed]
However, strong debates and controversies continue regarding the exact indications of immunomodulators like pimecrolimus and their duration of use in the absence of active controlled trials.[5] A study released in 2015 (tested were 7,457 children with a total of 26,792 person-years) did not find any evidence that pimecrolimus could cause cancer.[6]
References
- ↑ Zanwar, Abhishek; Gupta, Latika; Misra, Ramnath (December 2018). "Balanitis circinata". European Journal of Rheumatology. 5 (4): 285–286. doi:10.5152/eurjrheum.2018.17153. ISSN 2147-9720. PMID 30071931.
- ↑ 2.0 2.1 Bakkour, W.; Chularojanamontri, L.; Motta, L.; Chalmers, R. J. G. (1 January 2014). "Successful use of dapsone for the management of circinate balanitis". Clinical and Experimental Dermatology. 39 (3): 333–335. doi:10.1111/ced.12299. ISSN 1365-2230. PMID 24635073. S2CID 11949436.
- ↑ Prof. Dr. med. Peter Altmeyer (2017-10-23). "Balanitis parakeratotica circinata N48.1" (in Deutsch). Altmeyers Enzyklopädie. Archived from the original on 2019-02-23. Retrieved 2019-02-22.
- ↑ Carter, John D.; Inman, Robert D. (June 2011). "Chlamydia-induced reactive arthritis: Hidden in plain sight?". Best Practice & Research Clinical Rheumatology. 25 (3): 359–374. doi:10.1016/j.berh.2011.05.001. PMID 22100286.
- ↑ Stern RS (2006). "Topical calcineurin inhibitors labeling: putting the "box" in perspective". Archives of Dermatology. 142 (9): 1233–1235. doi:10.1001/archderm.142.9.1233. PMID 16983018.
- ↑ David J. Margolis, Katrina Abuabara, Ole J. Hoffstad, Joy Wan, Denise Raimondo (1 June 2015), "Association Between Malignancy and Topical Use of Pimecrolimus", JAMA Dermatology (in German), vol. 151, no. 6, pp. 594–599, doi:10.1001/jamadermatol.2014.4305, PMC 4465068, PMID 25692459
{{citation}}: CS1 maint: multiple names: authors list (link) CS1 maint: unrecognized language (link)
- Pages with script errors
- CS1 Deutsch-language sources (de)
- CS1 maint: multiple names: authors list
- CS1 maint: unrecognized language
- All articles with unsourced statements
- Articles with unsourced statements from April 2021
- Articles with invalid date parameter in template
- Articles with unsourced statements from May 2020
- Inflammations
- Urological conditions
- Cutaneous conditions
- Chlamydia infections