Autoimmune disease
| Autoimmune disease | |
|---|---|
| Other names: Autoimmune condition | |
 | |
| Young woman with the typical "butterfly rash" found in systemic lupus erythematosus | |
| Specialty | Rheumatology, immunology, gastroenterology, neurology, dermatology |
| Symptoms | Depends on the condition. Commonly low grade fever, feeling tired[1] |
| Usual onset | Adulthood[1] |
| Types | List of autoimmune diseases (alopecia areata, celiac disease, diabetes mellitus type 1, Graves' disease, inflammatory bowel disease, multiple sclerosis, psoriasis, rheumatoid arthritis, systemic lupus erythematosus, others)[1] |
| Medication | Nonsteroidal anti-inflammatory drugs, immunosuppressants, intravenous immunoglobulin[1][2] |
| Frequency | 24 million / 7% (USA)[1][3] |
An autoimmune disease is a condition arising from an abnormal immune response to a functioning body part.[1] There are at least 80 types of autoimmune diseases.[1] Nearly any body part can be involved.[3] Common symptoms include low grade fever and feeling tired.[1] Often symptoms come and go.[1]
The cause is generally unknown.[3] Some autoimmune diseases such as lupus run in families, and certain cases may be triggered by infections or other environmental factors.[1] Some common diseases that are generally considered autoimmune include celiac disease, diabetes mellitus type 1, Graves' disease, inflammatory bowel disease, multiple sclerosis, psoriasis, rheumatoid arthritis, and systemic lupus erythematosus.[1][4] The diagnosis can be difficult to determine.[1]
Treatment depends on the type and severity of the condition.[1] Nonsteroidal anti-inflammatory drugs (NSAIDs) and immunosuppressants are often used.[1] Intravenous immunoglobulin may also occasionally be used.[2] While treatment usually improves symptoms, they do not typically cure the disease.[1]
About 24 million (7%) people in the United States are affected by an autoimmune disease.[1][3] Women are more commonly affected than men.[1] Often they start during adulthood.[1] The first autoimmune diseases were described in the early 1900s.[5]
Signs and symptoms
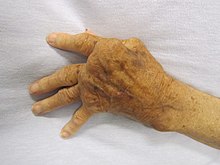
Autoimmune diseases present similar symptoms across the more than eighty different types.[citation needed] The appearance and severity of these signs and symptoms depends on the location and type of autoimmune response that occurs. An individual may also have more than one autoimmune disease simultaneously, and display symptoms of multiple diseases. Signs and symptoms presented, and the disease itself, can be influenced by various other factors such as age, hormones, and environmental factors.[6] In general, the common symptoms are:[7]
- Fatigue
- Low grade fever
- General feeling of unwell (malaise)
- Muscle aches and joint pain
- Rash on different areas of the skin
The appearance of these signs and symptoms can fluctuate, and when they reappear, it is known as a flare-up.[7] Such signs and symptoms may aid in diagnosis by supporting the results from biologic markers of autoimmune diseases.[8]
There are several areas that are commonly impacted by autoimmune diseases. These areas include: blood vessels, underlying connective tissues, joints and muscles, red blood cells, skin, and endocrine glands, like thyroid or pancreas glands.[7]
These diseases tend to have characteristic pathological effects which characterize them as an autoimmune disease. Such features include damage to or destruction of tissues where there is an abnormal immune response, altered organ growth, and altered organ function depending on the location of the disease.[7] Some diseases are organ specific and are restricted to affecting certain tissues, while others are systemic diseases that impact many tissues throughout the body. Signs and symptoms may vary depending on which of these categories an individual’s disease falls under.[9]
Cancer
