Aneurysm of sinus of Valsalva
| Aneurysm of sinus of Valsalva | |
|---|---|
| Other names: Aortic sinus aneurysm | |
 | |
| Aorta laid open to show the semilunar valves. (Aortic sinus, also known as "sinus of Valsalva", is labeled at upper left.) | |
| Specialty | Cardiology |
| Complications | Rupture, heart failure, stroke |
| Diagnostic method | Echocardiogram, cardiac CT scan, cardiac MRI scan |
| Treatment | Blood pressure control, surgery |
| Medication | Beta-adrenoceptor antagonists |
| Prognosis | Median survival after rupture 3.9 years |
| Frequency | 0.09% |
Aneurysm of the aortic sinus, also known as the sinus of Valsalva, is a rare abnormality of the aorta, the largest artery in the body. The aorta normally has three small pouches that sit directly above the aortic valve (the sinuses of Valsalva), and an aneurysm of one of these sinuses is a thin-walled swelling. Aneurysms may affect the right (65–85%), non-coronary (10–30%), or rarely the left (< 5%) coronary sinus.[1] These aneurysms may not cause any symptoms but if large can cause shortness of breath, palpitations or blackouts. Aortic sinus aneurysms can burst or rupture into adjacent cardiac chambers, which can lead to heart failure if untreated.
Aortic sinus aneurysms may occur in isolation, or may been seen in association with other diseases of the aorta including Marfan syndrome, Loeys-Dietz syndrome, and bicuspid aortic valve. They can be diagnosed using an echocardiogram or cardiac magnetic resonance imaging (MRI) scan. Treatment includes blood pressure control but surgical repair may be needed, especially if the aneurysm ruptures.
Symptoms and signs
If unruptured, sinus of Valsalva aneurysm (commonly abbreviated SVA or SOVA) is usually asymptomatic and typically goes undetected until symptoms appear or medical imaging is performed for other reasons. If symptoms do occur, the most common are shortness of breath, palpitations, myocardial ischemia, and syncope. Even less common, but more serious, presentations are embolic stroke and myocardial infarction due to blockage of a coronary artery by the aneurysm.[2]
A ruptured aneurysm typically leads to an aortocardiac shunt and progressively worsening heart failure.[2]
An aneurysm of the aortic sinus may rupture due to infective endocarditis involving the aortic wall and tertiary-stage syphilis.[citation needed]
The manifestations appear depending on the site where the sinus has ruptured. For example, if the sinus ruptures in a low pressure area like the right atrium or right ventricle then a continuous type of murmur is heard. The murmur is located in the left parasternal region mainly confined to the lower sternum. It is also accompanied by a superficial thrill. A ruptured Sinus of Valsalva abscess represents a surgical emergency.[citation needed]
Causes
This type of aneurysm is typically congenital and may be associated with heart defects. It is sometimes associated with Marfan syndrome or Loeys–Dietz syndrome, but may also result from Ehlers–Danlos syndrome, bicuspid aortic valve,[3] atherosclerosis, hypoplastic left heart syndrome, syphilis, cystic medial necrosis, chest injury, or infective endocarditis.
Diagnosis
-
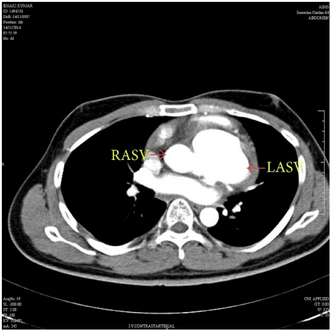
MDCT aortogram suggested left aneurysm of sinus of Valsalva and right aneurysm of sinus of Valsalva with extension into the interventricular septum.
-
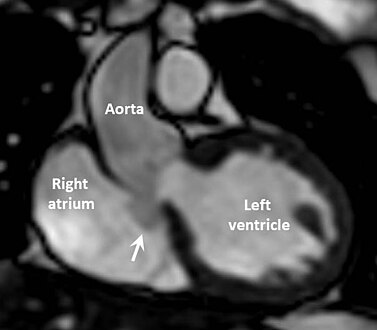
Cardiac MRI scan showing intact sinus of Valsalva aneurysm (arrowed) extending from non-coronary cusp to right atrium.