Research suggests an overall correlation between autoimmune diseases and cancer, in that having an autoimmune disease increases the risk or likelihood of developing certain cancers.[10] Autoimmune diseases cause inflammation through a variety of mechanisms, however, the way in which inflammation is created does not greatly influence cancer risk.[10] Rather, the cancer risk is largely dependent on the fact that all autoimmune diseases increase chronic inflammation which has been linked to cancer.[10] Below are some autoimmune diseases most commonly linked to cancer including celiac disease, inflammatory bowel disease (Crohn's disease and ulcerative colitis), multiple sclerosis, rheumatoid arthritis, and systemic lupus erythematosus.[10]
Causes
The cause is generally unknown.[3] Some autoimmune diseases such as lupus run in families, and certain cases may be triggered by infections or other environmental factors.[1] There are more than 100 autoimmune diseases.[11] Some common diseases that are generally considered autoimmune include celiac disease, diabetes mellitus type 1, Graves' disease, inflammatory bowel disease, multiple sclerosis, psoriasis, rheumatoid arthritis, and systemic lupus erythematosus.[1][4]
Genetics
Autoimmune diseases are conditions in which the human immune system attacks healthy human tissues within the body. The exact genes responsible for causing each autoimmune disease have not been completely isolated. However, several experimental methods such as the genome-wide association scans have been used to identify certain genetic risk variants.[12] Research focusing on both genome scanning and family trait inheritance analysis has enabled scientists to further understand the etiology of autoimmune diseases such as Type 1 diabetes and Rheumatoid arthritis.[13]
- Type 1 diabetes is a condition in which pancreatic β-cells are targeted and destroyed by the immune system.[14] The condition is a result of neo-natal mutations to the insulin gene (INS) which is responsible for mediating the production of the insulin in the pancreas.[14] The INS gene is located on the short arm of chromosome 11p15.5 in between the genes for tyrosine hydroxylase and insulin-like growth factor II.[15] In addition to chromosome 11, a genetic determinant of type 1 diabetes is a locus called the major histocompatibility complex (MHC) located on chromosome 6p21.[13]
- Rheumatoid arthritis: Although there is no complete genetic mapping for this condition, several genes are thought to play a role in causing RA. The genes that influence the human immune system contain a TNF receptor associated factor 1(TRAF1). This TRAF1 is located on chromosome 9q33-34.[16] In addition, B1 genes in the human genome contain an increased concentration of HLA-DRB1 alleles that are most commonly seen in RA patients.[17] RA can vary in severity as a consequence of polymorphisms within the genome.[17]
Environmental factors
A range of environmental factors have been recognized as either having a direct role in development, or being a catalyst to many autoimmune diseases. Current studies indicate up to seventy percent of autoimmune disease are due to environmental factors, including: chemicals, infection, diet, and gut dysbiosis. A single set of steps has been identified to be the most likely theory for autoimmune disease onset.[18]
- Environmental triggers
- Reduced oral tolerance
- Gut dysbiosis
- Enhanced gut permeability
- Increased immune reactivity
- Autoimmunity
Chemicals can be found within the direct environment or in the form of drugs, including: hydrazines, hair dyes, trichloroethylene, tartrazines, hazardous wastes, and industrial emissions.[19]
UV radiation is found to be a possible cause of development of the autoimmune disease dermatomyositis,[20] exposure to pesticides plays a role in rheumatoid arthritis development,[21] and vitamin D has been found to be a key in preventing immune dysfunctions in older populations.[22] Infectious agents are considered T cell activators, a step needed for activation of autoimmune diseases. These mechanisms are relatively unknown, but are one of the current theories to explain autoimmune diseases triggered by infection such as Guillain-Barre syndrome and rheumatic fever.[23]
Types
Following are the few examples of autoimmune diseases.
Coeliac disease
Coeliac disease presents the strongest associations to gastrointestinal and lymphoproliferative cancers.[10] In coeliac disease, the autoimmune reaction is caused by the body’s loss of immune tolerance to ingested gluten, found primarily in wheat, barley, and rye.[10] This explains the increased risk of gastrointestinal cancers, as the gastrointestinal tract includes the esophagus, stomach, small intestine, large intestine, rectum, and anus, all areas that the ingested gluten would traverse in digestion.[10] The incidence of gastrointestinal cancer can be partially reduced or eliminated if a patient removes gluten from their diet.[10][24][25][26][27] Additionally, celiac disease is correlated with lymphoproliferative cancers.[10]
Inflammatory bowel disease
Inflammatory bowel disease is associated with cancers of the gastrointestinal tract and some lymphoproliferative cancers.[10] Inflammatory bowel disease (IBD) can be further categorized as Crohn's disease or ulcerative colitis.[10] In both cases, individuals with IBD lose immune tolerance for normal bacteria present in the gut microbiome.[10] In this case, the immune system attacks the bacteria and induces chronic inflammation, which has been linked to increased cancer risk.[10]
Multiple sclerosis
Multiple sclerosis is associated with decreased risk of cancer overall but an increased risk of central nervous system cancer, primarily in the brain.[10] Multiple sclerosis is a neurodegenerative disease in which T-cells – a specific type of immune cells – attack the important myelin sheath in brain neurons.[28] This reduces the nervous system function, creating inflammation and subsequent cancer of the brain.[10]
Rheumatoid arthritis
Rheumatoid arthritis presents mild, yet significant associations with focal cancers all throughout the body as well as lymphoproliferative cancers.[10] In rheumatoid arthritis, cells that make up the body’s joints and cartilages become invasive and induce local inflammation.[10] Additionally, the chronic inflammation and over-activation of the immune system creates an environment that favors further malignant transformation of other cells. This can explain the associations to cancer of the lungs and skin as well as the increased risk of other hematologic cancers none of which are directly affected by the inflammation of joints.[29][30]
Lupus
Systemic lupus erythematosus is associated with focal cancers throughout the body and lymphoproliferative cancers.[10] Systemic lupus erythematosus affects multiple organ systems and is characterized by a widespread loss of immune tolerance.[31] The chronic inflammation throughout the entire body promotes the malignant transformation of other cells which contributes to the increased risk of systemic and lymphoproliferative cancers.[10] Conversely, systemic lupus erythematosus is correlated with a decrease in some cancers. This is best explained by increased immunosurveillance in these areas, however, the mechanism for why these areas experience lower incidence is poorly understood.[10]
Aplastic anemia
In aplastic anemia the body fails to produce blood cells in sufficient numbers. Blood cells are produced in the bone marrow by stem cells that reside there. Aplastic anaemia causes a deficiency of all blood cell types: red blood cells, white blood cells, and platelets.
Pathophysiology
The human immune system typically produces both T cells and B cells that are capable of being reactive with self-antigens, but these self-reactive cells are usually either killed prior to becoming active within the immune system, placed into a state of anergy (silently removed from their role within the immune system due to over-activation), or removed from their role within the immune system by regulatory cells. When any one of these mechanisms fail, it is possible to have a reservoir of self-reactive cells that become functional within the immune system. The mechanisms of preventing self-reactive T cells from being created take place through negative selection process within the thymus as the T cell is developing into a mature immune cell.
Some infections, such as Campylobacter jejuni, have antigens that are similar (but not identical) to our own self-molecules. In this case, a normal immune response to C. jejuni can result in the production of antibodies that also react to a lesser degree with gangliosides of myelin sheath surrounding peripheral nerves' axons (i.e., Guillain–Barré). A major understanding of the underlying pathophysiology of autoimmune diseases has been the application of genome-wide association scans that have identified a degree of genetic sharing among the autoimmune diseases.[32]
Autoimmunity, on the other hand, is the presence of self-reactive immune response (e.g., auto-antibodies, self-reactive T cells), with or without damage or pathology resulting from it.[33] This may be restricted to certain organs (e.g. in autoimmune thyroiditis) or involve a particular tissue in different places (e.g. Goodpasture's disease which may affect the basement membrane in both the lung and the kidney).
There are many theories as to how an autoimmune disease state arises. Some common ones are listed below.