The first step in diagnosis is typically transthoracic echocardiography. However, if surgery is planned or if the standard echocardiogram lacks sufficient detail, then one or more additional studies are recommended. These studies include transesophageal echocardiography, 3D echocardiography, CT Angiography and aortic angiography.[4] Cardiac MRI may be another option.[2]
Treatment
Medical therapy of aneurysm of the aortic sinus includes blood pressure control through the use of drugs, such as beta blockers.[citation needed]
Another approach is surgical repair.[5] The determination to perform surgery is usually based upon the diameter of the aortic root (with 5 centimeters being a rule of thumb - a normal size is 2-3 centimeters) and the rate of increase in its size (as determined through repeated echocardiography).[citation needed]
An alternative to surgical repair or a ruptured aneurysm is percutaneous closure.[6] In this technique, a wire is introduced via a small incision in the groin and advanced through the vascular system to the aneurysm. A closure device is advanced along the wire before being expanded to straddle the site of rupture.[7]
Prognosis
If a sinus of Valsalva aneurysm ruptures, the life expectancy without treatment is approximately four years.[8] Surgery carries a 1% risk of intra-operative death with higher risks associated with infected aneurysms, and 5- to 10-year survival rates following surgery range from 82-97%.[8]
Epidemiology
Aneurysms of the sinuses of Valsalva are estimated to affect 0.09% of the population.[8] Rupture of a sinus of Valsalva can occur at any age.[8] Rupture is five times more likely to occur in those of far eastern than western ethnic backgrounds, and is twice as likely to occur in males than females. [8]
History
The first description of sinus of Valsalva aneurysm was made in 1939.[9][8]
See also
References
- ↑ Topi, Bernard; John Jinu (2012). "An uncommon cause of a continuous murmur". Experimental and Clinical Cardiology. 17 (3): 148–149. PMC 3628432. PMID 23620707.
- ↑ 2.0 2.1 2.2 Hanna, Mina F.; et al. (17 August 2017). "Cross-sectional imaging of sinus of Valsalva aneurysms: lessons learned". Diagn Interv Radiol. 23 (5): 339–346. doi:10.5152/dir.2017.16522. PMC 5602357. PMID 28814376.
- ↑ Weinreich, M; Yu, PJ; Trost, B (2015). "Sinus of valsalva aneurysms: review of the literature and an update on management". Clinical Cardiology. 38 (3): 185–9. doi:10.1002/clc.22359. PMC 6711005. PMID 25757442.
- ↑ Yang, Yali; et al. (14 March 2017). "Echocardiographic diagnosis of rare pathological patterns of sinus of Valsalva aneurysm". PLOS ONE. 12 (3): e0173122. Bibcode:2017PLoSO..1273122Y. doi:10.1371/journal.pone.0173122. PMC 5349664. PMID 28291779.
- ↑ Vural KM, Sener E, Taşdemir O, Bayazit K (July 2001). "Approach to sinus of Valsalva aneurysms: a review of 53 cases". Eur J Cardiothorac Surg. 20 (1): 71–6. doi:10.1016/S1010-7940(01)00758-8. PMID 11423277.
- ↑ Hanna, Mina F.; Malguria, Nagina; Saboo, Sachin S.; Jordan, Kirk G.; Landay, Michael; Ghoshhajra, Brian B.; Abbara, Suhny (September 2017). "Cross-sectional imaging of sinus of Valsalva aneurysms: lessons learned". Diagnostic and Interventional Radiology (Ankara, Turkey). 23 (5): 339–346. doi:10.5152/dir.2017.16522. ISSN 1305-3612. PMC 5602357. PMID 28814376.
- ↑ Kenny, Damien; Hijazi, Ziyad M. (December 2011). "Transcatheter approaches to non-valvar structural heart disease". The International Journal of Cardiovascular Imaging. 27 (8): 1133–1141. doi:10.1007/s10554-011-9806-5. ISSN 1875-8312. PMID 21331612. S2CID 24898261.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 Ott, David A. (2006). "Aneurysm of the sinus of valsalva". Seminars in Thoracic and Cardiovascular Surgery. Pediatric Cardiac Surgery Annual. 9: 165–176. doi:10.1053/j.pcsu.2006.02.014. ISSN 1092-9126. PMID 16638563.
- ↑ Hope, James (1839). A treatise on the diseases of the heart and great vessels, and on the affections that may be mistaken for them: comprising the author's view of the physiology of the heart's actions and sounds, as demonstrated by his experiments on the motions and sounds. Oxford University.
External links
| Classification | |
|---|---|
| External resources |