Diagnosis
For a disease to be regarded as an autoimmune disease it needs to answer to Witebsky's postulates (first formulated by Ernest Witebsky and colleagues in 1957 and modified in 1994):[34][35]
- Direct evidence from transfer of disease-causing antibody or disease-causing T lymphocyte white blood cells
- Indirect evidence based on reproduction of the autoimmune disease in experimental animals
- Circumstantial evidence from clinical clues
Symptoms of early autoimmune disease are often the exact same as common illnesses, including: fatigue, fever, malaise, joint pain, and rash. Due to the fact symptoms vary for affected location, disease causing agents, and individuals, it is difficult for proper diagnosis.[36] Typically, diagnosis begins with looking into a patient’s family's history for genetic predisposition. This is combined with various tests, as no single test can identify an autoimmune disease.[19]
Antinuclear antibody
A test used to identify abnormal proteins, known as antinuclear antibodies, produced when the body attacks its own tissues.[36][19] It may test positive in several disorders. This test is most useful for diagnosing systemic lupus erythematosus, having a 95% positive test rate.[37]
Complete blood count
A test taking measurements on maturity levels, count, and size of blood cells.[19][36] Targeted cells include: red blood cells, white blood cells, hemoglobin, hematocrit, and platelets. Based on increased or decreased numbers in these counts, underlying medical conditions may be present; typically, autoimmune disease is represented by low white blood cell count (Leukopenia). For proper diagnosis, further testing is needed.[38]
Complement
A test used to measure levels of a protein group of the immune system called complement within blood. If complement is found in low levels, this may be an indication of disease.[36][19]
C reactive protein
C reactive protein, a protein made in the liver generally increases with inflammation, and may be high in autoimmune disease.[36][19]
Erythrocyte sedimentation rate
This test measures the rate at which a patient’s blood cells descend in a test tube. More rapid descents may indicate inflammation, a common symptom of autoimmune disease.[19][36]
If these tests are indicative antibody abnormalities and inflammation, further tests will be conducted to identify the autoimmune disease present.[19]
Treatment
Treatment depends on the type and severity of the condition. The majority of the autoimmune diseases are chronic and there is no definitive cure, but symptoms can be alleviated and controlled with treatment.[7] Overall, the aim of the various treatment methods is to lessen the presented symptoms for relief and manipulate the body’s autoimmune response, while still preserving the ability of the patient to combat diseases that they may encounter.[39] Traditional treatment options may include immunosuppressant drugs to weaken the overall immune response, such as:[40]
- Non-steroidal anti-inflammatory drugs (NSAIDs) to reduce inflammation
- Glucocorticoids to reduce inflammation
- Disease-modifying anti-rheumatic drugs (DMARDs) to decrease the damaging tissue and organ effects of the inflammatory autoimmune response
Other standard treatment methods include:[7]
- Vitamin or hormone supplements for what the body is lacking due to the disease (insulin, vitamin B12, thyroid hormone, etc.)
- Blood transfusions if the disease is blood related
- Physical therapy if the disease impacts bones, joints, or muscles
Because these drugs aim to reduce the immune response against the body’s own tissues, there are side effects of these traditional treatment methods, such as being more vulnerable to infections that can potentially be life threatening. There are new advancements in medicine for the treatment of autoimmune diseases that are currently being researched, developed, and used today, especially when traditional treatment options fail. These methods aim to either block the activation of pathogenic cells in the body, or alter the pathway that suppresses these cells naturally.[39][41] The goal for these advancements is to have treatment options available that are less toxic to the patient, and have more specific targets.[41] Such options include:
- Monoclonal antibodies that can be used to block pro-inflammatory cytokines
- Antigen-specific immunotherapy which allows immune cells to specifically target the abnormal cells that cause autoimmune disease[41]
- Co-stimulatory blockade that works to block the pathway that leads to the autoimmune response
- Regulatory T cell therapy that utilizes this special type of T cell to suppress the autoimmune response[39]
Epidemiology
The first estimate of US prevalence for autoimmune diseases as a group was published in 1997 by Jacobson, et al. They reported US prevalence to be around 9 million, applying prevalence estimates for 24 diseases to a US population of 279 million.[42] Jacobson's work was updated by Hayter & Cook in 2012.[43] This study used Witebsky's postulates, as revised by Rose & Bona,[35] to extend the list to 81 diseases and estimated overall cumulative US prevalence for the 81 autoimmune diseases at 5.0%, with 3.0% for males and 7.1% for females. The estimated community prevalence, which takes into account the observation that many people have more than one autoimmune disease, was 4.5% overall, with 2.7% for males and 6.4% for females.[43]
Research
In both autoimmune and inflammatory diseases, the condition arises through aberrant reactions of the human adaptive or innate immune systems. In autoimmunity, the patient's immune system is activated against the body's own proteins. In chronic inflammatory diseases, neutrophils and other leukocytes are constitutively recruited by cytokines and chemokines, resulting in tissue damage.
Mitigation of inflammation by activation of anti-inflammatory genes and the suppression of inflammatory genes in immune cells is a promising therapeutic approach.[44][45][46] There is a body of evidence that once the production of autoantibodies has been initialized, autoantibodies have the capacity to maintain their own production.[47]
Stem cell transplantation is being studied and has shown promising results in certain cases.[48]
Altered glycan theory
According to this theory, the effector function of the immune response is mediated by the glycans (polysaccharides) displayed by the cells and humoral components of the immune system. Individuals with autoimmunity have alterations in their glycosylation profile such that a proinflammatory immune response is favored. It is further hypothesized that individual autoimmune diseases will have unique glycan signatures.[49]
Hygiene hypothesis
According to the hygiene hypothesis, high levels of cleanliness expose children to fewer antigens than in the past, causing their immune systems to become overactive and more likely to misidentify own tissues as foreign, resulting in autoimmune or allergic conditions such as asthma.[50]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 "Autoimmune diseases fact sheet". Office on Women's Health. U.S. Department of Health and Human Services. 16 July 2012. Archived from the original on 5 October 2016. Retrieved 5 October 2016.
- ↑ 2.0 2.1 Katz U, Shoenfeld Y, Zandman-Goddard G (2011). "Update on intravenous immunoglobulins (IVIg) mechanisms of action and off- label use in autoimmune diseases". Current Pharmaceutical Design. 17 (29): 3166–75. doi:10.2174/138161211798157540. PMID 21864262.
- ↑ 3.0 3.1 3.2 3.3 3.4 Borgelt, Laura Marie (2010). Women's Health Across the Lifespan: A Pharmacotherapeutic Approach. ASHP. p. 579. ISBN 978-1-58528-194-7. Archived from the original on 2017-09-08.
- ↑ 4.0 4.1 Hohlfeld R, Dornmair K, Meinl E, Wekerle H (February 2016). "The search for the target antigens of multiple sclerosis, part 1: autoreactive CD4+ T lymphocytes as pathogenic effectors and therapeutic targets". The Lancet. Neurology. 15 (2): 198–209. doi:10.1016/S1474-4422(15)00334-8. PMID 26724103. S2CID 20082472.
- ↑ Ananthanarayan R, Paniker CK (2005). Ananthanarayan and Paniker's Textbook of Microbiology. Orient Blackswan. p. 169. ISBN 9788125028086. Archived from the original on 2017-09-08.
- ↑ Smith DA, Germolec DR (October 1999). "Introduction to immunology and autoimmunity". Environmental Health Perspectives. 107 Suppl 5 (suppl 5): 661–5. doi:10.1289/ehp.99107s5661. PMC 1566249. PMID 10502528.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 "Autoimmune disorders". MedlinePlus Medical Encyclopedia. U.S. National Library of Medicine. 2016-01-12. Archived from the original on 2016-01-12. Retrieved 2020-04-14.
- ↑ National Research Council (US) Subcommittee on Immunotoxicology (1992). Autoimmune Diseases. National Academies Press (US). Archived from the original on 2021-04-07. Retrieved 2020-04-16.
- ↑ Wang L, Wang FS, Gershwin ME (October 2015). "Human autoimmune diseases: a comprehensive update". Journal of Internal Medicine. 278 (4): 369–95. doi:10.1111/joim.12395. PMID 26212387.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 10.13 10.14 10.15 10.16 10.17 10.18 10.19 Franks AL, Slansky JE (April 2012). "Multiple associations between a broad spectrum of autoimmune diseases, chronic inflammatory diseases and cancer". Anticancer Research. 32 (4): 1119–36. PMC 3349285. PMID 22493341.
- ↑ "Autoimmune Disease List • AARDA". AARDA. 2016-06-01. Archived from the original on 2021-05-06. Retrieved 2019-03-21.
- ↑ Gregersen PK, Olsson LM (2009). "Recent advances in the genetics of autoimmune disease". Annual Review of Immunology. 27: 363–91. doi:10.1146/annurev.immunol.021908.132653. PMC 2992886. PMID 19302045.
- ↑ 13.0 13.1 Hill NJ, King C, Flodstrom-Tullberg M (May 2008). "Recent acquisitions on the genetic basis of autoimmune disease". Frontiers in Bioscience: A Journal and Virtual Library. 13 (13): 4838–51. doi:10.2741/3043. PMID 18508549.
- ↑ 14.0 14.1 Molven A, Ringdal M, Nordbø AM, Raeder H, Støy J, Lipkind GM, et al. (April 2008). "Mutations in the insulin gene can cause MODY and autoantibody-negative type 1 diabetes". Diabetes. 57 (4): 1131–5. doi:10.2337/db07-1467. PMID 18192540.
- ↑ Bennett ST, Todd JA (1996). "Human type 1 diabetes and the insulin gene: principles of mapping polygenes". Annual Review of Genetics. 30: 343–70. doi:10.1146/annurev.genet.30.1.343. PMID 8982458.
- ↑ Kurreeman FA, Padyukov L, Marques RB, Schrodi SJ, Seddighzadeh M, Stoeken-Rijsbergen G, et al. (September 2007). "A candidate gene approach identifies the TRAF1/C5 region as a risk factor for rheumatoid arthritis". PLOS Medicine. 4 (9): e278. doi:10.1371/journal.pmed.0040278. PMC 1976626. PMID 17880261.
- ↑ 17.0 17.1 Weyand CM, McCarthy TG, Goronzy JJ (May 1995). "Correlation between disease phenotype and genetic heterogeneity in rheumatoid arthritis". The Journal of Clinical Investigation. 95 (5): 2120–6. doi:10.1172/JCI117900. PMC 295811. PMID 7738179.
- ↑ Vojdani A (2014). "A Potential Link between Environmental Triggers and Autoimmunity". Autoimmune Diseases. 2014: 437231. doi:10.1155/2014/437231. PMC 3945069. PMID 24688790.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 19.6 19.7 "Autoimmune Diseases: Symptoms & Causes". Boston Children's Hospital. Archived from the original on 7 April 2021. Retrieved 23 March 2020.
- ↑ Shah M, Targoff IN, Rice MM, Miller FW, Rider LG (July 2013). "Brief report: ultraviolet radiation exposure is associated with clinical and autoantibody phenotypes in juvenile myositis". Arthritis and Rheumatism. 65 (7): 1934–41. doi:10.1002/art.37985. PMC 3727975. PMID 23658122.
- ↑ Meyer A, Sandler DP, Beane Freeman LE, Hofmann JN, Parks CG (July 2017). "Pesticide Exposure and Risk of Rheumatoid Arthritis among Licensed Male Pesticide Applicators in the Agricultural Health Study". Environmental Health Perspectives. 125 (7): 077010. doi:10.1289/EHP1013. PMC 5744649. PMID 28718769.
- ↑ Meier HC, Sandler DP, Simonsick EM, Parks CG (December 2016). "Association between Vitamin D Deficiency and Antinuclear Antibodies in Middle-Aged and Older U.S. Adults". Cancer Epidemiology, Biomarkers & Prevention. 25 (12): 1559–1563. doi:10.1158/1055-9965.EPI-16-0339. PMC 5135624. PMID 27543618.
- ↑ Wucherpfennig KW (October 2001). "Mechanisms for the induction of autoimmunity by infectious agents". The Journal of Clinical Investigation. 108 (8): 1097–104. doi:10.1172/JCI14235. PMC 209539. PMID 11602615.
- ↑ Meresse B, Ripoche J, Heyman M, Cerf-Bensussan N (January 2009). "Celiac disease: from oral tolerance to intestinal inflammation, autoimmunity and lymphomagenesis". Mucosal Immunology. 2 (1): 8–23. doi:10.1038/mi.2008.75. PMID 19079330. S2CID 24980464.
- ↑ Green PH, Fleischauer AT, Bhagat G, Goyal R, Jabri B, Neugut AI (August 2003). "Risk of malignancy in patients with celiac disease". The American Journal of Medicine. 115 (3): 191–5. doi:10.1016/s0002-9343(03)00302-4. PMID 12935825.
- ↑ Volta U, Vincentini O, Silano M (2011). "Papillary cancer of thyroid in celiac disease". Journal of Clinical Gastroenterology. 45 (5): e44-6. doi:10.1097/mcg.0b013e3181ea11cb. PMID 20697293.
- ↑ Catassi C, Bearzi I, Holmes GK (April 2005). "Association of celiac disease and intestinal lymphomas and other cancers". Gastroenterology. 128 (4 Suppl 1): S79-86. doi:10.1053/j.gastro.2005.02.027. PMID 15825131.
- ↑ Frohman EM, Racke MK, Raine CS (March 2006). "Multiple sclerosis--the plaque and its pathogenesis". The New England Journal of Medicine. 354 (9): 942–55. doi:10.1056/nejmra052130. PMID 16510748.
- ↑ Turesson, Carl; Matteson, Eric L. (2009). "Clinical Features of Rheumatoid Arthritis: Extra-Articular Manifestations". Rheumatoid Arthritis. Elsevier. pp. 62–67. doi:10.1016/b978-032305475-1.50014-8. ISBN 978-0-323-05475-1.
- ↑ Khurana R, Berney SM (October 2005). "Clinical aspects of rheumatoid arthritis". Pathophysiology. 12 (3): 153–65. doi:10.1016/j.pathophys.2005.07.009. PMID 16125918.
- ↑ Tsokos GC (December 2011). "Systemic lupus erythematosus". The New England Journal of Medicine. 365 (22): 2110–21. doi:10.1056/nejmra1100359. PMID 22129255.
- ↑ Cotsapas C, Hafler DA (January 2013). "Immune-mediated disease genetics: the shared basis of pathogenesis". Trends in Immunology. 34 (1): 22–6. doi:10.1016/j.it.2012.09.001. PMID 23031829.
- ↑ Harrison's Principles of Internal Medicine. Vol. 1–2 (18th ed.). McGraw-Hill Professional. 2011-08-11. ISBN 978-0-07-174889-6.
- ↑ Witebsky E, Rose NR, Terplan K, Paine JR, Egan RW (July 1957). "Chronic thyroiditis and autoimmunization". Journal of the American Medical Association. 164 (13): 1439–47. doi:10.1001/jama.1957.02980130015004. PMID 13448890.
- ↑ 35.0 35.1 Rose NR, Bona C (September 1993). "Defining criteria for autoimmune diseases (Witebsky's postulates revisited)". Immunology Today. 14 (9): 426–30. doi:10.1016/0167-5699(93)90244-F. PMID 8216719.
- ↑ 36.0 36.1 36.2 36.3 36.4 36.5 "Autoimmune disorders". MedlinePlus Medical Encyclopedia. U.S. National Library of Medicine. Archived from the original on 5 July 2016. Retrieved 23 March 2020.
- ↑ "Antinuclear Antibody (ANA)". labtestsonline.org. Archived from the original on 6 May 2021. Retrieved 14 April 2020.
- ↑ "Complete blood count (CBC)". www.mayoclinic.org. 19 December 2018. Archived from the original on 7 May 2021. Retrieved 14 April 2020.
- ↑ 39.0 39.1 39.2 Rosenblum MD, Gratz IK, Paw JS, Abbas AK (March 2012). "Treating human autoimmunity: current practice and future prospects". Science Translational Medicine. 4 (125): 125sr1. doi:10.1126/scitranslmed.3003504. PMC 4061980. PMID 22422994.
- ↑ Li P, Zheng Y, Chen X (2017). "Drugs for Autoimmune Inflammatory Diseases: From Small Molecule Compounds to Anti-TNF Biologics". Frontiers in Pharmacology. 8: 460. doi:10.3389/fphar.2017.00460. PMC 5506195. PMID 28785220.
- ↑ 41.0 41.1 41.2 Smilek DE, Ehlers MR, Nepom GT (May 2014). "Restoring the balance: immunotherapeutic combinations for autoimmune disease". Disease Models & Mechanisms. 7 (5): 503–13. doi:10.1242/dmm.015099. PMC 4007402. PMID 24795433.
- ↑ Jacobson DL, Gange SJ, Rose NR, Graham NM (September 1997). "Epidemiology and estimated population burden of selected autoimmune diseases in the United States". Clinical Immunology and Immunopathology. 84 (3): 223–43. doi:10.1006/clin.1997.4412. PMID 9281381.
- ↑ 43.0 43.1 Hayter SM, Cook MC (August 2012). "Updated assessment of the prevalence, spectrum and case definition of autoimmune disease". Autoimmunity Reviews. 11 (10): 754–65. doi:10.1016/j.autrev.2012.02.001. PMID 22387972.
- ↑ Mukundan L, Odegaard JI, Morel CR, Heredia JE, Mwangi JW, Ricardo-Gonzalez RR, et al. (November 2009). "PPAR-delta senses and orchestrates clearance of apoptotic cells to promote tolerance". Nature Medicine. 15 (11): 1266–72. doi:10.1038/nm.2048. PMC 2783696. PMID 19838202.
- ↑ Roszer T, Menéndez-Gutiérrez MP, Lefterova MI, Alameda D, Núñez V, Lazar MA, et al. (January 2011). "Autoimmune kidney disease and impaired engulfment of apoptotic cells in mice with macrophage peroxisome proliferator-activated receptor gamma or retinoid X receptor alpha deficiency". Journal of Immunology. 186 (1): 621–31. doi:10.4049/jimmunol.1002230. PMC 4038038. PMID 21135166.
- ↑ Singh RP, Waldron RT, Hahn BH (July 2012). "Genes, tolerance and systemic autoimmunity". Autoimmunity Reviews. 11 (9): 664–9. doi:10.1016/j.autrev.2011.11.017. PMC 3306516. PMID 22155015.
- ↑ Böhm I (May 2003). "Disruption of the cytoskeleton after apoptosis induction with autoantibodies". Autoimmunity. 36 (3): 183–9. doi:10.1080/0891693031000105617. PMID 12911286. S2CID 37887253.
- ↑ Swart JF, Delemarre EM, van Wijk F, Boelens JJ, Kuball J, van Laar JM, Wulffraat NM (April 2017). "Haematopoietic stem cell transplantation for autoimmune diseases". Nature Reviews. Rheumatology. 13 (4): 244–256. doi:10.1038/nrrheum.2017.7. PMID 28228650. S2CID 21264933.
- ↑ Maverakis E, Kim K, Shimoda M, Gershwin ME, Patel F, Wilken R, et al. (February 2015). "Glycans in the immune system and The Altered Glycan Theory of Autoimmunity: a critical review". Journal of Autoimmunity. 57: 1–13. doi:10.1016/j.jaut.2014.12.002. PMC 4340844. PMID 25578468.
- ↑ Rook GA (February 2012). "Hygiene hypothesis and autoimmune diseases". Clinical Reviews in Allergy & Immunology. 42 (1): 5–15. doi:10.1007/s12016-011-8285-8. PMID 22090147. S2CID 15302882.
Further reading
- Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2010). Robbins and Cotran Pathologic Basis of Disease (8th ed.). Elsevier. p. 1464. ISBN 978-1-4160-3121-5.
- Asherson, Ronald (ed.). Handbook of Systemic Autoimmune Diseases. Elsevier. Archived from the original on 2011-08-09. Retrieved 2012-01-25.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1: long volume value
- All articles with unsourced statements
- Articles with unsourced statements from April 2020
- Articles with invalid date parameter in template
- Articles with hatnote templates targeting a nonexistent page
- Articles with Curlie links
- Portal templates with all redlinked portals
- Autoimmune diseases
- Autoinflammatory syndromes
- Medical lists
- RTT
- RTTNEURO
- WHRTT
- RTTOSH